 Cancer
Cancer
Cancer is a malignant growth or tumor caused by abnormal and uncontrolled cell division. The hallmark of cancer is its potential ability to invade neighboring tissue or to spread (metastasize) to other parts of the body through the lymphatic system or the bloodstream.
Early cancers may have done neither, remaining localized to the tissue of origin. The majority of cancers in the head and neck are classified as carcinomas.
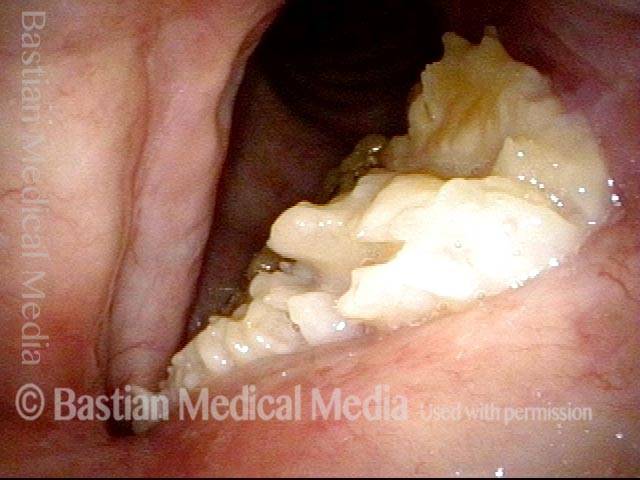
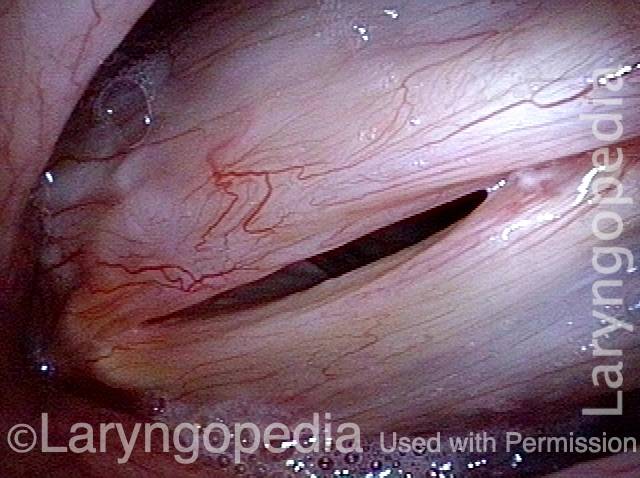
Laser Removal of Vocal Cord Cancer with Bilateral Disease
For treatment of early vocal cord cancer, both laser excision and radiotherapy are in competition as good treatment modalities. See also Early Vocal Cord Cancer: Remove with a Laser, or Radiate? Often, radiation is used when disease is bilateral, in the interest of preserving voice.
This is an example of the ability to do fairly extensive laser surgery bilaterally, yet preserving good voice. This man had a friend who had severe difficulty with radiation, and he was therefore opposed to that option.
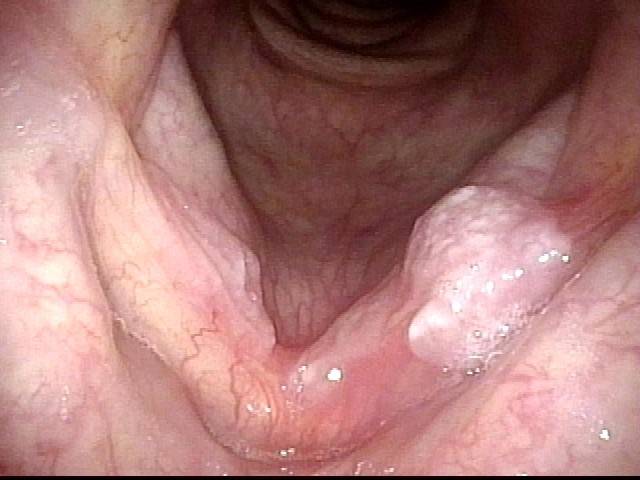
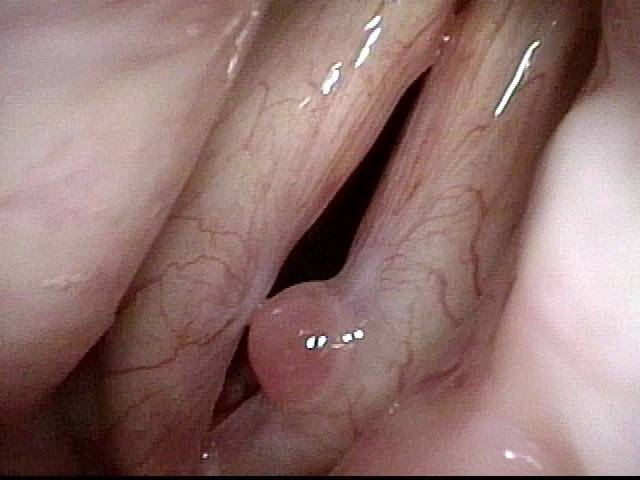
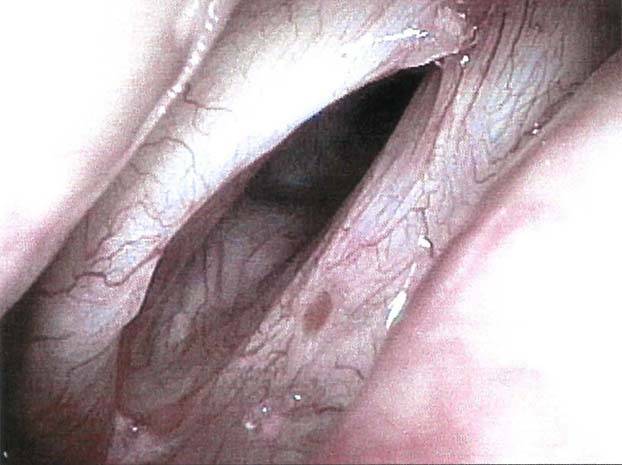
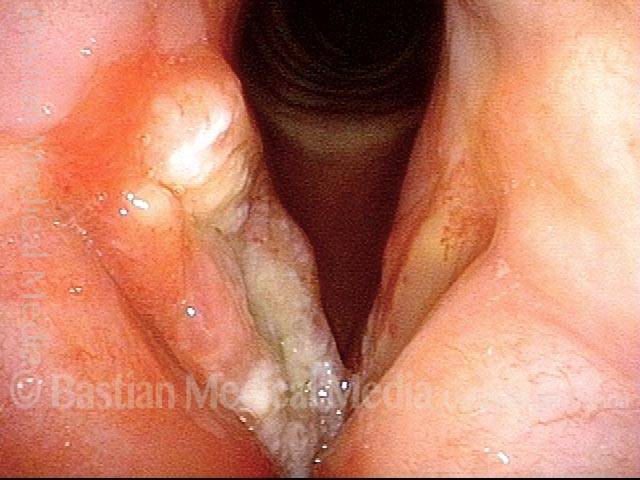
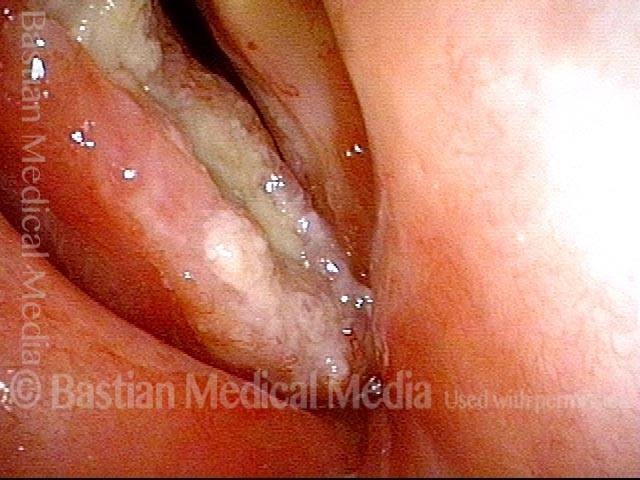
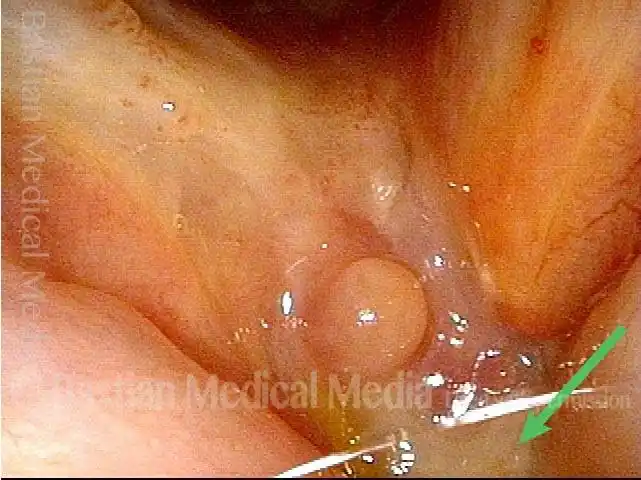
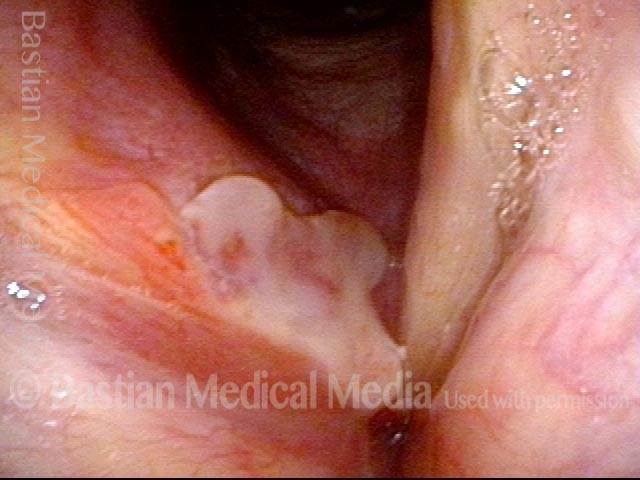
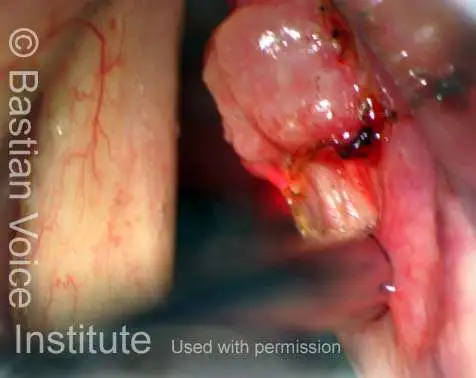
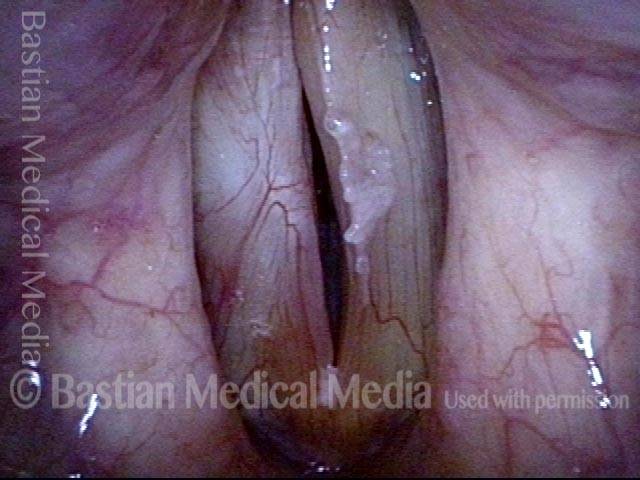
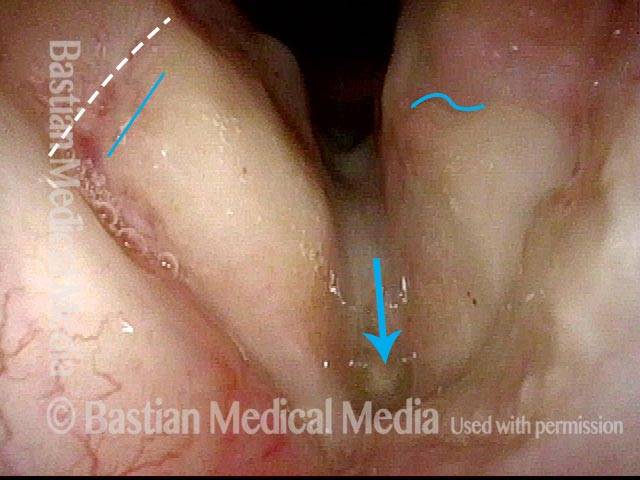
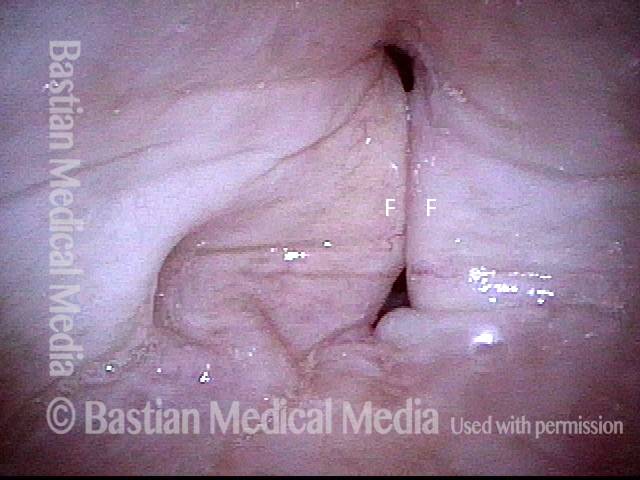
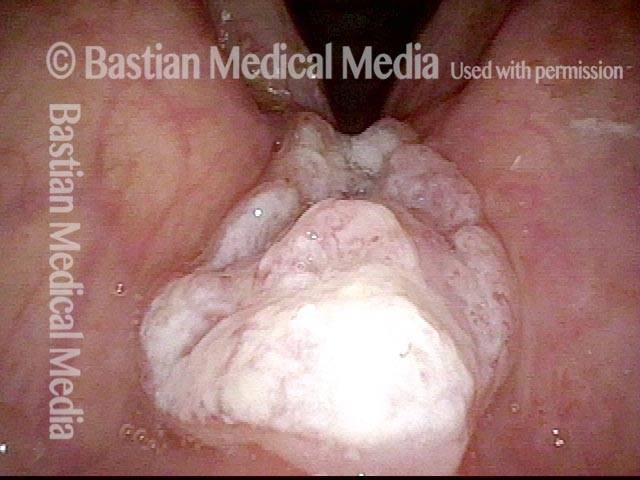
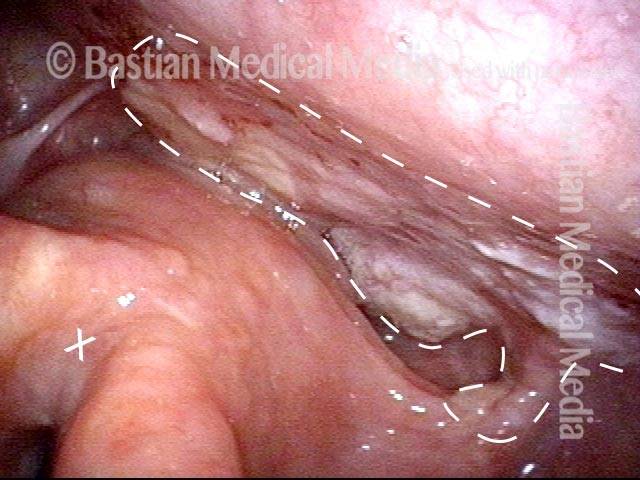
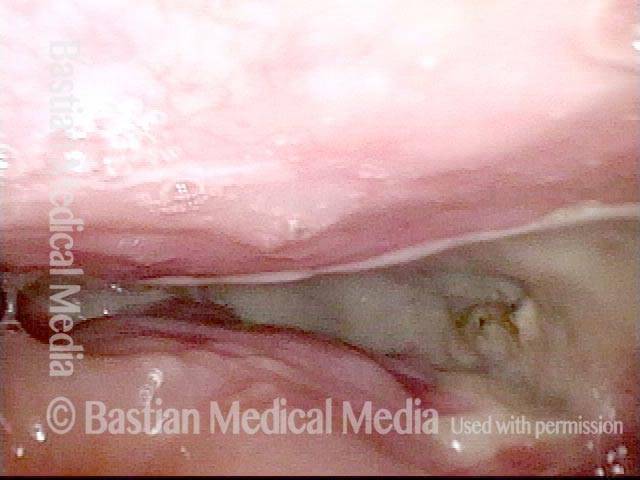
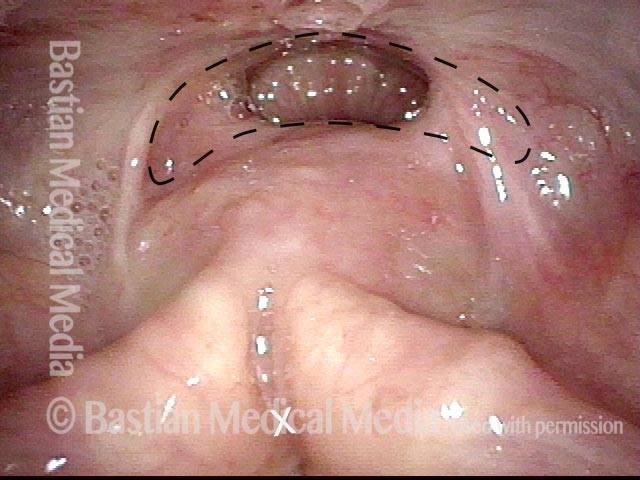
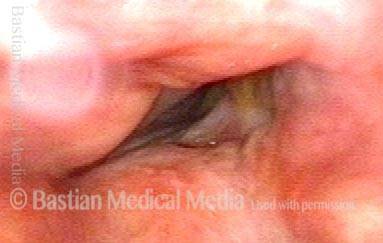
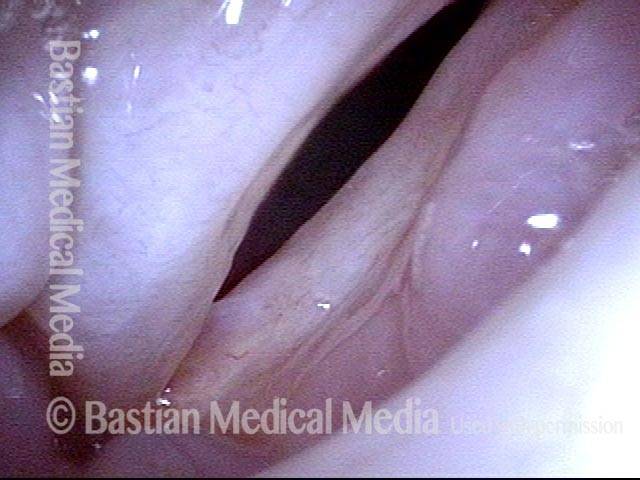
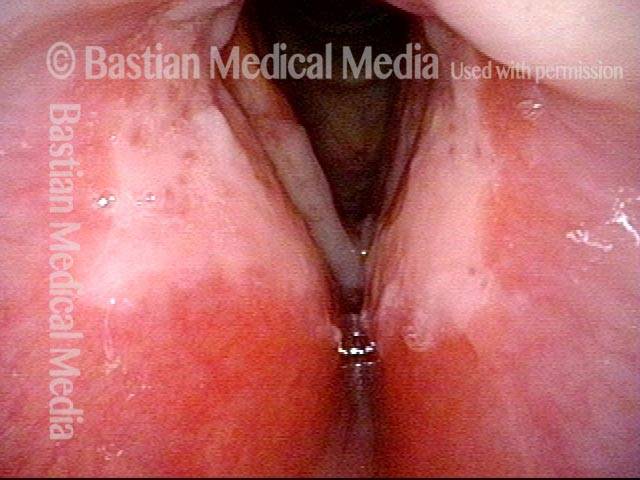
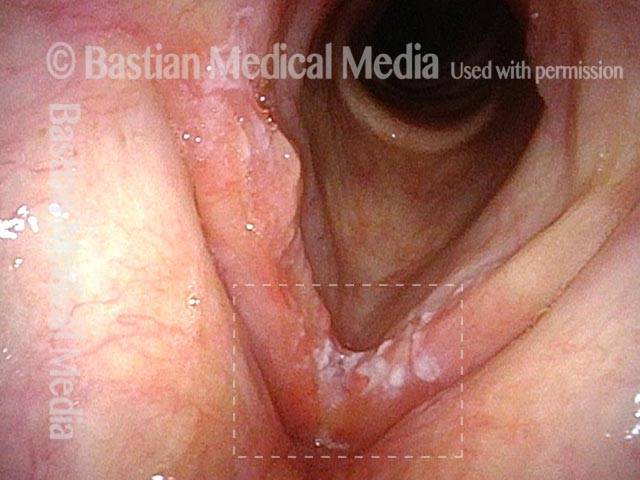
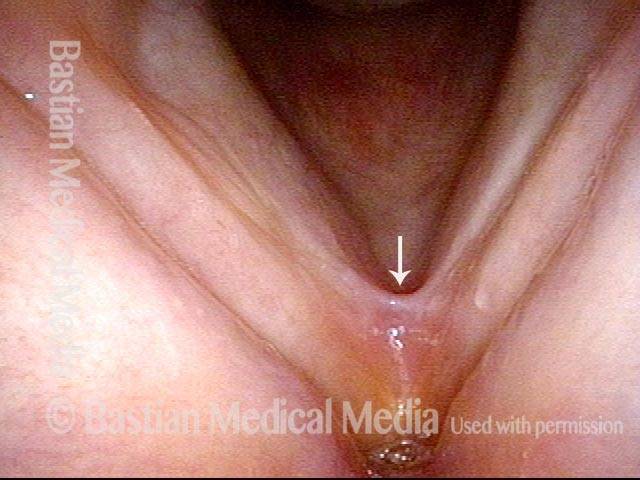
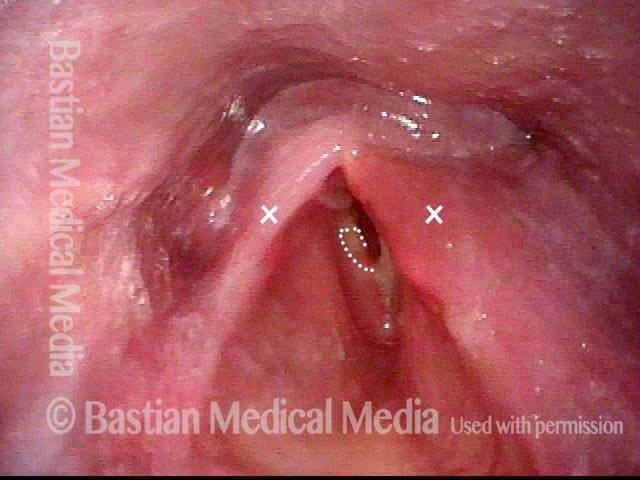
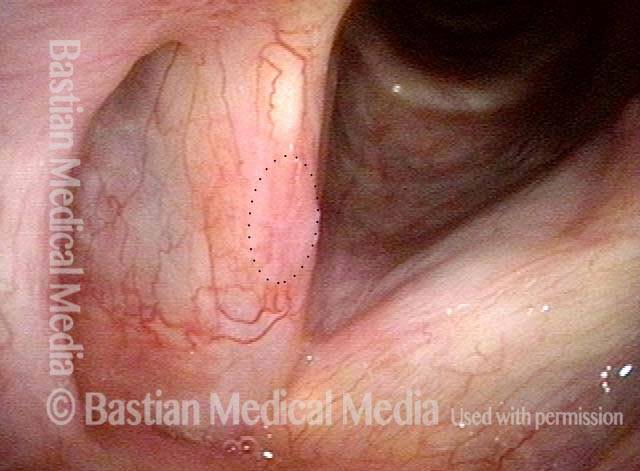
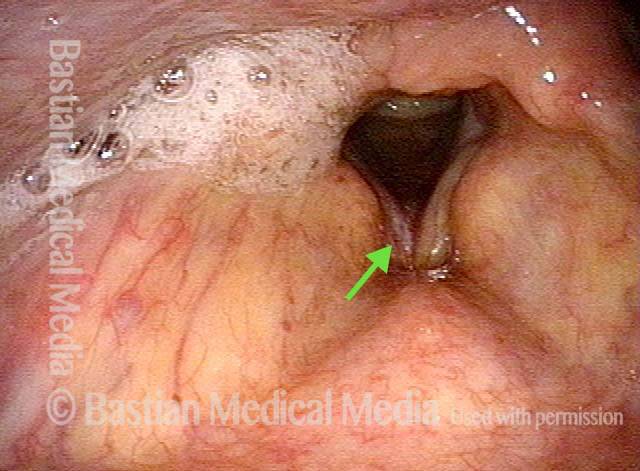
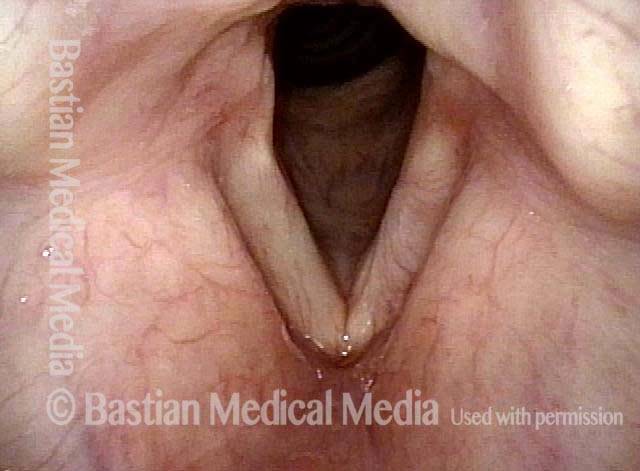
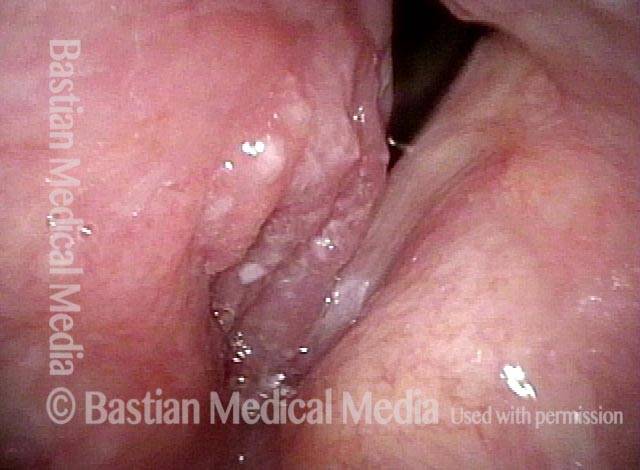
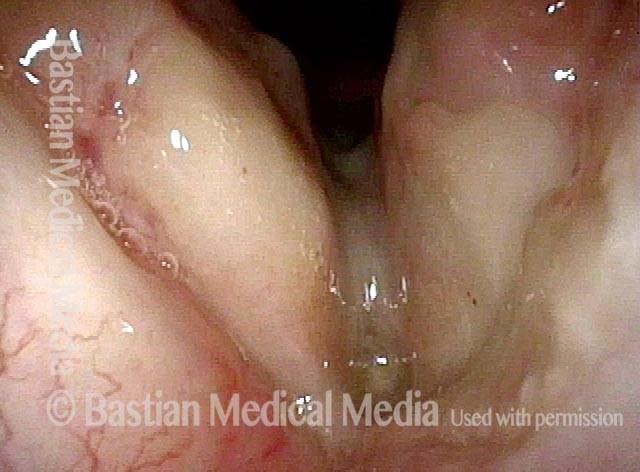
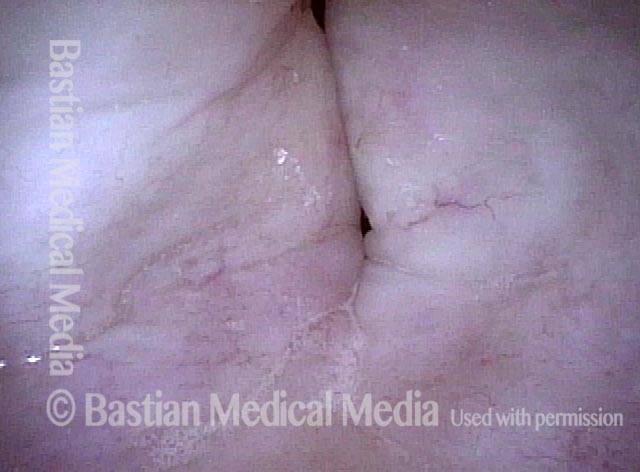
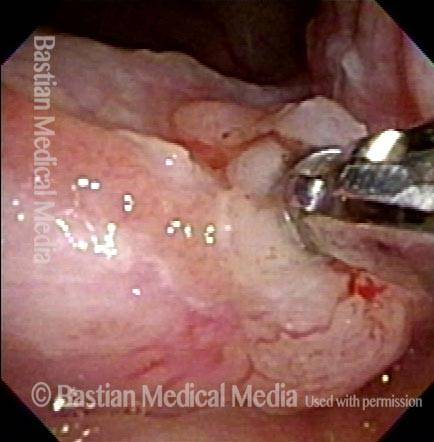
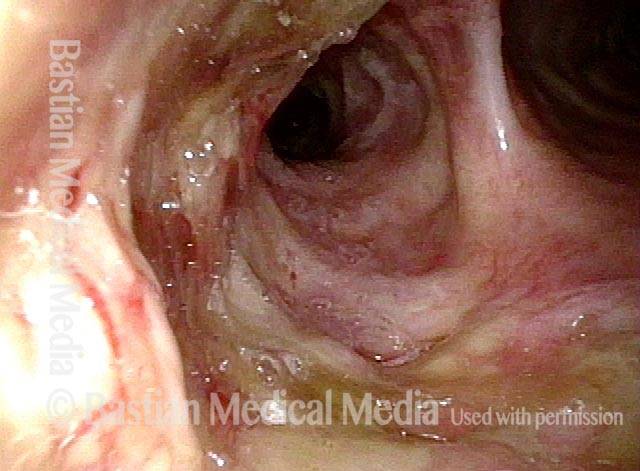
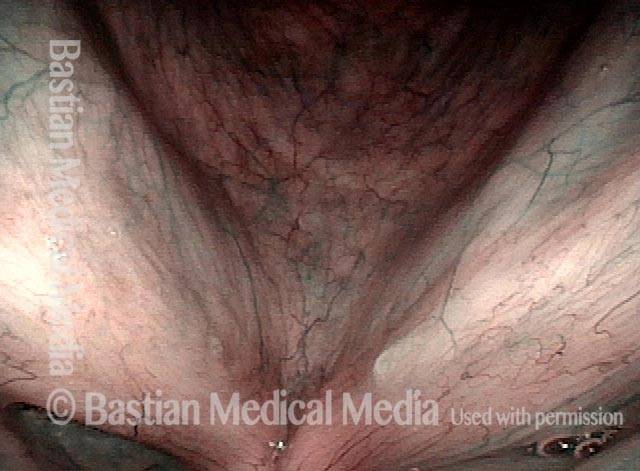
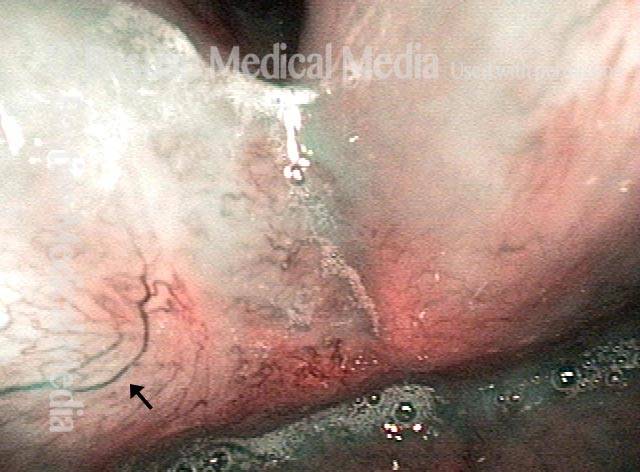
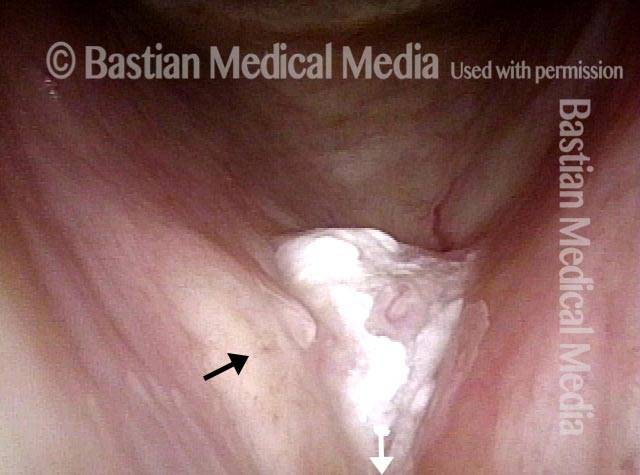
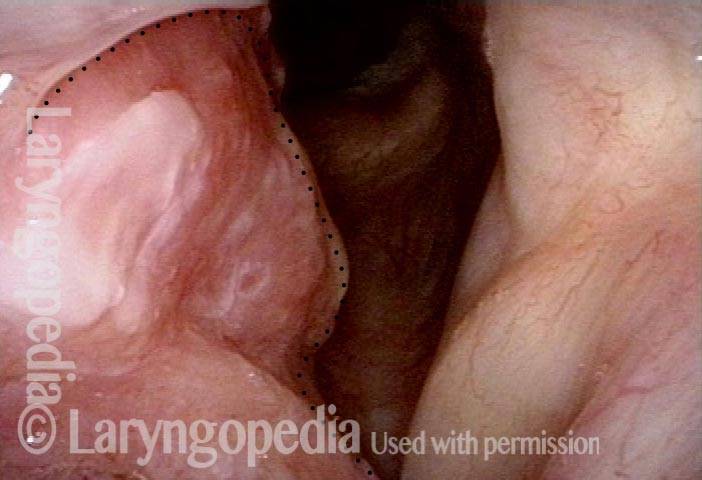
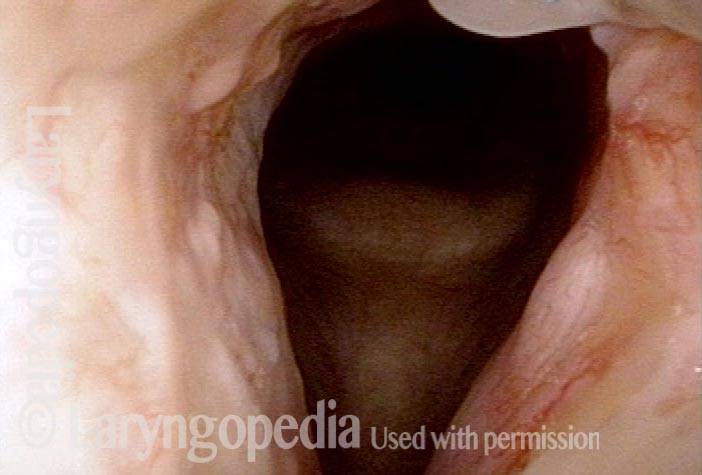
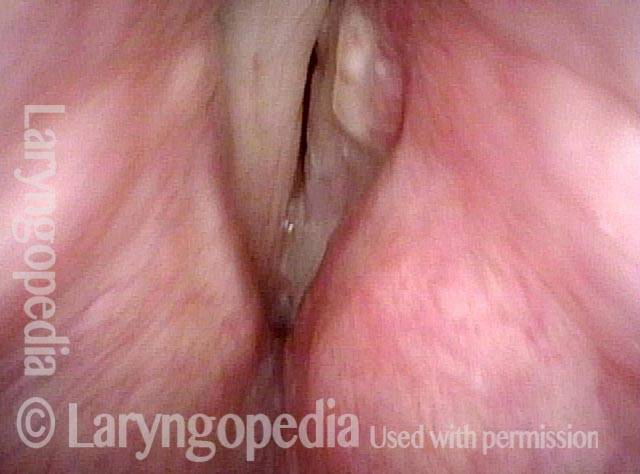
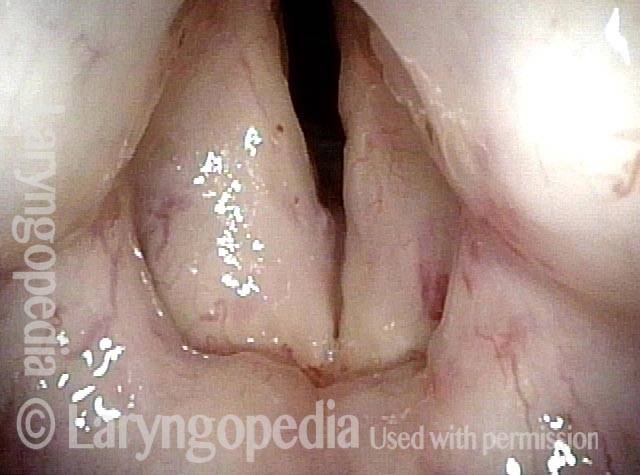
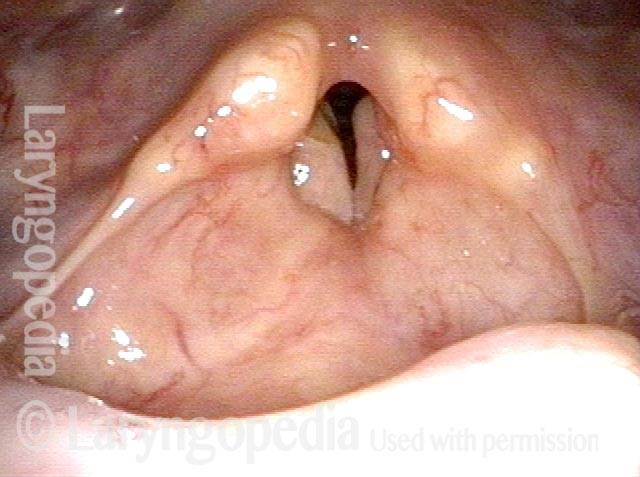
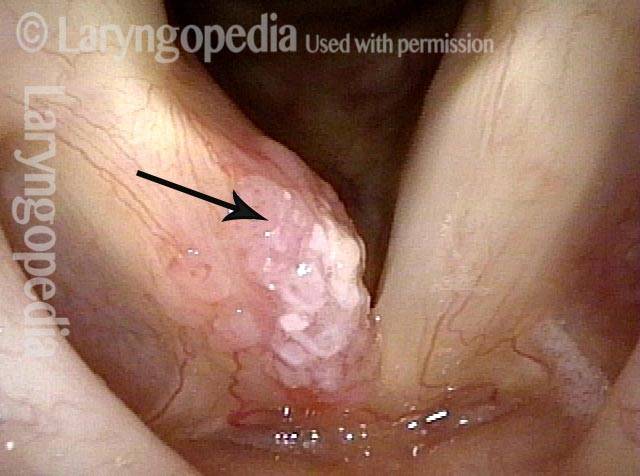
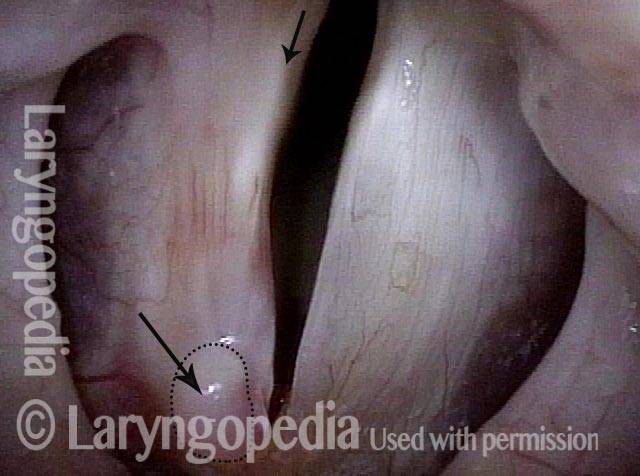
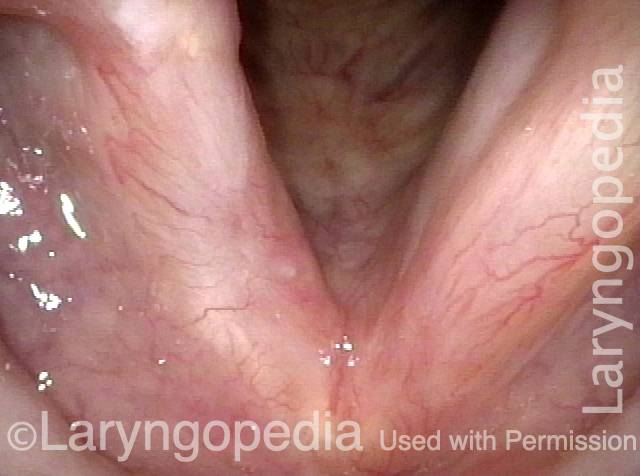
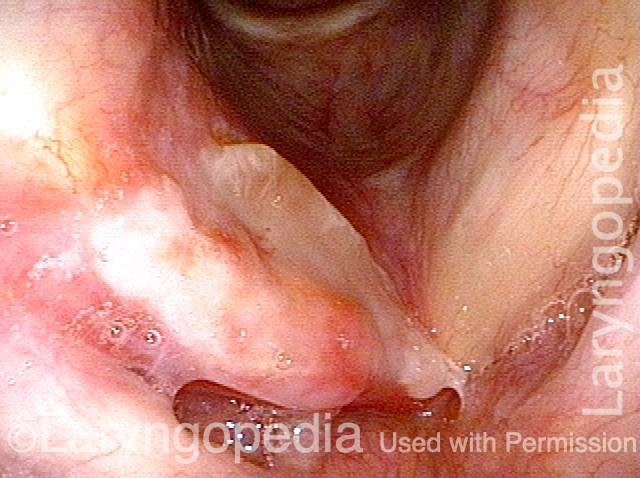
Vocal cord cancer (1 of 10)
Vocal cord cancer (1 of 10)
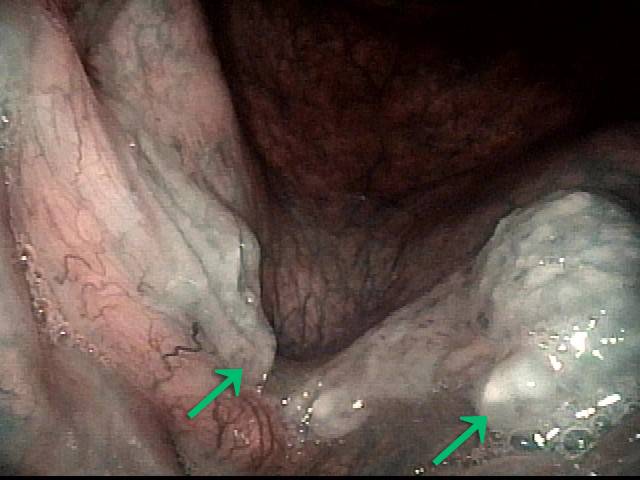
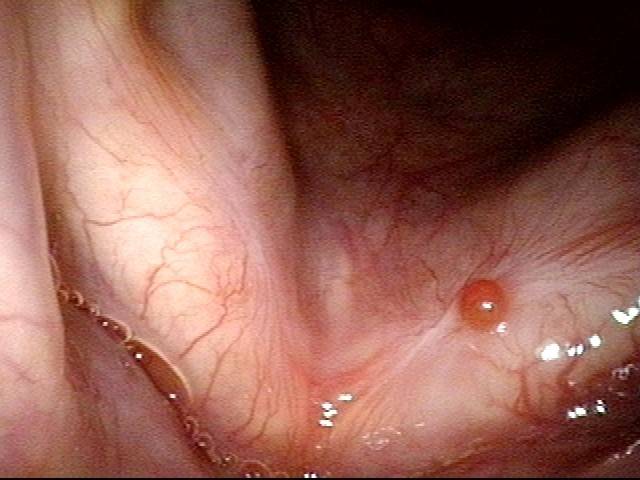
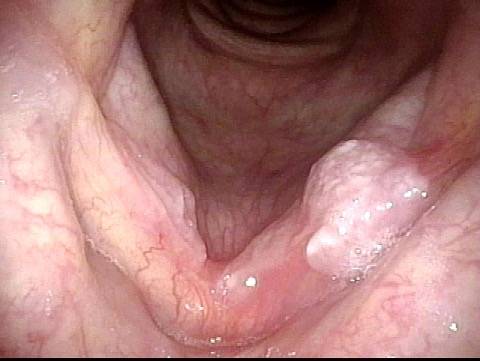
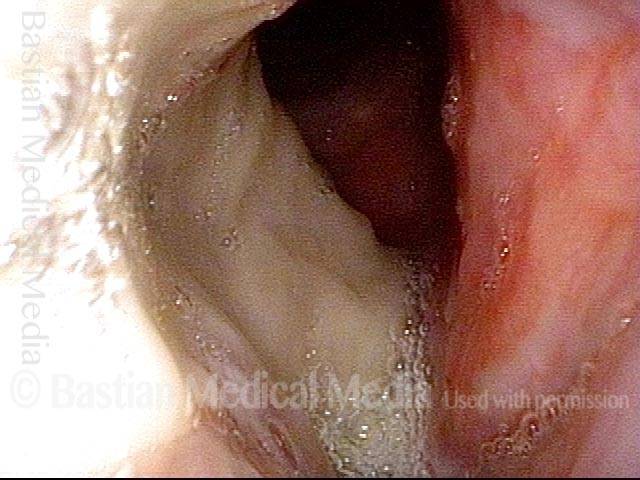
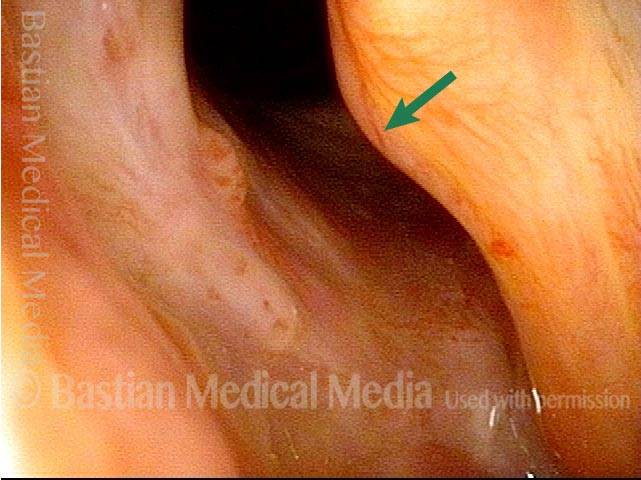
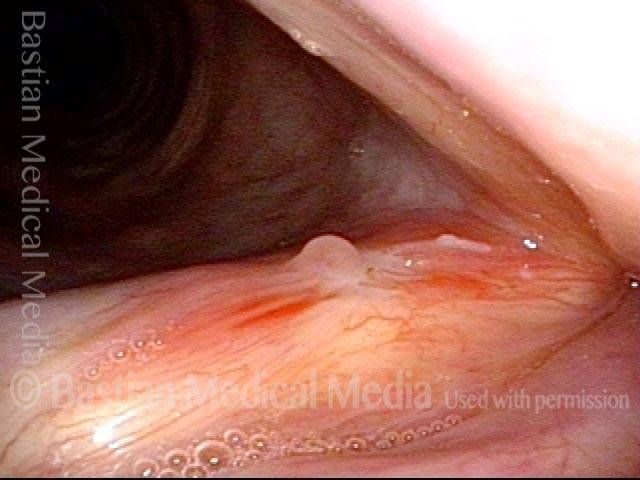
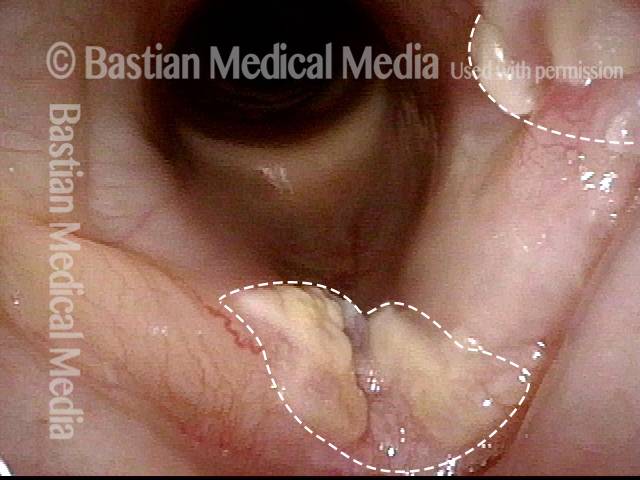
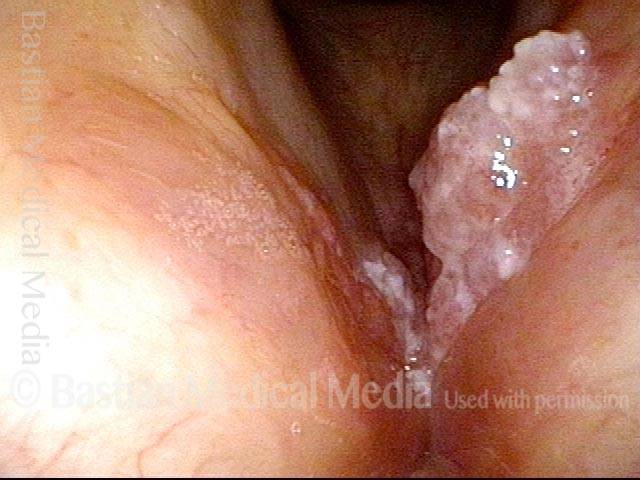
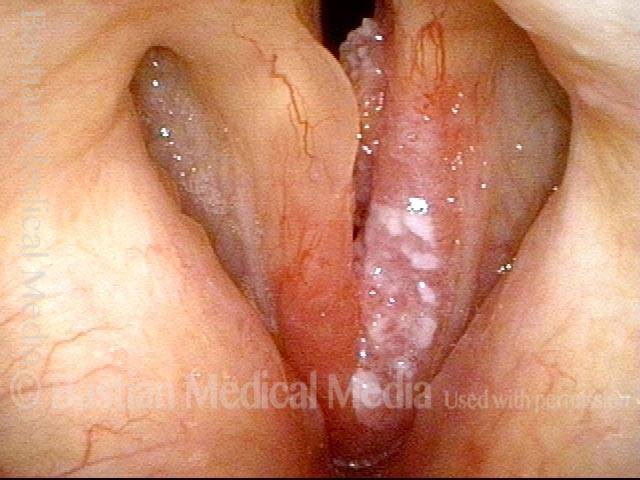
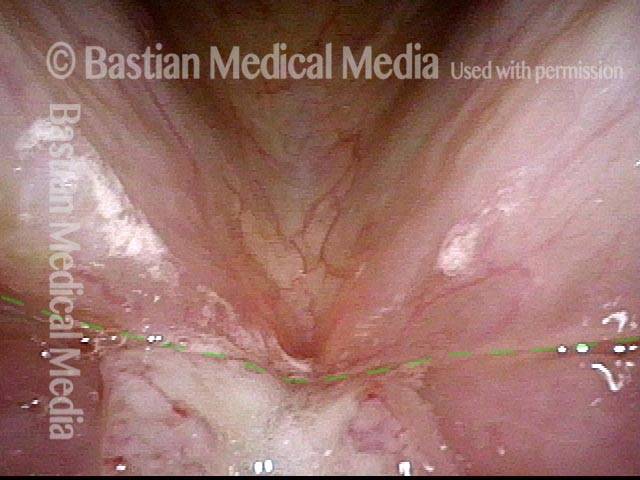
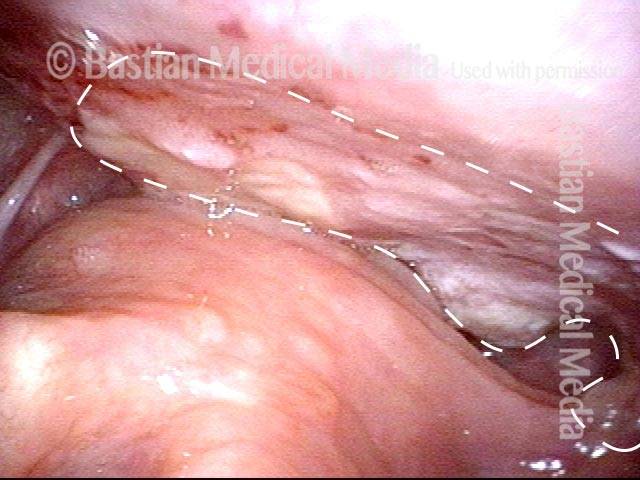
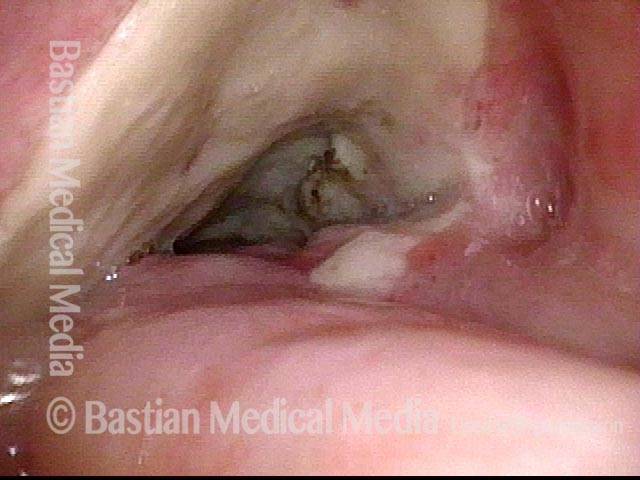
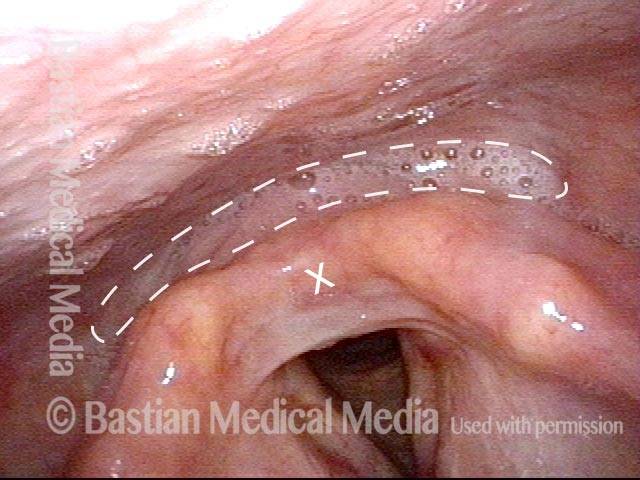
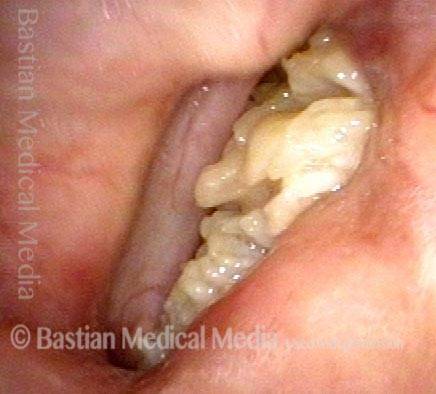
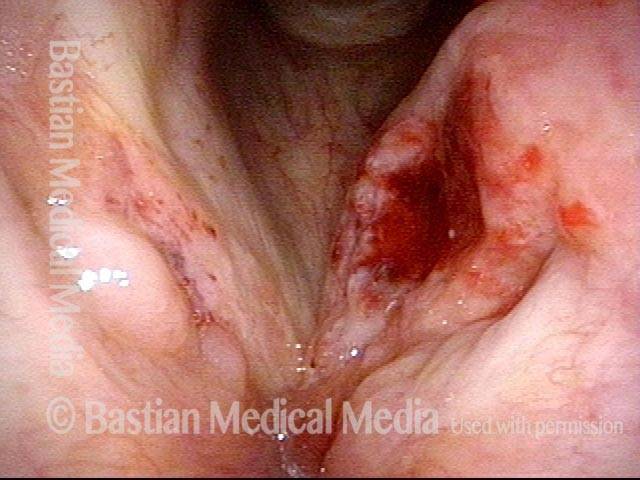
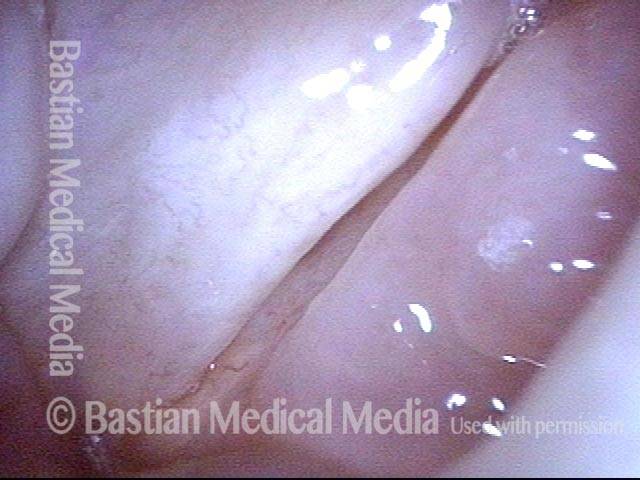
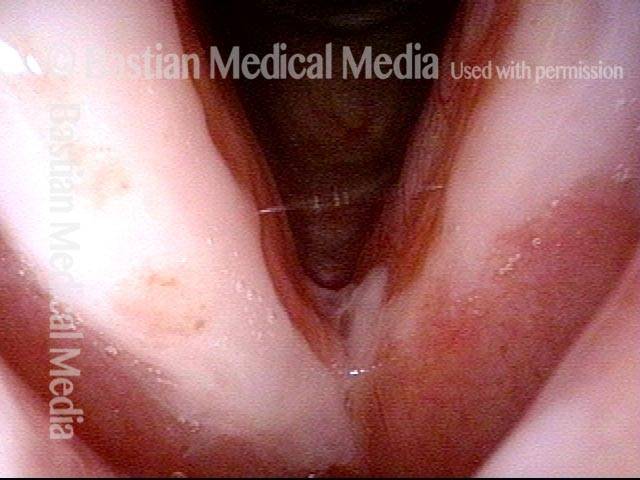
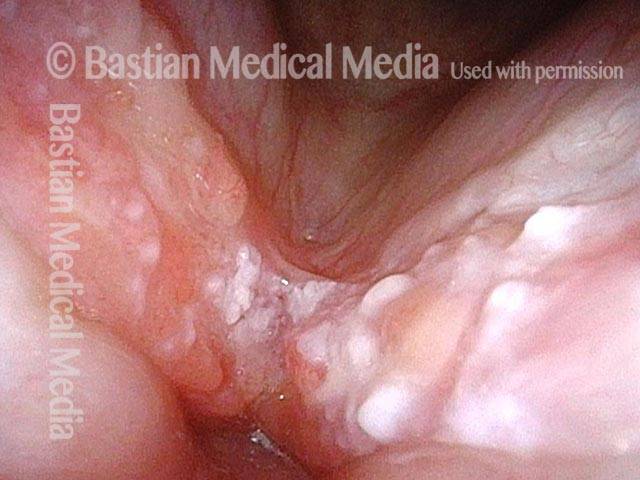
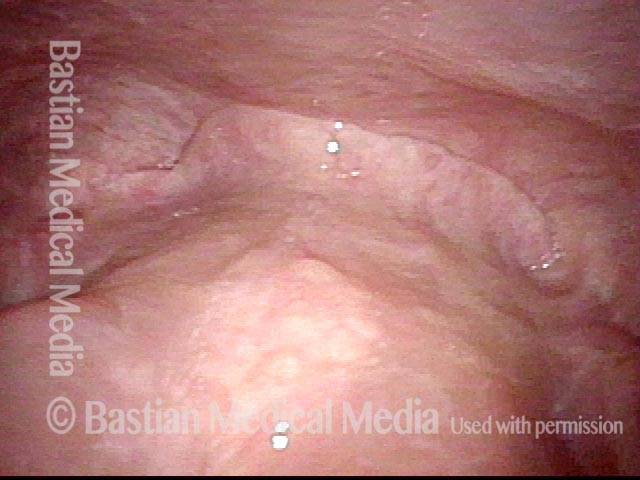
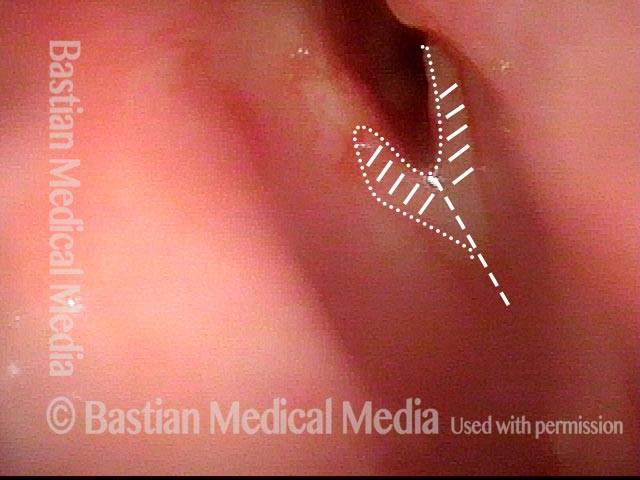
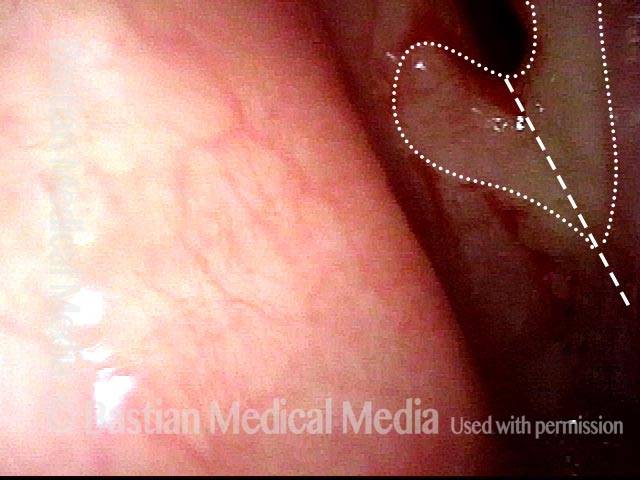
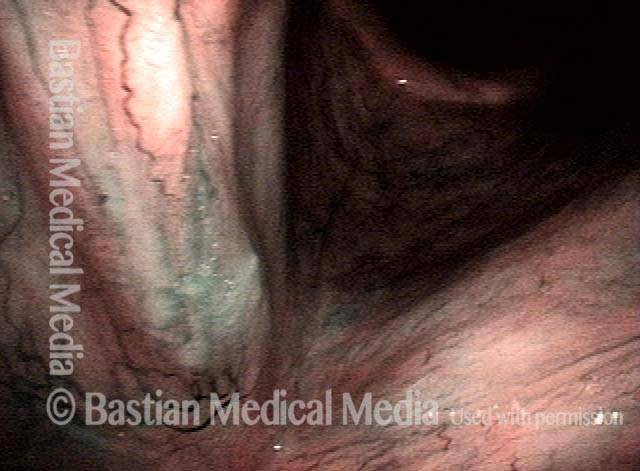
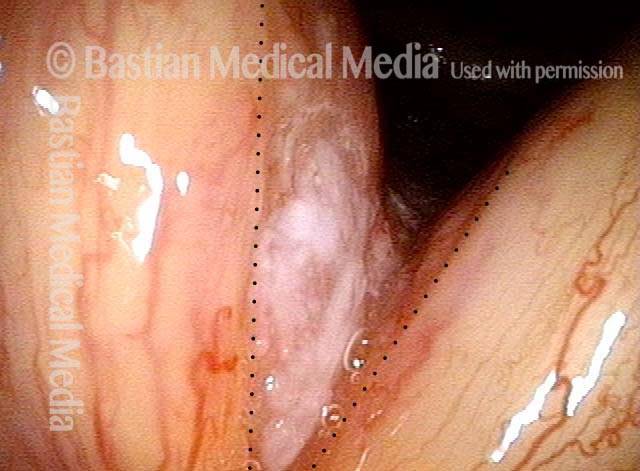
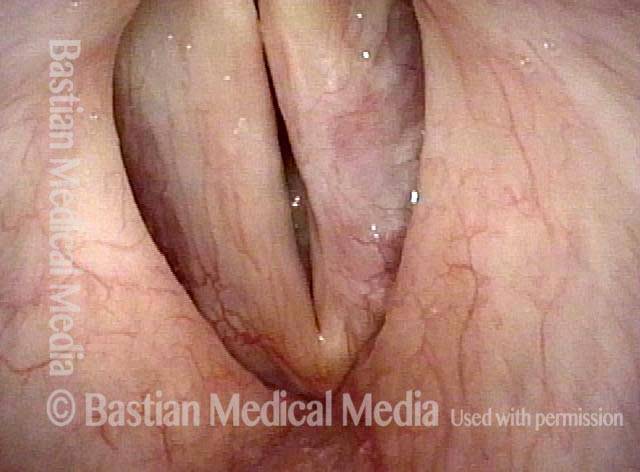
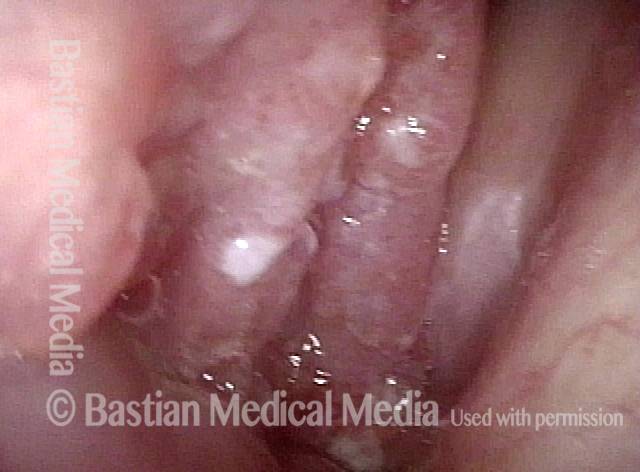
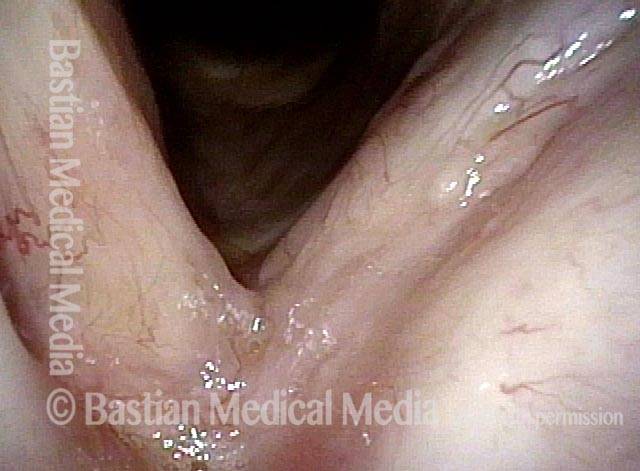
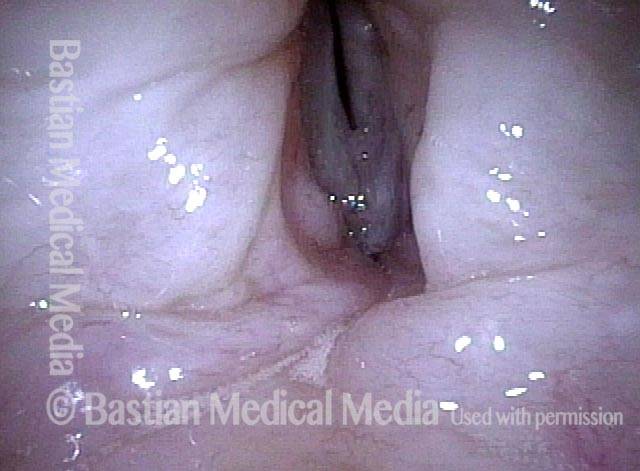
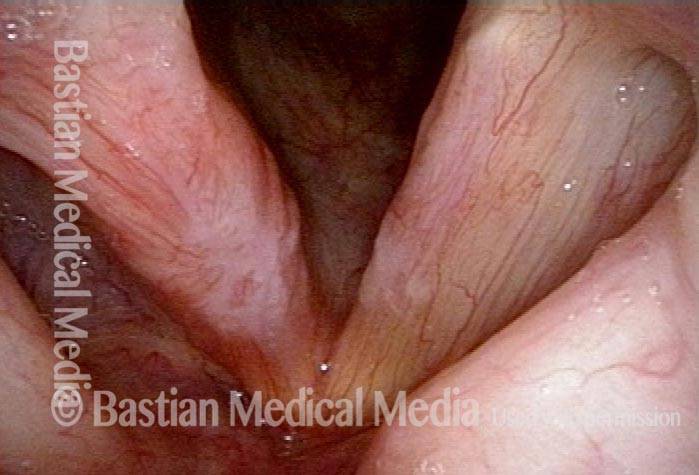
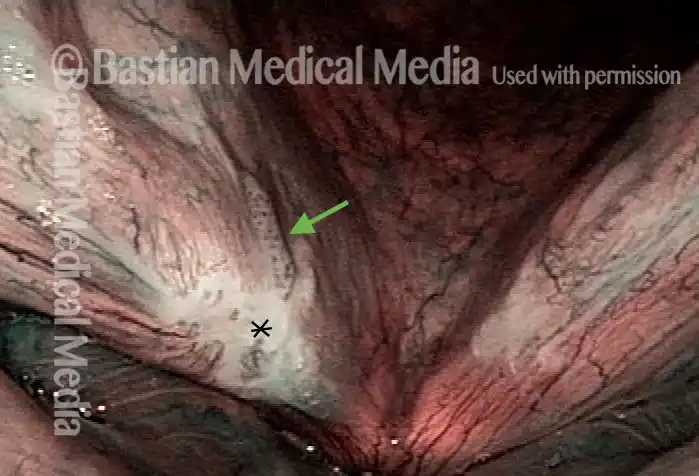
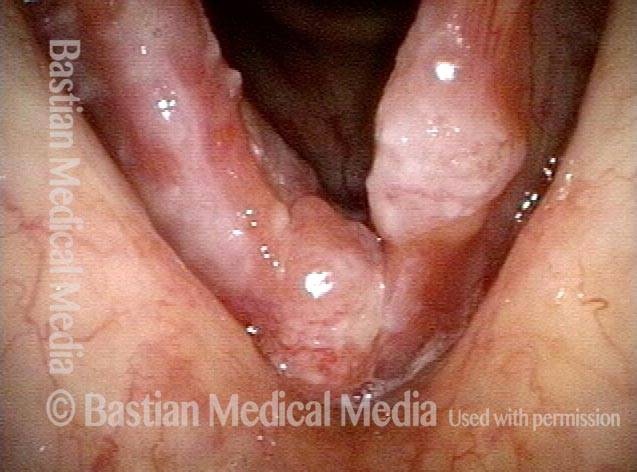
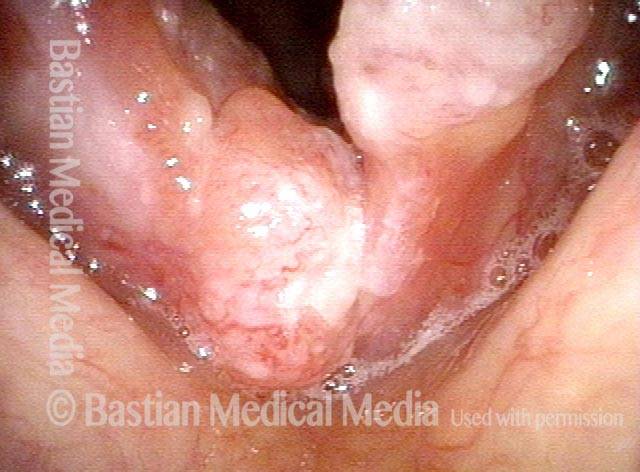
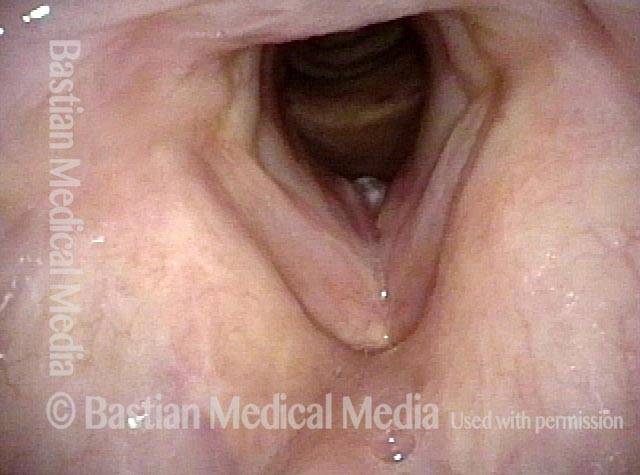
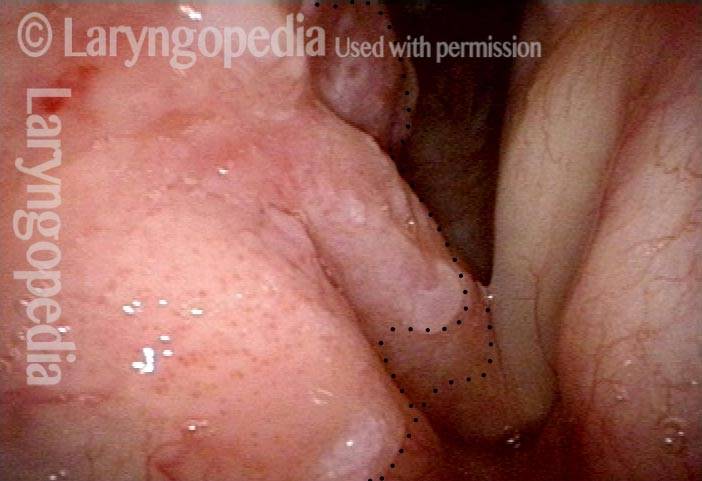
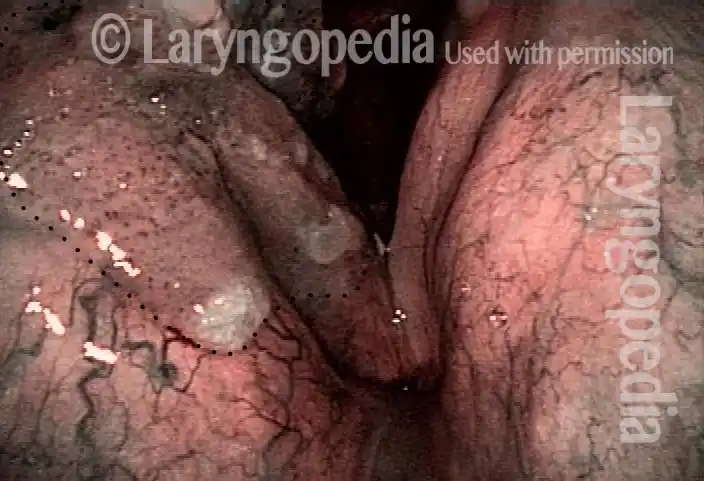
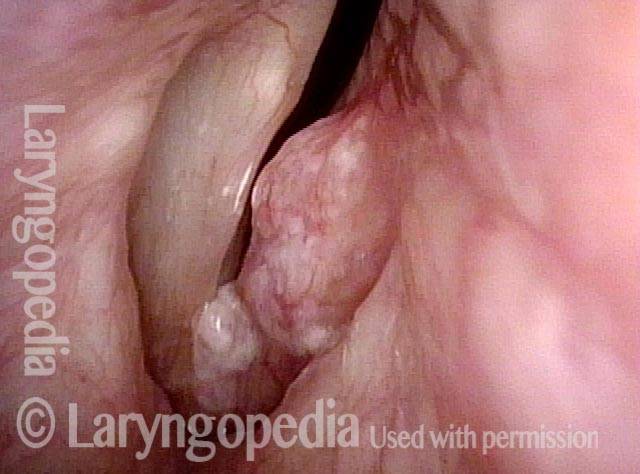
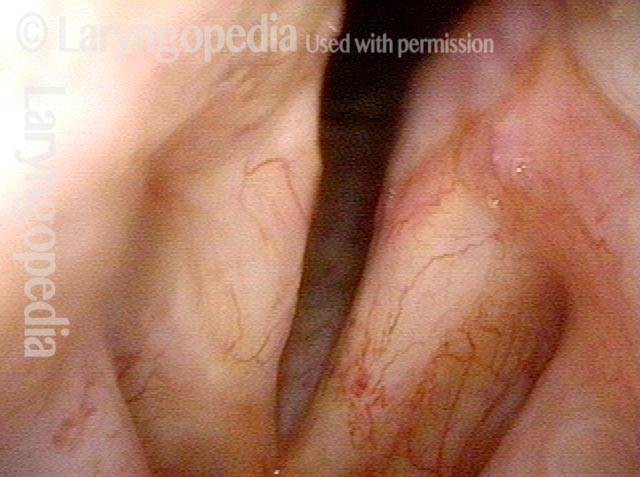
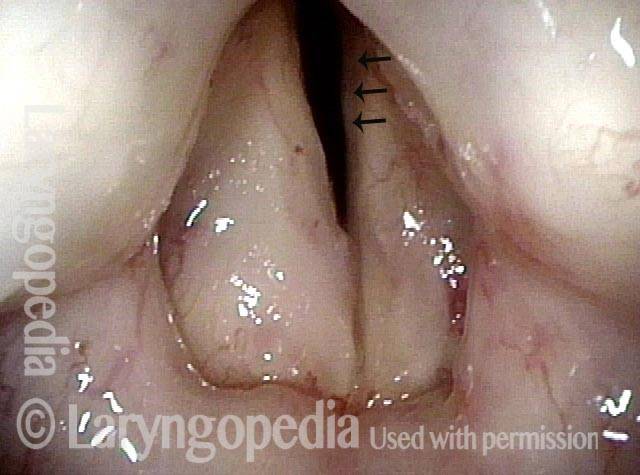
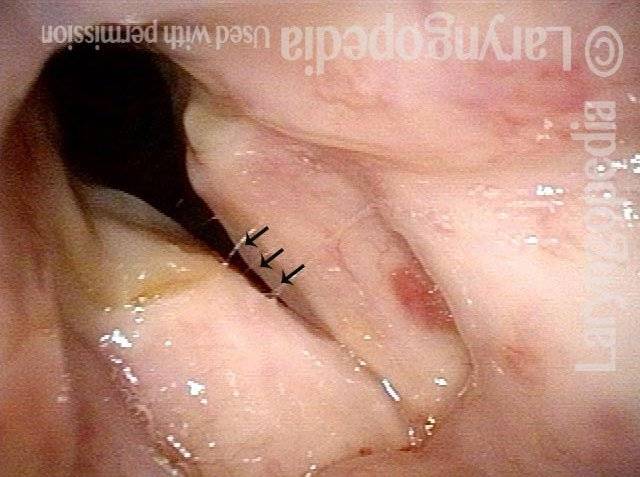
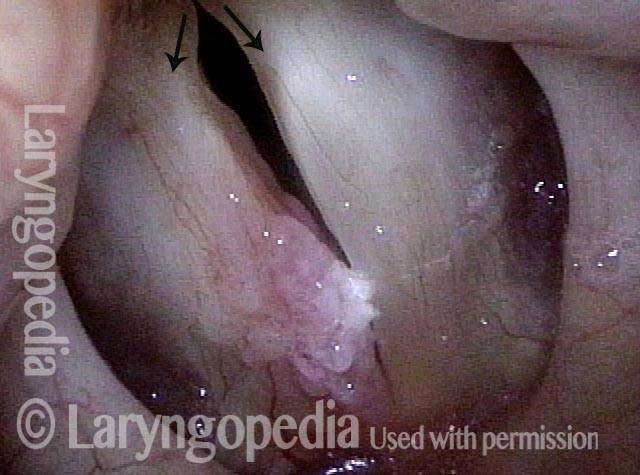
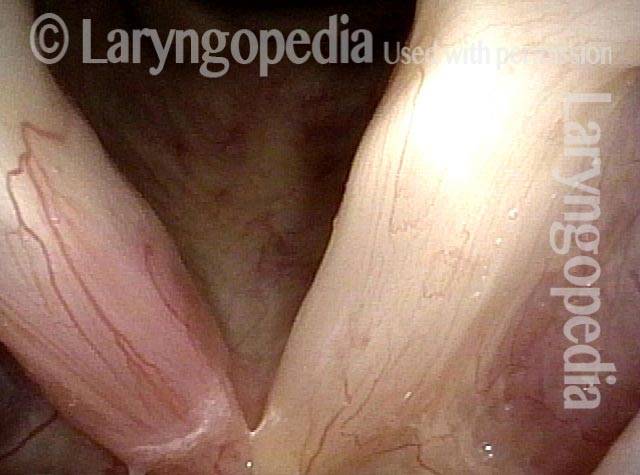
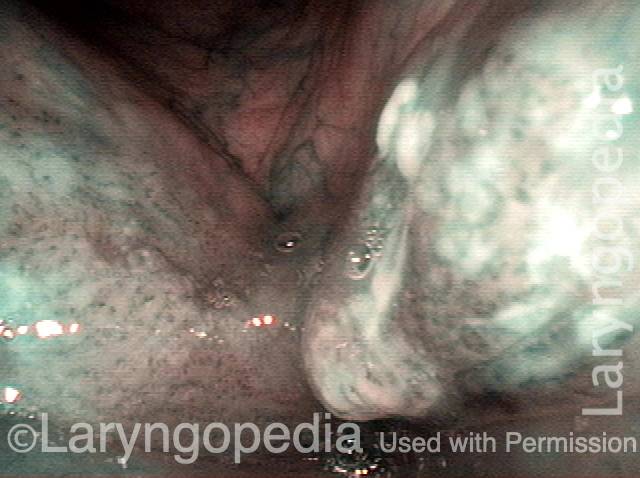
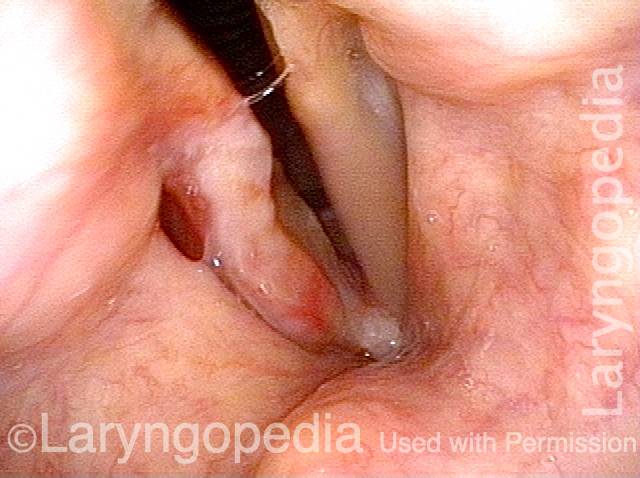
Stippling (2 of 10)
Stippling (2 of 10)
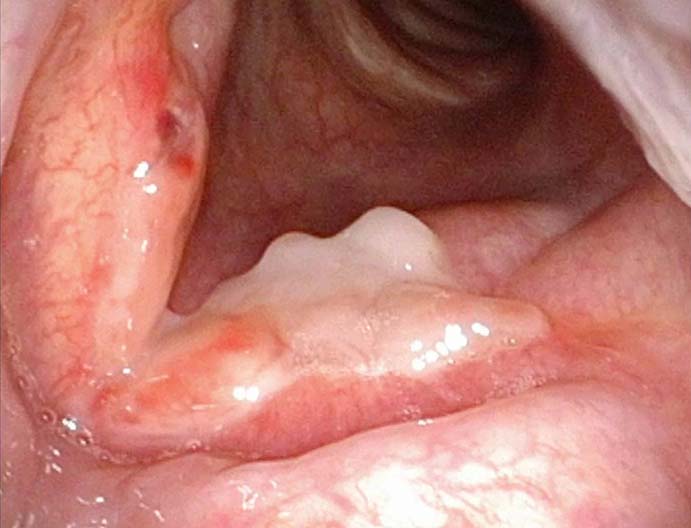
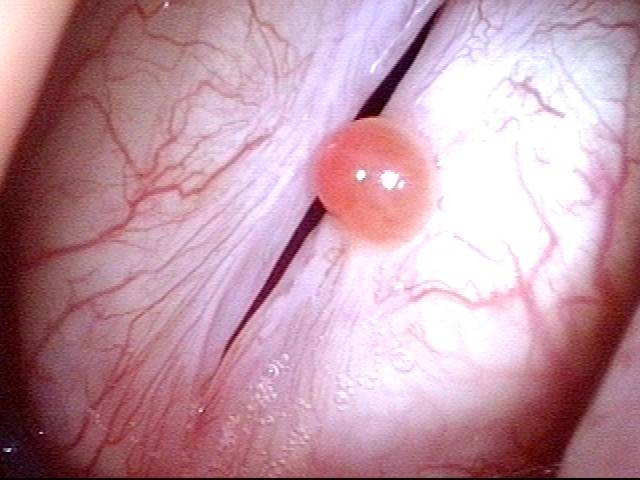
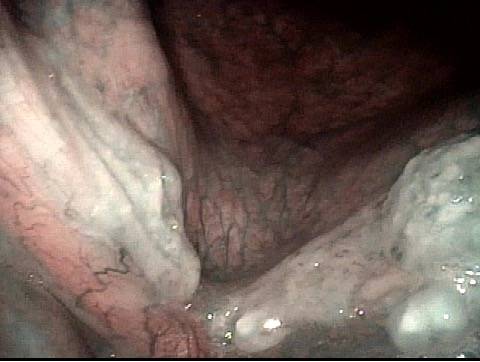
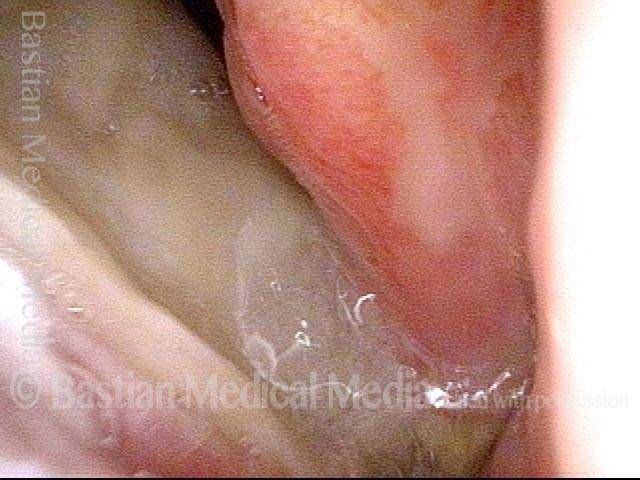
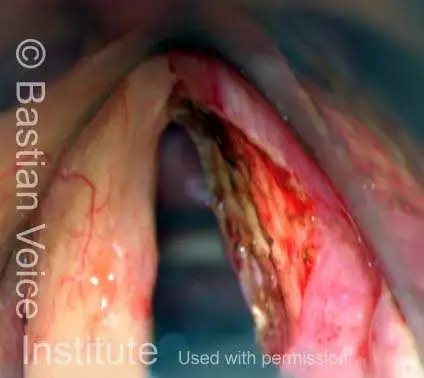
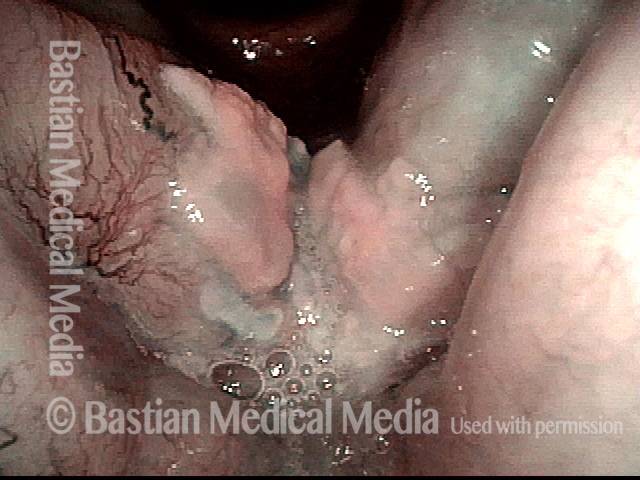
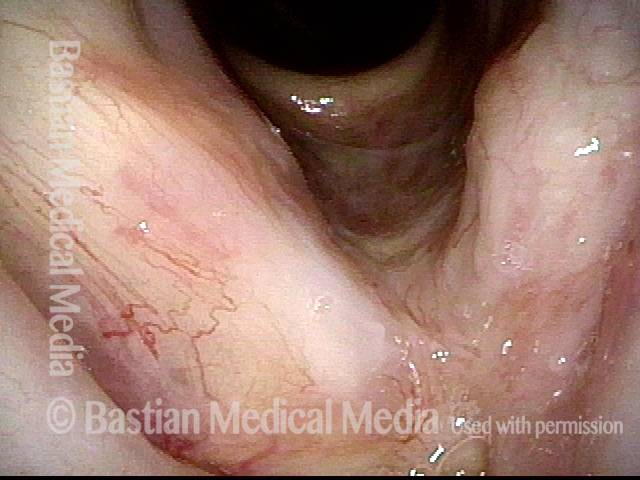
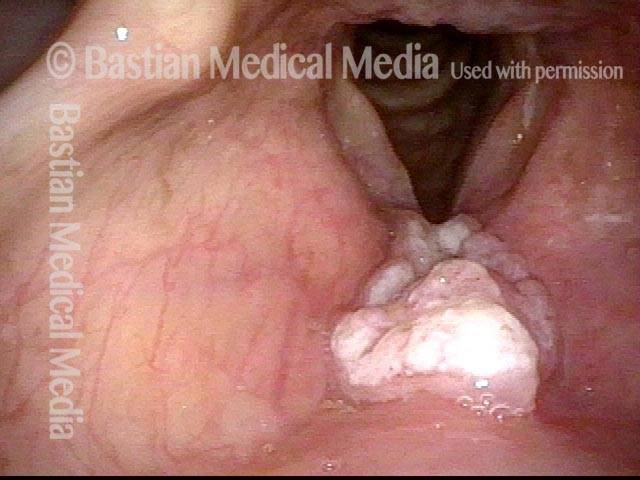
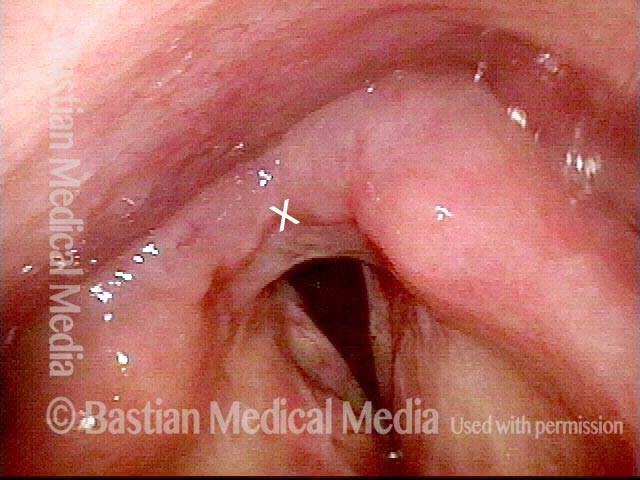
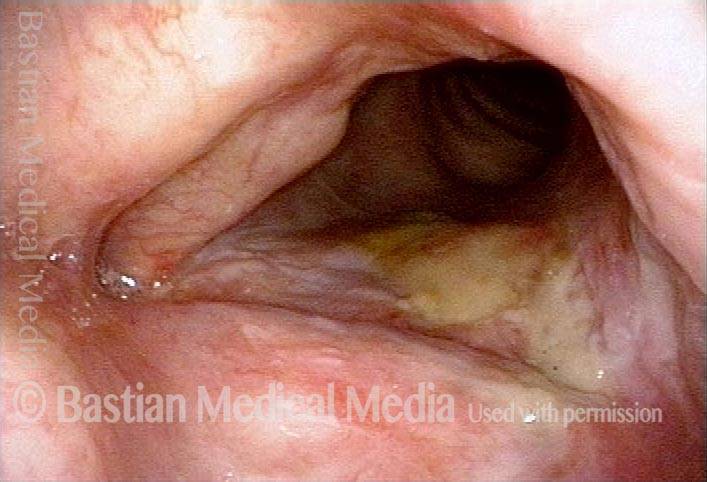
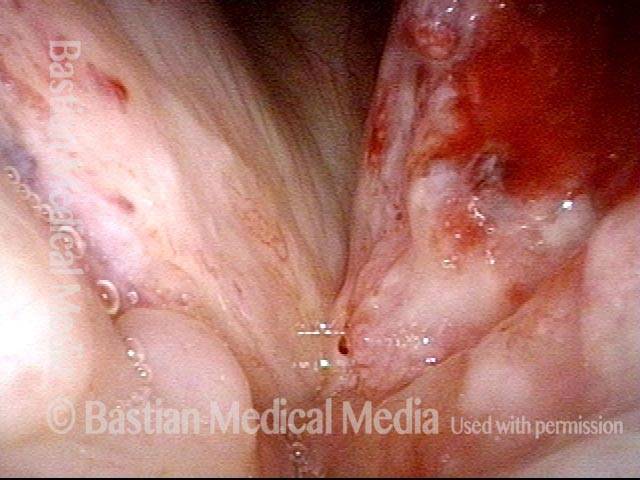
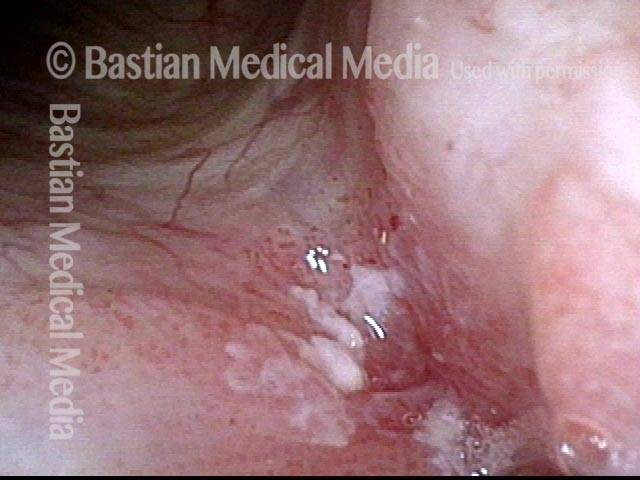
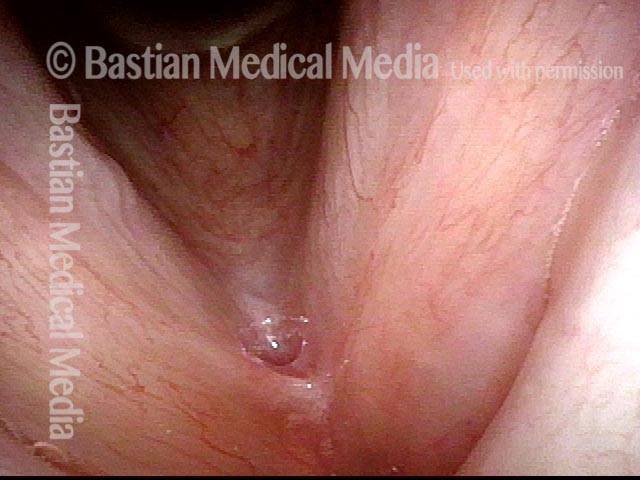
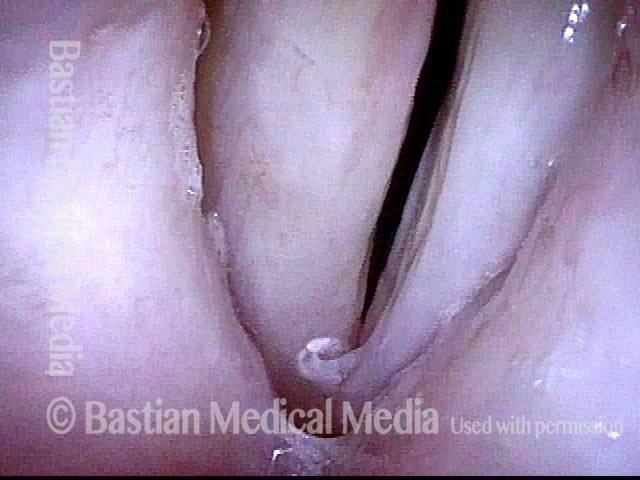
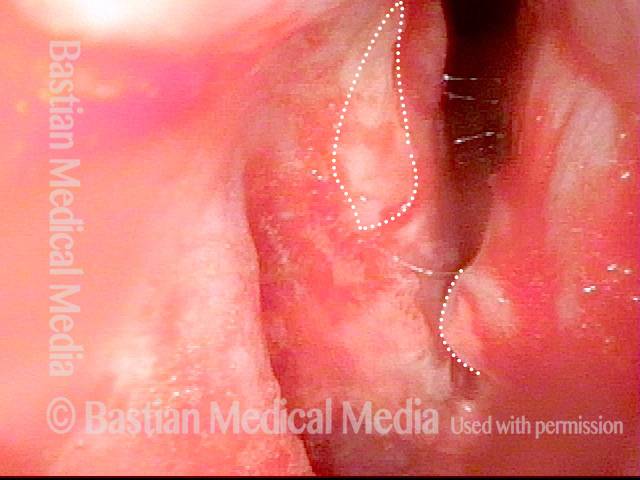
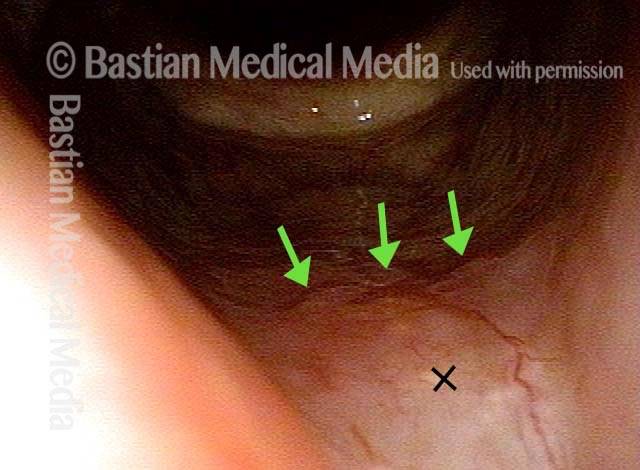
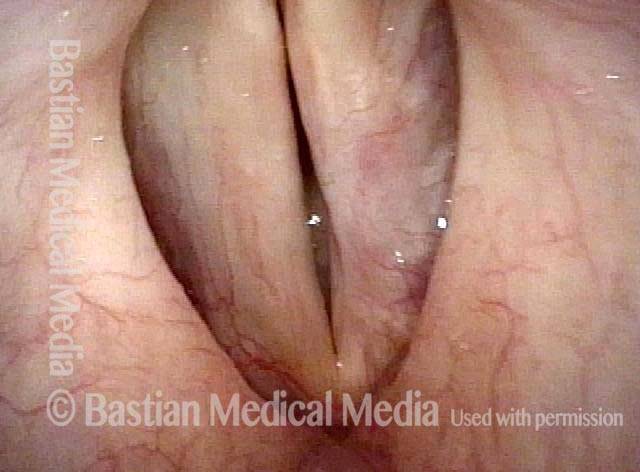
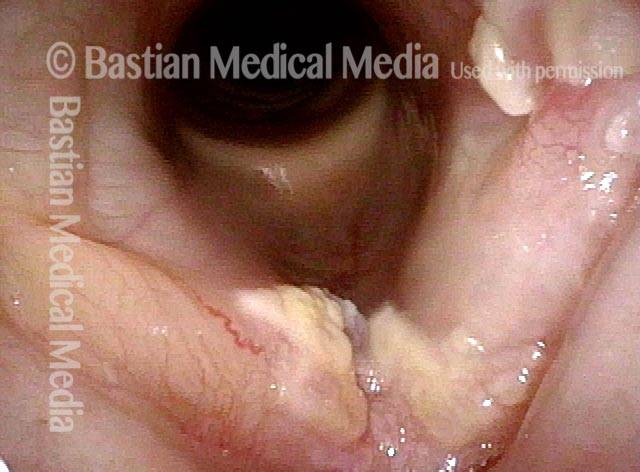
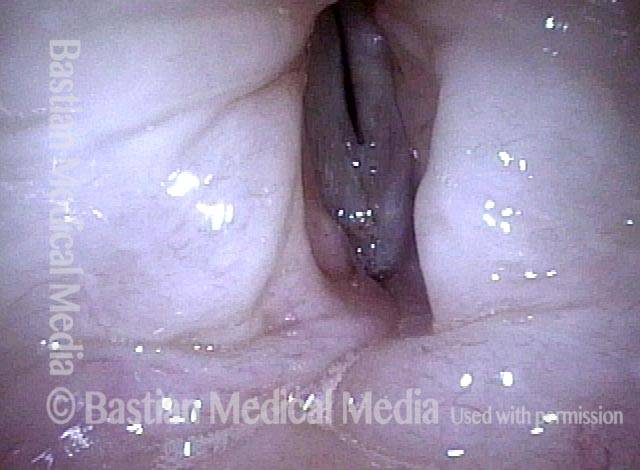
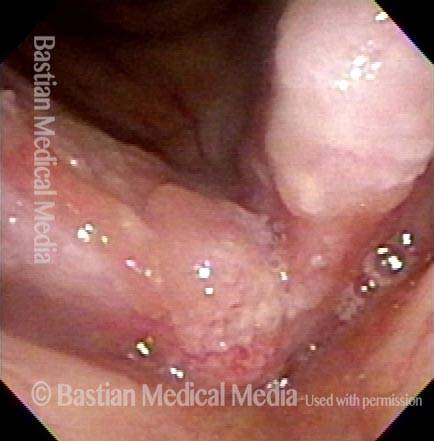
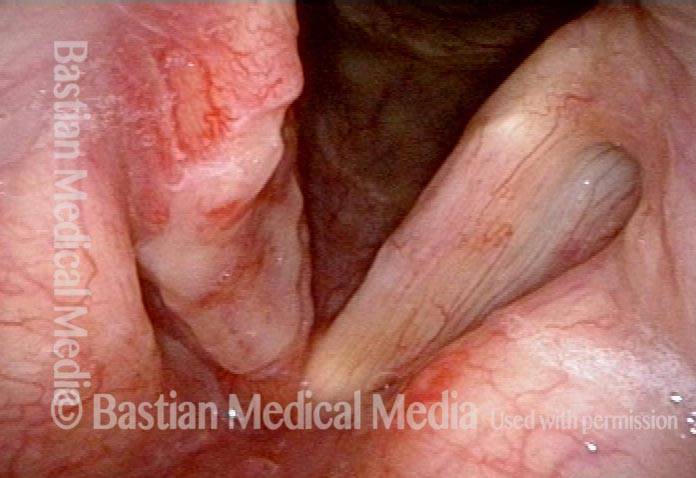
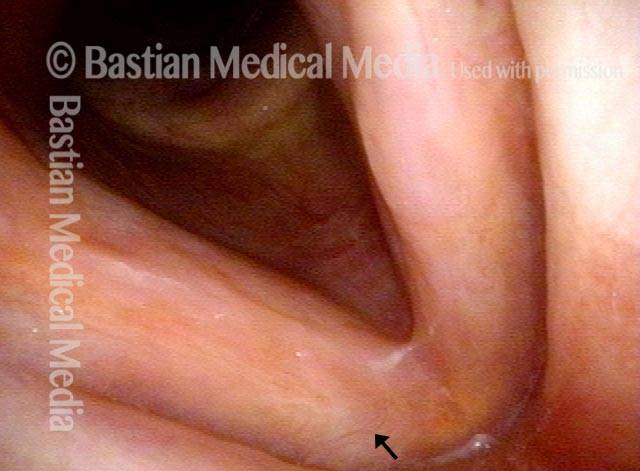
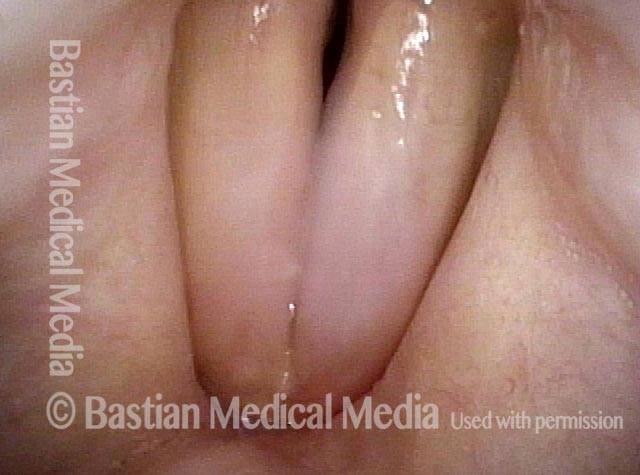
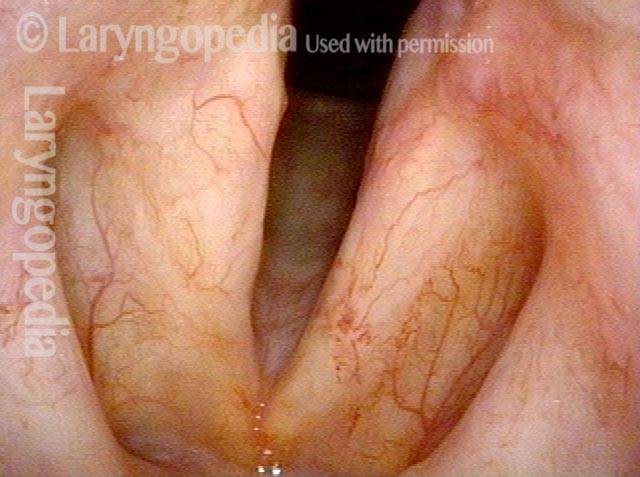
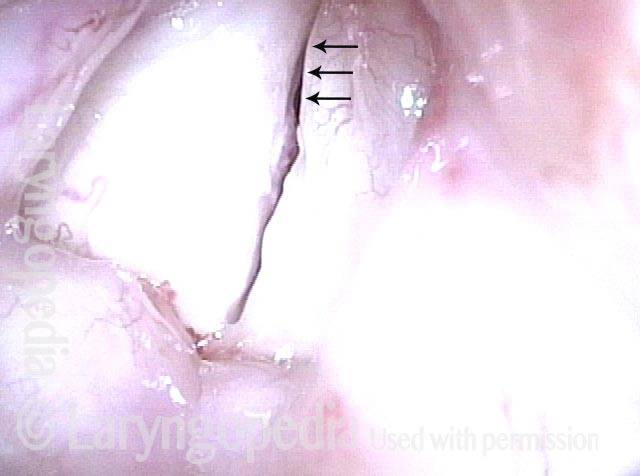
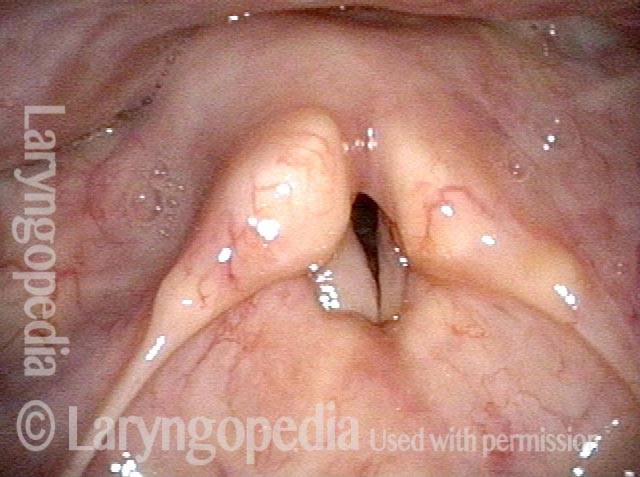
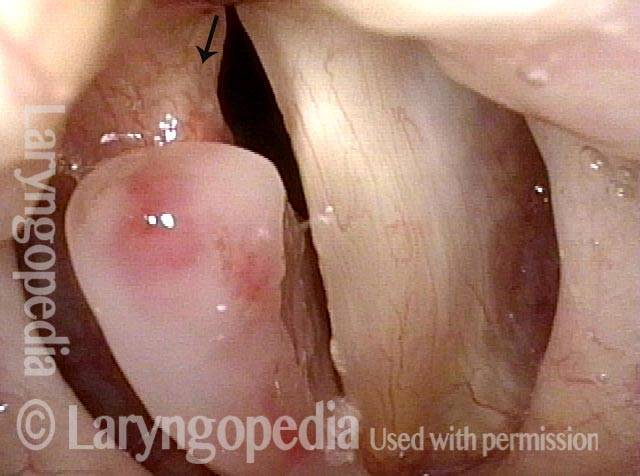
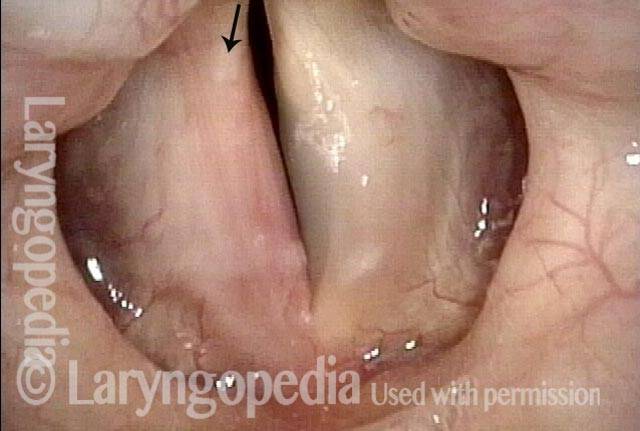
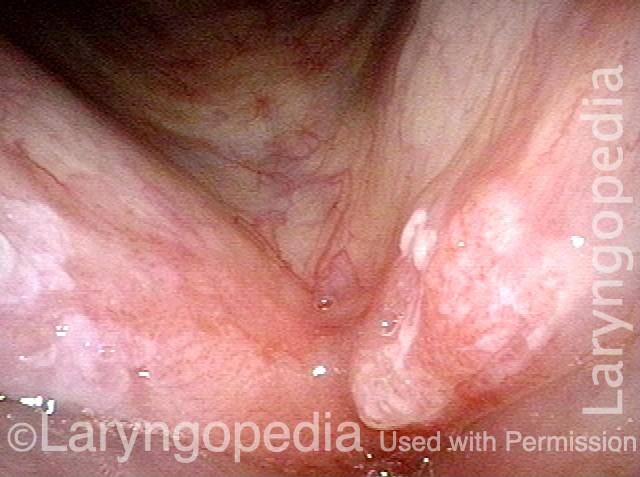
1 week after excision (3 of 10)
1 week after excision (3 of 10)
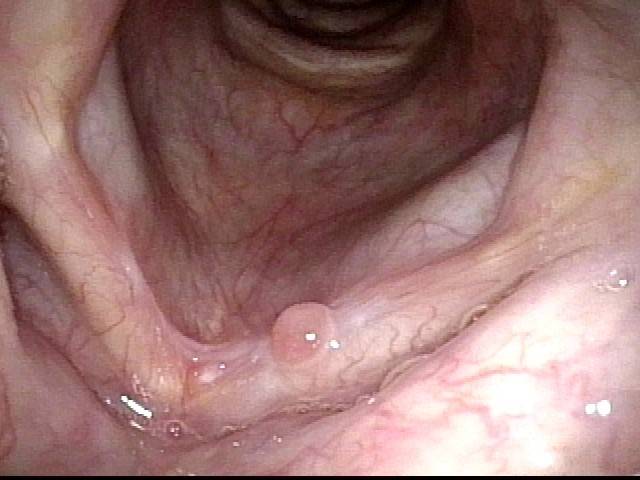
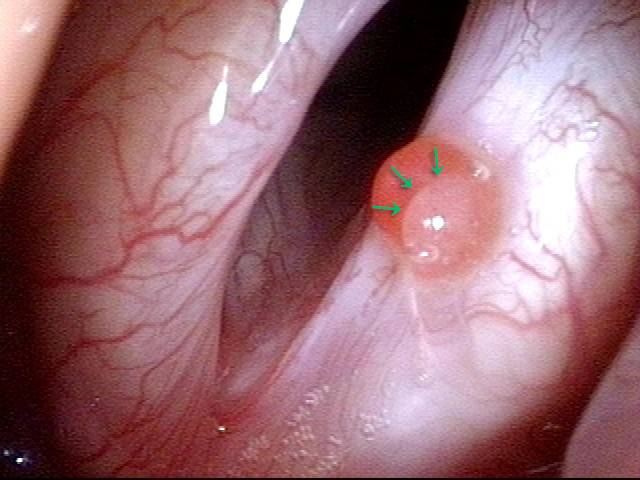
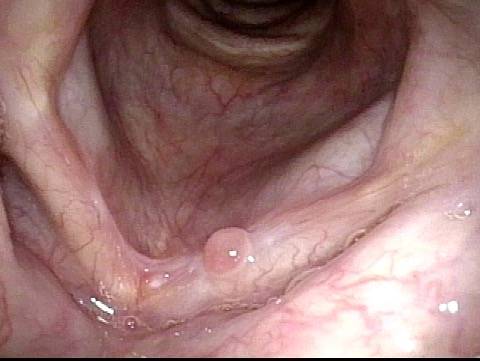
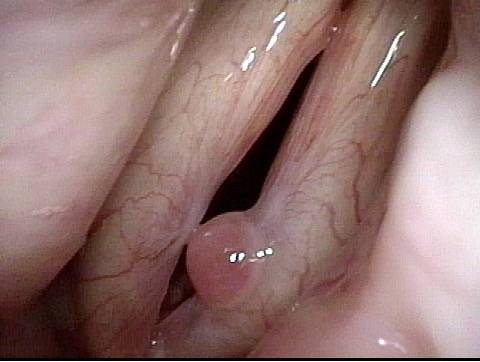
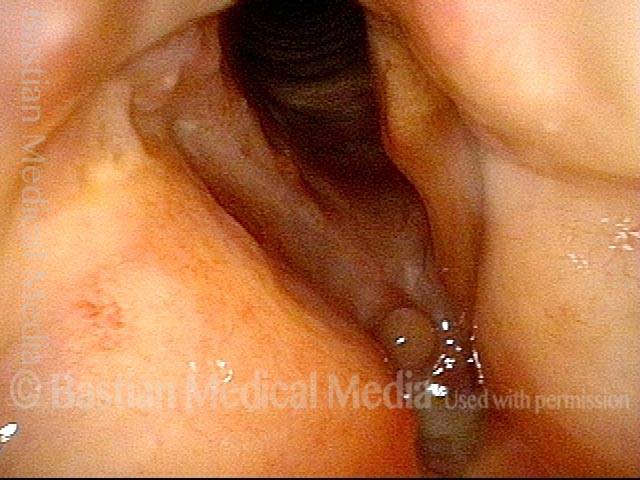
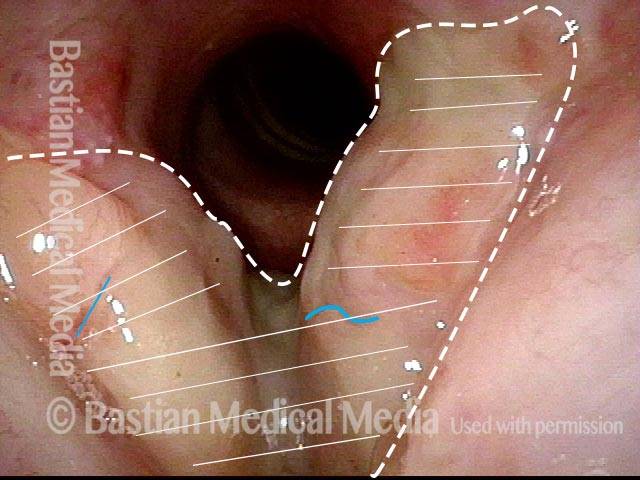
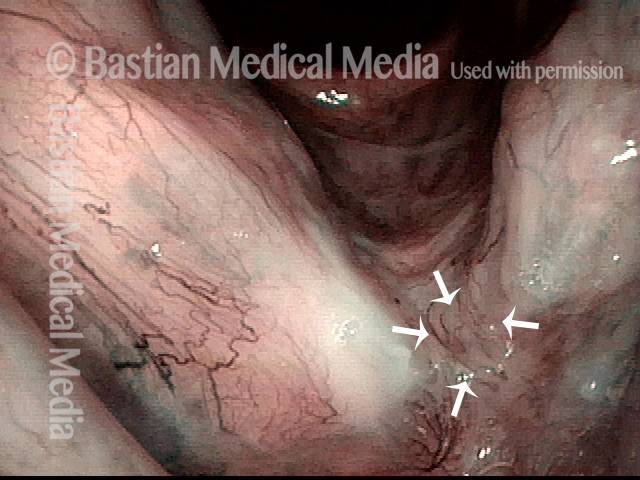
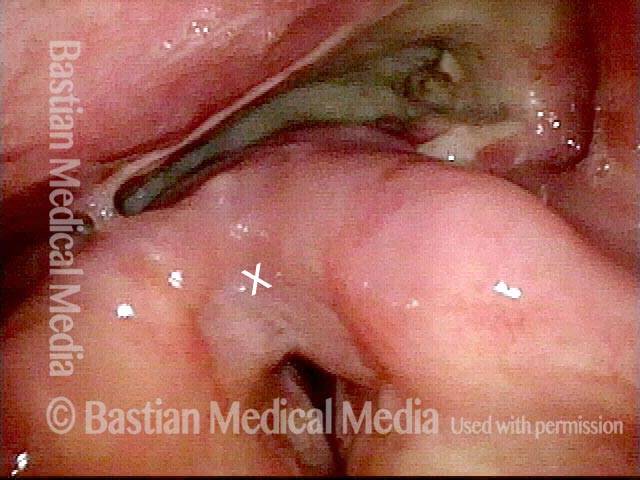
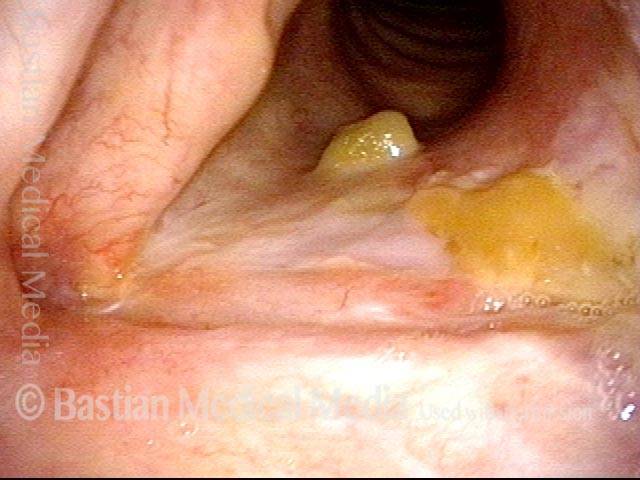
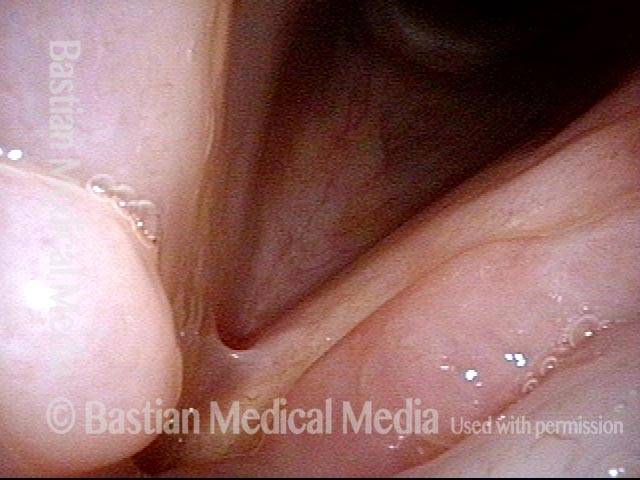
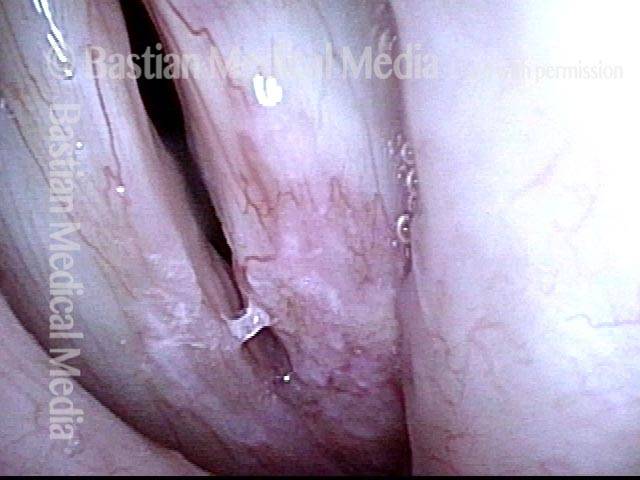
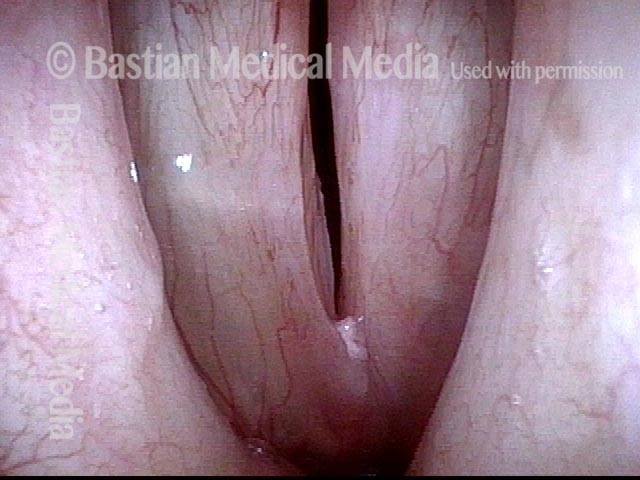
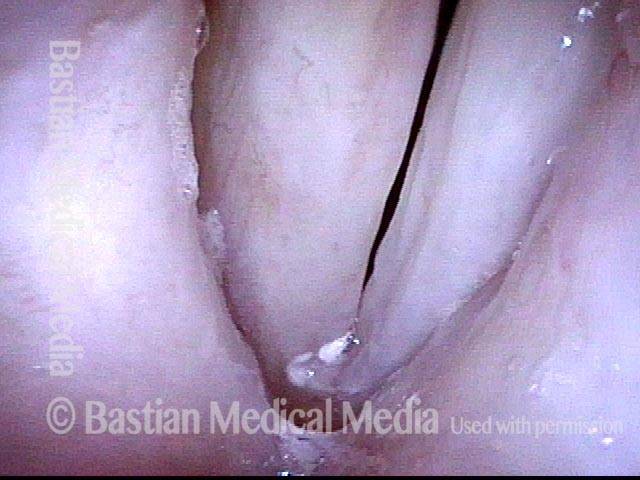
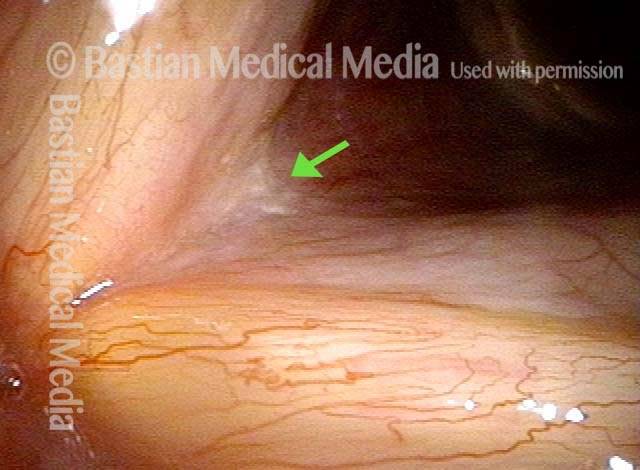
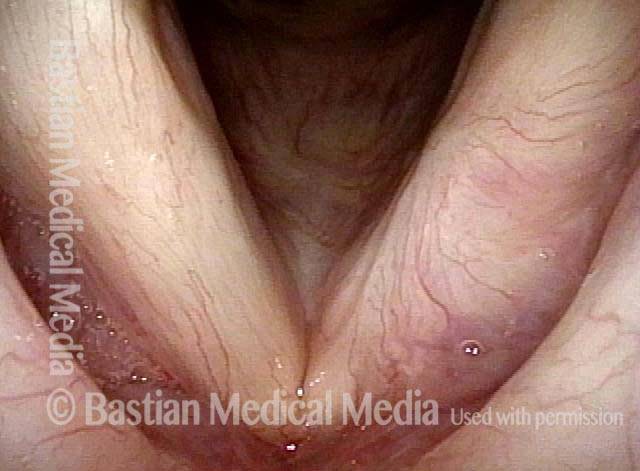
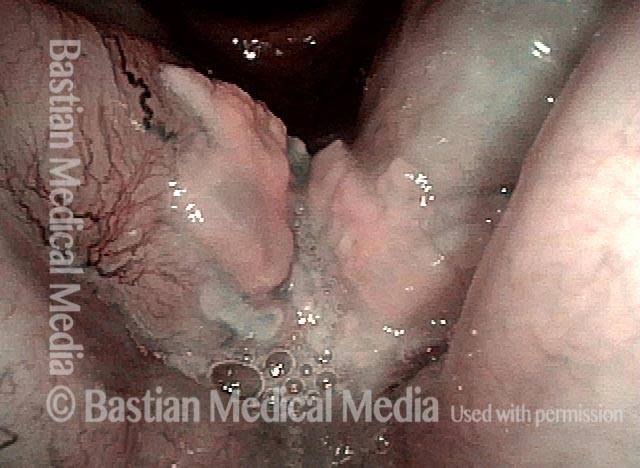
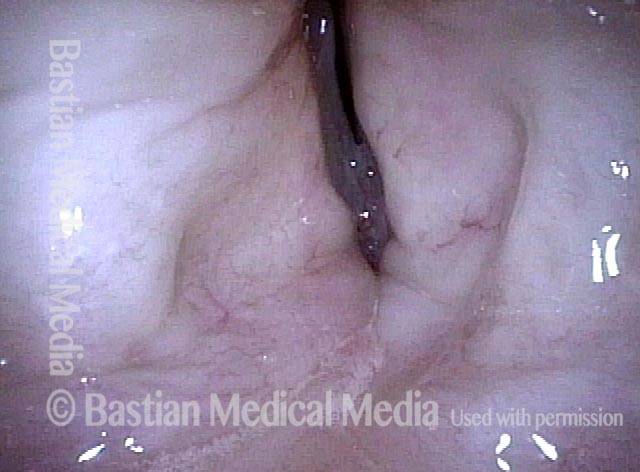
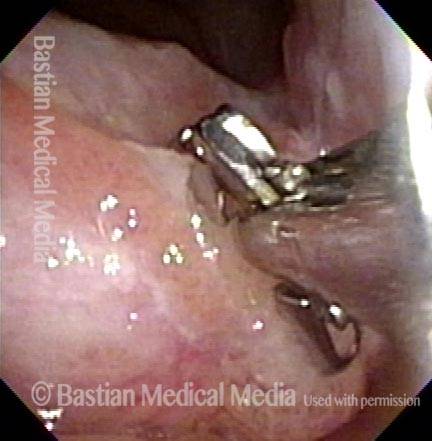
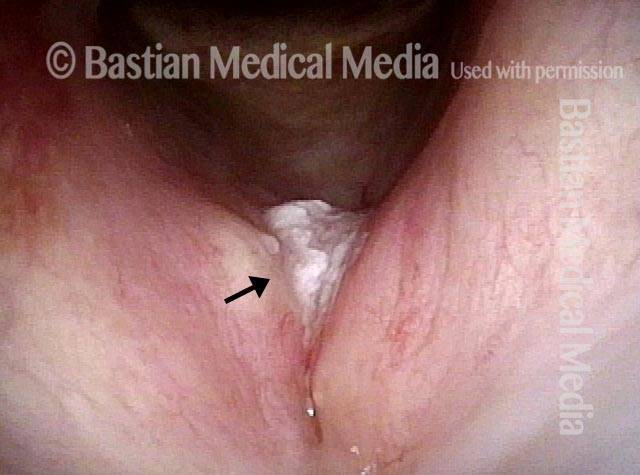
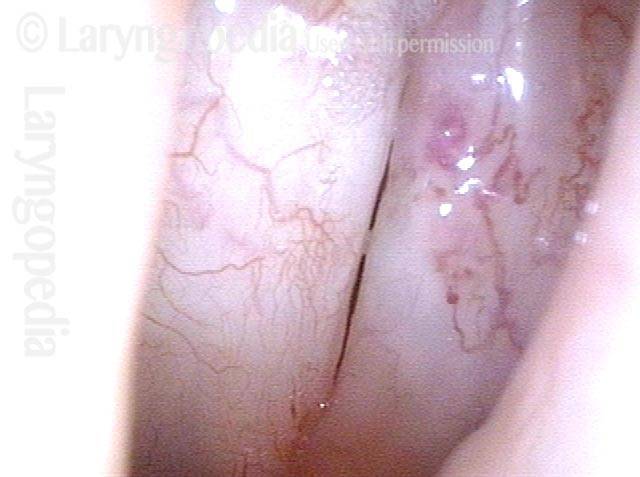
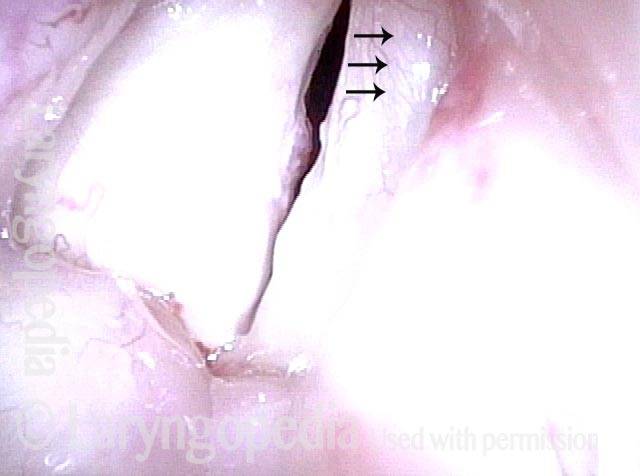
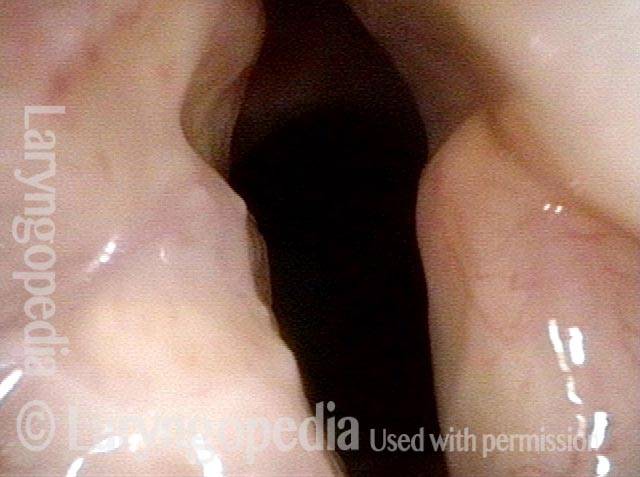
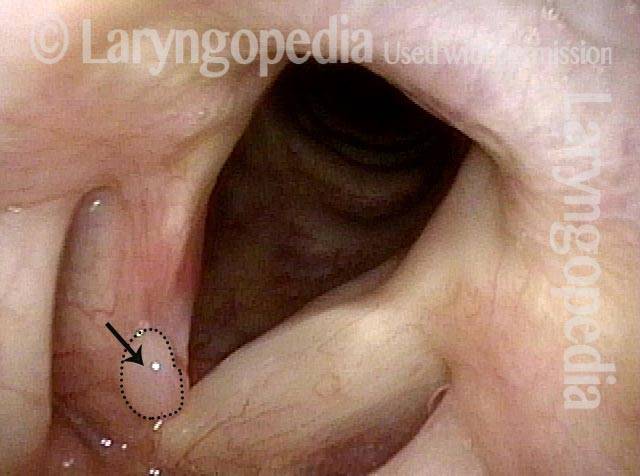
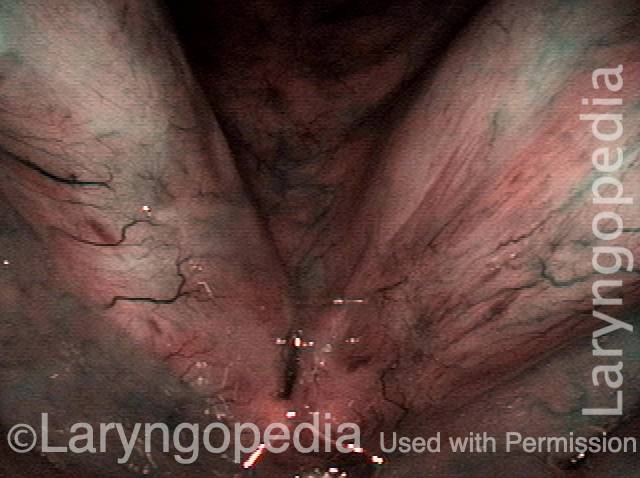
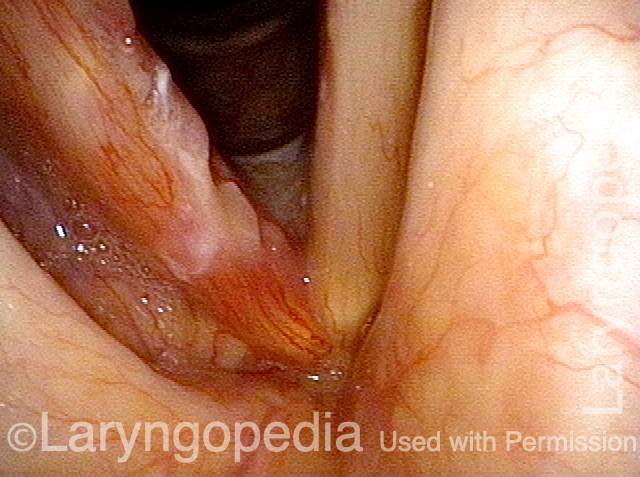
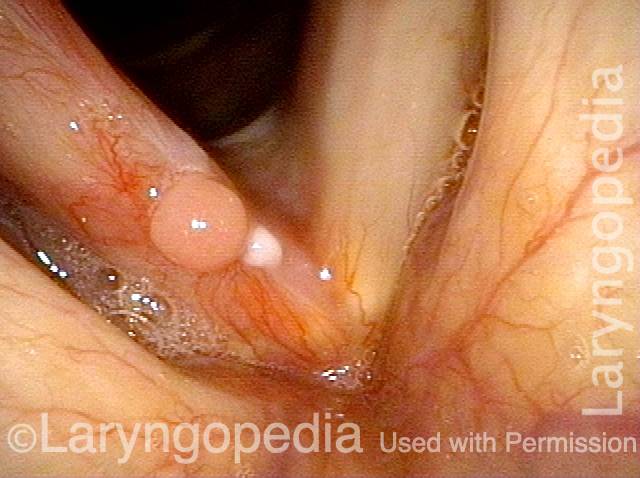
Reparative Granuloma emerges (4 of 10)
Reparative Granuloma emerges (4 of 10)
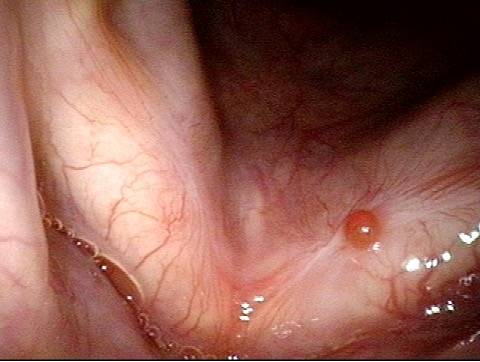
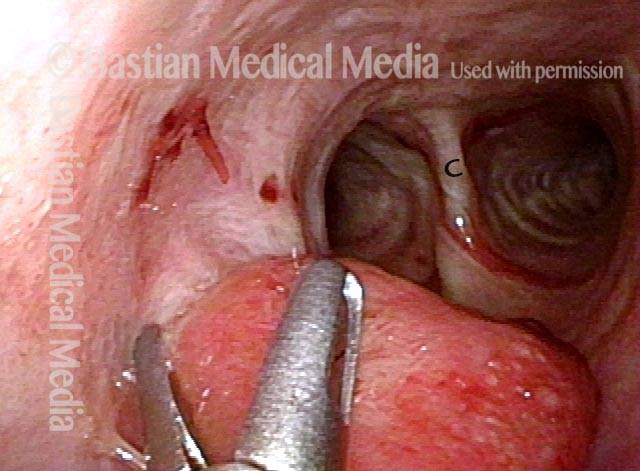
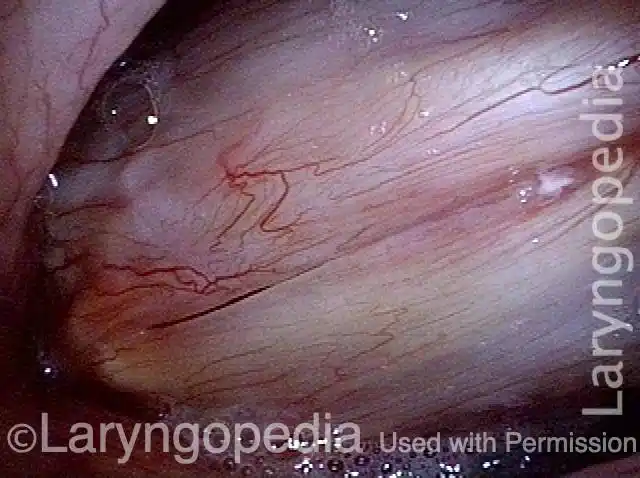
Granuloma interferes with voicing (5 of 10)
Granuloma interferes with voicing (5 of 10)
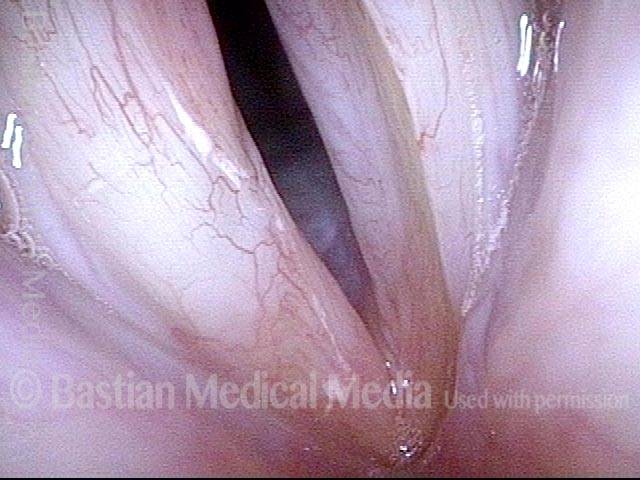
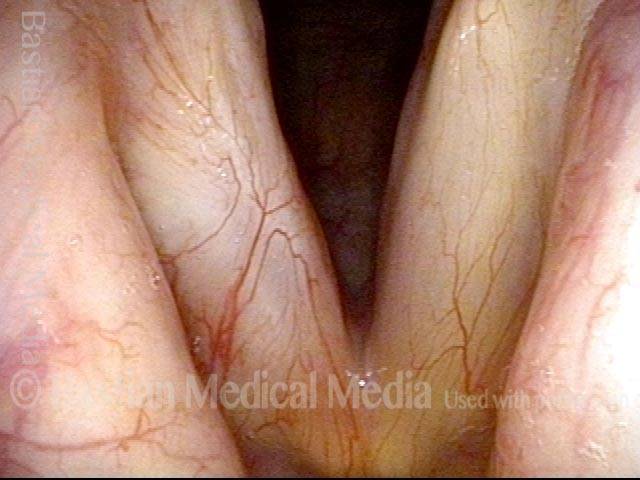
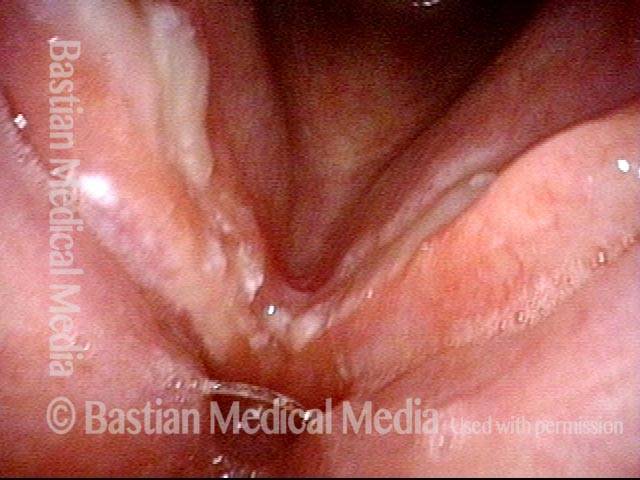
Granuloma fades away (6 of 10)
Granuloma fades away (6 of 10)
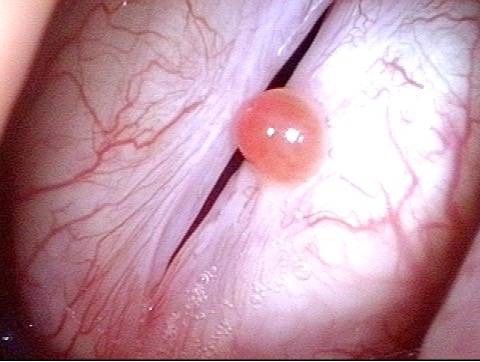
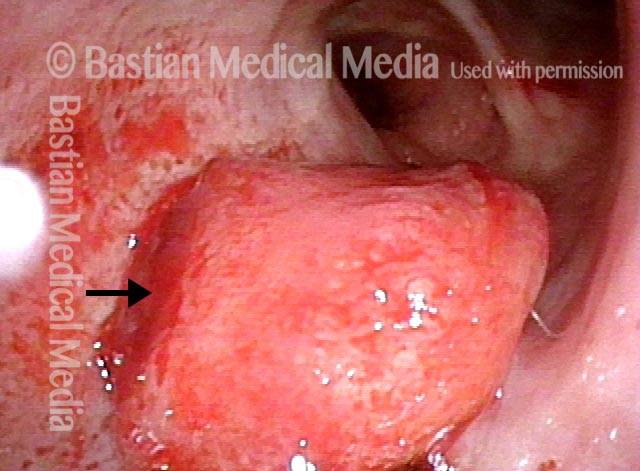
Closer view (7 of 10)
Closer view (7 of 10)
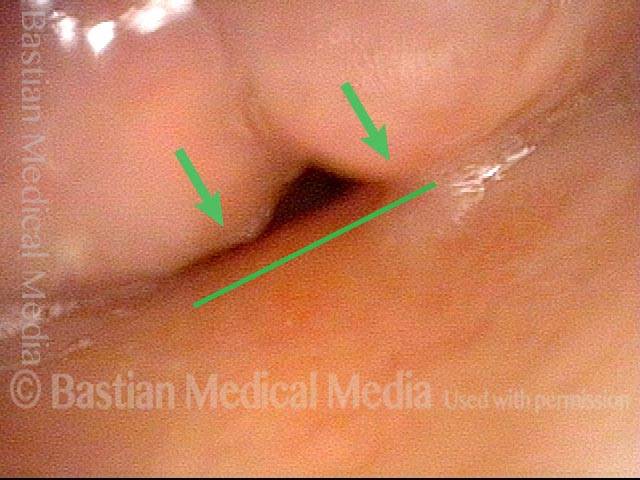
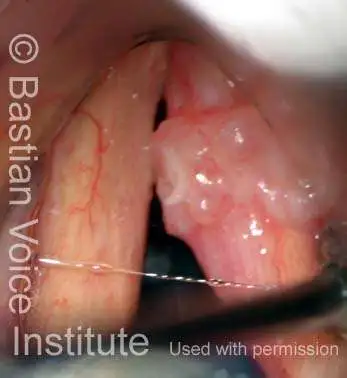
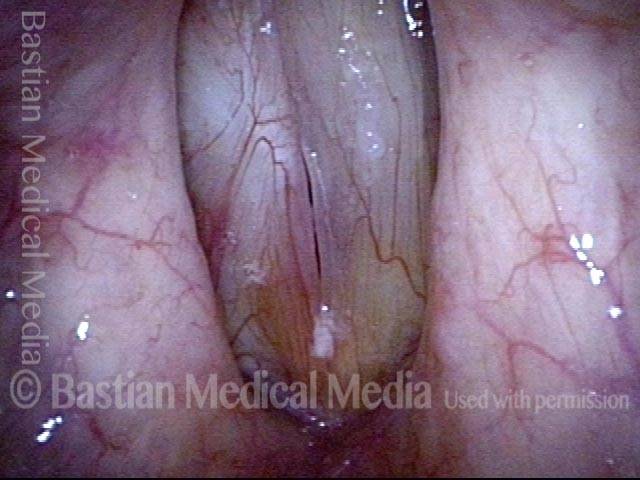
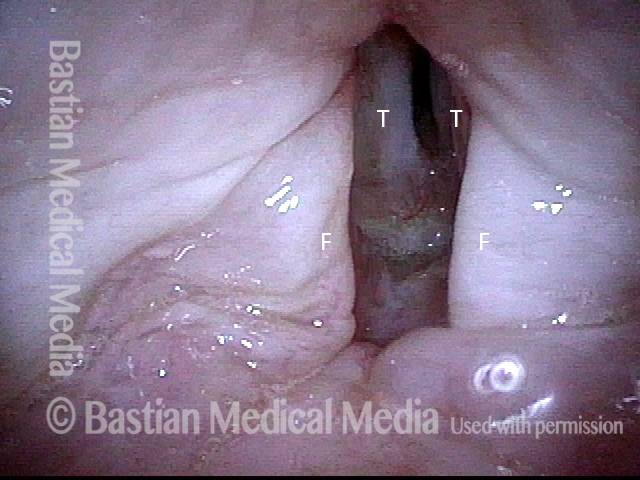
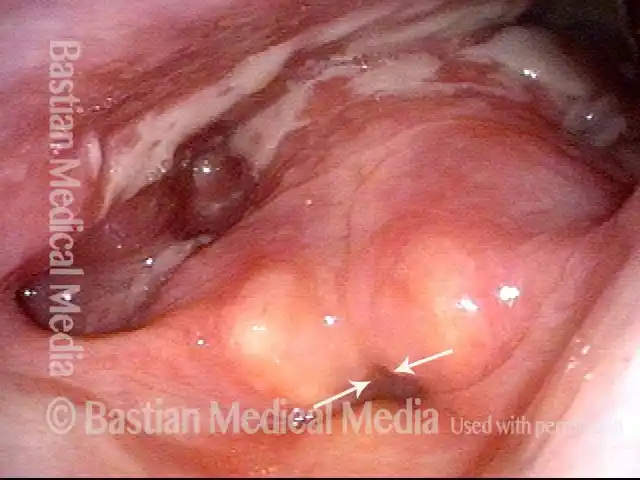
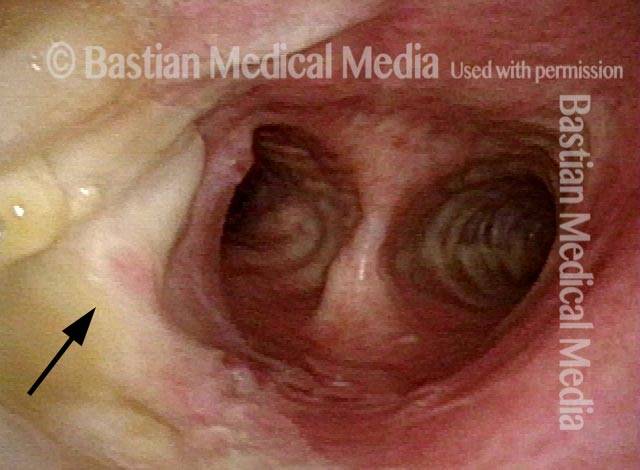
Granuloma cleft (8 of 10)
Granuloma cleft (8 of 10)
Blood tattoo (9 of 10)
Blood tattoo (9 of 10)
Voice is improved (10 of 10)
Voice is improved (10 of 10)
Laser Surgery for Bilateral Vocal Cord Cancer
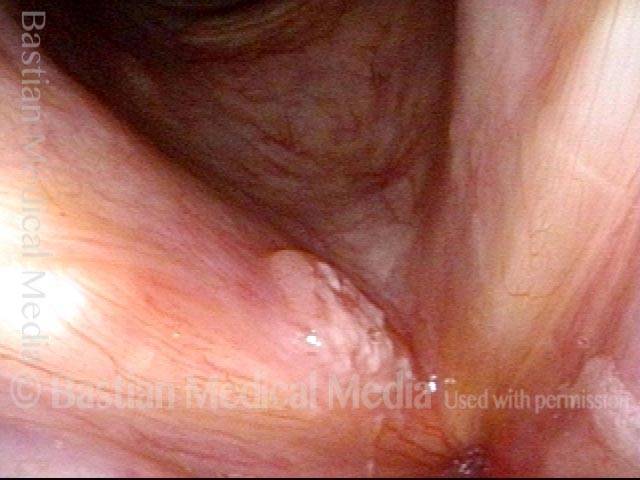
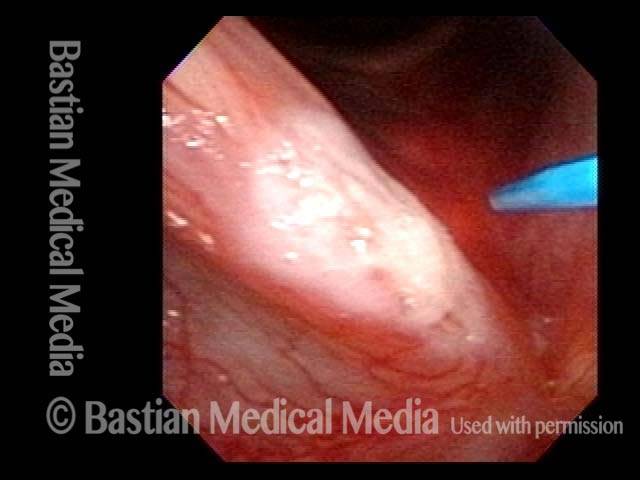
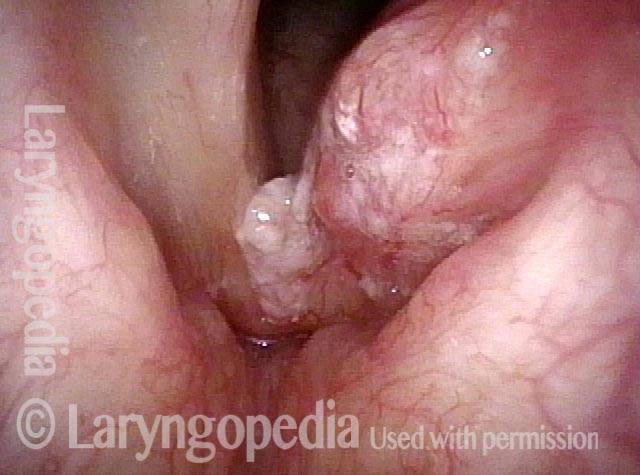
Squamous cell carcinoma (1 of 6)
Squamous cell carcinoma (1 of 6)
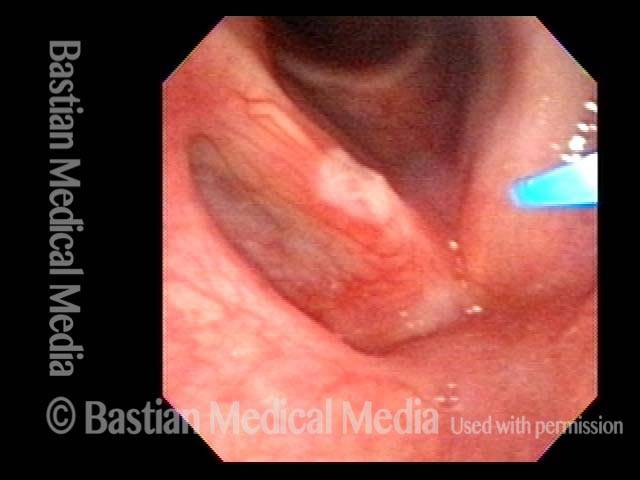
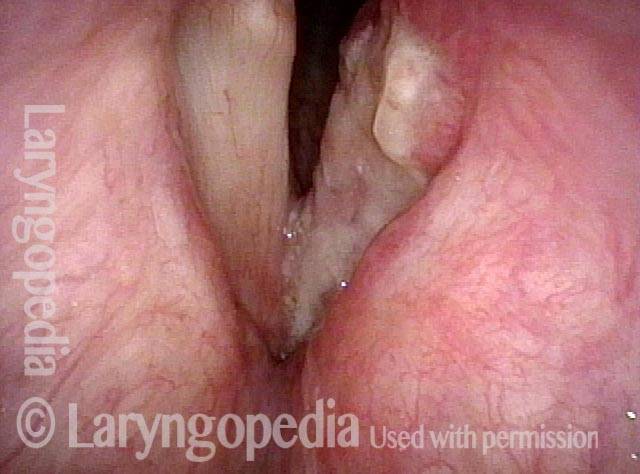
Tumor on the vocal cords (2 of 6)
Tumor on the vocal cords (2 of 6)
Granuloma delays voice recovery (3 of 6)
Granuloma delays voice recovery (3 of 6)
Closer view of granuloma (4 of 6)
Closer view of granuloma (4 of 6)
Granuloma is smaller (5 of 6)
Granuloma is smaller (5 of 6)
Granuloma doesn’t impede voice (6 of 6)
Granuloma doesn’t impede voice (6 of 6)
Vocal Cord Cancer, before and after Surgery
Vocal cord cancer (1 of 8)
Vocal cord cancer (1 of 8)
Vocal cord cancer (2 of 8)
Vocal cord cancer (2 of 8)
Vocal cord cancer, 1 week after surgery (3 of 8)
Vocal cord cancer, 1 week after surgery (3 of 8)
Vocal cord cancer, 1 week after surgery (4 of 8)
Vocal cord cancer, 1 week after surgery (4 of 8)
Vocal cord cancer, 7 weeks after surgery (5 of 8)
Vocal cord cancer, 7 weeks after surgery (5 of 8)
Vocal cord cancer, 7 weeks after surgery (6 of 8)
Vocal cord cancer, 7 weeks after surgery (6 of 8)
Vocal cord cancer, 7 weeks after surgery (7 of 8)
Vocal cord cancer, 7 weeks after surgery (7 of 8)
Vocal cord cancer, 7 weeks after surgery (8 of 8)
Vocal cord cancer, 7 weeks after surgery (8 of 8)
Example 2
Vocal cord cancer (1 of 4)
Vocal cord cancer (1 of 4)
Vocal cord cancer, 1 week after surgery (2 of 4)
Vocal cord cancer, 1 week after surgery (2 of 4)
Vocal cord cancer, 1 month after surgery (3 of 4)
Vocal cord cancer, 1 month after surgery (3 of 4)
Vocal cord cancer, after complete healing (4 of 4)
Vocal cord cancer, after complete healing (4 of 4)
Glottic Cancer, Laser Removal
Glottic cancer, laser removal (1 of 3)
Glottic cancer, laser removal (1 of 3)
Glottic cancer, laser removal (2 of 3)
Glottic cancer, laser removal (2 of 3)
Glottic cancer, laser removal (3 of 3)
Glottic cancer, laser removal (3 of 3)
Glottic Cancer, After Surgery
Glottic cancer, after surgery (1 of 3)
Glottic cancer, after surgery (1 of 3)
Glottic cancer, after surgery (2 of 3)
Glottic cancer, after surgery (2 of 3)
Glottic cancer, after surgery (3 of 3)
Glottic cancer, after surgery (3 of 3)
Breaking cancer “rules” intelligently with use of laser
Post radiotherapy stage (1 of 8)
Post radiotherapy stage (1 of 8)
Laser surgery typically not acceptable (2 of 8)
Laser surgery typically not acceptable (2 of 8)
Laser removal of tumor with careful followup (3 of 8)
Laser removal of tumor with careful followup (3 of 8)
Second view post laser surgery (4 of 8)
Second view post laser surgery (4 of 8)
Six months post laser surgery (5 of 8)
Six months post laser surgery (5 of 8)
Blood vessels stable two months post surgery (6 of 8)
Blood vessels stable two months post surgery (6 of 8)
Open phase of false vocal cord phonation (7 of 8)
Open phase of false vocal cord phonation (7 of 8)
Closed phase of false vocal cord phonation (8 of 8)
Closed phase of false vocal cord phonation (8 of 8)
Glottic/vocal cord cancer
Glottic/vocal cord cancer (1 of 2)
Glottic/vocal cord cancer (1 of 2)
Glottic/vocal cord cancer (2 of 2)
Glottic/vocal cord cancer (2 of 2)
Supraglottic cancer
Supraglottic cancer (1 of 4)
Supraglottic cancer (1 of 4)
Supraglottic cancer (2 of 4)
Supraglottic cancer (2 of 4)
Supraglottic cancer (3 of 4)
Supraglottic cancer (3 of 4)
Supraglottic cancer (4 of 4)
Supraglottic cancer (4 of 4)
Hypopharyngeal Cancer, before and after Surgery
Hypopharyngeal cancer (1 of 10)
Hypopharyngeal cancer (1 of 10)
Hypopharyngeal cancer (2 of 10)
Hypopharyngeal cancer (2 of 10)
Hypopharyngeal cancer (3 of 10)
Hypopharyngeal cancer (3 of 10)
Hypopharyngeal cancer (4 of 10)
Hypopharyngeal cancer (4 of 10)
Hypopharyngeal cancer: 1 week after surgery (5 of 10)
Hypopharyngeal cancer: 1 week after surgery (5 of 10)
Hypopharyngeal cancer: 1 week after surgery (6 of 10)
Hypopharyngeal cancer: 1 week after surgery (6 of 10)
Hypopharyngeal cancer: 1 week after surgery (7 of 10)
Hypopharyngeal cancer: 1 week after surgery (7 of 10)
Hypopharyngeal cancer: 1 week after surgery (8 of 10)
Hypopharyngeal cancer: 1 week after surgery (8 of 10)
Hypopharyngeal cancer: several months after surgery (9 of 10)
Hypopharyngeal cancer: several months after surgery (9 of 10)
Hypopharyngeal cancer: several months after surgery (10 of 10)
Hypopharyngeal cancer: several months after surgery (10 of 10)
Verrucous Carcinoma, before and after Laser Treatment
Verrucous carcinoma (1 of 5)
Verrucous carcinoma (1 of 5)
During voicing (2 of 5)
During voicing (2 of 5)
After laser treatment (3 of 5)
After laser treatment (3 of 5)
Mucus remains several weeks after laser treatment (4 of 5)
Mucus remains several weeks after laser treatment (4 of 5)
Much improvement several weeks after laser treatment (5 of 5)
Much improvement several weeks after laser treatment (5 of 5)
Cancer, HPV Subtype 16, before and after Radiation
Cancer: HPV Subtype 16 (1 of 5)
Cancer: HPV Subtype 16 (1 of 5)
Cancer: HPV Subtype 16, after radiation therapy (3 of 5)
Cancer: HPV Subtype 16, after radiation therapy (3 of 5)
Cancer: HPV Subtype 16, after radiation therapy (4 of 5)
Cancer: HPV Subtype 16, after radiation therapy (4 of 5)
Cancer: HPV Subtype 16, after radiation therapy (5 of 5)
Cancer: HPV Subtype 16, after radiation therapy (5 of 5)
Vocal Cord Cancer, before, during, and after Radiation
Vocal cord cancer (1 of 7)
Vocal cord cancer (1 of 7)
Vocal cord cancer (2 of 7)
Vocal cord cancer (2 of 7)
Vocal cord cancer, 3 weeks after radiotherapy (4 of 7)
Vocal cord cancer, 3 weeks after radiotherapy (4 of 7)
Vocal cord cancer, 3 weeks after radiotherapy (5 of 7)
Vocal cord cancer, 3 weeks after radiotherapy (5 of 7)
Vocal cord cancer, 2 months after radiotherapy (6 of 7)
Vocal cord cancer, 2 months after radiotherapy (6 of 7)
Vocal cord cancer, 2 months after radiotherapy (7 of 7)
Vocal cord cancer, 2 months after radiotherapy (7 of 7)
Example 2
Vocal cord cancer (1 of 8)
Vocal cord cancer (1 of 8)
Vocal cord cancer (2 of 8)
Vocal cord cancer (2 of 8)
Vocal cord cancer, during radiation (3 of 8)
Vocal cord cancer, during radiation (3 of 8)
Vocal cord cancer, during radiation (4 of 8)
Vocal cord cancer, during radiation (4 of 8)
Vocal cord cancer, 2 months after radiation (5 of 8)
Vocal cord cancer, 2 months after radiation (5 of 8)
Vocal cord cancer, 4 months after radiation (6 of 8)
Vocal cord cancer, 4 months after radiation (6 of 8)
Vocal cord cancer, 6 months after radiation (7 of 8)
Vocal cord cancer, 6 months after radiation (7 of 8)
Vocal cord cancer, 6 months after radiation (8 of 8)
Vocal cord cancer, 6 months after radiation (8 of 8)
Radiation Induced Web
Post radiation therapy (1 of 4)
Post radiation therapy (1 of 4)
Web formation (2 of 4)
Web formation (2 of 4)
Closer view of ulceration and web (3 of 4)
Closer view of ulceration and web (3 of 4)
Flexible scope used to separate vocal cords (4 of 4)
Flexible scope used to separate vocal cords (4 of 4)
Larynx Cancer Managed like “skin cancer”
Two years after excision (1 of 4)
Two years after excision (1 of 4)
Narrow-band lighting (2 of 4)
Narrow-band lighting (2 of 4)
During thulium laser coagulation (3 of 4)
During thulium laser coagulation (3 of 4)
After thulium laser coagulation (4 of 4)
After thulium laser coagulation (4 of 4)
Vocal cord CA—a Case for Radiation Instead of Laser Resection
Long term smoker (1 of 4)
Long term smoker (1 of 4)
Tumor (2 of 4)
Tumor (2 of 4)
Radiation therapy suggested (3 of 4)
Radiation therapy suggested (3 of 4)
Two months later (4 of 4)
Two months later (4 of 4)
Scarring after Cancer Treatment but with Very Good Voice
Post laser excision (1 of 4)
Post laser excision (1 of 4)
Prephonatory instant (2 of 4)
Prephonatory instant (2 of 4)
Phonation (3 of 4)
Phonation (3 of 4)
Close-up view (4 of 4)
Close-up view (4 of 4)
Cancer Beginning to Block Airway
Formerly heavy smoker (1 of 2)
Formerly heavy smoker (1 of 2)
Breaking the Rules in Larynx Cancer
Recurrent cancer (1 of 8)
Recurrent cancer (1 of 8)
Closer view (2 of 8)
Closer view (2 of 8)
One week post laser resection (3 of 8)
One week post laser resection (3 of 8)
One year postop (4 of 8)
One year postop (4 of 8)
True cord phonation (5 of 8)
True cord phonation (5 of 8)
False vocal cords (6 of 8)
False vocal cords (6 of 8)
False vocal cord closure (7 of 8)
False vocal cord closure (7 of 8)
True cords (8 of 8)
True cords (8 of 8)
Biopsy of Early Vocal Cord Cancer
Chronic hoarseness (1 of 3)
Chronic hoarseness (1 of 3)
Just before biopsy (2 of 3)
Just before biopsy (2 of 3)
Cancer finding (3 of 3)
Cancer finding (3 of 3)
Tumor in Trachea
Biopsy (1 of 4)
Biopsy (1 of 4)
After biopsy (2 of 4)
After biopsy (2 of 4)
Tumor gone (3 of 4)
Tumor gone (3 of 4)
Slow return (4 of 4)
Slow return (4 of 4)
HPV 31 Cancer Cure
Carcinoma in situ (1 of 4)
Carcinoma in situ (1 of 4)
HPV subtype 31 (2 of 4)
HPV subtype 31 (2 of 4)
Excisions (3 of 4)
Excisions (3 of 4)
Seven years later (4 of 4)
Seven years later (4 of 4)
Before and after Radiation for Vocal Cord Cancer
Bilateral vocal cord cancer (1 of 4)
Bilateral vocal cord cancer (1 of 4)
“Tumor vessels” (2 of 4)
“Tumor vessels” (2 of 4)
After radiotherapy (3 of 4)
After radiotherapy (3 of 4)
Vascular pattern (4 of 4)
Vascular pattern (4 of 4)
Small, but Dangerous!
Post radiotherapy (1 of 4)
Post radiotherapy (1 of 4)
Normal voice (2 of 4)
Normal voice (2 of 4)
Persistent cancer (3 of 4)
Persistent cancer (3 of 4)
T4 tumor (4 of 4)
T4 tumor (4 of 4)
Unusual Posterior and Transglottic Epicenter for Larynx Cancer
Tumor (1 of 4)
Tumor (1 of 4)
Accentuation of the vascularity (2 of 4)
Accentuation of the vascularity (2 of 4)
Posterior commissure (3 of 4)
Posterior commissure (3 of 4)
A year later (4 of 4)
A year later (4 of 4)
Nice try, but on to Radiation
Vocal cord lesion (1 of 4)
Vocal cord lesion (1 of 4)
Closer view (2 of 4)
Closer view (2 of 4)
Removal of tumor (3 of 4)
Removal of tumor (3 of 4)
Nice try, but on to radiation (4 of 4)
Nice try, but on to radiation (4 of 4)
Progressive Cricoarytenoid Joint Fibrosis / Fixation as a Late Complication of Radiation
25 years post radiotherapy (1 of 4)
25 years post radiotherapy (1 of 4)
Fibrosis (2 of 4)
Fibrosis (2 of 4)
Closed phase (3 of 4)
Closed phase (3 of 4)
Open phase (4 of 4)
Open phase (4 of 4)
Progressive Radiation Fibrosis Effects on the Larynx and a Solution to some of it
Forty years post-radiation (1 of 8)
Forty years post-radiation (1 of 8)
Involuntary inspiratory voice (2 of 8)
Involuntary inspiratory voice (2 of 8)
Only capable of high pitch (3 of 8)
Only capable of high pitch (3 of 8)
Open phase vibration (4 of 8)
Open phase vibration (4 of 8)
One week post-commissuroplasty (5 of 8)
One week post-commissuroplasty (5 of 8)
Rapid inhalation, closer view (6 of 8)
Rapid inhalation, closer view (6 of 8)
Three months post-surgery (7 of 8)
Three months post-surgery (7 of 8)
Closer view, post-surgery (8 of 8)
Closer view, post-surgery (8 of 8)
Evolution of the Wound after Laser Removal of a vocal Cord Cancer: Not Pretty at First, but Voice Result can be very Good
Vocal cord cancer (1 of 8)
Vocal cord cancer (1 of 8)
Voice-making with tumor (2 of 8)
Voice-making with tumor (2 of 8)
One week post-removal (3 of 8)
One week post-removal (3 of 8)
Voice-making, post-removal (4 of 8)
Voice-making, post-removal (4 of 8)
Six weeks post-op (5 of 8)
Six weeks post-op (5 of 8)
Voice-making, post-op (6 of 8)
Voice-making, post-op (6 of 8)
Four months post-op (7 of 8)
Four months post-op (7 of 8)
Voice-making, four months post-op (8 of 8)
Voice-making, four months post-op (8 of 8)
Laser can Beat Cancer and Spare Voice even after Radiotherapy Failure
Healing post-laser excision(4 of 4)
Healing post-laser excision(4 of 4)
Post-laser excision (3 of 4)
Post-laser excision (3 of 4)
Leukoplakia and Stippled Vascularity(2 of 4)
Leukoplakia and Stippled Vascularity(2 of 4)
Return of cancer (1 of 4)
Return of cancer (1 of 4)
How a Vocal Cord Heals after Laser Removal of a Cancer
squamous cell carcinoma (1 of 6)
squamous cell carcinoma (1 of 6)
1 week after laser excision (2 of 6)
1 week after laser excision (2 of 6)
Difficulty speaking (3 of 6)
Difficulty speaking (3 of 6)
Natural granulation after laser excision (4 of 6)
Natural granulation after laser excision (4 of 6)
Abnormal capillary pattern (5 of 6)
Abnormal capillary pattern (5 of 6)
Stiff right vocal cord (6 of 6)
Stiff right vocal cord (6 of 6)
Early Vocal Cord Cancer
This video provides an introduction to early vocal cord cancer (stages 1 and 2) and compares the two main treatment options: laser surgery and radiation therapy.