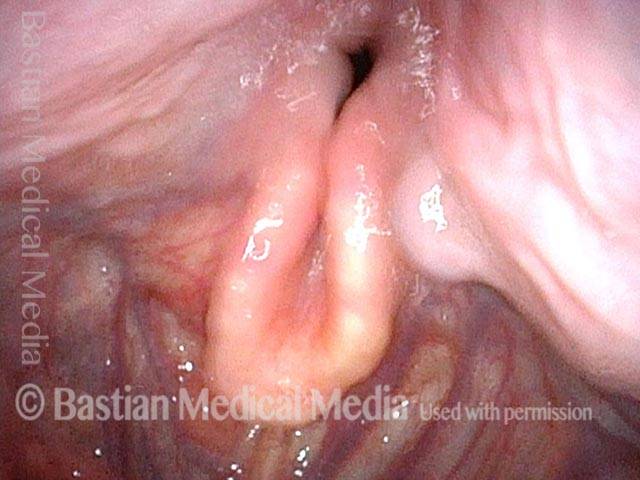
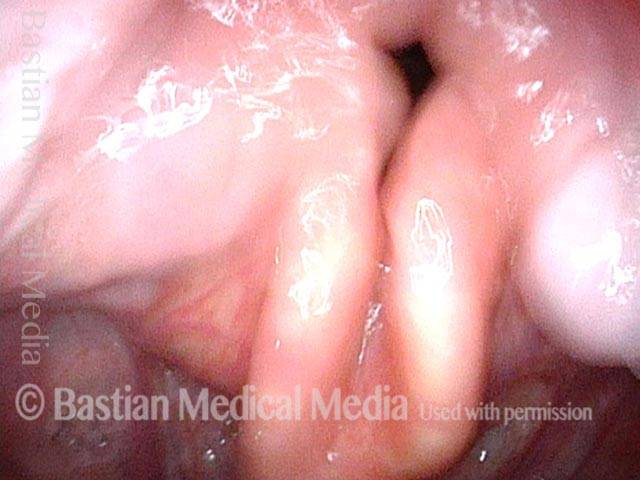
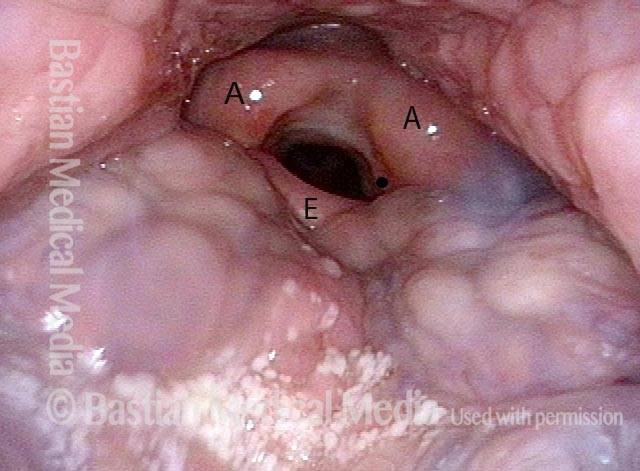
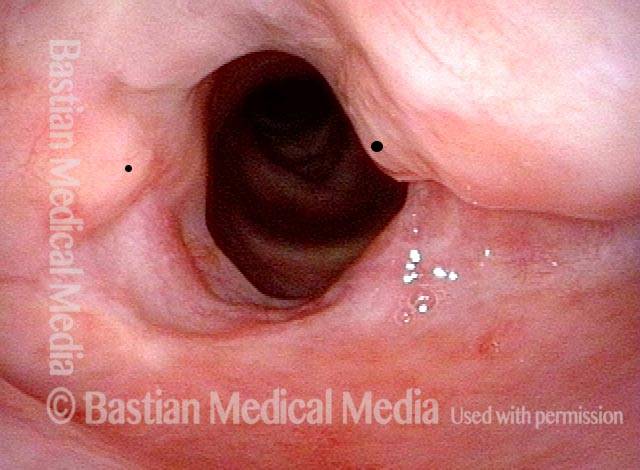
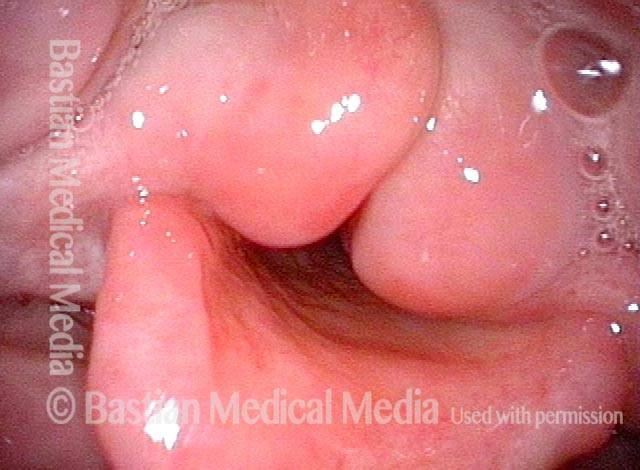
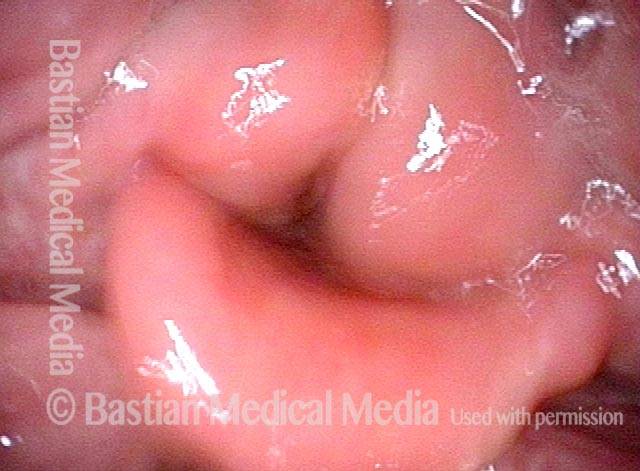
Hemilaryngectomy is a surgical procedure that removes part of the front of the larynx, typically done in order to remove a cancerous growth. This procedure was once the primary treatment option for medium and large vocal cord cancers that could not be removed by endoscopic (through the mouth) laser.
Today, when laser cannot be used because of patient preference or anatomical difficulty, chemotherapy and radiation therapy are usually attempted first. The biggest role for hemilaryngectomy now seems to be for carefully selected tumors (in the earlier stages, T1 through large T2) that have persisted or recurred after initial treatment of radiation therapy with or without chemotherapy.
How the Procedure Works
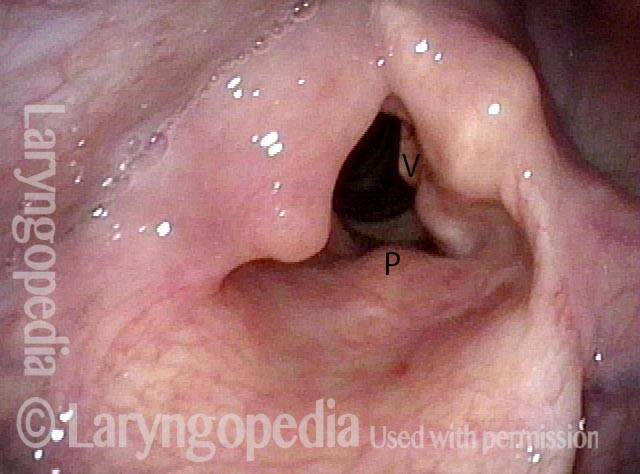
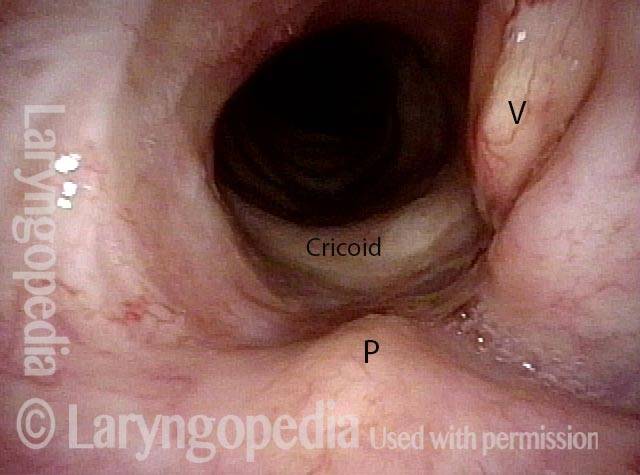
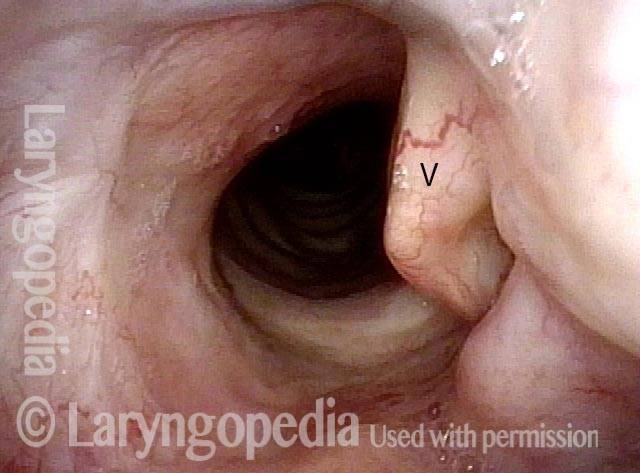
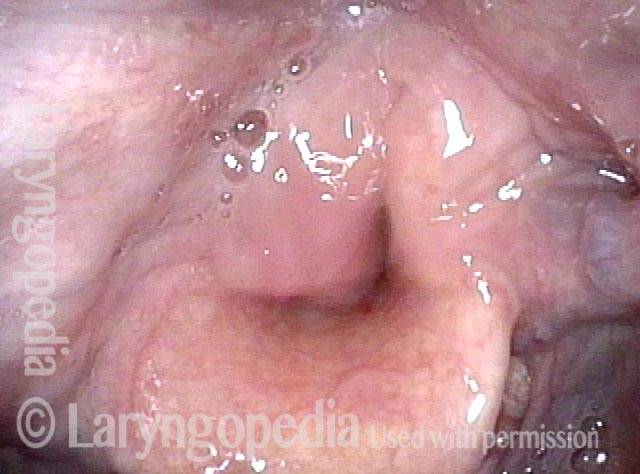
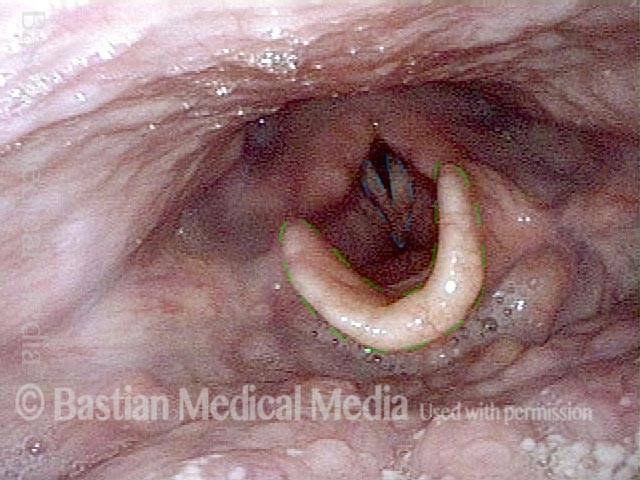
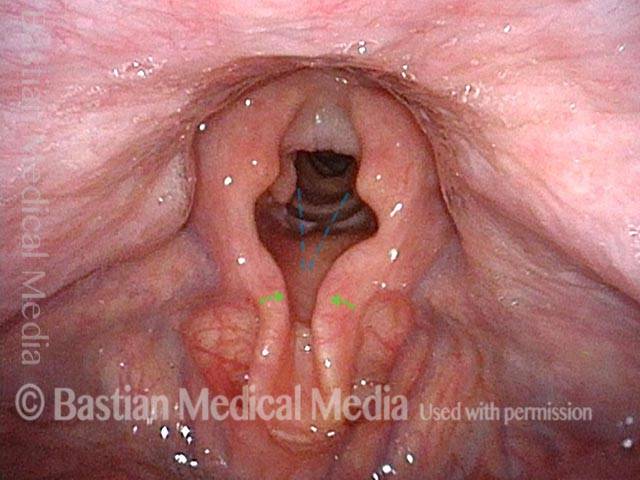
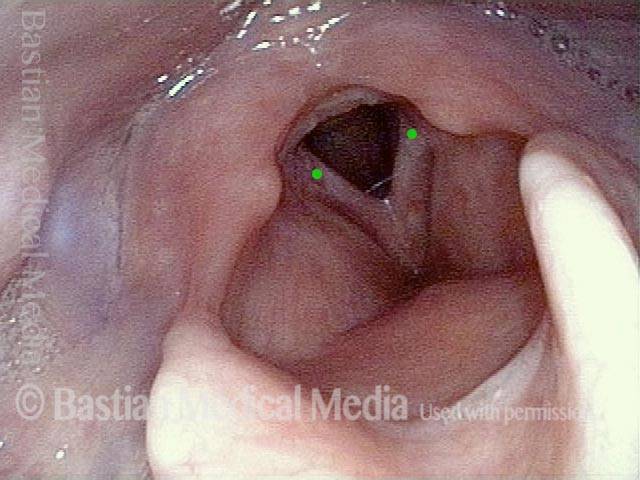
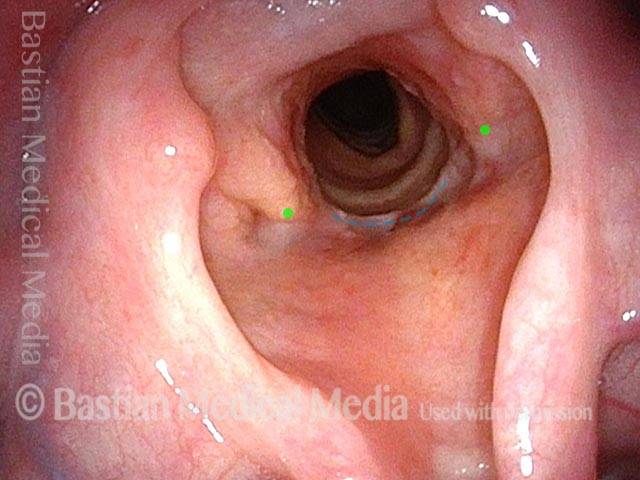
In a hemilaryngectomy, the surgeon removes part of the thyroid cartilage, including the underlying vocal cord or cords. The extent of removal varies from procedure to procedure. In fact, the term “hemilaryngectomy” is somewhat misleading; “hemi” means “half,” but most hemilaryngectomies remove much less than half of the larynx. A very minimal procedure might only remove most of one side of the thyroid cartilage with the underlying soft tissue but not touch the arytenoid cartilage. On the other hand, a very extensive procedure might remove most of both sides of the thyroid cartilage, leaving the patient with only one arytenoid. Many other procedures would fall on a spectrum between these two extremes.