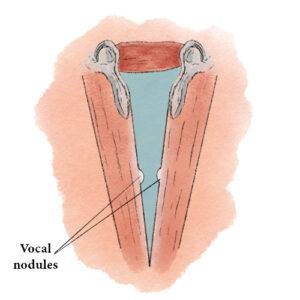
Vocal Nodules
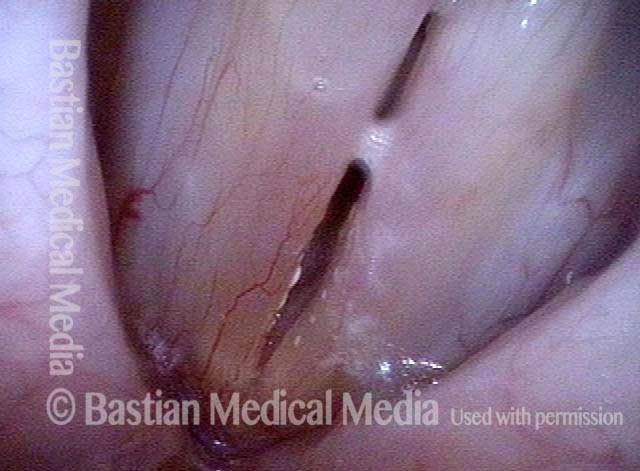
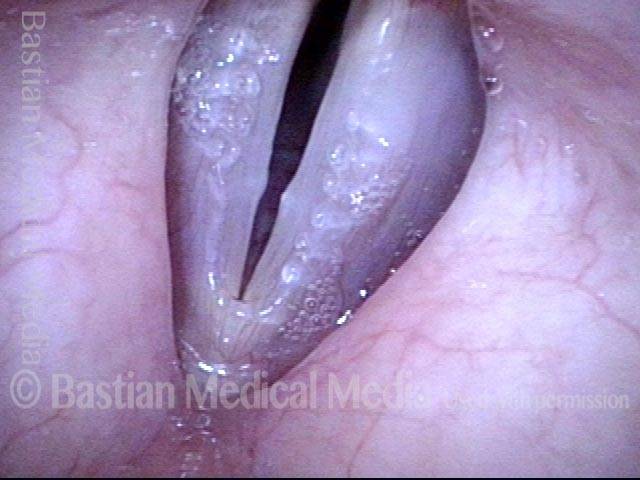
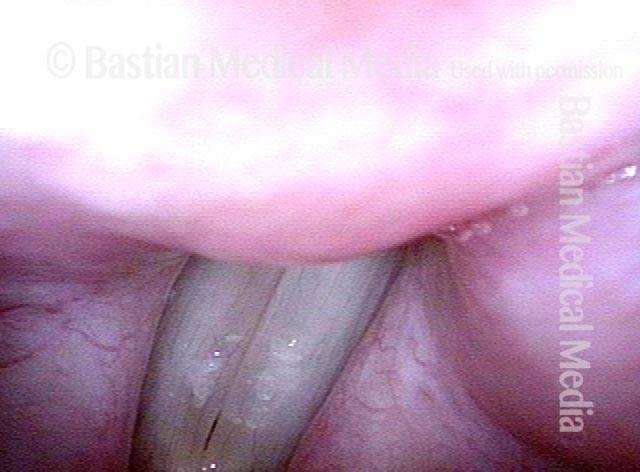
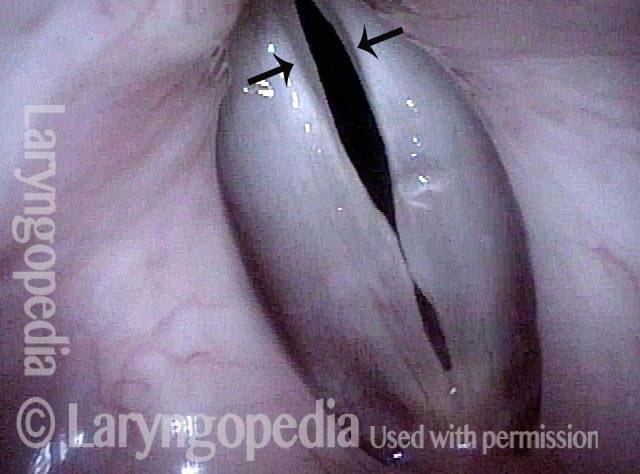
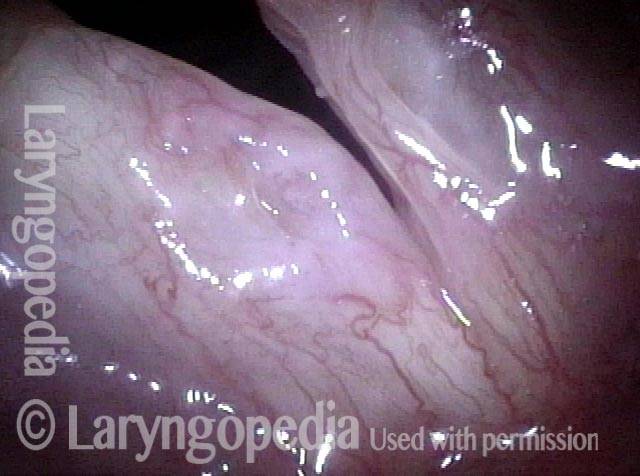
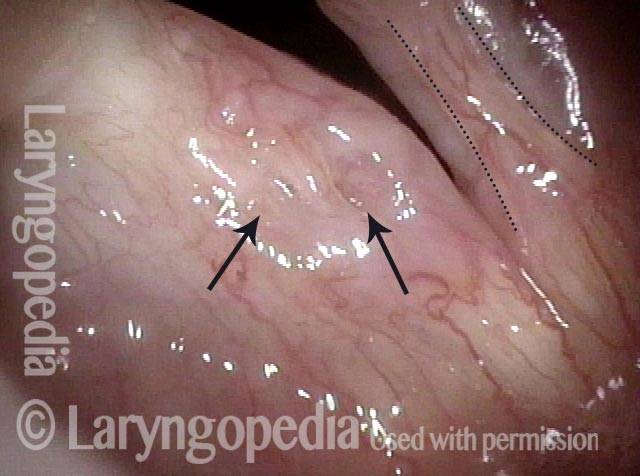
Small chronic swellings that appear in the junction of the middle and anterior thirds of the vocal cord. These swellings, or nodules (nodes), are vibratory injuries caused by vocal overuse.
Symptoms
The most obvious symptom of medium-to-large nodules tends to be hoarseness. The top 5 symptoms for nodules of any size may include:
- Difficulty with high, soft singing;
- Day-to-day variability of vocal capability and clarity;
- A sense of increased effort to produce voice, especially for singing;
- Reduced endurance, so that the voice becomes husky or “tired” after less voice use than formerly;
- Phonatory onset delays, when there is a slight hiss of air before the voice “pops in.”
Etiology
When you overuse your voice, your body tries to cushion the vocal cords by pooling together edema (fluid) beneath the vocal cord mucosa (the surface layer of the cords); this pooled edema is like a small, low-profile blister on your finger. If after a few days you stop overusing your voice, the edema disperses readily, within a few days, and this “blister” on the vocal cords vanishes.
If, however, the amount or manner of voice use remains excessive for many weeks or months, then more chronic swelling materials (no longer just edema fluid) are laid down by the body, and the vocal cords develop true nodules.
Why Nodes Affect the Voice
In either case (acute swellings or chronic nodules), this injury to the mucosa can impair the voice in two ways: it reduces the vibratory flexibility of the mucosa, and it interferes with the accurate match of the cords when they come together to produce voice. This impairment causes the voice to be hoarse or, more subtly, to suffer from onset delays, difficulty with high notes, and other similar problems.
Treatment
Nodules will often dissipate, with the help of rest and perhaps speech/voice therapy, over a period of weeks or months. Sometimes, the swellings are so stubborn that microsurgery is required.
How Is the Voice after Treatment?
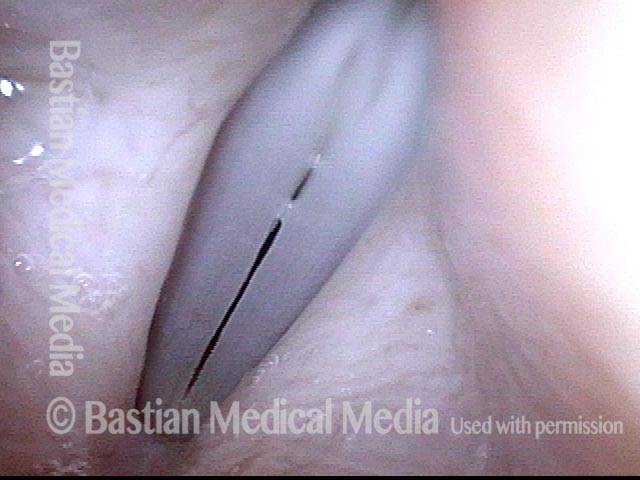
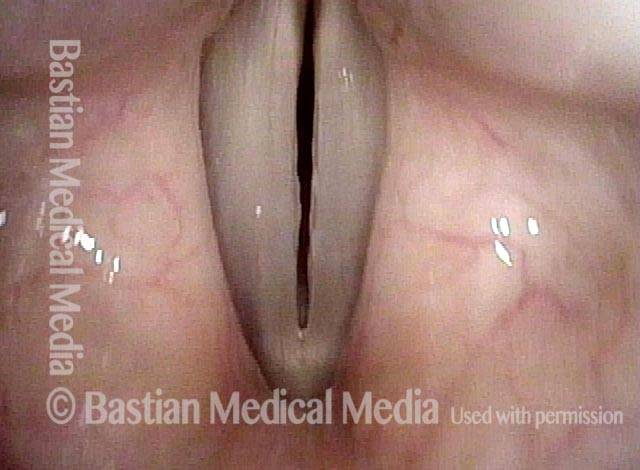
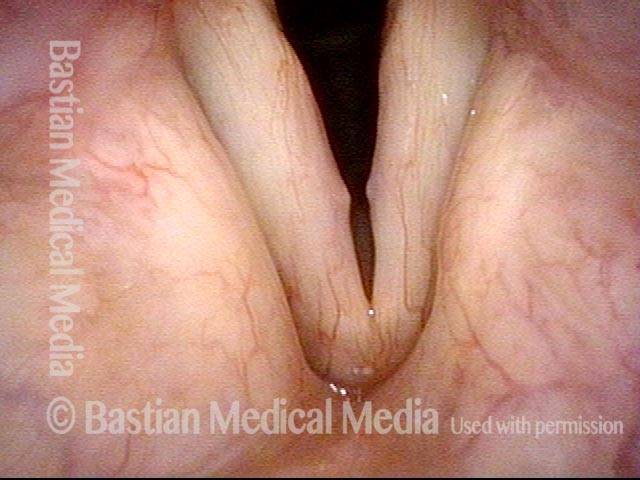
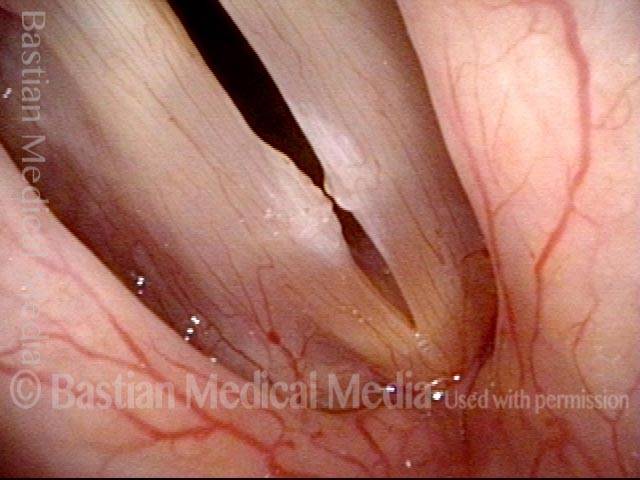
Vocal nodules’ effect on the voice, BEFORE surgical removal (see this patient’s photos just below):
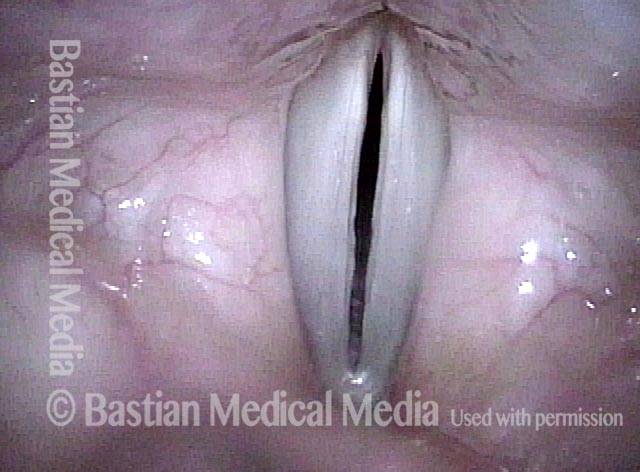
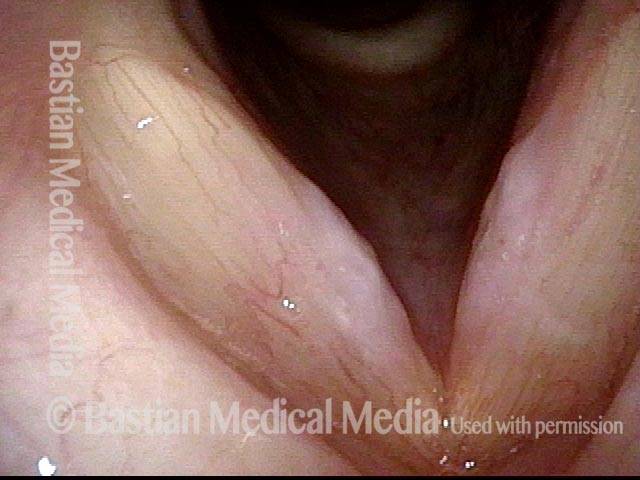
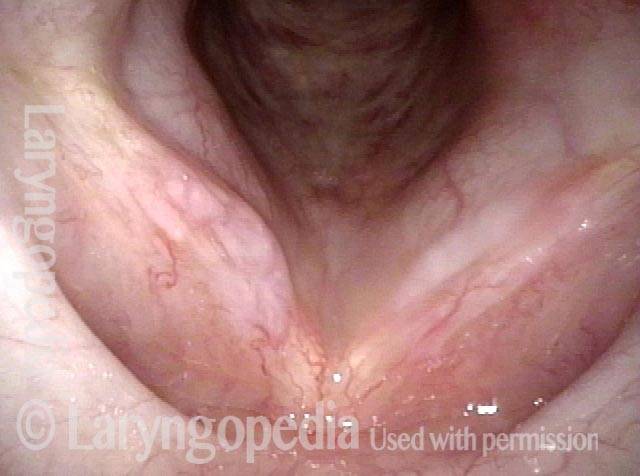
Same patient, seven weeks AFTER surgical removal of the vocal nodules:
Vocal Nodules, Before and After Surgery
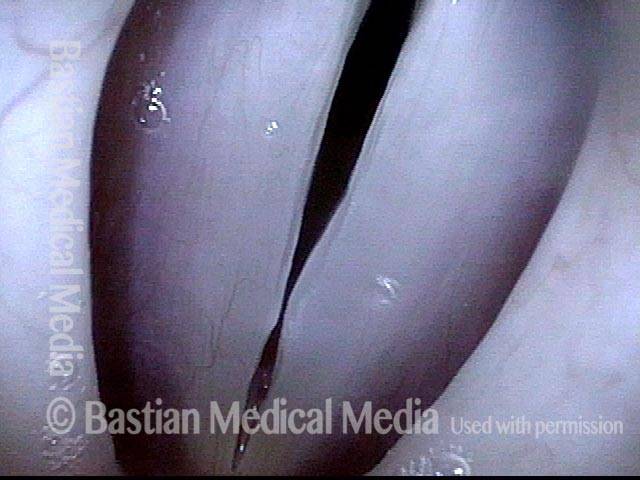
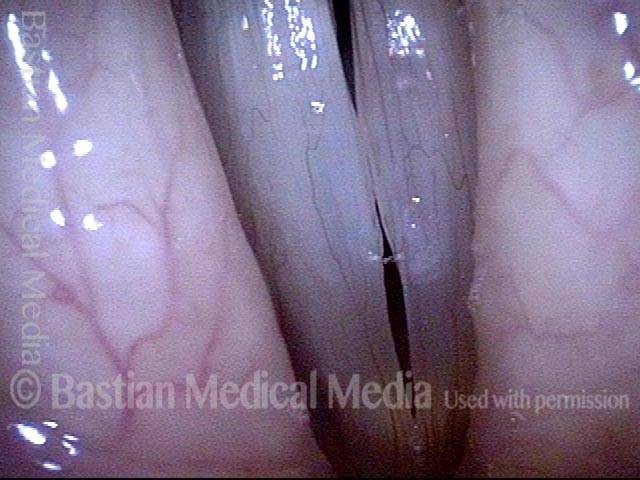
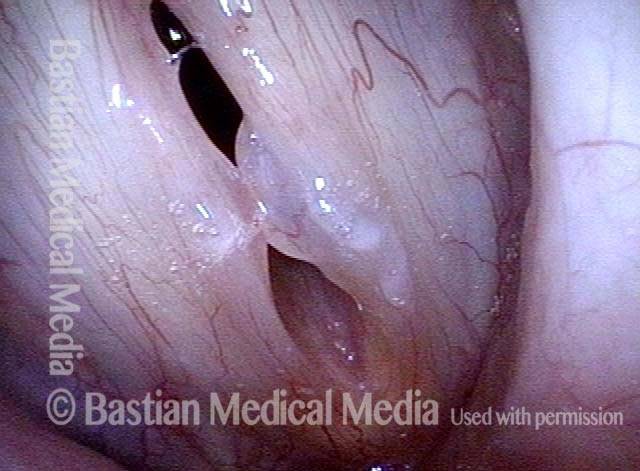
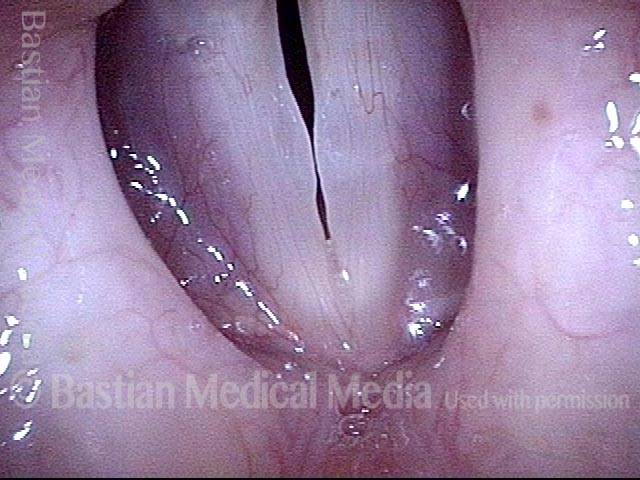
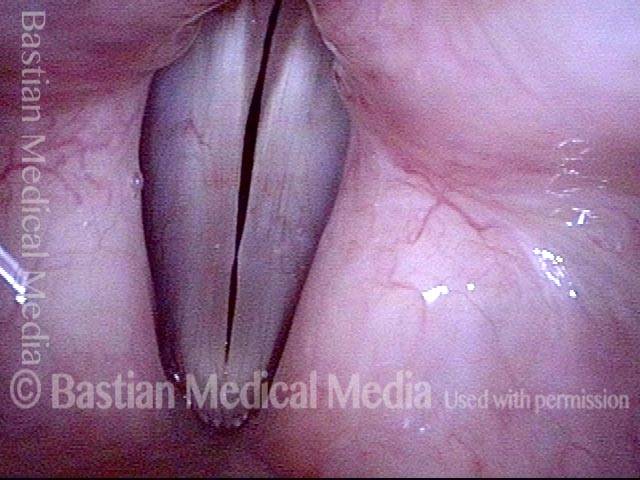
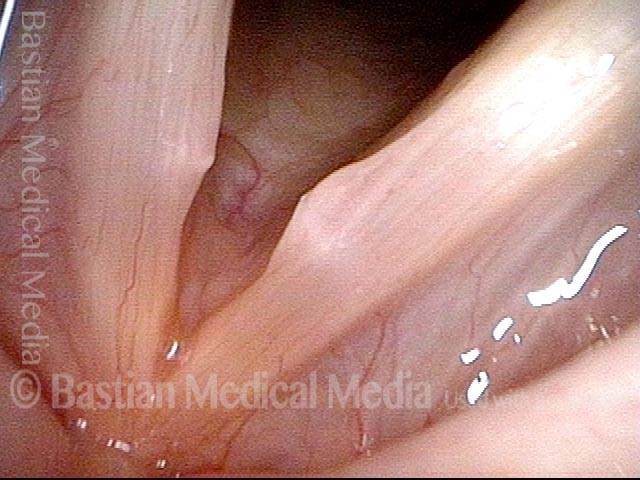
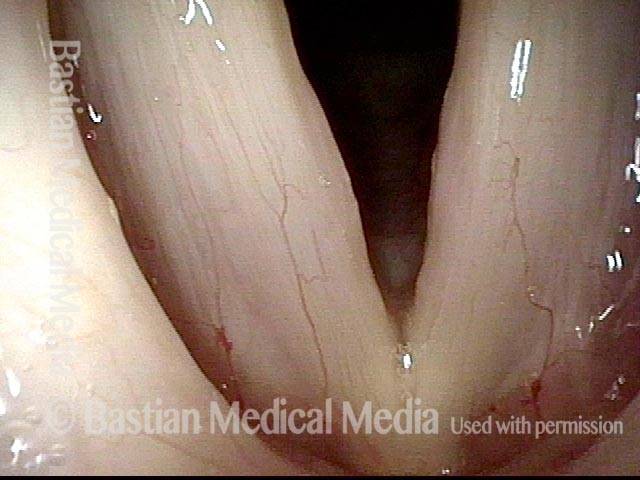
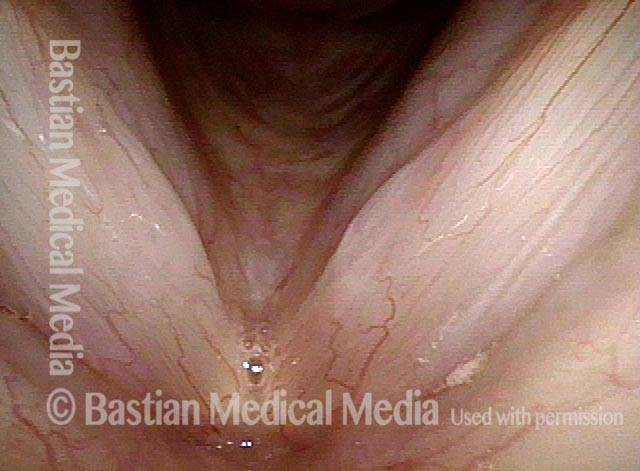
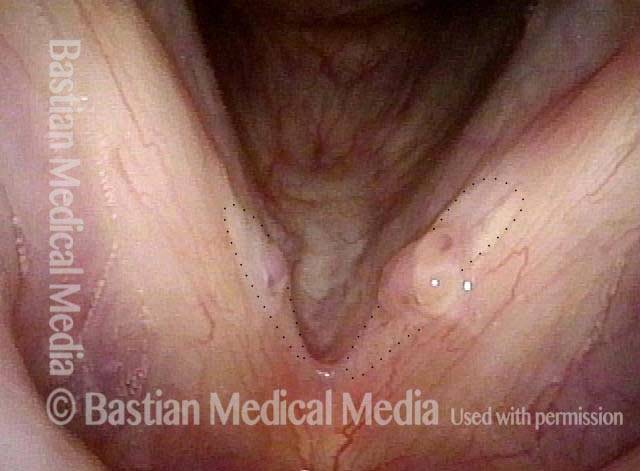
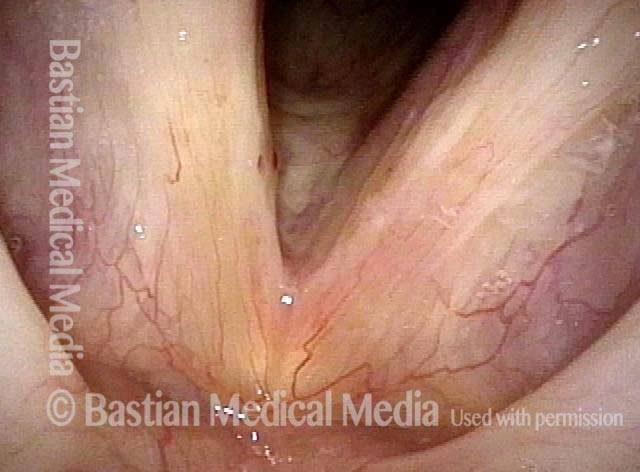
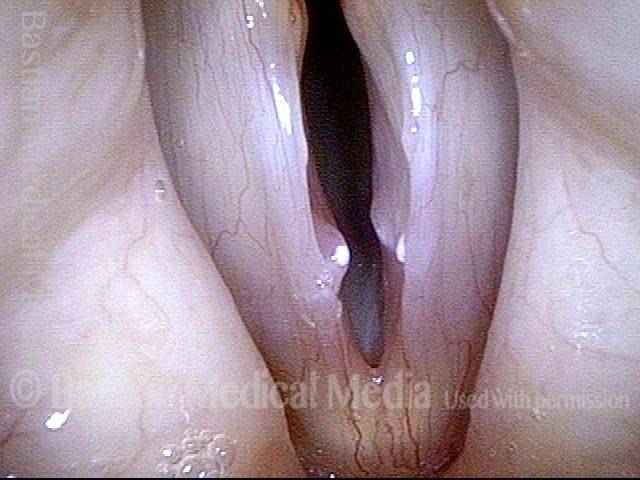
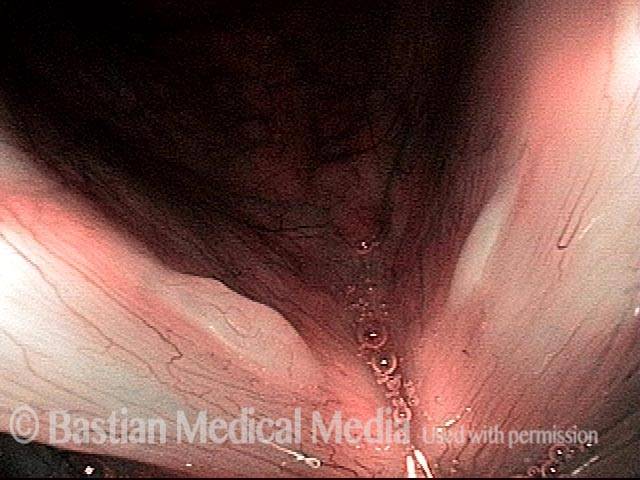
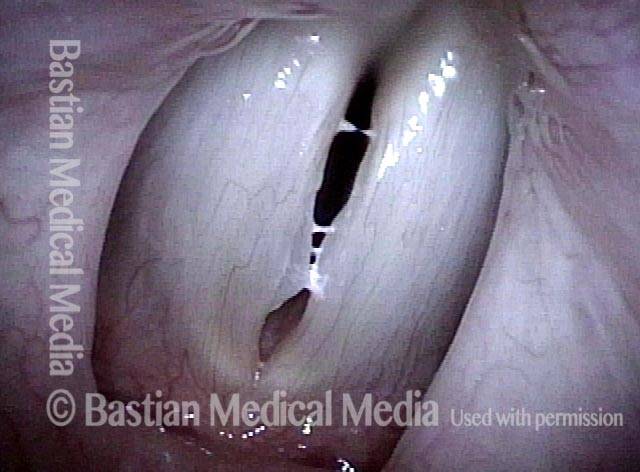
Vocal nodules (1 of 6)
Vocal nodules (1 of 6)
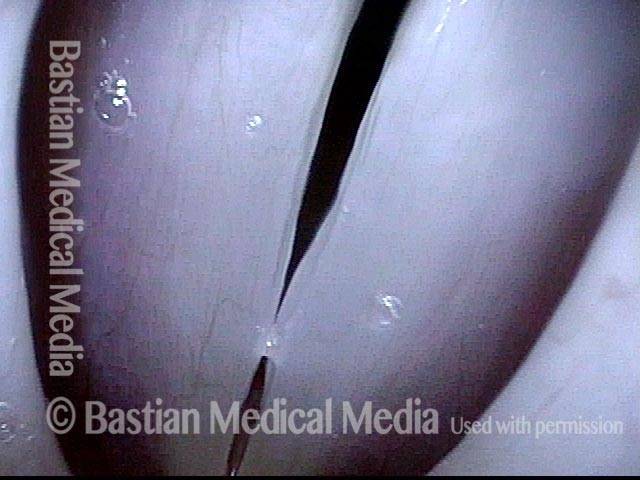
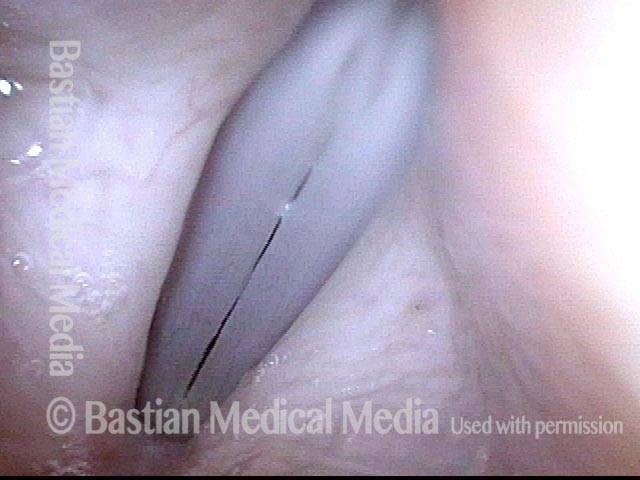
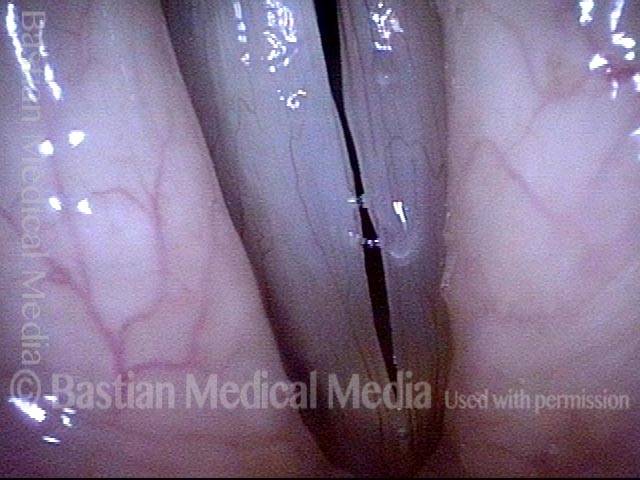
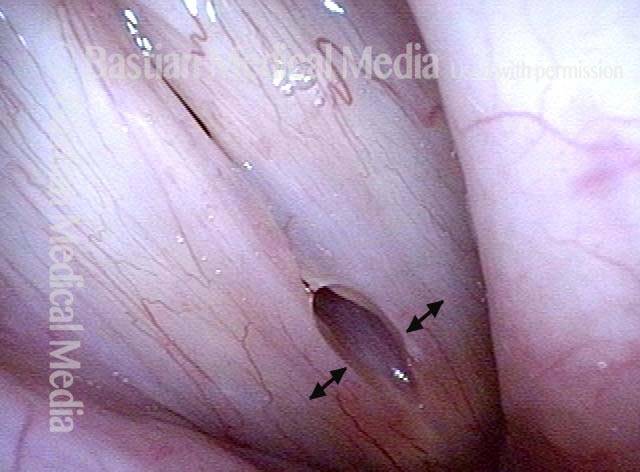
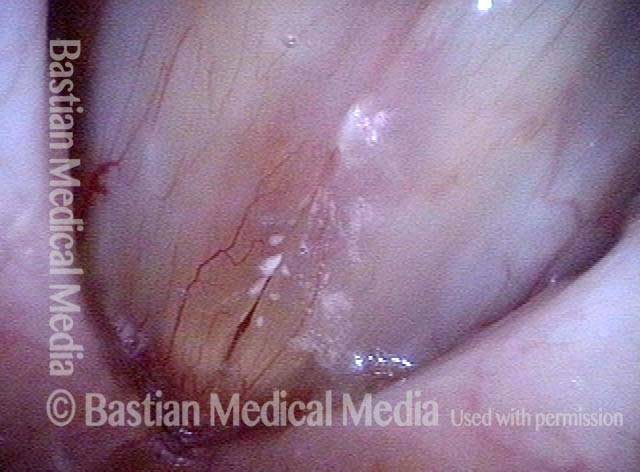
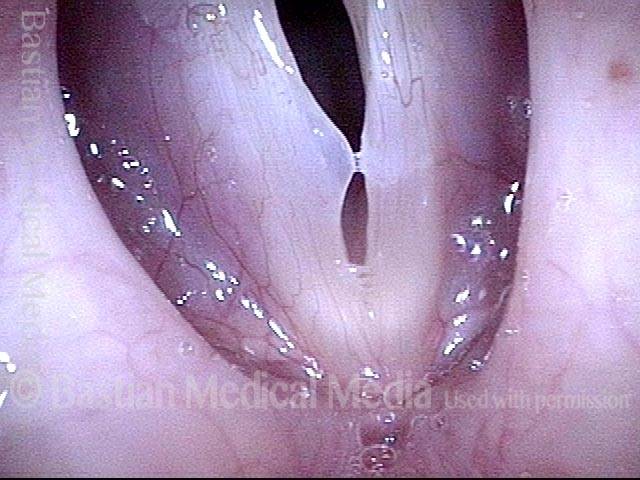
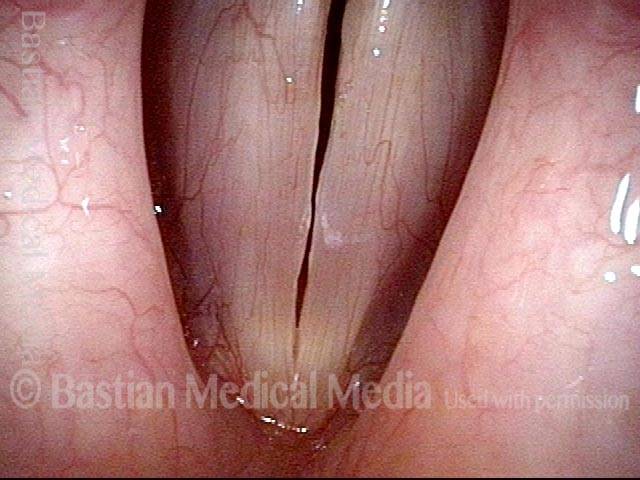
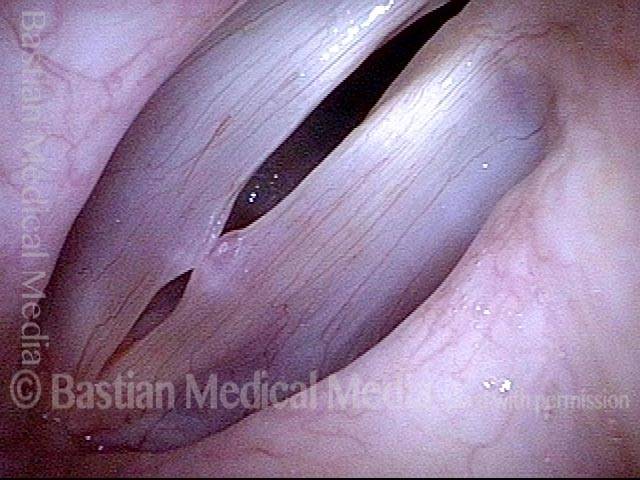
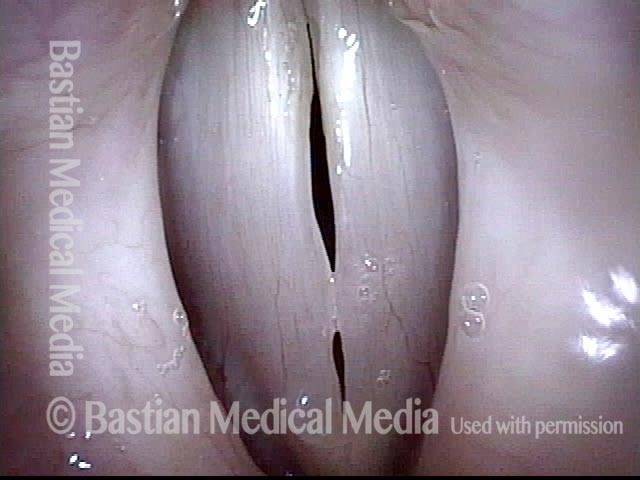
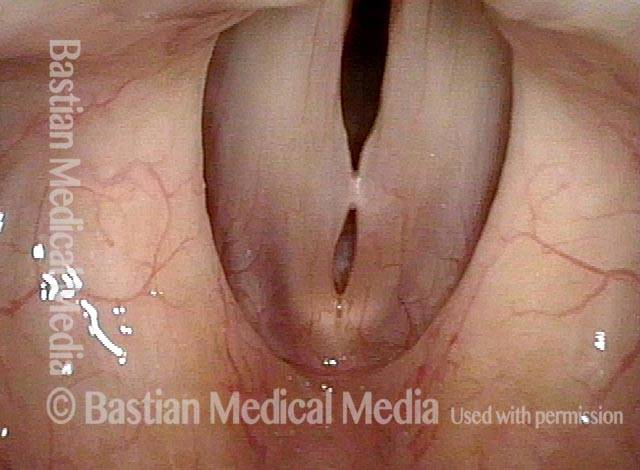
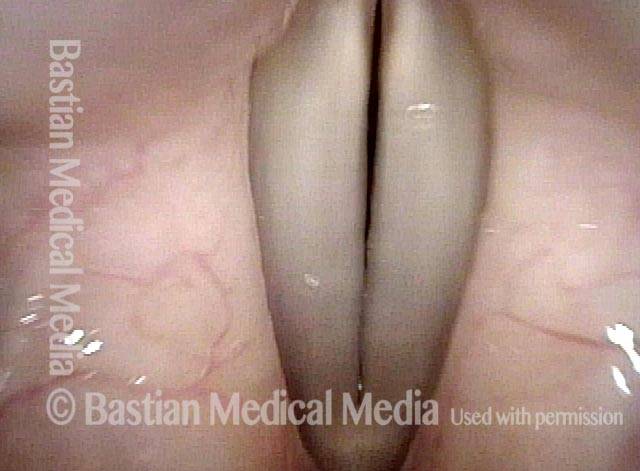
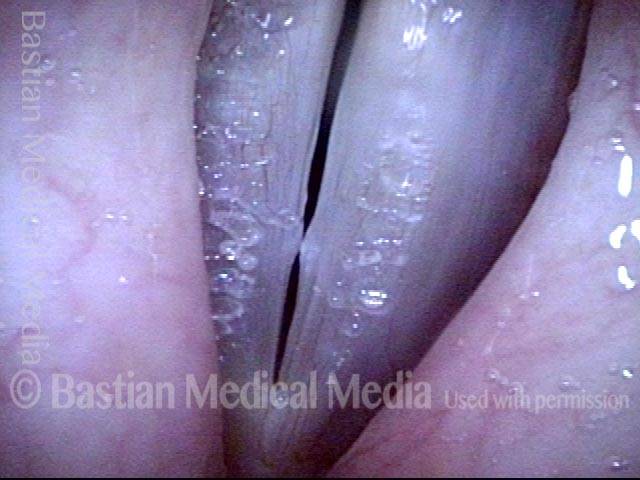
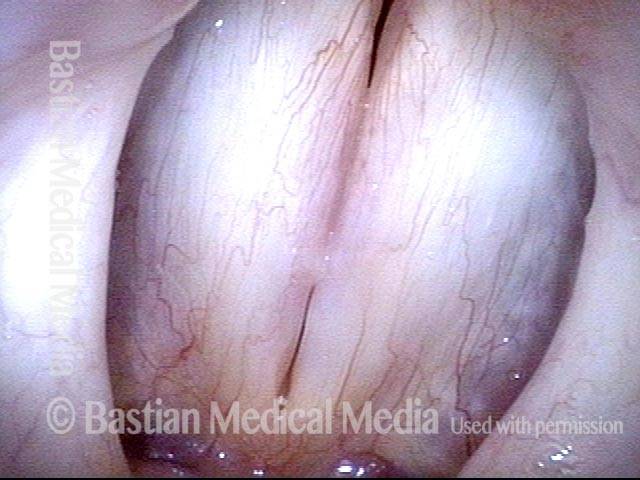
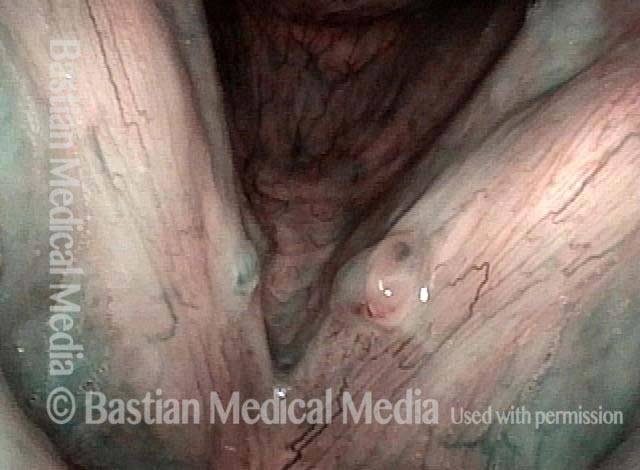
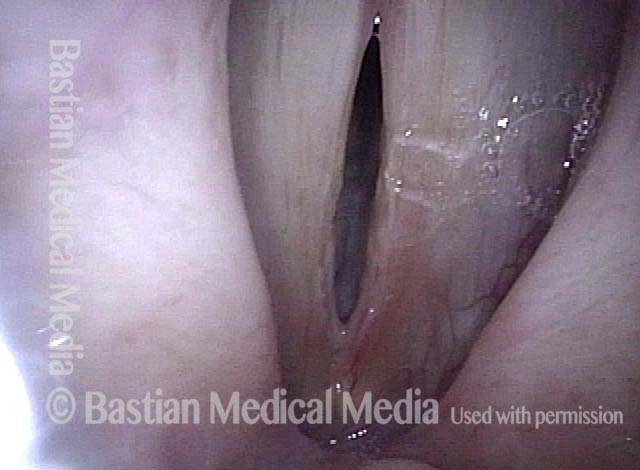
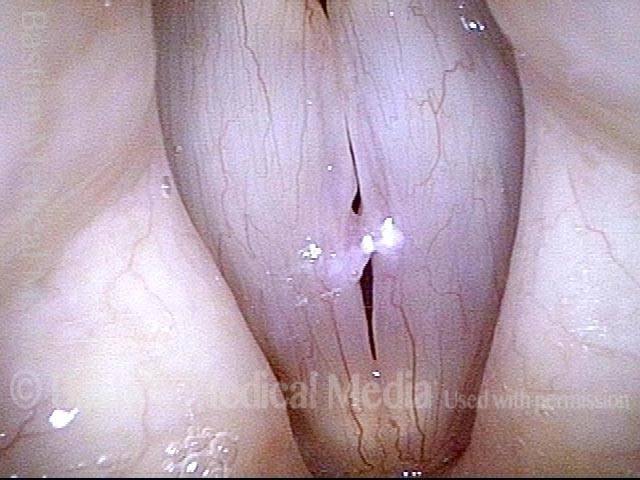
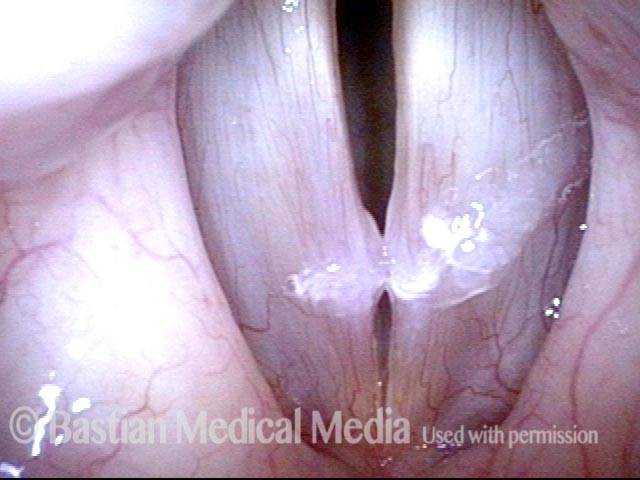
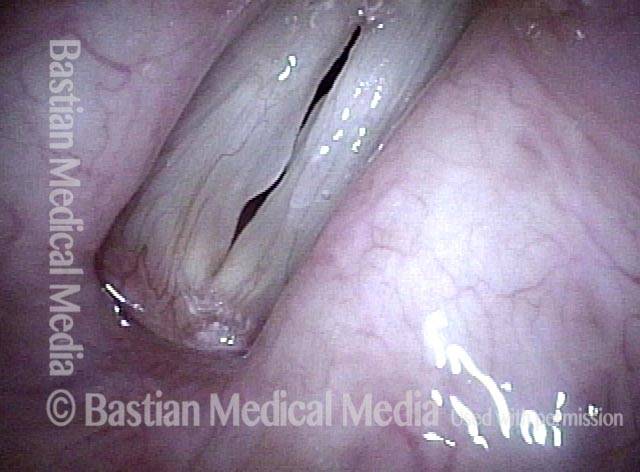
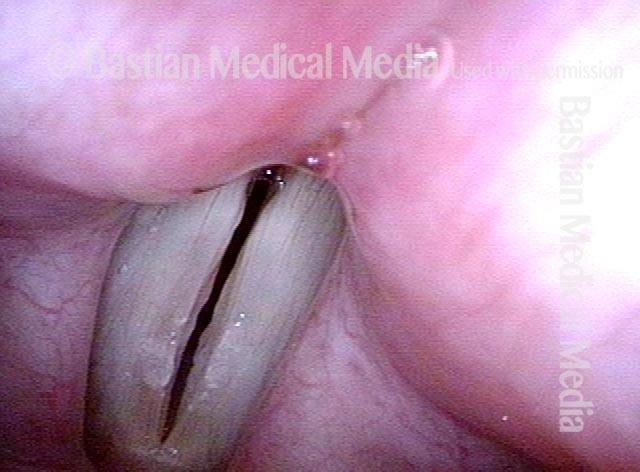
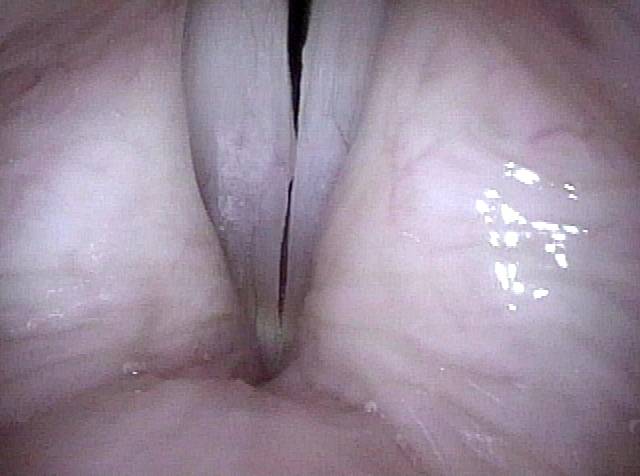
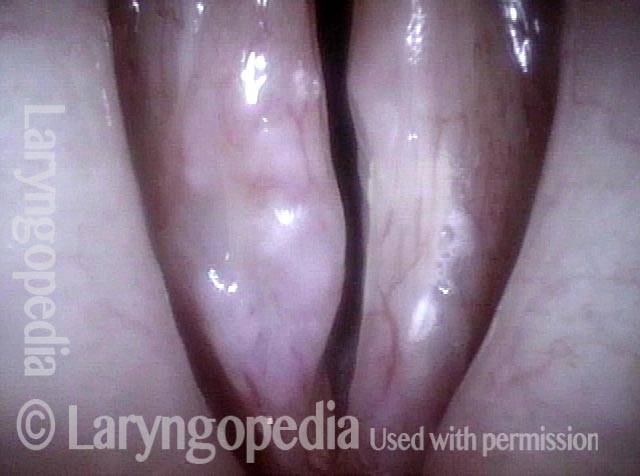
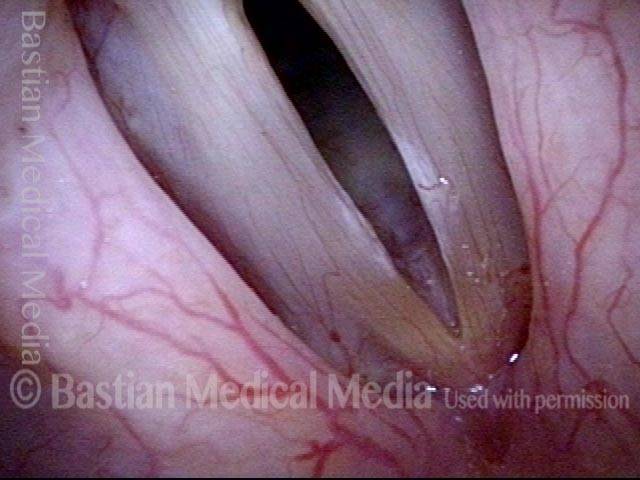
Breathy voice (2 of 6)
Breathy voice (2 of 6)
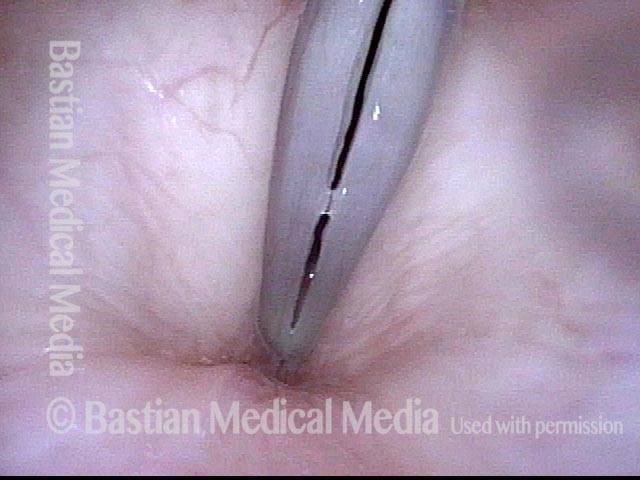
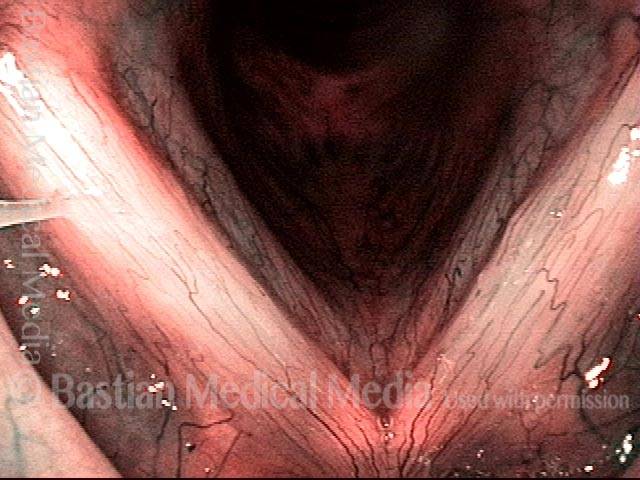
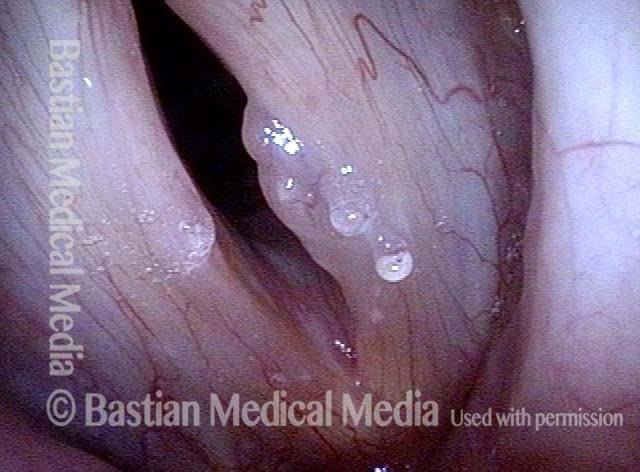
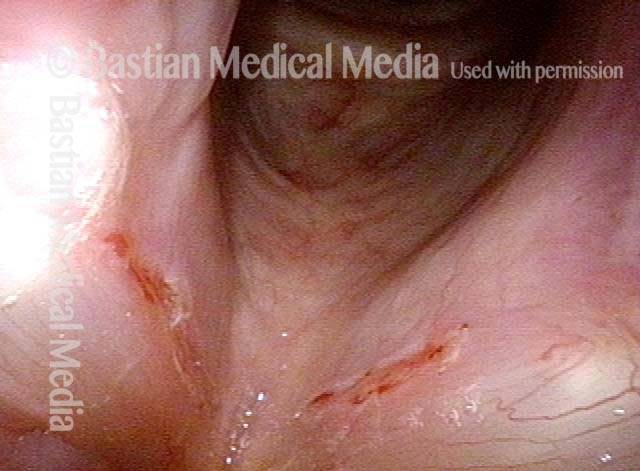
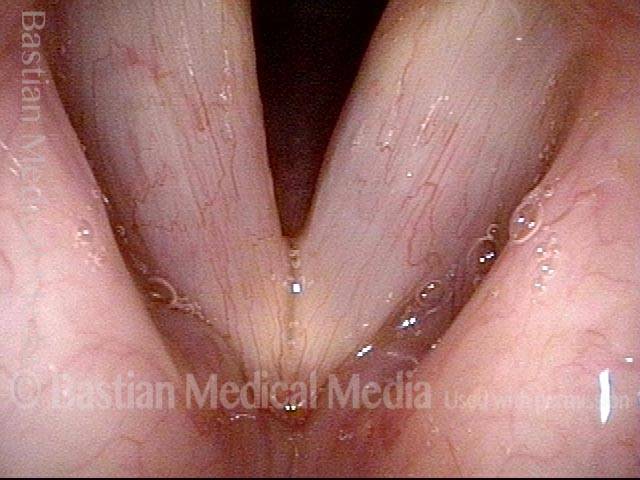
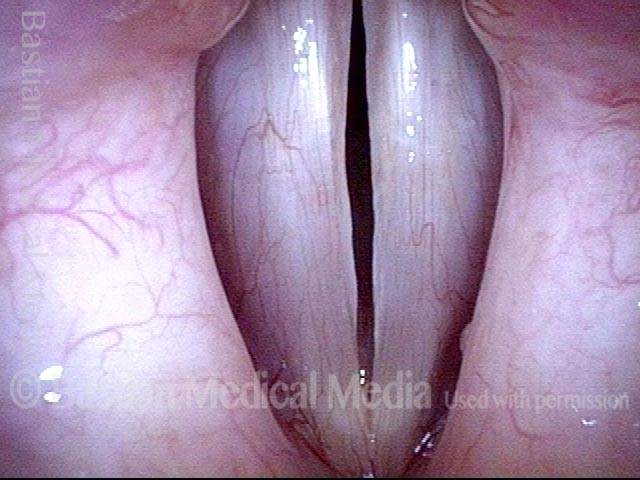
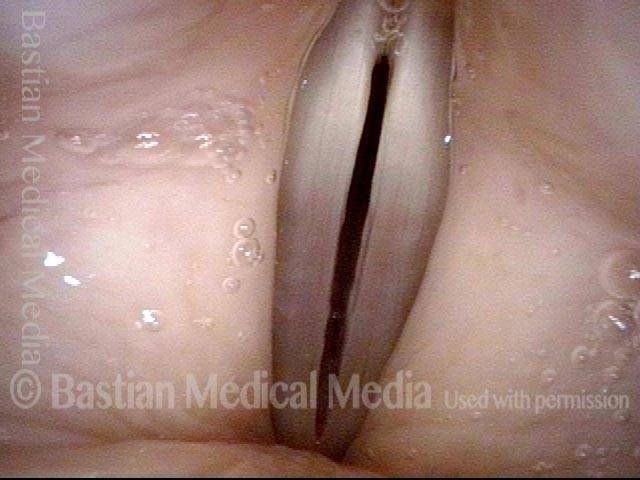
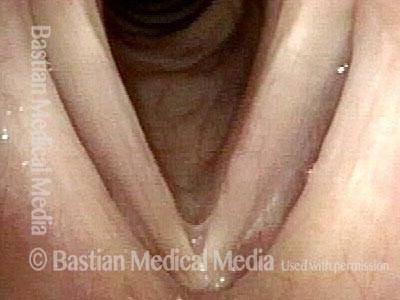
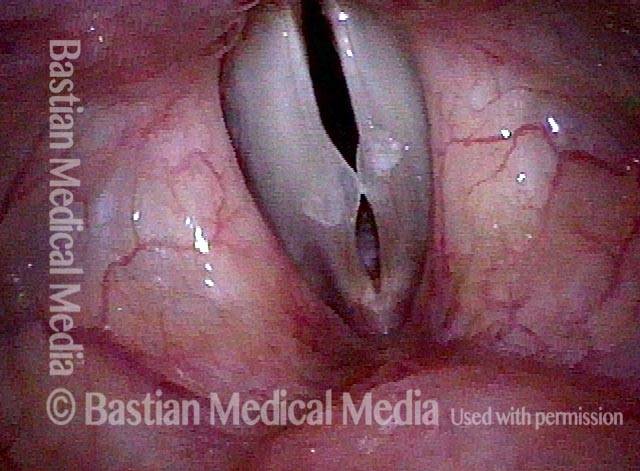
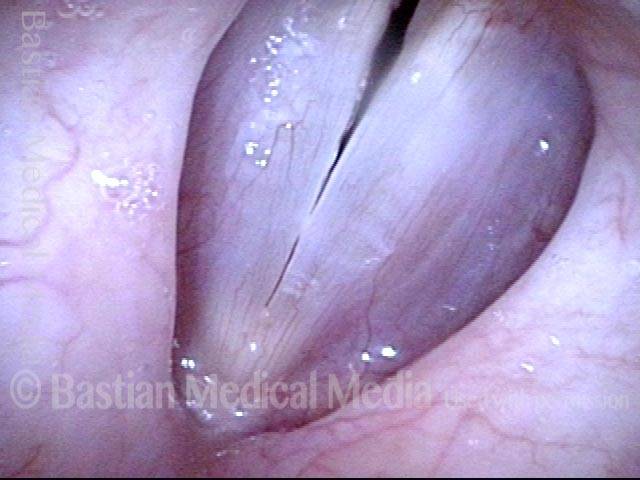
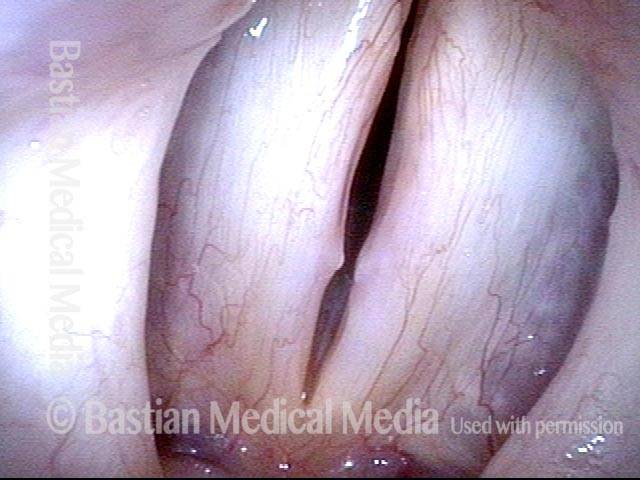
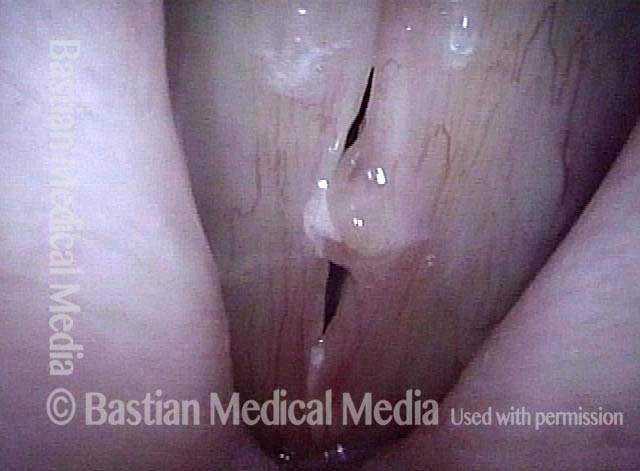
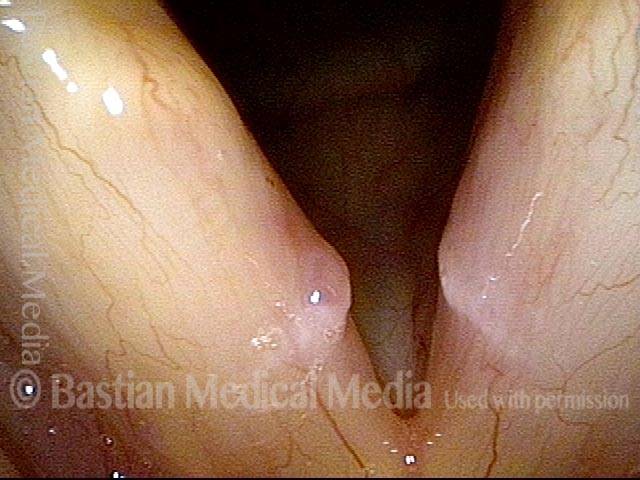
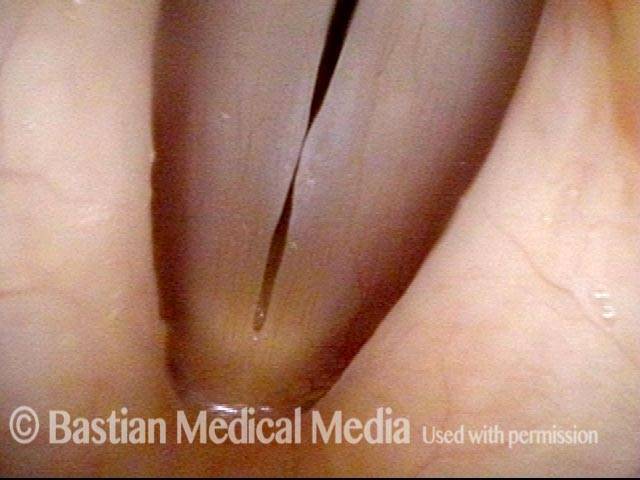
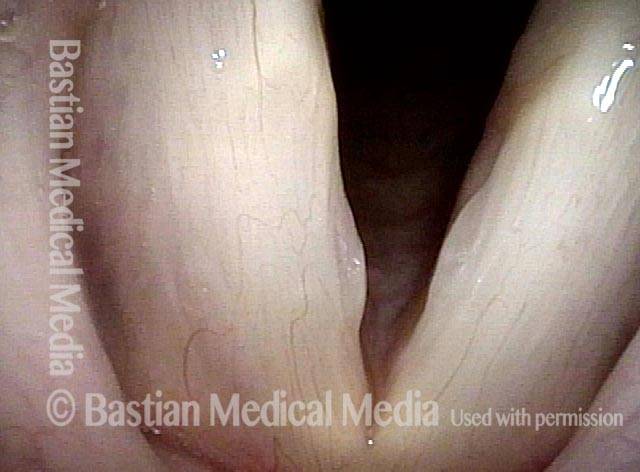
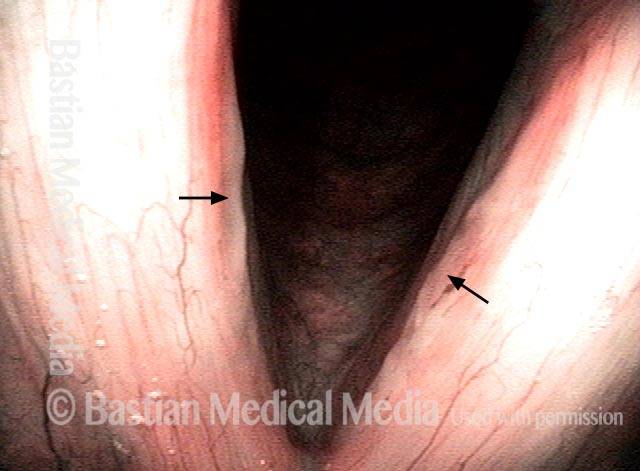
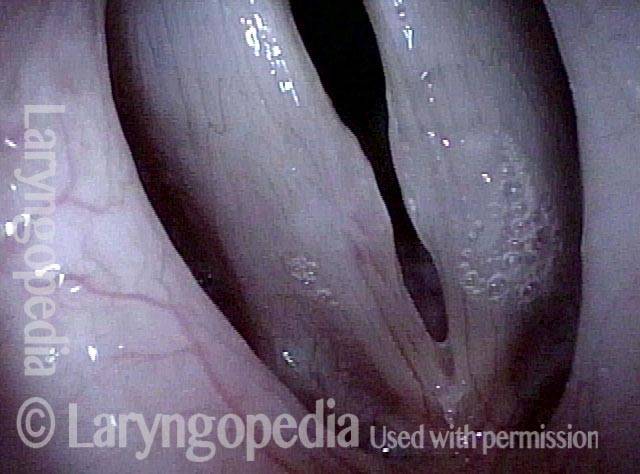
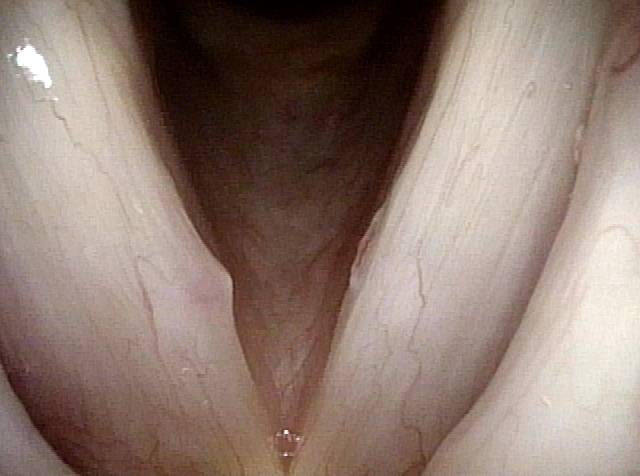
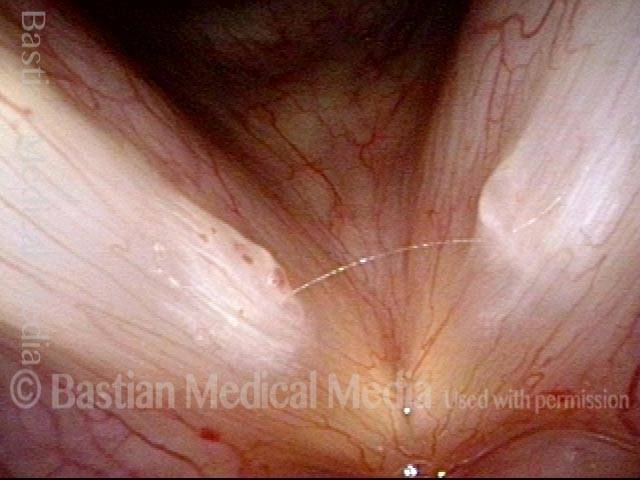
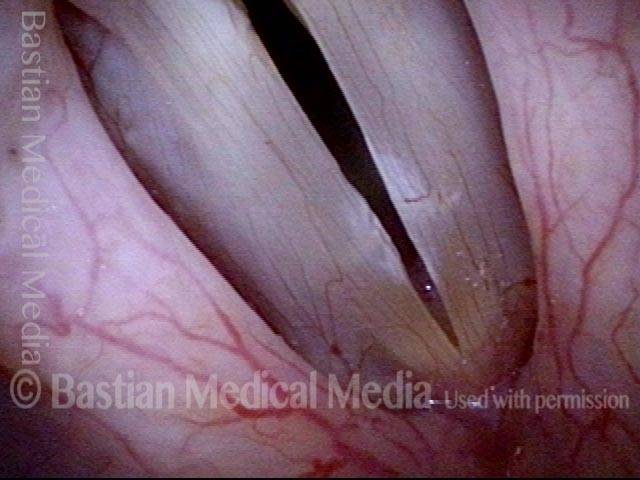
1 week after surgery (3 of 6)
1 week after surgery (3 of 6)
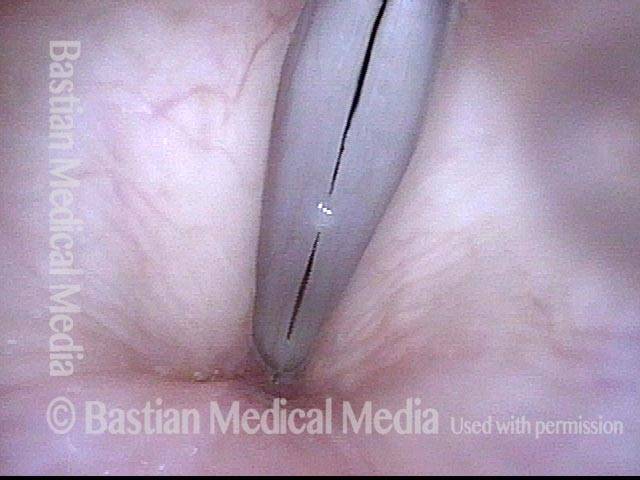
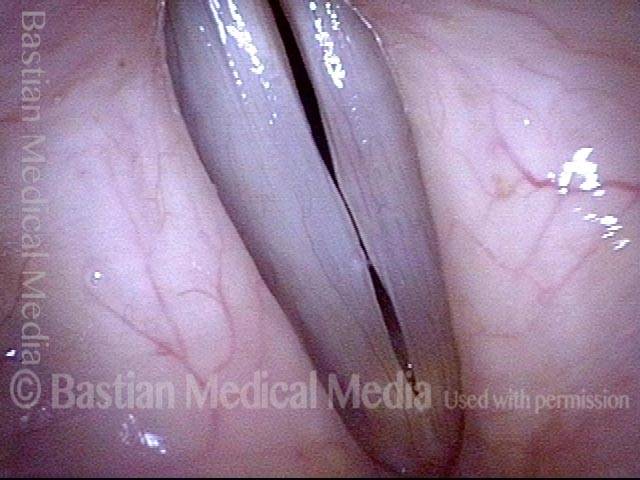
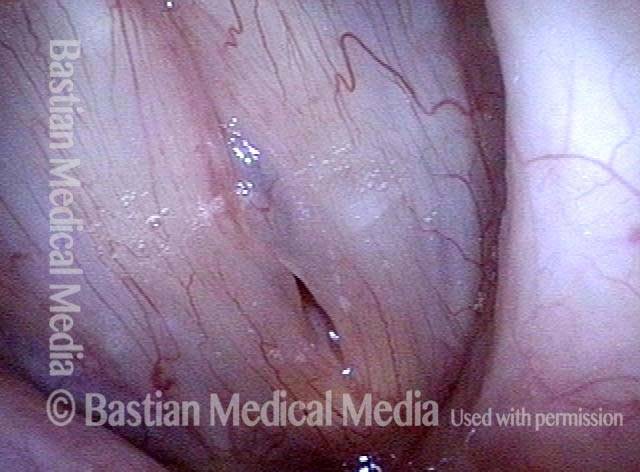
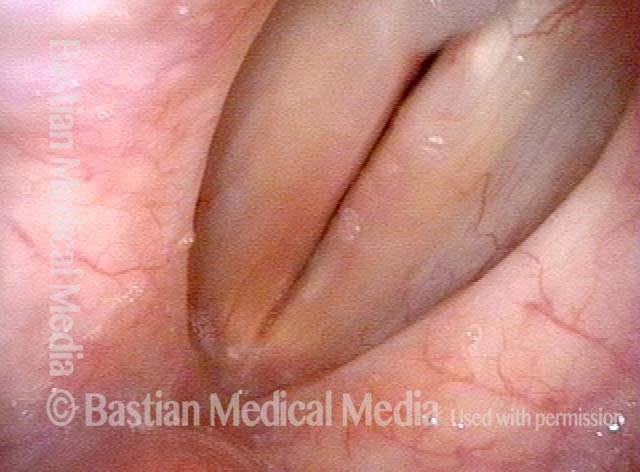
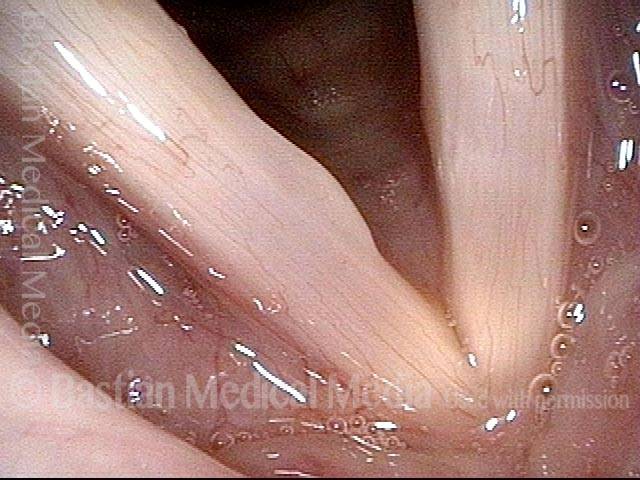
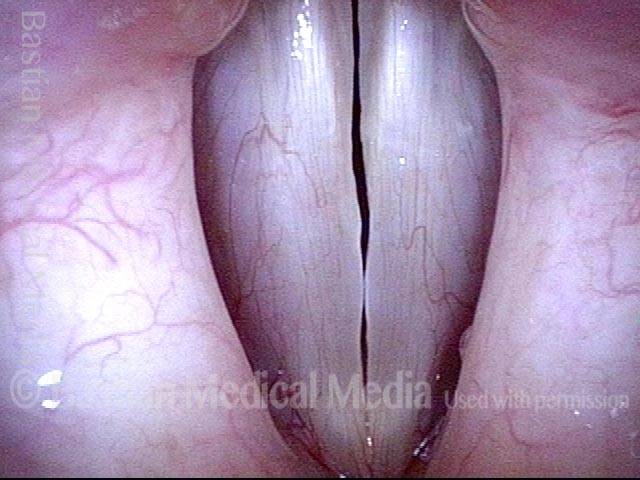
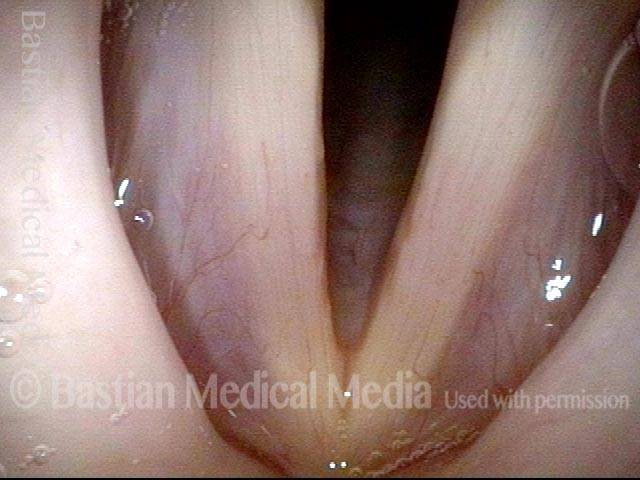
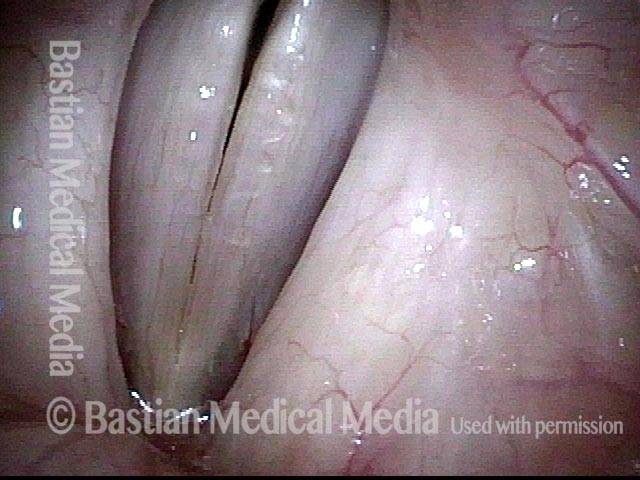
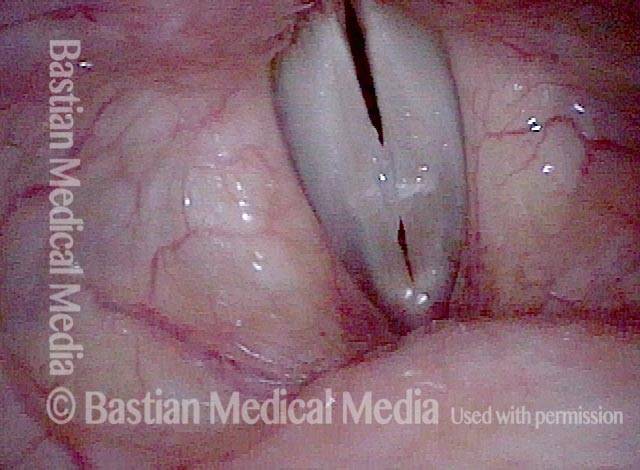
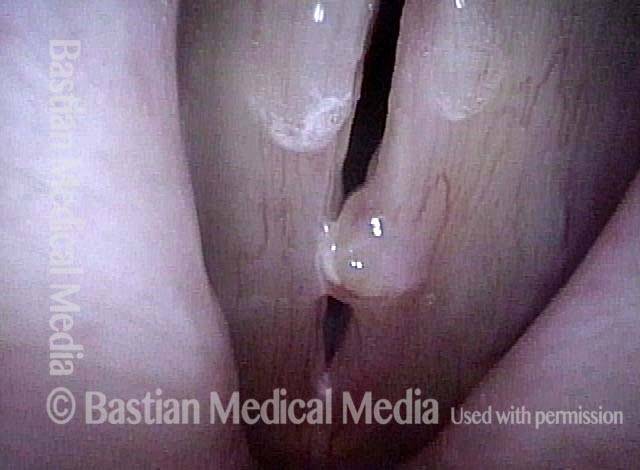
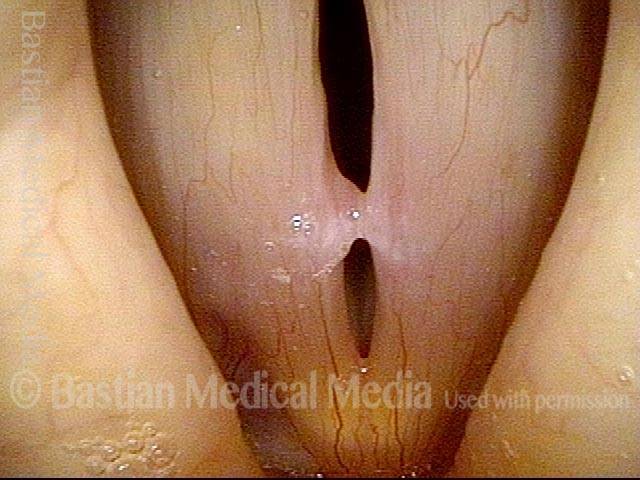
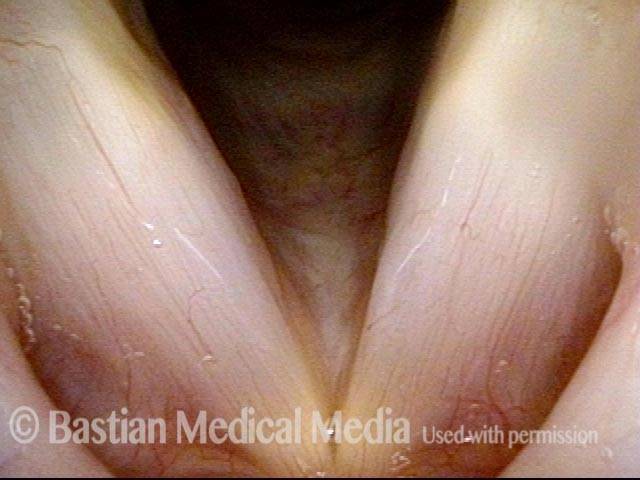
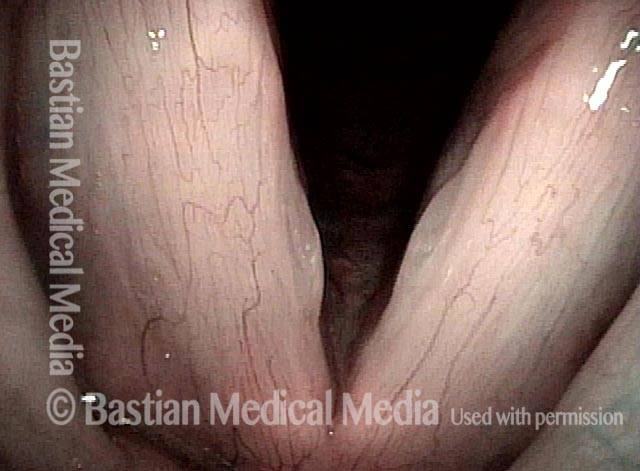
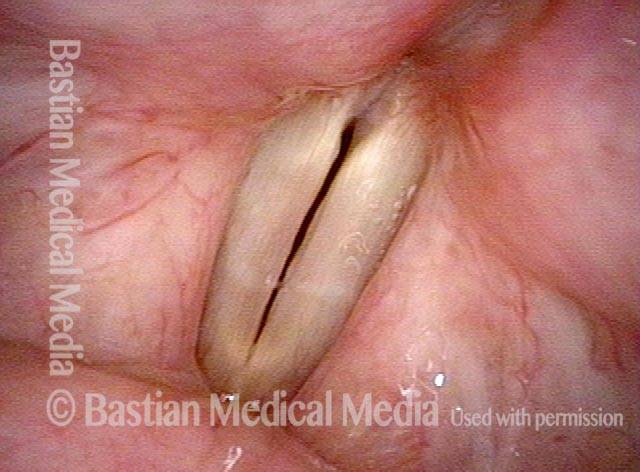
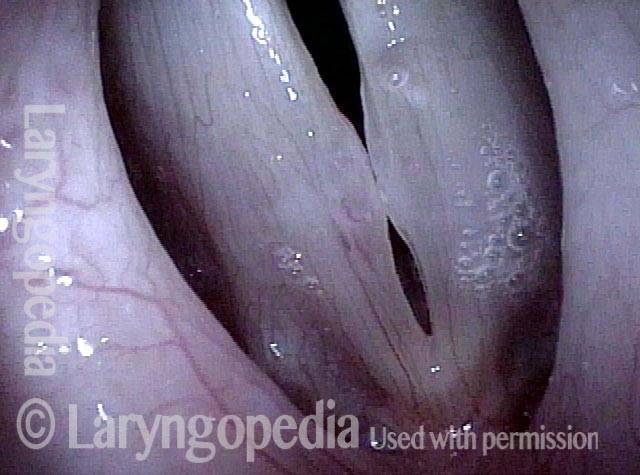
Closed phase (4 of 6)
Closed phase (4 of 6)
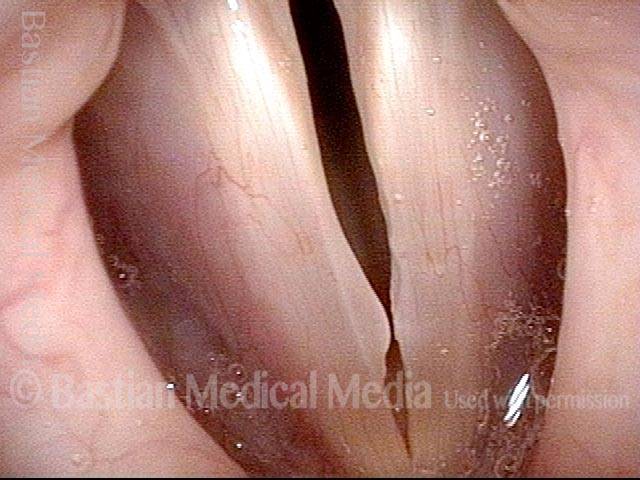
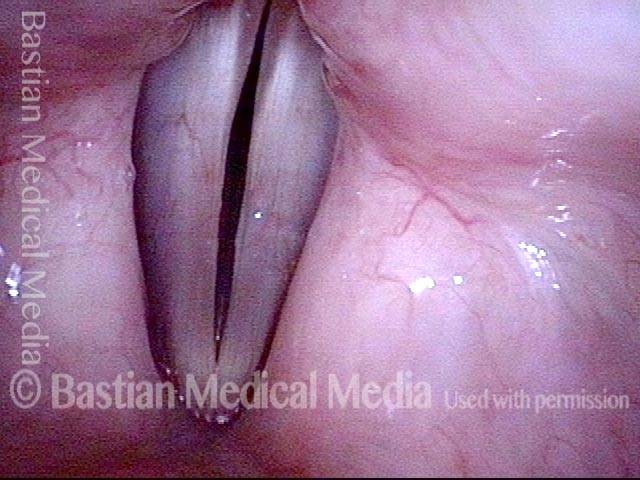
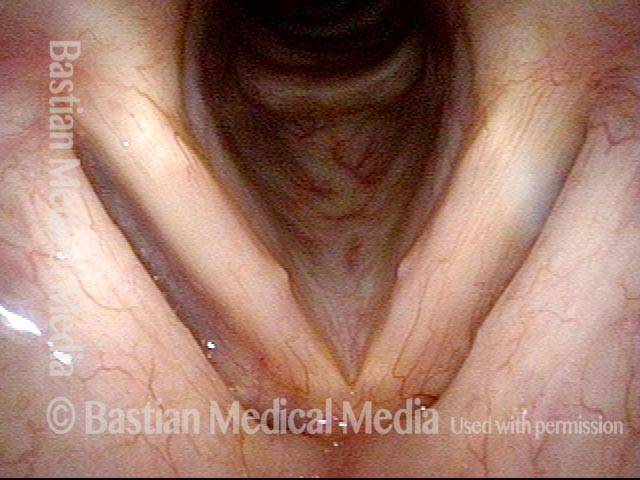
7 weeks after surgery (5 of 6)
7 weeks after surgery (5 of 6)
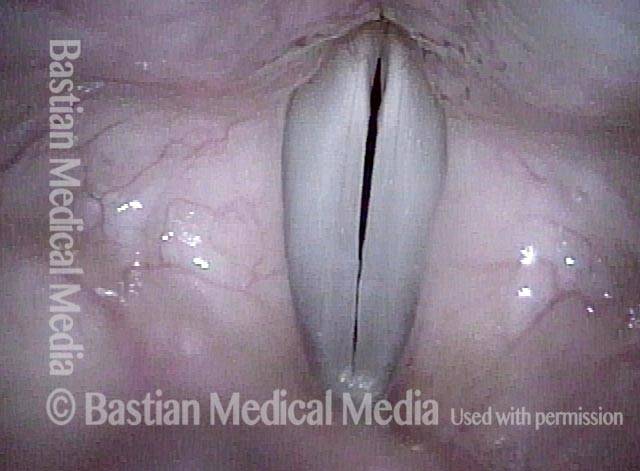
7 weeks after surgery (6 of 6)
7 weeks after surgery (6 of 6)
 Vocal Cord Mucosa Vibratory Decoupling
Vocal Cord Mucosa Vibratory Decoupling
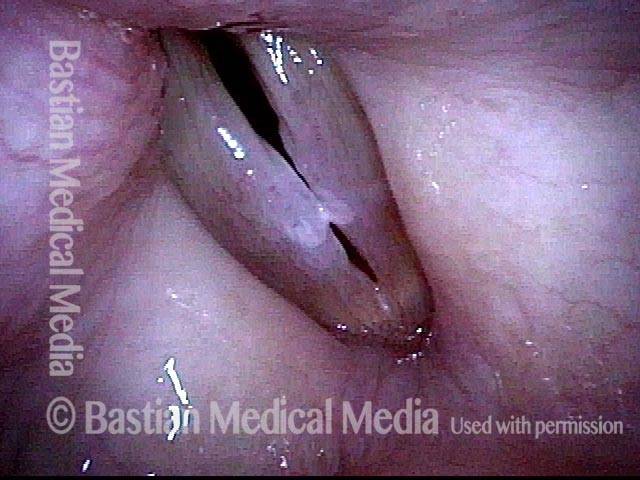
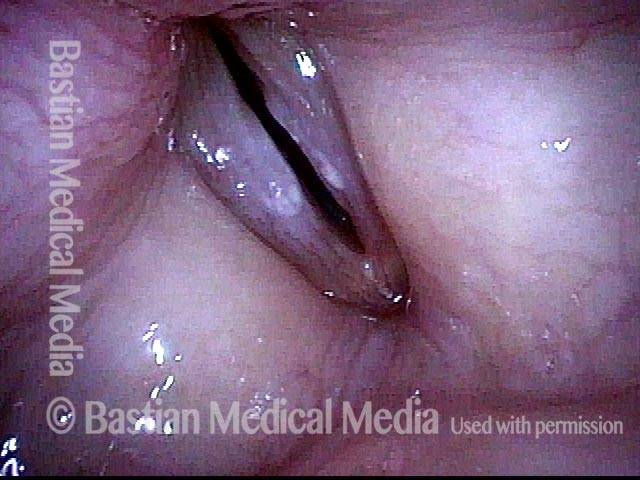
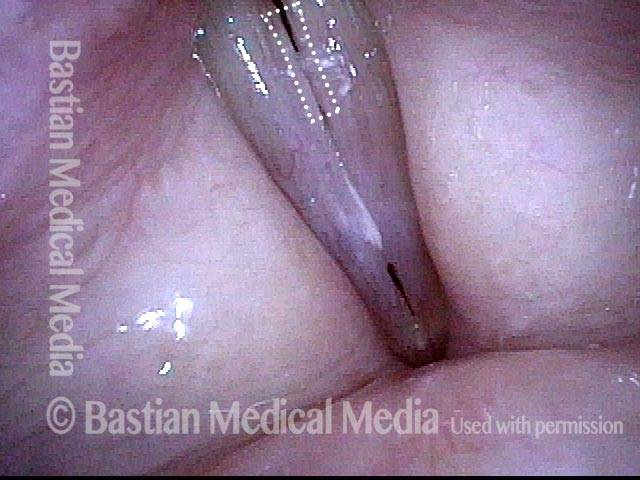
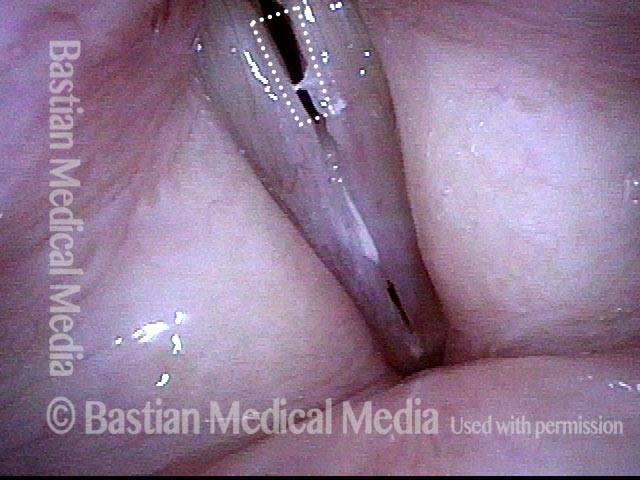
This series is designed to highlight the crucial importance of vocal cord mucosal flexibility—its ability to stretch and move independently of deeper structures. A surgical sequence illustrates this principle:
This singer requires removal of a polypoid nodule that therapy and time would not resolve from her right vocal cord. During the procedure, the polyp is gently grasped and tented away from the underlying vocal ligament and muscle, vividly demonstrating how stretchable the mucosa is.
Think of the way the skin on the back of your hand can be lifted without moving the hand itself. Another analogy is the classic child’s paddleball toy: the wooden paddle represents the muscle and vocal ligament, the red rubber ball corresponds to the epithelium (the surface layer of cells), and the elastic band connecting them symbolizes the flexible attachment layer to underlying structures that do not vibrate.
In surgery, the goal is to remove not just the superficial epithelium—which easily regenerates—but only a short segment of that elastic “rubber band.” By preserving most of this attachment layer, the newly regenerated epithelium won’t adhere directly to the deeper “paddle.” This maintains the mucosal pliability essential for optimal voice.
Vocal Cord Anatomy — Surgical View (1 of 8)
Vocal Cord Anatomy — Surgical View (1 of 8)
Mucosal “Stretch” Demonstration (2 of 8)
Mucosal “Stretch” Demonstration (2 of 8)
Skin-Stretch Analogy (3 of 8)
Skin-Stretch Analogy (3 of 8)
Limited Excision (4 of 8)
Limited Excision (4 of 8)
Vibratory Blur Analogy (5 of 8)
Vibratory Blur Analogy (5 of 8)
Post-Excision Result (6 of 8)
Post-Excision Result (6 of 8)
To review: Preop (7 of 8)
To review: Preop (7 of 8)
Final result (8 of 8)
Final result (8 of 8)
Polypoid Vocal Nodules
Polypoid vocal nodules (1 of 4)
Polypoid vocal nodules (1 of 4)
Incomplete closure (2 of 4)
Incomplete closure (2 of 4)
Polypoid vocal nodules (3 of 4)
Polypoid vocal nodules (3 of 4)
Polypoid vocal nodules (4 of 4)
Polypoid vocal nodules (4 of 4)
Example 2 (Vocal Cord ‘Wounds,’ 2 Hours after Surgery)
Polypoid nodule, open phase (1 of 8)
Polypoid nodule, open phase (1 of 8)
Polypoid nodule, closed phase (2 of 8)
Polypoid nodule, closed phase (2 of 8)
Polypoid nodule, right and left cords (3 of 8)
Polypoid nodule, right and left cords (3 of 8)
Segmental vibration (4 of 8)
Segmental vibration (4 of 8)
Post-surgery wounds (5 of 8)
Post-surgery wounds (5 of 8)
Post-surgery, closed phase (6 of 8)
Post-surgery, closed phase (6 of 8)
Post-surgery, open phase (7 of 8)
Post-surgery, open phase (7 of 8)
Post-surgery, precise match (8 of 8)
Post-surgery, precise match (8 of 8)
Vocal Nodules, Before & After Surgery
Vocal nodules (1 of 10)
Vocal nodules (1 of 10)
Prephonatory instant (2 of 10)
Prephonatory instant (2 of 10)
Translucency (3 of 10)
Translucency (3 of 10)
Open phase (4 of 10)
Open phase (4 of 10)
1 week after surgery (5 of 10)
1 week after surgery (5 of 10)
1 week after surgery (6 of 10)
1 week after surgery (6 of 10)
1 week after surgery (7 of 10)
1 week after surgery (7 of 10)
Vocal nodules: 10 weeks after surgery (8 of 10)
Vocal nodules: 10 weeks after surgery (8 of 10)
10 weeks after surgery (9 of 10)
10 weeks after surgery (9 of 10)
10 weeks after surgery (10 of 10)
10 weeks after surgery (10 of 10)
Example 2
Vocal nodules (1 of 4)
Vocal nodules (1 of 4)
Phonation (2 of 4)
Phonation (2 of 4)
After surgery (3 of 4)
After surgery (3 of 4)
After surgery (4 of 4)
After surgery (4 of 4)
Example 3
Vocal nodules, before surgery (1 of 4)
Vocal nodules, before surgery (1 of 4)
Before surgery (2 of 4)
Before surgery (2 of 4)
After surgery (3 of 4)
After surgery (3 of 4)
Vocal nodules, after surgery (4 of 4)
Vocal nodules, after surgery (4 of 4)
Example 4 (Pre- & 1 Week Post-removal)
Vocal nodules (1 of 8)
Vocal nodules (1 of 8)
Muscular tension dysphonia (2 of 8)
Muscular tension dysphonia (2 of 8)
Open phase (3 of 8)
Open phase (3 of 8)
Closed phase (4 of 8)
Closed phase (4 of 8)
Post-op, one week (5 of 8)
Post-op, one week (5 of 8)
Phonation (6 of 8)
Phonation (6 of 8)
Open phase (7 of 8)
Open phase (7 of 8)
Closed phase (8 of 8)
Closed phase (8 of 8)
Vocal Nodules, Spicule-shaped
Vocal nodules (1 of 3)
Vocal nodules (1 of 3)
During phonation (2 of 3)
During phonation (2 of 3)
Closed phase (3 of 3)
Closed phase (3 of 3)
Example 2
Vocal nodules (1 of 4)
Vocal nodules (1 of 4)
Small nodules (2 of 4)
Small nodules (2 of 4)
Phonation (3 of 4)
Phonation (3 of 4)
Open phase (4 of 4)
Open phase (4 of 4)
Fibrotic Nodules
Fibrotic nodules (1 of 5)
Fibrotic nodules (1 of 5)
Fibrotic nodules: full-length vibration at low pitch (2 of 5)
Fibrotic nodules: full-length vibration at low pitch (2 of 5)
Fibrotic nodules: full-length vibration at low pitch (3 of 5)
Fibrotic nodules: full-length vibration at low pitch (3 of 5)
Fibrotic nodules: segmental vibration at high pitch (4 of 5)
Fibrotic nodules: segmental vibration at high pitch (4 of 5)
Fibrotic nodules: segmental vibration at high pitch (5 of 5)
Fibrotic nodules: segmental vibration at high pitch (5 of 5)
Example 2 (Fibrosis as a Base to Nodules, Before & After Surgery)
Bilateral polypoid nodules (1 of 8)
Bilateral polypoid nodules (1 of 8)
Narrow-band lighting (2 of 8)
Narrow-band lighting (2 of 8)
Closed phase (3 of 8)
Closed phase (3 of 8)
Open phase (4 of 8)
Open phase (4 of 8)
Two weeks after surgery (5 of 8)
Two weeks after surgery (5 of 8)
Phonation (6 of 8)
Phonation (6 of 8)
Margin fibrosis (7 of 8)
Margin fibrosis (7 of 8)
Open phase (8 of 8)
Open phase (8 of 8)
More Examples of Vocal Nodules
Vocal nodules (1 of 4)
Vocal nodules (1 of 4)
Prephonatory instant (2 of 4)
Prephonatory instant (2 of 4)
Open phase of vibration (3 of 4)
Open phase of vibration (3 of 4)
Closed phase of vibration (4 of 4)
Closed phase of vibration (4 of 4)
Example 2
Vocal nodules (1 of 2)
Vocal nodules (1 of 2)
Vocal nodules (2 of 2)
Vocal nodules (2 of 2)
Example 3
Vocal nodules (1 of 1)
Vocal nodules (1 of 1)
Example 4
Vocal nodules (1 of 1)
Vocal nodules (1 of 1)
Example 5 (Vocal Nodule Postop Irregularity yet Match & Flexibility)
Large vocal nodules (1 of 8)
Large vocal nodules (1 of 8)
Narrow band light (2 of 8)
Narrow band light (2 of 8)
One week after surgery (5 of 8)
One week after surgery (5 of 8)
Prephonatory instant (6 of 8)
Prephonatory instant (6 of 8)
Open phase (7 of 8)
Open phase (7 of 8)
Search not Only for Nodules, but Also for Segmental Vibration and Look at the Posterior Commissure for MTD
Open phase (1 of 4)
Open phase (1 of 4)
Closed phase (2 of 4)
Closed phase (2 of 4)
Segmental vibration (3 of 4)
Segmental vibration (3 of 4)
Posterior commissure (4 of 4)
Posterior commissure (4 of 4)
Ask Both Voice (via vocal phenomenology) and Larynx (via a motivated examination) to Give up their Secrets
Obvious mucosal injury (1 of 3)
Obvious mucosal injury (1 of 3)
Vocal nodules (2 of 3)
Vocal nodules (2 of 3)
Capillary ectasia (3 of 3)
Capillary ectasia (3 of 3)
Mottled Vocal Cord Mucosa May Hide Glottic Sulci
Vocal cord swelling and mucosa (1 of 4)
Vocal cord swelling and mucosa (1 of 4)
Same view under strobe light (2 of 4)
Same view under strobe light (2 of 4)
Closed phase (3 of 4)
Closed phase (3 of 4)
Glottic sulcus is visible (4 of 4)
Glottic sulcus is visible (4 of 4)
Vocal Nodules, Leukoplakia, & Capillary Ectasia
Vocal nodules, leukoplakia, and capillary ectasia (1 of 4)
Vocal nodules, leukoplakia, and capillary ectasia (1 of 4)
Vocal nodules, leukoplakia, and capillary ectasia (2 of 4)
Vocal nodules, leukoplakia, and capillary ectasia (2 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (3 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (3 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (4 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (4 of 4)
Share this article
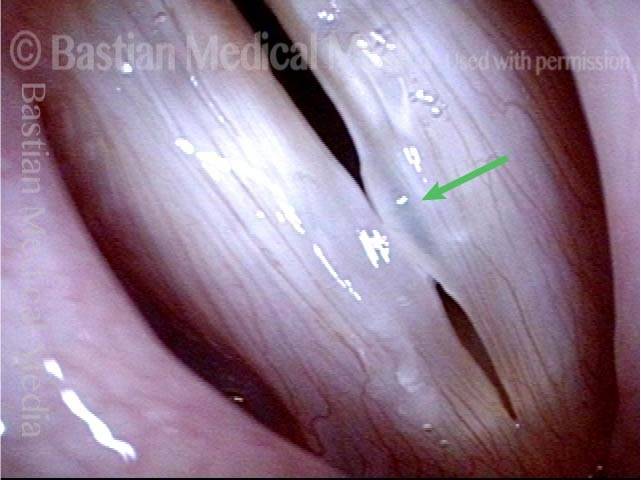

Nodules and Other Vocal Cord Injuries: How They Occur and Can Be Treated
This video explains how nodules and other vocal cord injuries occur: by excessive vibration of the vocal cords, which happens with vocal overuse. Having laid that foundational understanding, the video goes on to explore the roles of treatment options like voice therapy and vocal cord microsurgery.

Vocal Fold Swelling Checks
In this video, Dr. Bastian introduces and demonstrates two swelling checks: two simple vocal exercises that can be used to help detect the early signs of vocal fold injury. He also discusses the physiology of vocal fold injury and explains how to make the best use of these swelling checks in your daily routine.
5 Symptoms of Vocal Cord Mucosal Injury
Singers or others who have injured the mucosa—surface layer—of their vocal cords may have normal-sounding speaking voices and at the same time, singing voice frustrations.
This video explains the 5 most common symptoms of injury. In addition, Dr. Bastian’s prior video on vocal cord swelling checks can help the singer know when to begin thinking “my problem may be injury, and not acid reflux or a technical deficit.”

Mucosal Chattering
In this video, Dr. Bastian makes extensive use of elicitation with his own voice in order to hear the “vocal phenomenology” of a voice under evaluation. He has named one phenomenon he has not heard described elsewhere as mucosal chatter.

Vocal Money – Recovering from Vocal Cord Injury
Individuals who develop chronic vibratory injuries of the vocal cords, such as nodules and polyps, can be thought of as having been vocal overspenders.
And so, conceptualizing voice use as spending vocal money can provide a helpful analogy for those rehabilitating from their injuries. The idea is to think of having vocal money to spend every day, and to manage the amount, manner, and spacing of expenditure, in order to get out of the vocal debt of vibratory injury.