The posterior pharyngeal wall is the back wall of the swallowing passage. The upper part of the posterior pharyngeal wall can be seen when one looks through an opened mouth, beyond the soft palate, uvula, and tonsils. There is a layer of mucosa, then muscle, and then the bodies of the cervical vertebrae.
Pharyngocutaneous Fistula
Pharyngocutaneous fistula (1 of 3)
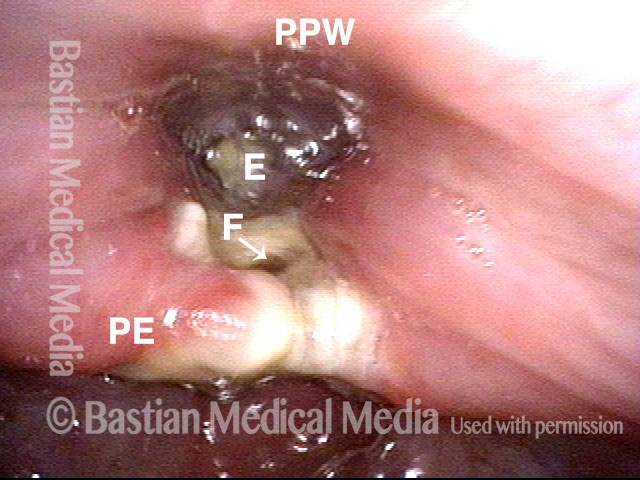
Panorama of reconstructed hypopharynx one week after laryngectomy for persistent cancer after radiotherapy. (PPW = posterior pharyngeal wall. PE = pseudo-epiglottis, often seen after reconstruction. F's arrow = fistula. E = esophageal entrance.)
Pharyngocutaneous fistula (1 of 3)
Panorama of reconstructed hypopharynx one week after laryngectomy for persistent cancer after radiotherapy. (PPW = posterior pharyngeal wall. PE = pseudo-epiglottis, often seen after reconstruction. F's arrow = fistula. E = esophageal entrance.)
Closer view (2 of 3)
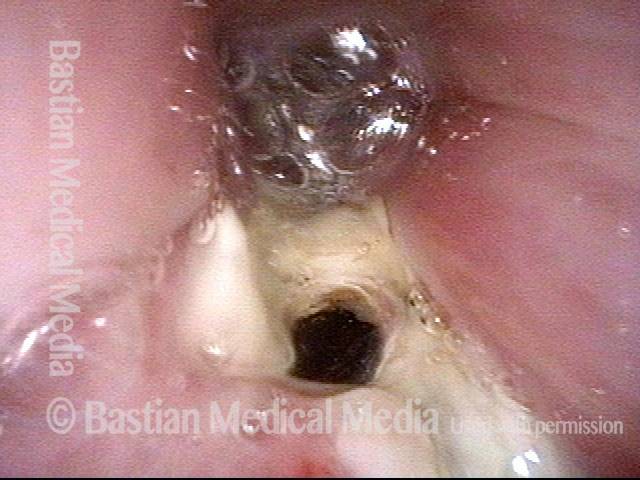
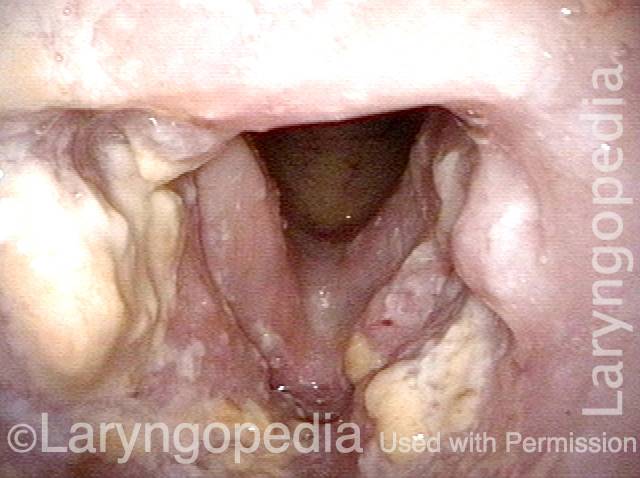
Closer view of fistula opening and esophageal entrance, with salivary pooling.
Closer view (2 of 3)
Closer view of fistula opening and esophageal entrance, with salivary pooling.
Pharyngocutaneous fistula (3 of 3)
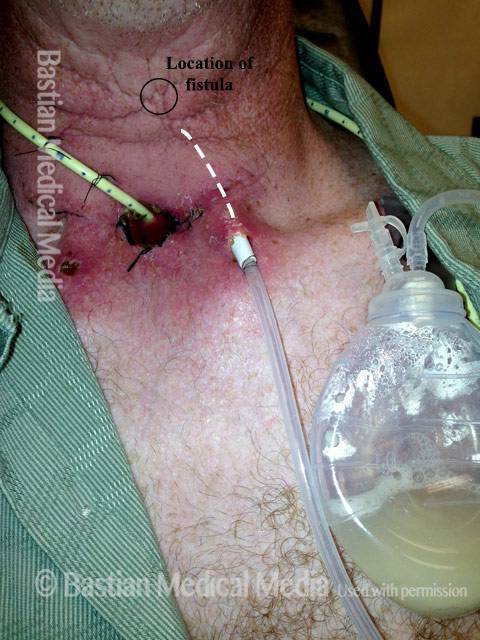
Patient receiving suction drain treatment. The suction tubing evacuates saliva drop by drop as it forms, eliminating the need for wound dressings and long term antibiotics. This treatment also prevents infection and causes less discomfort for the patient than traditional treatment.
Pharyngocutaneous fistula (3 of 3)
Patient receiving suction drain treatment. The suction tubing evacuates saliva drop by drop as it forms, eliminating the need for wound dressings and long term antibiotics. This treatment also prevents infection and causes less discomfort for the patient than traditional treatment.
Sometimes “low-tech” Is Best for Stenosis
Esophageal bougie (1 of 4)
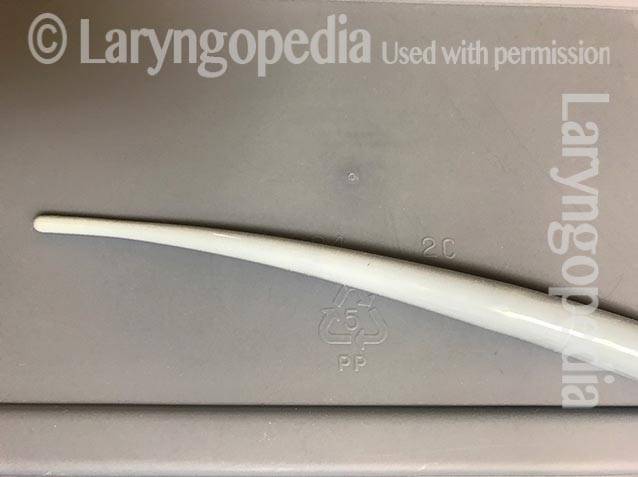
This is an esophageal bougie. With the patient sitting in a chair and after gargling topical anesthetic, this tapered and flexible dilator is passed through the mouth and into the upper esophagus to dilate (stretch) an area narrowed by radiation therapy for a larynx cancer.
Esophageal bougie (1 of 4)
This is an esophageal bougie. With the patient sitting in a chair and after gargling topical anesthetic, this tapered and flexible dilator is passed through the mouth and into the upper esophagus to dilate (stretch) an area narrowed by radiation therapy for a larynx cancer.
Swallowing crescent (2 of 4)
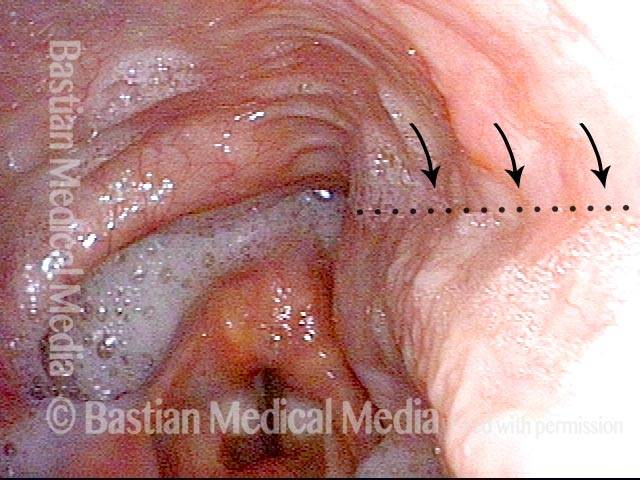
The area of stenosis is just below the swallowing crescent (dotted outline). Arytenoid mounds are permanently swollen due to (expected, typical) radiation damage. The arrow shows the trajectory of the bougie that is about to be inserted.
Swallowing crescent (2 of 4)
The area of stenosis is just below the swallowing crescent (dotted outline). Arytenoid mounds are permanently swollen due to (expected, typical) radiation damage. The arrow shows the trajectory of the bougie that is about to be inserted.
Post-arytenoid area (3 of 4)
The tapered tip is arriving at and just beginning to enter the post-arytenoid area. As it is inserted farther, its diameter will increase.
Post-arytenoid area (3 of 4)
The tapered tip is arriving at and just beginning to enter the post-arytenoid area. As it is inserted farther, its diameter will increase.
Maximum diameter (4 of 4)
Here, the bougie is at its maximum diameter. The real goal is to stretch the stenosis, but it also pulls the larynx forward, creating space (bracket) between posterior surface of arytenoid (A) and the posterior pharyngeal wall (PPW)
Maximum diameter (4 of 4)
Here, the bougie is at its maximum diameter. The real goal is to stretch the stenosis, but it also pulls the larynx forward, creating space (bracket) between posterior surface of arytenoid (A) and the posterior pharyngeal wall (PPW)
Pharyngeal Paralysis, Seen with Pharynx Contraction
Pharyngeal paralysis (1 of 2)
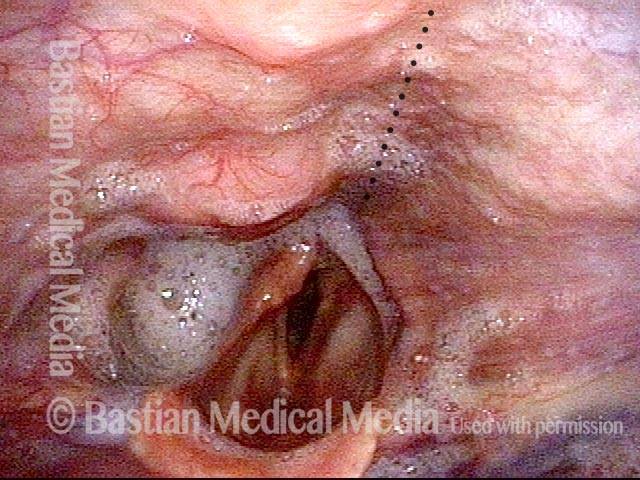
View of the laryngopharynx. This patient has pharyngeal paralysis on one side, which is already slightly evident because the posterior pharyngeal wall's midline (dotted line) is deviating here slightly to one side, even at rest.
Pharyngeal paralysis (1 of 2)
View of the laryngopharynx. This patient has pharyngeal paralysis on one side, which is already slightly evident because the posterior pharyngeal wall's midline (dotted line) is deviating here slightly to one side, even at rest.
Pharyngeal paralysis, more obvious with pharynx contraction (2 of 2)
The pharynx is contracted, and the posterior pharyngeal wall (midline again at dotted line) now deviates dramatically toward the non-paralyzed side of the pharynx. This pharynx contraction was elicited via extremely high-pitched voicing.
Pharyngeal paralysis, more obvious with pharynx contraction (2 of 2)
The pharynx is contracted, and the posterior pharyngeal wall (midline again at dotted line) now deviates dramatically toward the non-paralyzed side of the pharynx. This pharynx contraction was elicited via extremely high-pitched voicing.
Solid Food Dysphagia Due to an Unexplained Benign Mass
Benign mass (1 of 4)
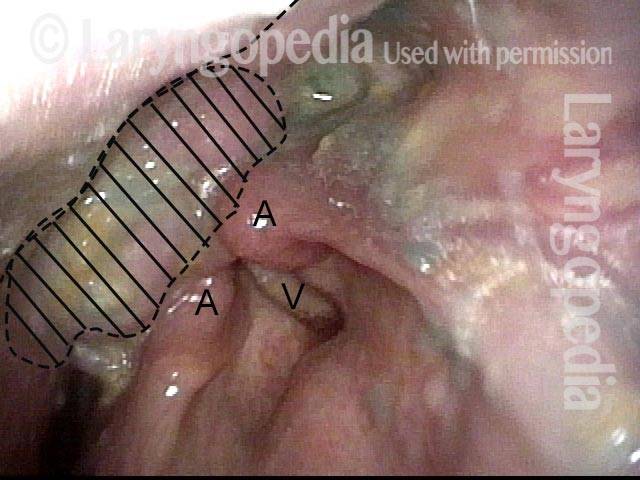
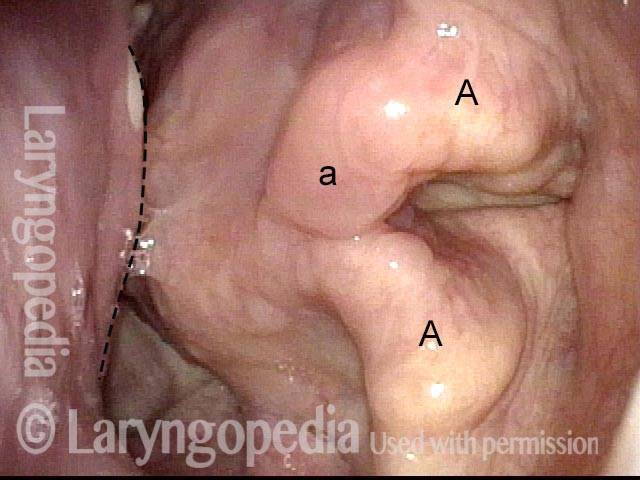
This elderly man is having a hard time swallowing solids. There is a mucosa-covered mass (marked with lines) between the posterior pharyngeal wall (longer dashed line) and the arytenoid towers ( marked with A). "V" denotes the right vocal cord.
Benign mass (1 of 4)
This elderly man is having a hard time swallowing solids. There is a mucosa-covered mass (marked with lines) between the posterior pharyngeal wall (longer dashed line) and the arytenoid towers ( marked with A). "V" denotes the right vocal cord.
Closer view (2 of 4)
At much closer range while having the patient perform a trumpet maneuver.
Closer view (2 of 4)
At much closer range while having the patient perform a trumpet maneuver.
One week post-op (3 of 4)
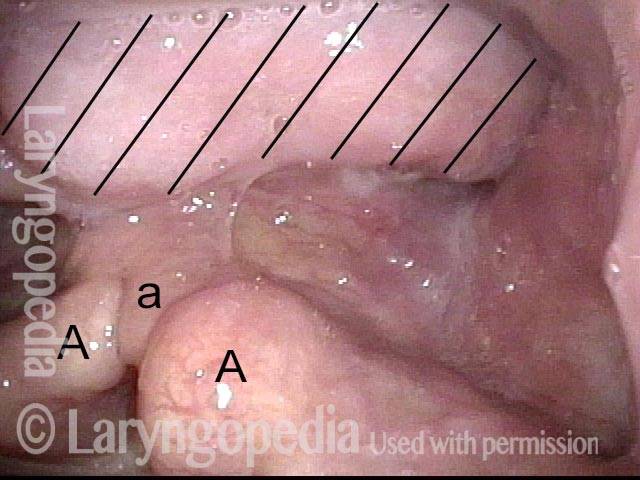
This is a week after laser excision of this mass. The dashed line again shows the posterior pharyngeal wall and A and V again denote arytenoid apices and V, the right vocal cord. The pathology examination shows only fibrosis and other nonspecific benign findings.
One week post-op (3 of 4)
This is a week after laser excision of this mass. The dashed line again shows the posterior pharyngeal wall and A and V again denote arytenoid apices and V, the right vocal cord. The pathology examination shows only fibrosis and other nonspecific benign findings.
Trumpet maneuver post-op (4 of 4)
Now performing trumpet maneuver (as in photo 2), the upper edge of the excision is shown (dashed line, left of photo). In spite of a very sore throat, this man can already sense improvement in his swallowing.
Trumpet maneuver post-op (4 of 4)
Now performing trumpet maneuver (as in photo 2), the upper edge of the excision is shown (dashed line, left of photo). In spite of a very sore throat, this man can already sense improvement in his swallowing.
Candida Infection with Cheesy Residue Before and After Fluconazole
white lesion (1 of 4)
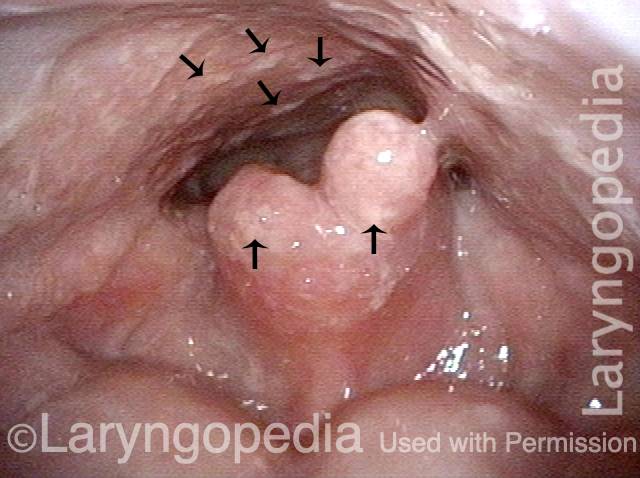
This patient was treated years earlier with radiotherapy for larynx cancer. The esophageal defect is chronic. The main finding here is white lesions on residual epiglottis and posterior pharyngeal wall. Arrows point to some examples of the countless candida colonies.
white lesion (1 of 4)
This patient was treated years earlier with radiotherapy for larynx cancer. The esophageal defect is chronic. The main finding here is white lesions on residual epiglottis and posterior pharyngeal wall. Arrows point to some examples of the countless candida colonies.
Inside the laryngeal vestibule (2 of 4)
Now viewing inside the laryngeal vestibule, notice the cheesy residue clinging in large areas, representing large amounts of candida overgrowth.
Inside the laryngeal vestibule (2 of 4)
Now viewing inside the laryngeal vestibule, notice the cheesy residue clinging in large areas, representing large amounts of candida overgrowth.
White Residue Is Gone (3 of 4)
After 15 days of fluconazole, notice the white residue on esophageal remnant and posterior pharyngeal wall is gone. Compare with photo 1.
White Residue Is Gone (3 of 4)
After 15 days of fluconazole, notice the white residue on esophageal remnant and posterior pharyngeal wall is gone. Compare with photo 1.
After treatment with fluconazole (4 of 4)
Again viewing inside the laryngeal vestibule, after treatment with fluconazole, the copious cheesy residue is also gone. Compare with photo 2.
After treatment with fluconazole (4 of 4)
Again viewing inside the laryngeal vestibule, after treatment with fluconazole, the copious cheesy residue is also gone. Compare with photo 2.
R-CPD and esophageal dilation
Posterior pharyngeal wall (1 of 3)
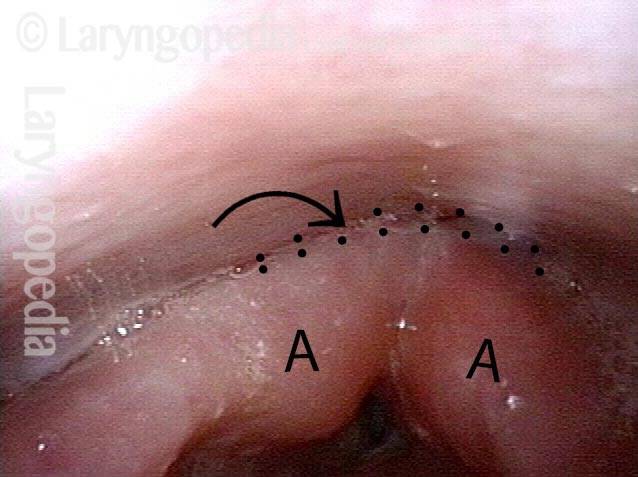
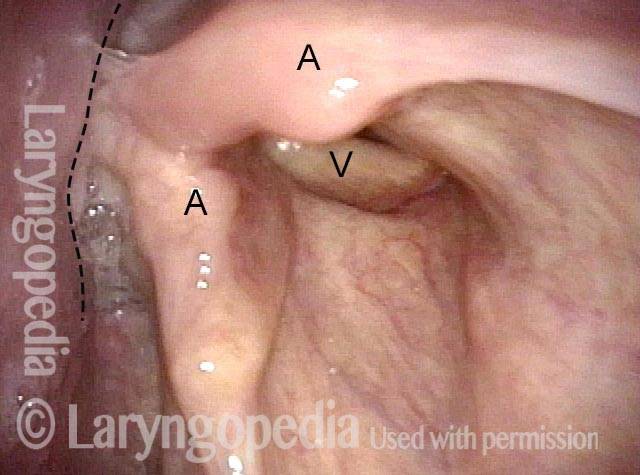
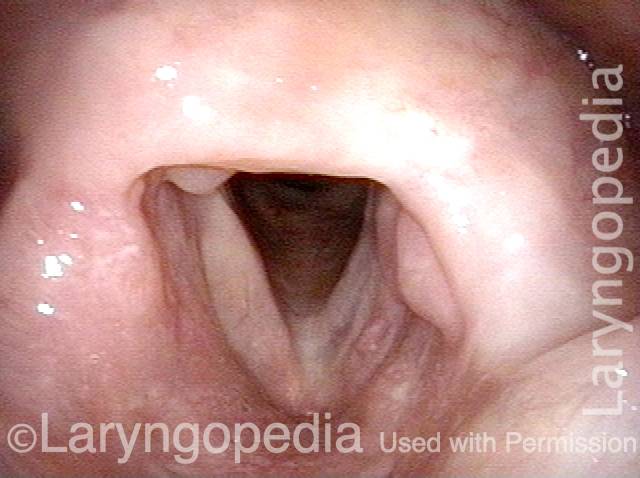
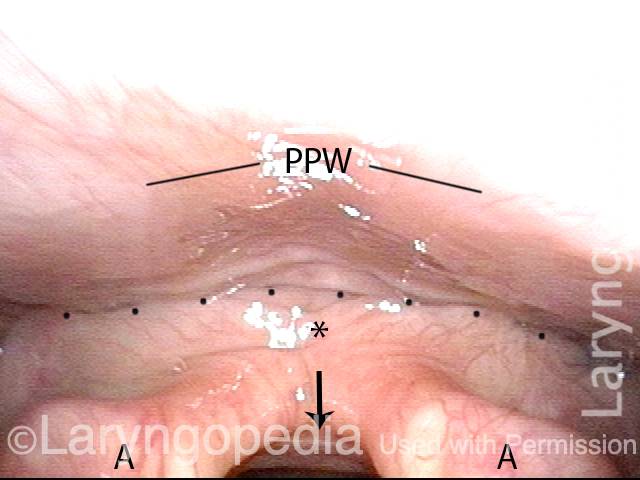
Here, in the panoramic view of the "bottom of the throat," between posterior pharyngeal wall (marked PPW) and arytenoid eminences (A). The airway is indicated by the short arrow, and the dotted line shows the waiting "entrance" to the upper esophagus just above the CPM. The "entrance" opens for a second to permit passage of food or liquid through the sphincter and into the upper esophagus. The * is for reference with photo 2.
Posterior pharyngeal wall (1 of 3)
Here, in the panoramic view of the "bottom of the throat," between posterior pharyngeal wall (marked PPW) and arytenoid eminences (A). The airway is indicated by the short arrow, and the dotted line shows the waiting "entrance" to the upper esophagus just above the CPM. The "entrance" opens for a second to permit passage of food or liquid through the sphincter and into the upper esophagus. The * is for reference with photo 2.
Is it R-CPD? (2 of 3)
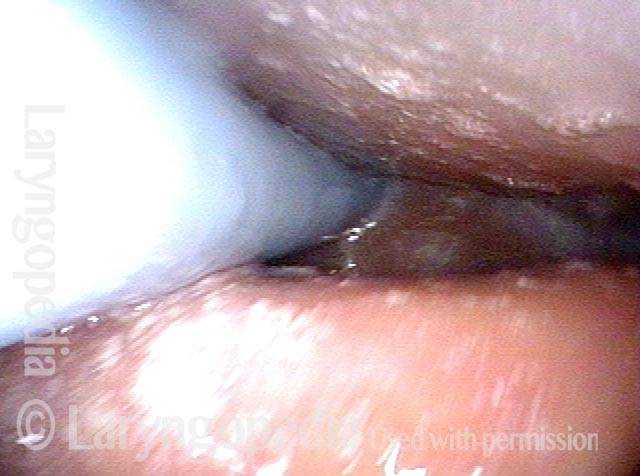
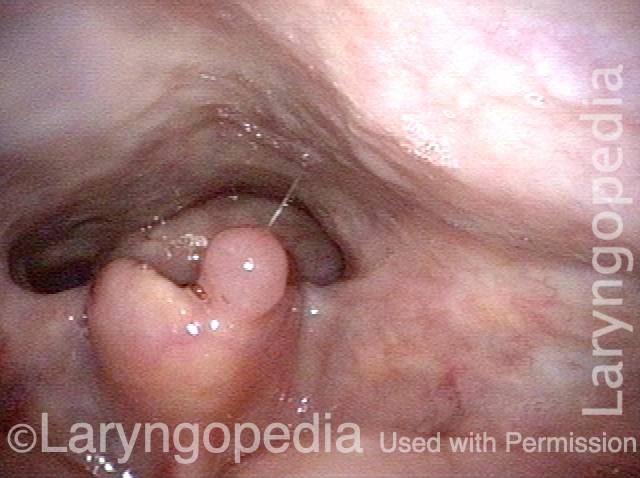
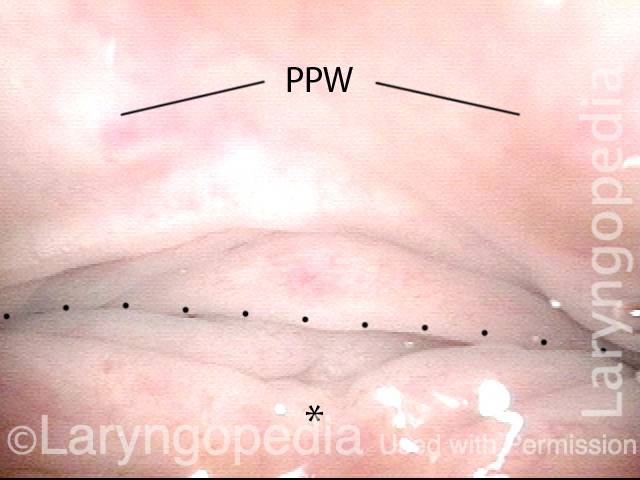
At the entrance to the esophagus, at closer range. Notice that the mucosa is redundant, a common but not universal finding in R-CPD.
Is it R-CPD? (2 of 3)
At the entrance to the esophagus, at closer range. Notice that the mucosa is redundant, a common but not universal finding in R-CPD.
Stretched esophagus indicates R-CPD (3 of 3)
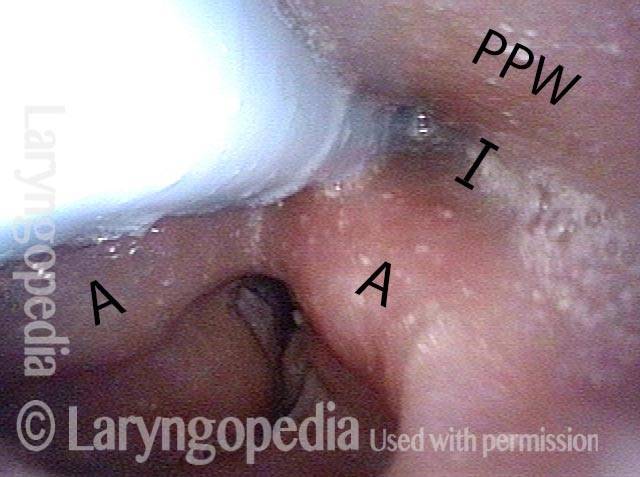
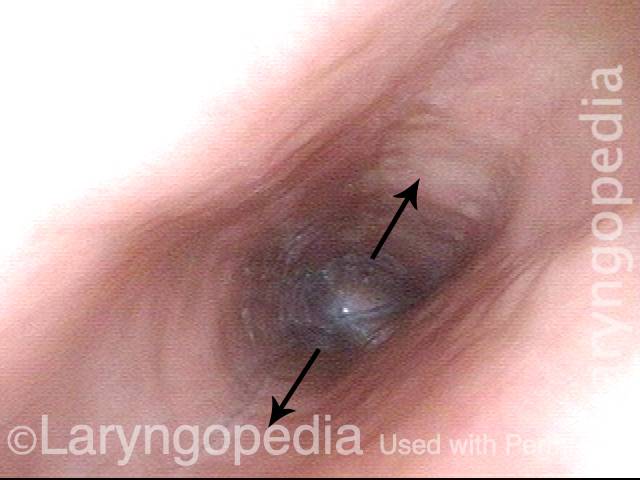
Now the view is within the upper esophagus. It almost appears that the lumen is dilated, especially in a lateral direction (arrows). Purely speculatively, one wonders if constant forcing of air upwards again a barrier ( the non-relaxing cricopharynxgeus muscle, aka upper esophageal sphincter), dilates the esophagus over time. Certainly, many with R-CPD experience not only gurgling, but also chest pressure and even pain that may be from "stretching" of the esophagus.
Stretched esophagus indicates R-CPD (3 of 3)
Now the view is within the upper esophagus. It almost appears that the lumen is dilated, especially in a lateral direction (arrows). Purely speculatively, one wonders if constant forcing of air upwards again a barrier ( the non-relaxing cricopharynxgeus muscle, aka upper esophageal sphincter), dilates the esophagus over time. Certainly, many with R-CPD experience not only gurgling, but also chest pressure and even pain that may be from "stretching" of the esophagus.
Tags
Tagged Anatomy & Physiology, Education