Submucosal fibrosis is a disorder in which the attachment of the mucosa to the underlying vocal ligament appears to thicken and toughen, yet without creating any protrusion, such as one sees with nodules or polyps. The mucosa thereby becomes less flexible. Think of satin turning into canvas of a similar thickness.
Surgery for Fibrosis, Polyp
Fibrosis + polyp (1 of 4)
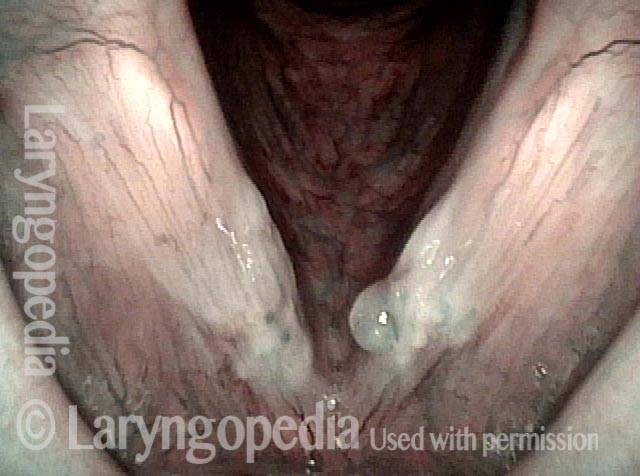
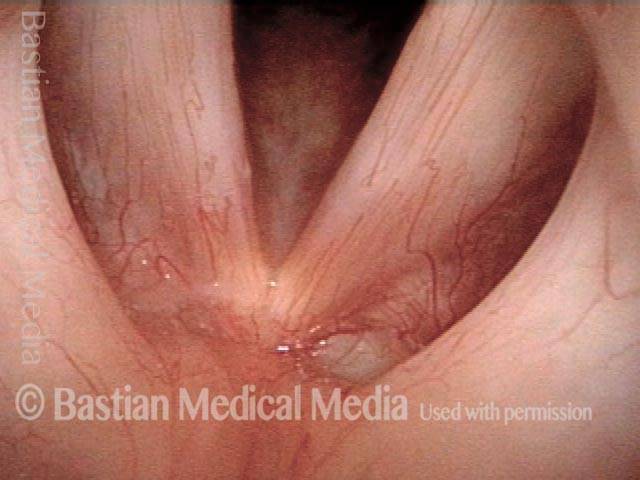
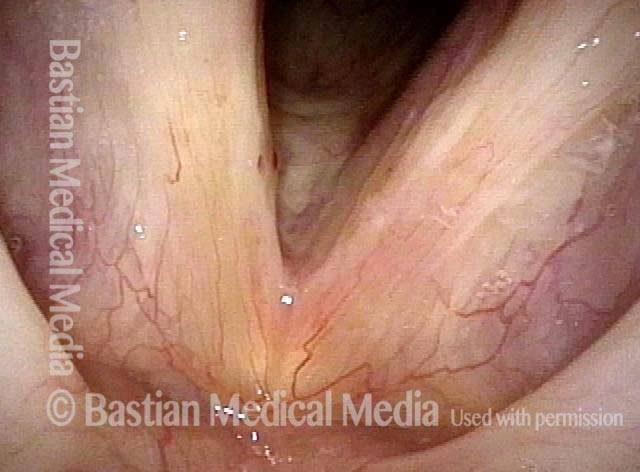
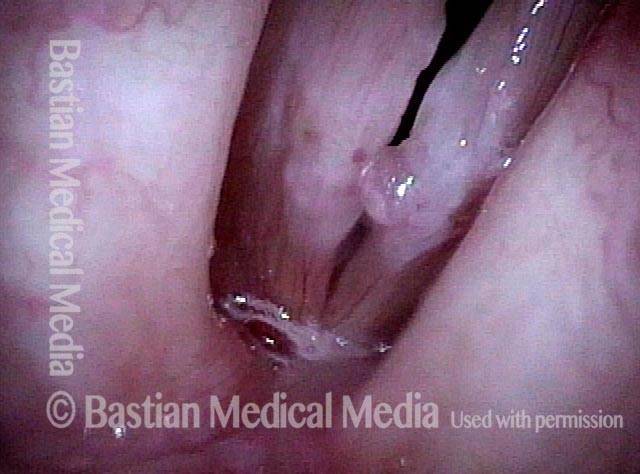
An intense and dynamic teacher (not a singer) has developed not only polyp/ elevation, but fibrosis--the white submucosal deposition of scar-like tissue deposits. Narrow band illumination makes the nature of these lesions more "emphatic."
Fibrosis + polyp (1 of 4)
An intense and dynamic teacher (not a singer) has developed not only polyp/ elevation, but fibrosis--the white submucosal deposition of scar-like tissue deposits. Narrow band illumination makes the nature of these lesions more "emphatic."
Strobe light (2 of 4)
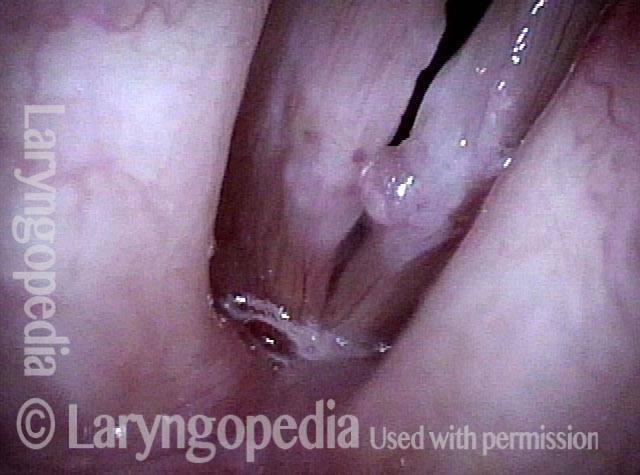
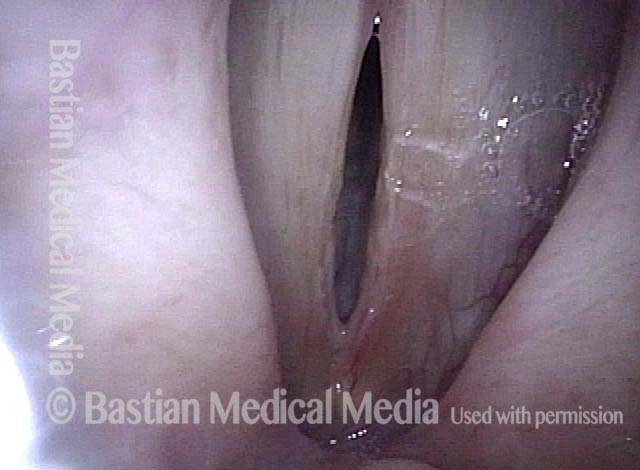
Under strobe light during voicing. Poor match and stiffness are best seen.
Strobe light (2 of 4)
Under strobe light during voicing. Poor match and stiffness are best seen.
Post microsurgery, open phase (3 of 4)
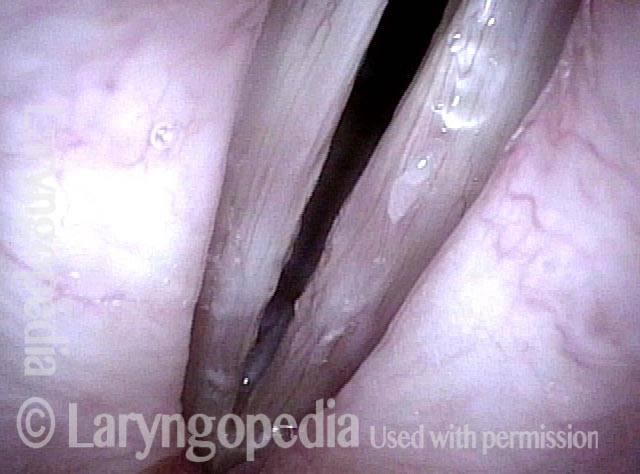
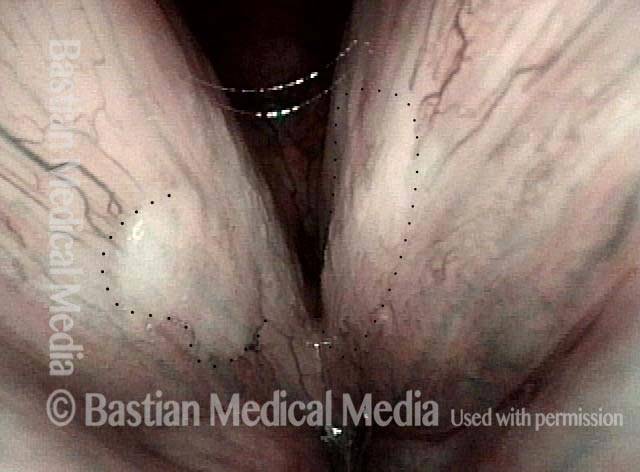
A week after vocal cord microsurgery, voice is markedly improved. No attempt was made to remove all of the fibrosis, but only to straighten the vocal cord margins. Open phase of vibration at F5.
Post microsurgery, open phase (3 of 4)
A week after vocal cord microsurgery, voice is markedly improved. No attempt was made to remove all of the fibrosis, but only to straighten the vocal cord margins. Open phase of vibration at F5.
Post microsurgery, open phase (4 of 4)
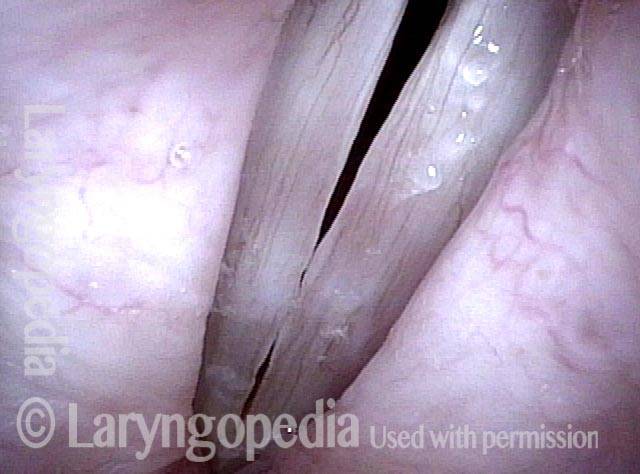
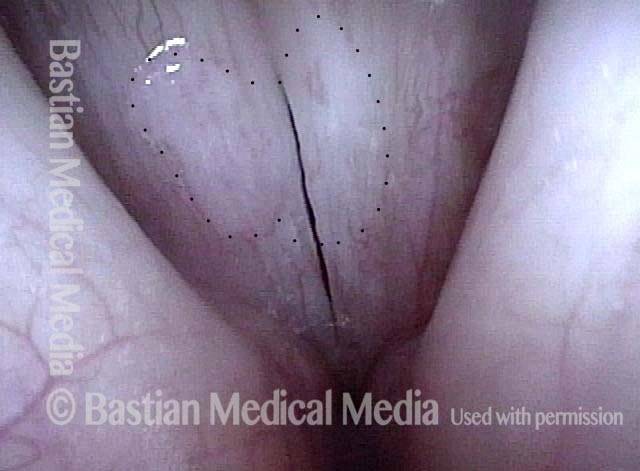
Closed phase of vibration at same pitch shows that some margin swelling remains. The patient also has MTD; posterior cords are widely separated.
Post microsurgery, open phase (4 of 4)
Closed phase of vibration at same pitch shows that some margin swelling remains. The patient also has MTD; posterior cords are widely separated.
Submucosal Fibrosis
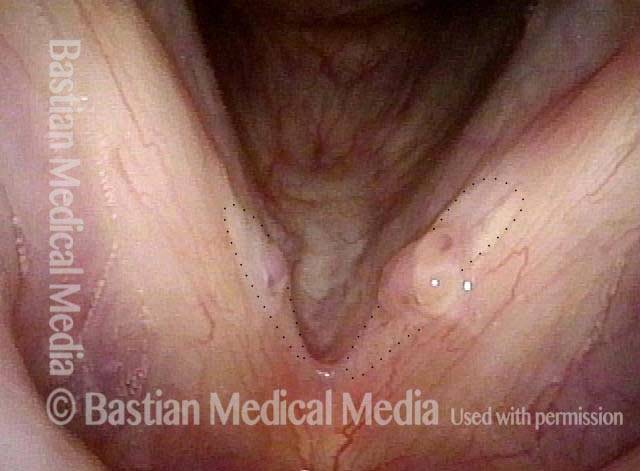
Submucosal fibrosis (1 of 4)
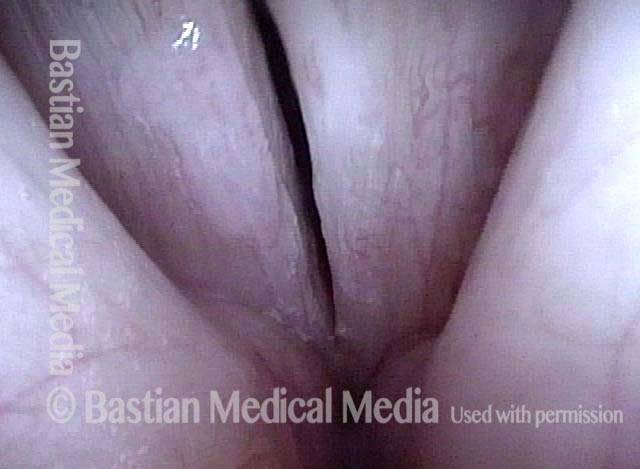
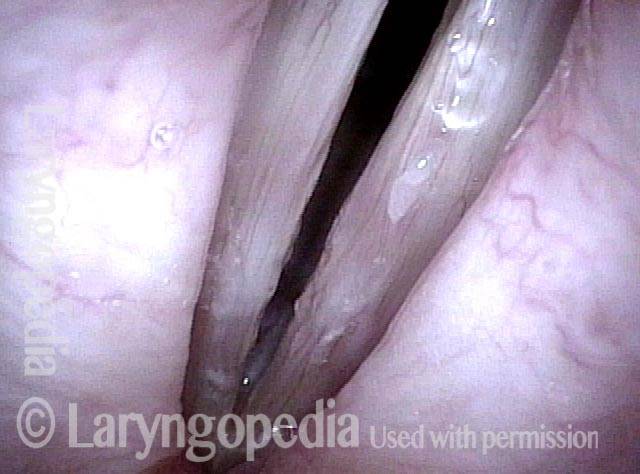
Under standard light. Note the whitish appearance that is visible through the mucosa.
Submucosal fibrosis (1 of 4)
Under standard light. Note the whitish appearance that is visible through the mucosa.
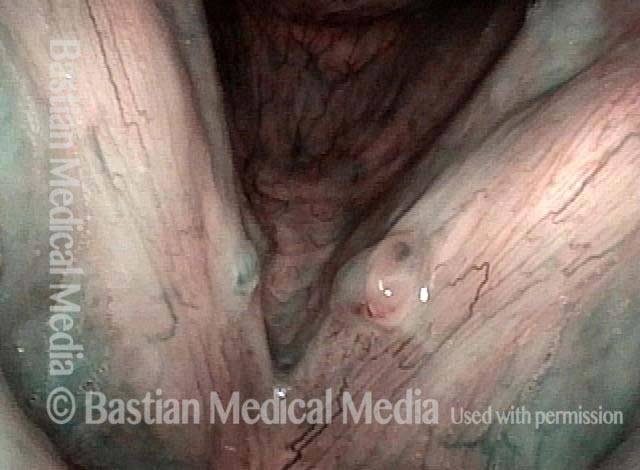
Submucosal fibrosis (2 of 4)
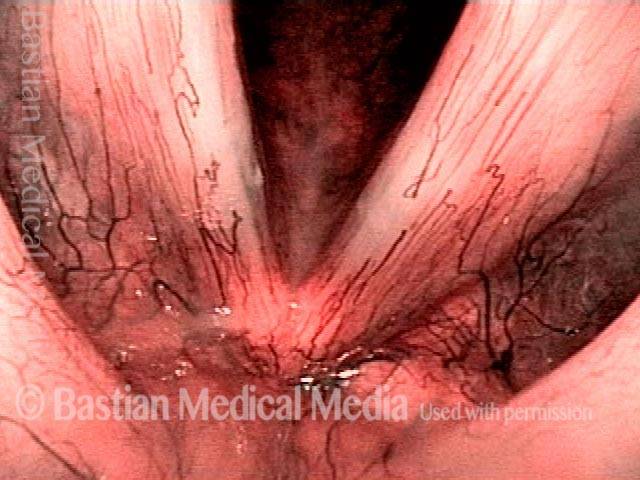
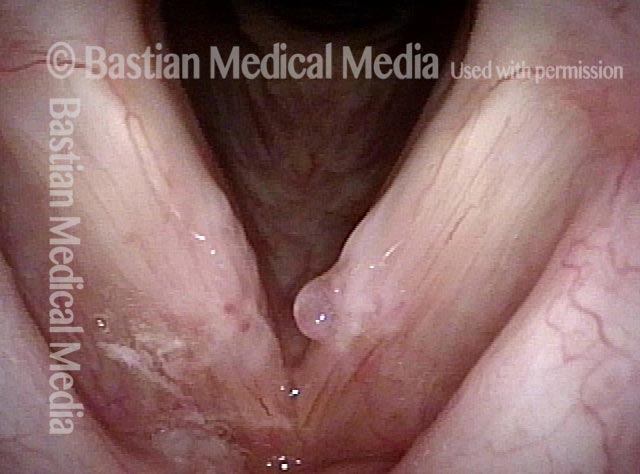
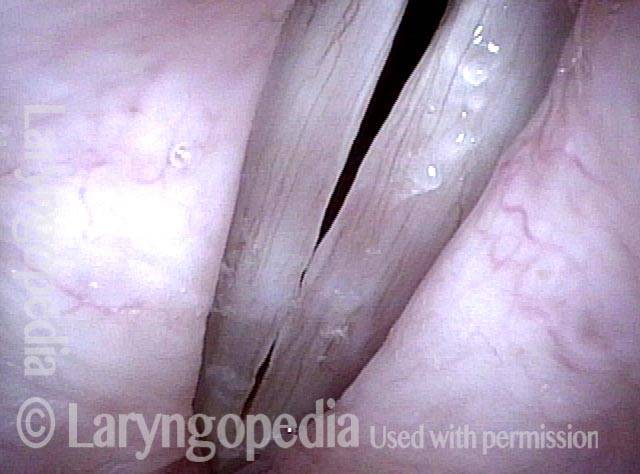
Under narrow-band light.
Submucosal fibrosis (2 of 4)
Under narrow-band light.
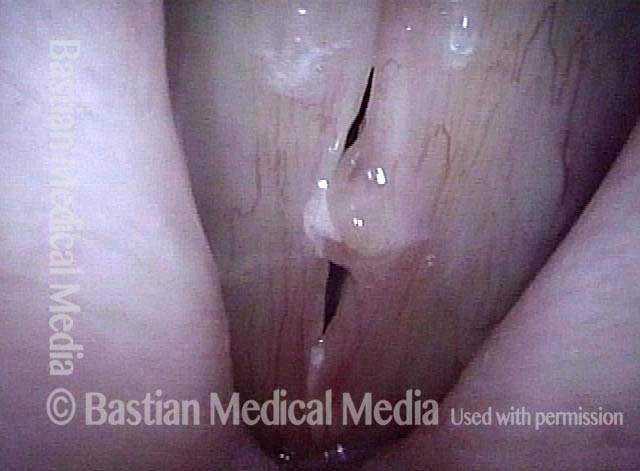
Submucosal fibrosis (3 of 4)
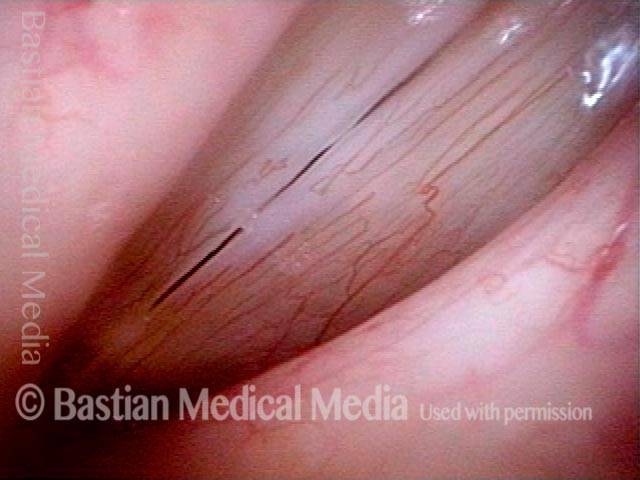
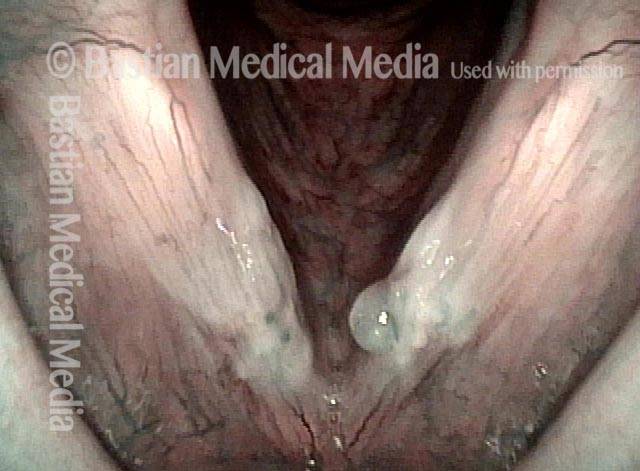
Under strobe light, closed phase of vibration. Shows imperfect match but no obvious protrusion.
Submucosal fibrosis (3 of 4)
Under strobe light, closed phase of vibration. Shows imperfect match but no obvious protrusion.
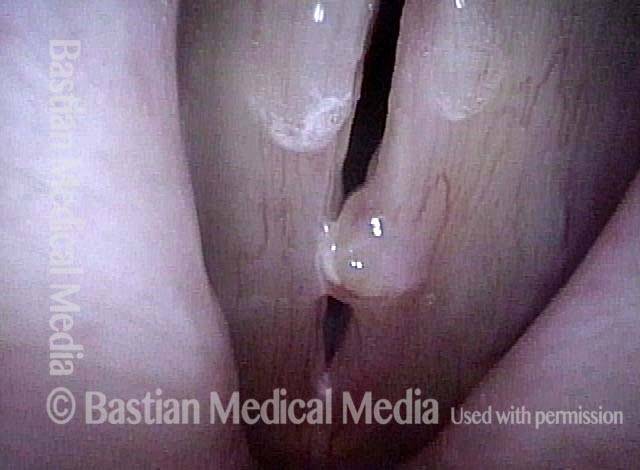
Submucosal fibrosis (4 of 4)
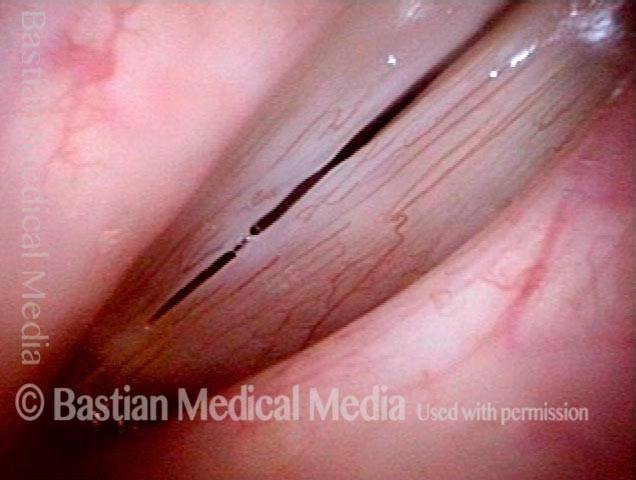
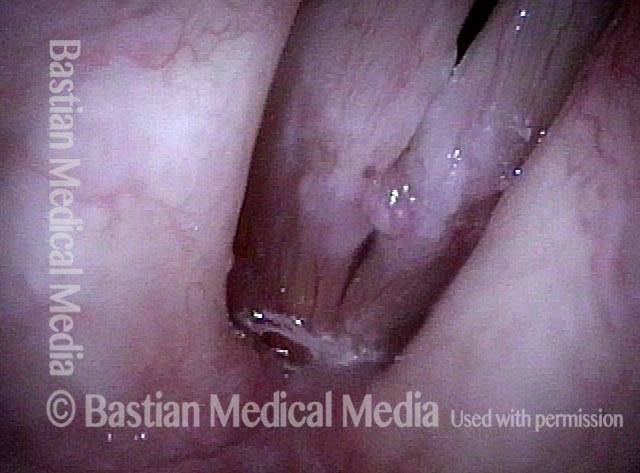
Under strobe light, open phase of vibration. Amplitude of vibration (distance of vibratory separation) not as great as would be expected in a normal larynx; this is due to the stiffening effect of fibrosis.
Submucosal fibrosis (4 of 4)
Under strobe light, open phase of vibration. Amplitude of vibration (distance of vibratory separation) not as great as would be expected in a normal larynx; this is due to the stiffening effect of fibrosis.
Fibrosis as a Base to Nodules, Before and After Surgery
Bilateral polypoid nodules (1 of 8)
Fibrosis as a Base to Nodules, Before and After Surgery
Bilateral polypoid nodules (1 of 8)
Fibrosis as a Base to Nodules, Before and After Surgery
Narrow-band lighting (2 of 8)
At greater magnification, and also under narrow-band light. The area of fibrosis is more clearly seen, now without the dotted lines.
Narrow-band lighting (2 of 8)
At greater magnification, and also under narrow-band light. The area of fibrosis is more clearly seen, now without the dotted lines.
Closed phase (3 of 8)
Closed phase of vibration at ~A4 (440 Hz), as seen under strobe light.
Closed phase (3 of 8)
Closed phase of vibration at ~A4 (440 Hz), as seen under strobe light.
Open phase (4 of 8)
Open phase of vibration also at ~ A4.
Open phase (4 of 8)
Open phase of vibration also at ~ A4.
Two weeks after surgery (5 of 8)
Less than two weeks after surgical removal of the polyps. The faint white zone of margin fibrosis is again seen. Compare with photo 1.
Two weeks after surgery (5 of 8)
Less than two weeks after surgical removal of the polyps. The faint white zone of margin fibrosis is again seen. Compare with photo 1.
Phonation (6 of 8)
Phonation under standard light shows that vocal cord margins now match, and both margins blur; suggesting vibratory flexibility.
Phonation (6 of 8)
Phonation under standard light shows that vocal cord margins now match, and both margins blur; suggesting vibratory flexibility.
Margin fibrosis (7 of 8)
Closed phase of vibration, at ~ A4 (440 Hz), as seen under strobe light. Margin fibrosis seen best here, indicated by the black dotted line. Compare with photo 3.
Margin fibrosis (7 of 8)
Closed phase of vibration, at ~ A4 (440 Hz), as seen under strobe light. Margin fibrosis seen best here, indicated by the black dotted line. Compare with photo 3.
Open phase (8 of 8)
Open phase of vibration. The same pitch (A4) reveals excellent vibratory flexibility and equal amplitude (lateral excursion) of vibration. Compare with photo 4.
Open phase (8 of 8)
Open phase of vibration. The same pitch (A4) reveals excellent vibratory flexibility and equal amplitude (lateral excursion) of vibration. Compare with photo 4.
Submucosal Fibrosis, not Leukoplakia or Candida
Submucosal fibrosis (1 of 3)
Middle-aged man who works in sales and also uses voice aggressively during regular athletic activity. Voice is raspy and variable. Note here "plaques" of white material that appear to be submucosal and extend beyond the obvious areas (dotted lines). No erythematous "surround" such as would be seen with candida.
Submucosal fibrosis (1 of 3)
Middle-aged man who works in sales and also uses voice aggressively during regular athletic activity. Voice is raspy and variable. Note here "plaques" of white material that appear to be submucosal and extend beyond the obvious areas (dotted lines). No erythematous "surround" such as would be seen with candida.
Closed phase (2 of 3)
Closed phase vibration, strobe light at F4, again showing submucosal fibrosis.
Closed phase (2 of 3)
Closed phase vibration, strobe light at F4, again showing submucosal fibrosis.
Open phase (3 of 3)
Open phase of vibration, also at F4.
Open phase (3 of 3)
Open phase of vibration, also at F4.
An Extreme Example of Protective Fibrosis Deposits
Extroverted elementary teacher (1 of 6)
Elementary teacher and major extrovert is grossly hoarse. Here you can see the fibrotic-appearing injuries bilaterally and an extra translucent polypoid component on the left cord (right of photo).
Extroverted elementary teacher (1 of 6)
Elementary teacher and major extrovert is grossly hoarse. Here you can see the fibrotic-appearing injuries bilaterally and an extra translucent polypoid component on the left cord (right of photo).
Submucosal fibrosis (2 of 6)
Under narrow band light, the white area is not hazy leukoplakia, but instead submucosal fibrosis, deposited as a protection against mucosal vibratory collision/ shearing injury.
Submucosal fibrosis (2 of 6)
Under narrow band light, the white area is not hazy leukoplakia, but instead submucosal fibrosis, deposited as a protection against mucosal vibratory collision/ shearing injury.
Phonatory view (3 of 6)
Under strobe light, closure is imperfect due to the mid-cord elevations.
Phonatory view (3 of 6)
Under strobe light, closure is imperfect due to the mid-cord elevations.
Open phase (4 of 6)
Open phase of vibration with small amplitude and absent “mucosal wave” due to stiffness of the mucosa.
Open phase (4 of 6)
Open phase of vibration with small amplitude and absent “mucosal wave” due to stiffness of the mucosa.
Post microsurgery, open phase (5 of 6)
A week after vocal cord microsurgery, voice is markedly improved. No attempt was made to remove all of the fibrosis, but only to straighten the vocal cord margins. Open phase of vibration at F5.
Post microsurgery, open phase (5 of 6)
A week after vocal cord microsurgery, voice is markedly improved. No attempt was made to remove all of the fibrosis, but only to straighten the vocal cord margins. Open phase of vibration at F5.
Post microsurgery, closed phase (6 of 6)
Closed phase of vibration at same pitch shows that some margin swelling remains. The patient also has MTD; posterior cords are widely separated.
Post microsurgery, closed phase (6 of 6)
Closed phase of vibration at same pitch shows that some margin swelling remains. The patient also has MTD; posterior cords are widely separated.
Anterior Saccular Cyst
Anterior saccular cyst (1 of 4)
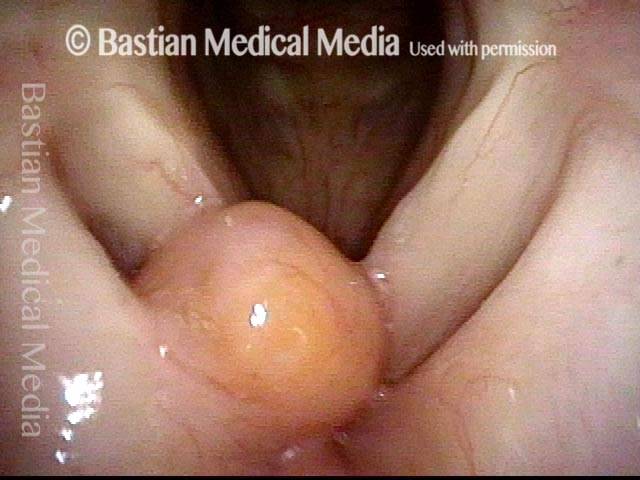
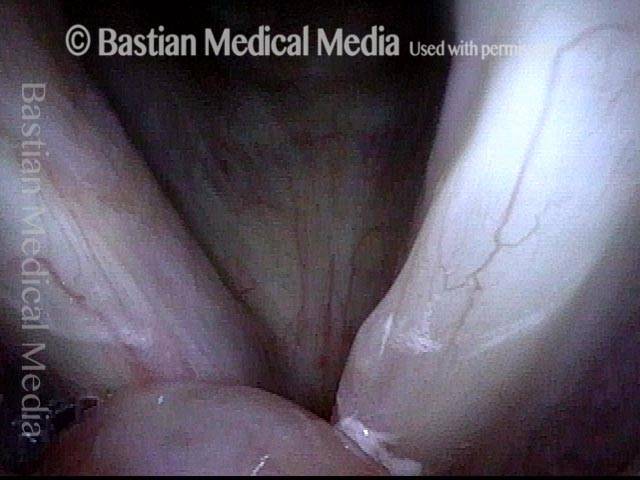
Breathing position, with a saccular cyst protruding from the right anterior ventricle (left of image). The cyst’s location, color, and superficial vessels indicate that it is neither a polyp nor granuloma.
Anterior saccular cyst (1 of 4)
Breathing position, with a saccular cyst protruding from the right anterior ventricle (left of image). The cyst’s location, color, and superficial vessels indicate that it is neither a polyp nor granuloma.
Closer view (2 of 4)
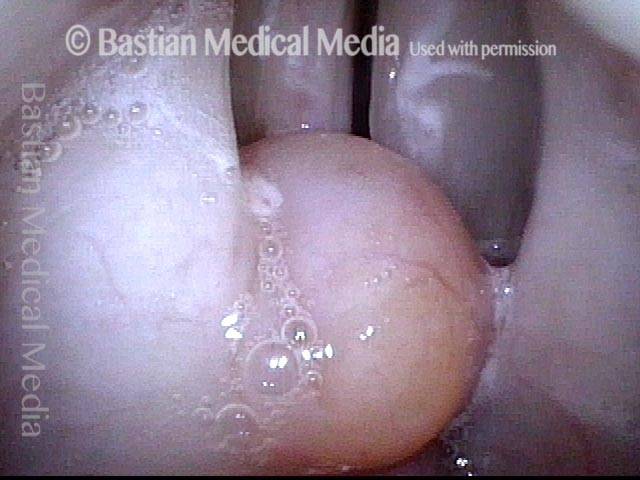
Still closer view (under strobe light), breathing position, showing that the cyst does not arise from the cord, but appears to be depressing the anterior end of the right cord (left of image) slightly. On the left cord is an incidental finding of margin swelling, which is unsurprising in this very talkative individual.
Closer view (2 of 4)
Still closer view (under strobe light), breathing position, showing that the cyst does not arise from the cord, but appears to be depressing the anterior end of the right cord (left of image) slightly. On the left cord is an incidental finding of margin swelling, which is unsurprising in this very talkative individual.
Cyst vibrates when speaking (3 of 4)
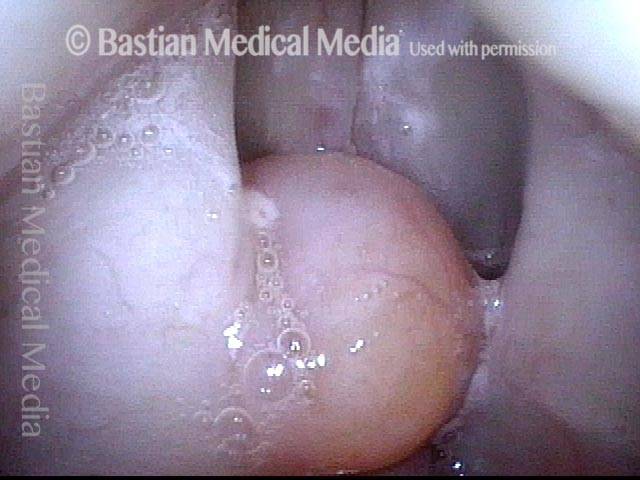
Phonation, strobe light, open phase of vibration. The laryngeal vestibule between the false cords is partially blocked. The cyst occasionally participates in vibration, making an extra sound.
Cyst vibrates when speaking (3 of 4)
Phonation, strobe light, open phase of vibration. The laryngeal vestibule between the false cords is partially blocked. The cyst occasionally participates in vibration, making an extra sound.
Anterior saccular cyst (4 of 4)
Phonation, strobe light, closed phase of vibration.
Anterior saccular cyst (4 of 4)
Phonation, strobe light, closed phase of vibration.