Laser Surgery
Laser surgery is surgery that uses a beam of laser light, rather than other instruments, to cut, dissect, remove, and so forth. The beam of light has advantages over other cutting instruments, such as scalpel or scissors.
First, at the same time that it cuts, it tends to seal off tiny blood vessels and reduce bleeding. Second, it may be especially useful in endoscopic surgery, where there is not a lot of room for instruments. Third, it is very precise. Both the microspot carbon dioxide laser and the RevoLix laser used at our practice have minimum spot sizes of about 1/5 of a millimeter.
Laser Surgery for Bilateral Vocal Cord Cancer
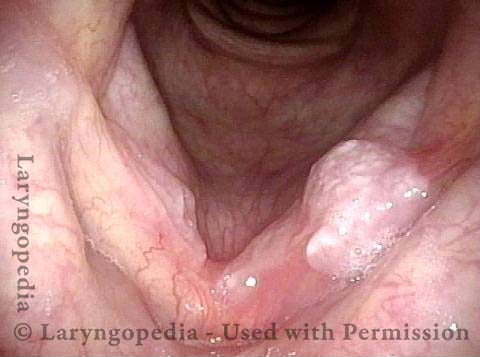
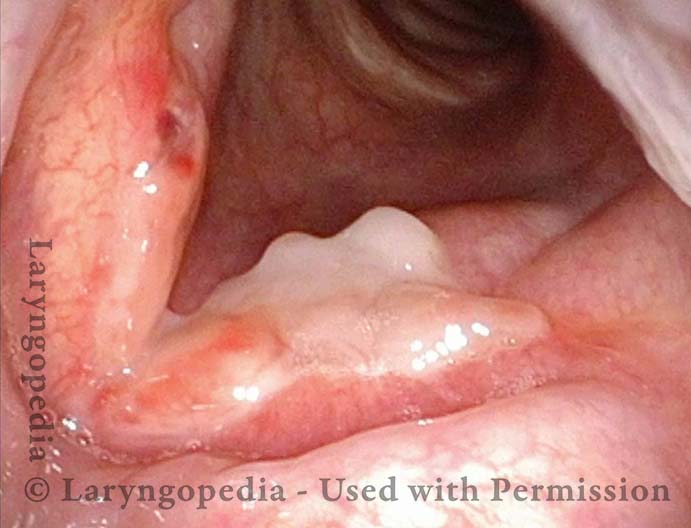
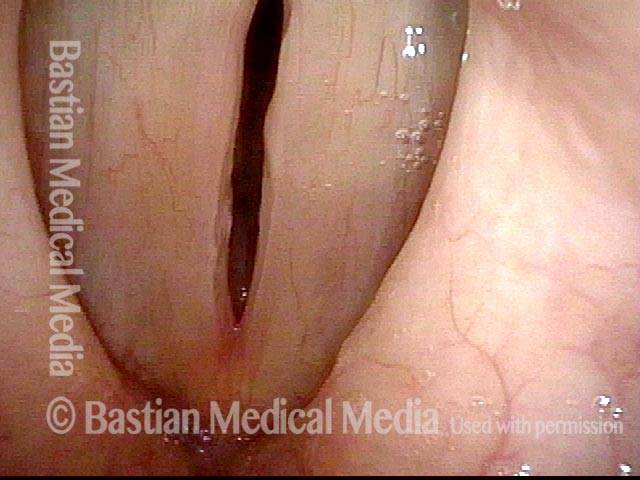
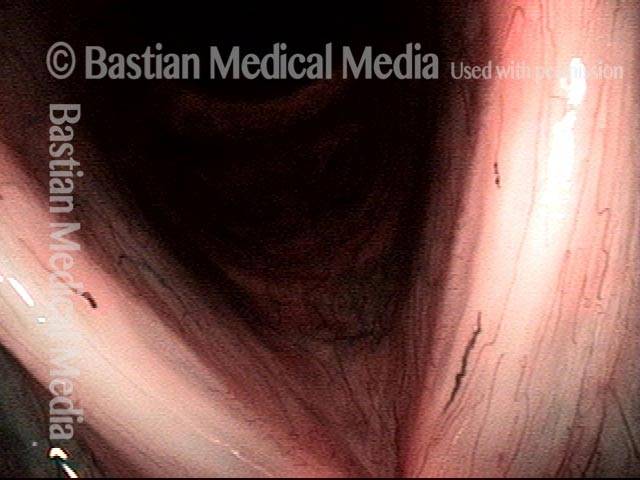
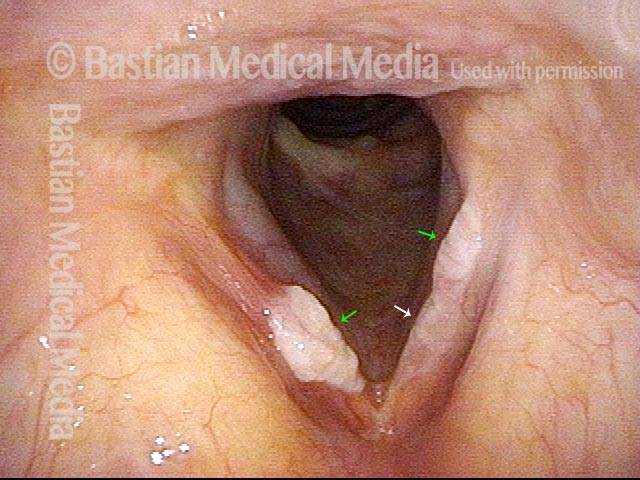
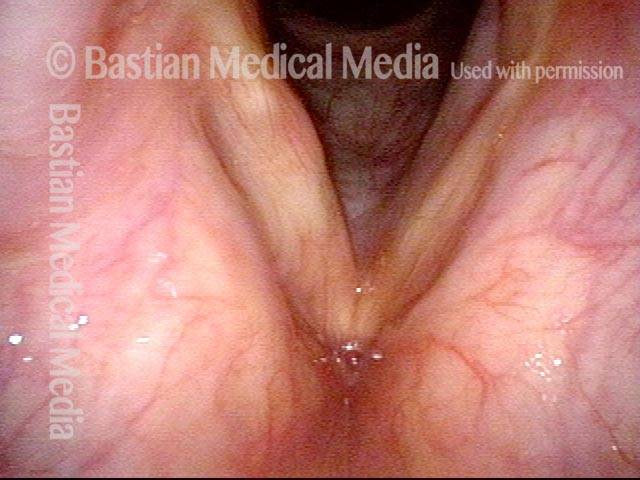
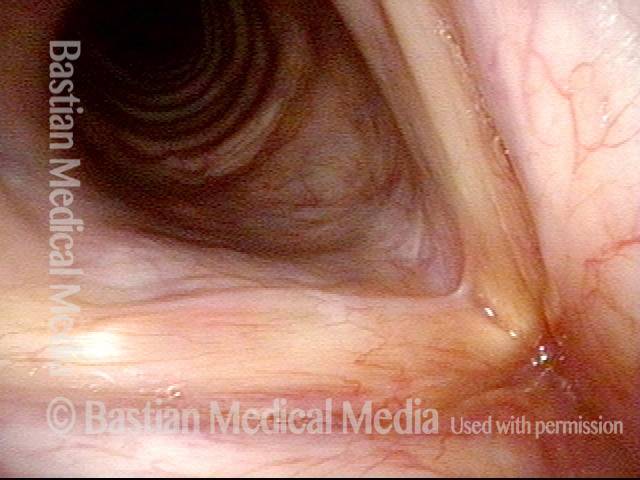
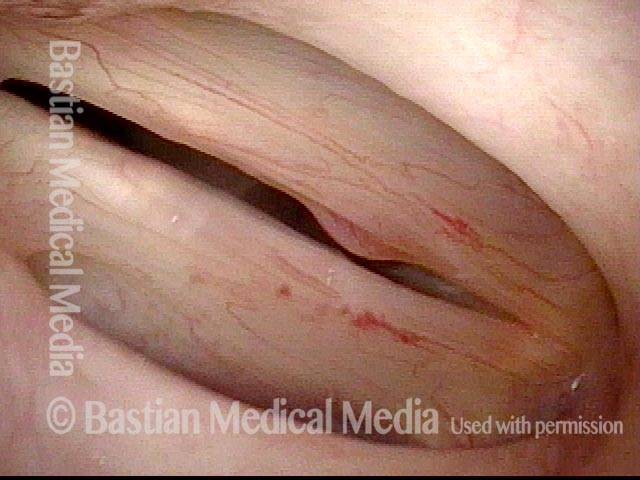
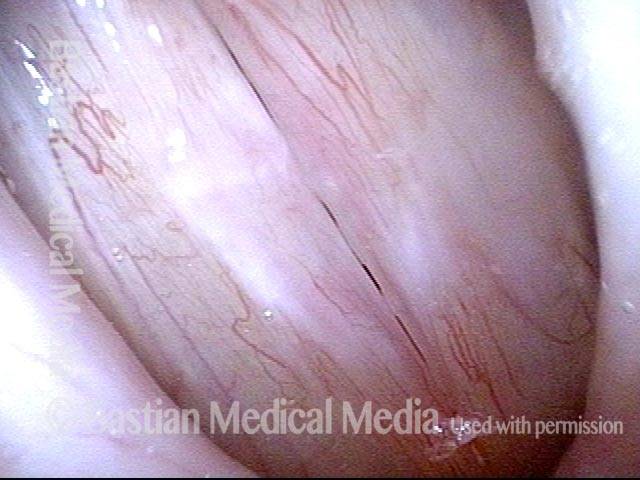
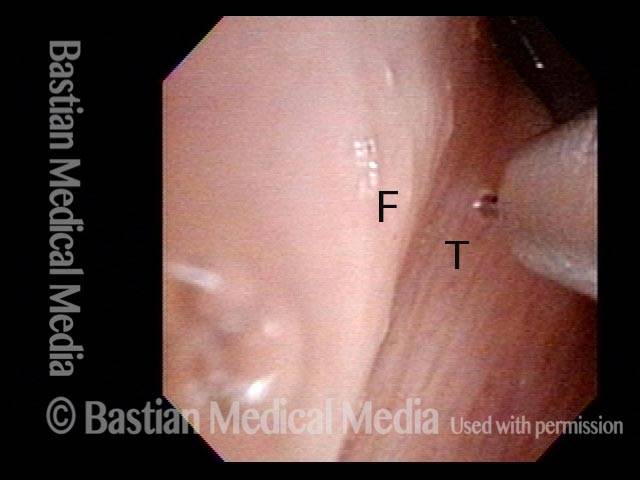
Squamous cell carcinoma (1 of 6)
Squamous cell carcinoma (1 of 6)
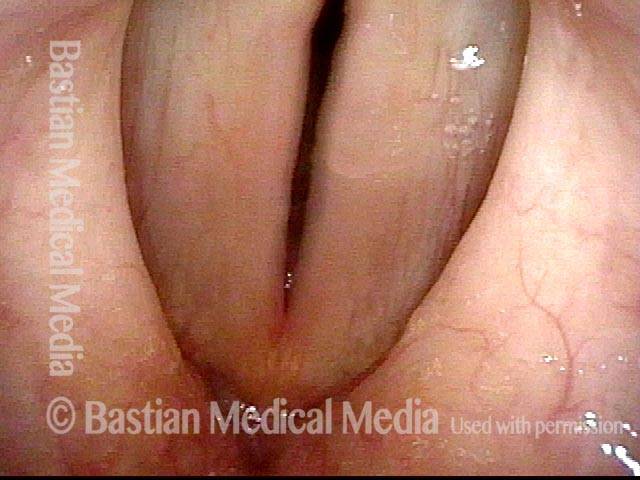
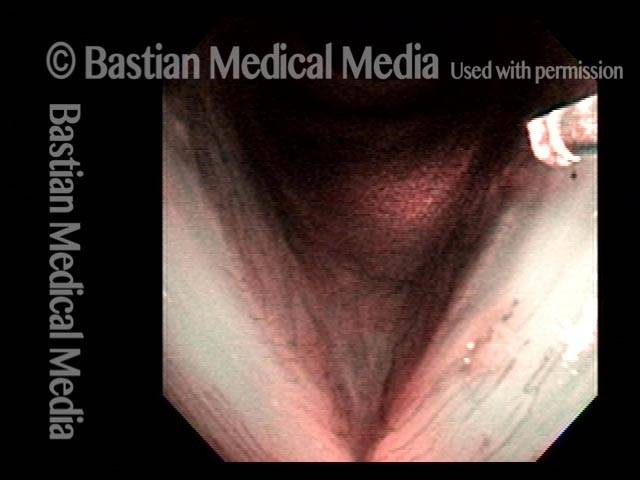
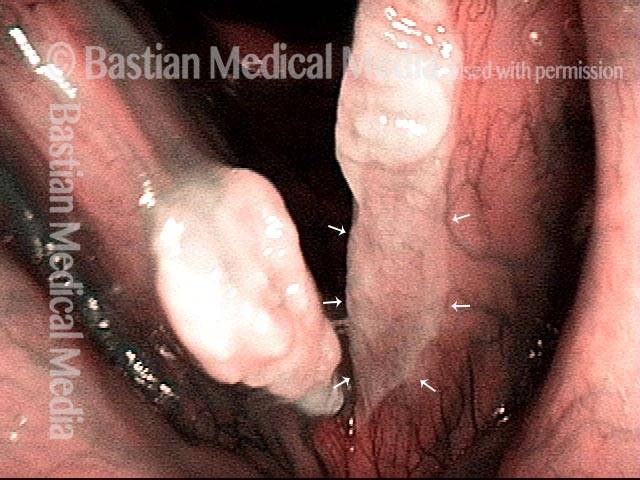
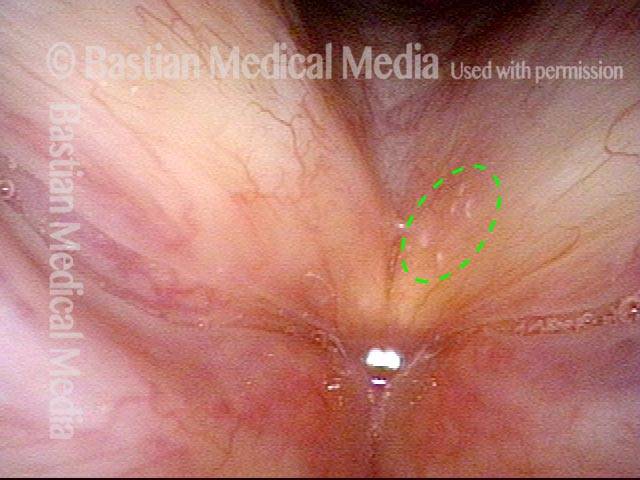
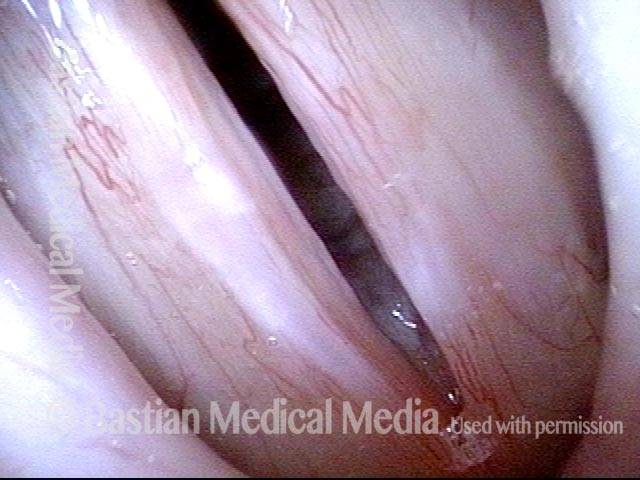
Tumor on the vocal cords (2 of 6)
Tumor on the vocal cords (2 of 6)
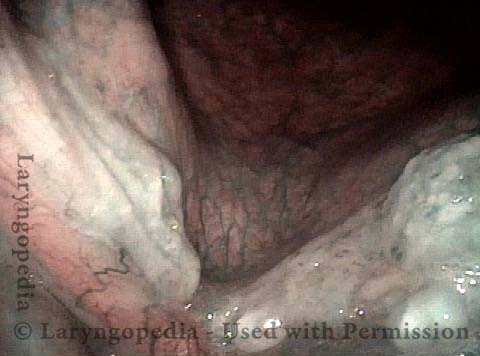
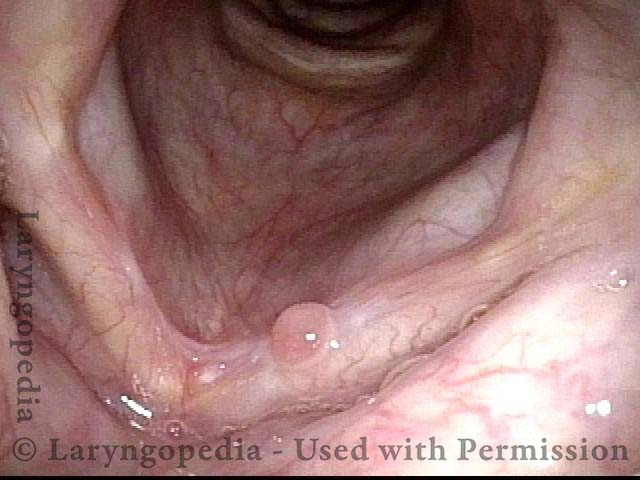
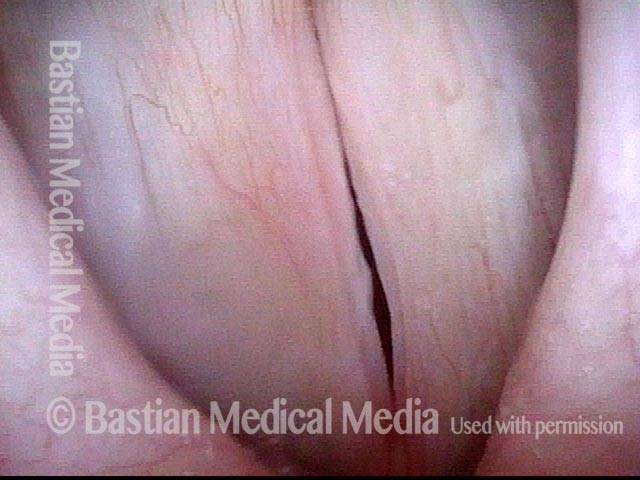
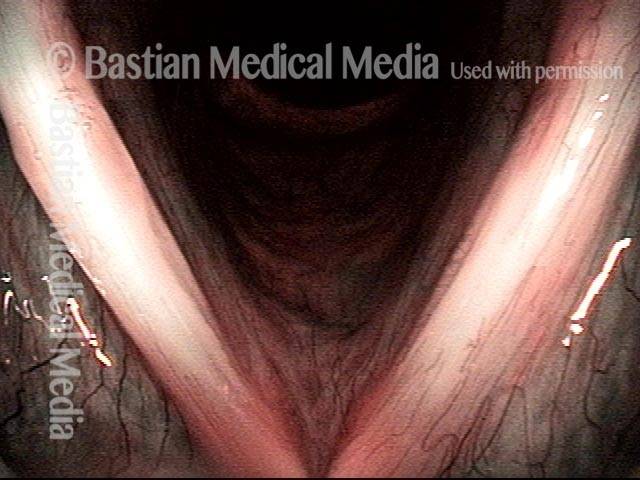
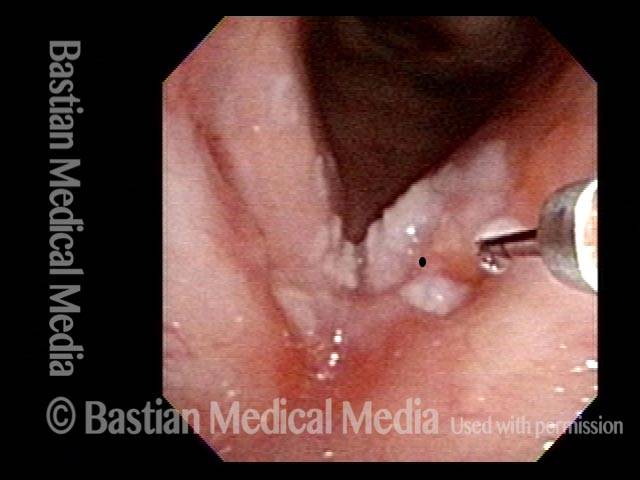
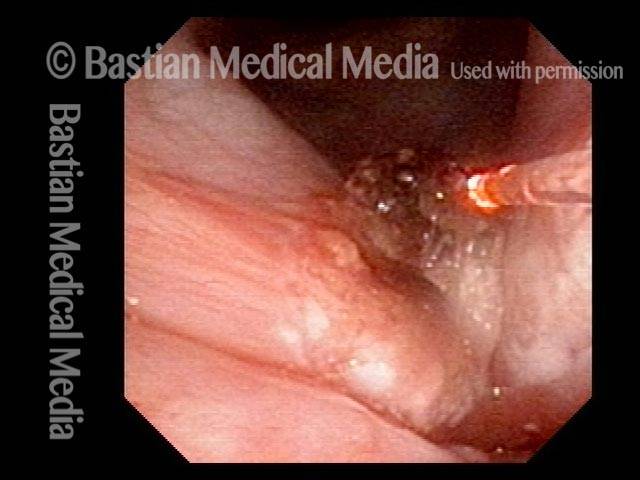
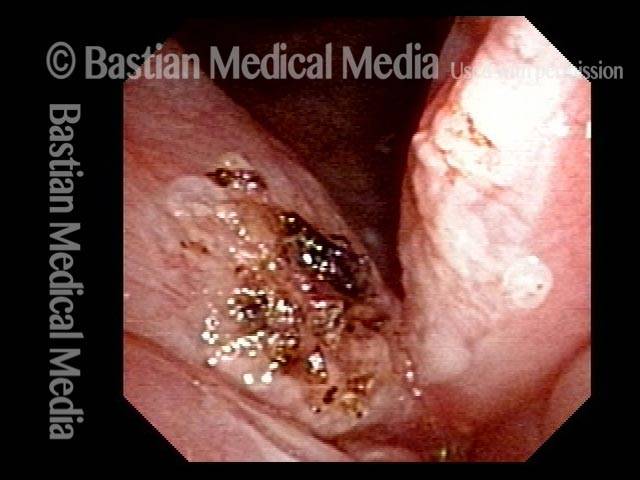
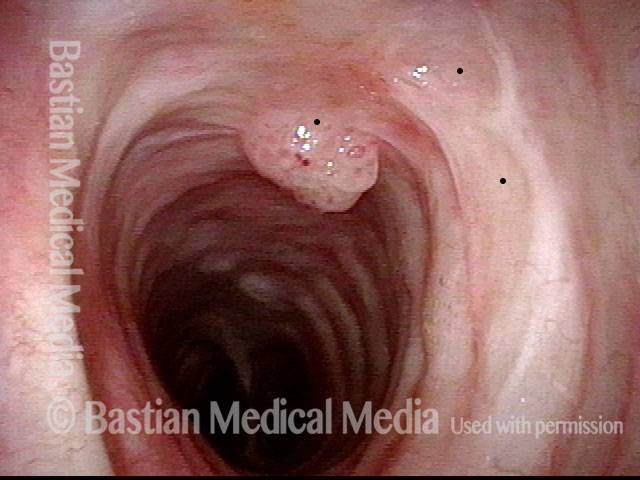
Granuloma delays voice recovery (3 of 6)
Granuloma delays voice recovery (3 of 6)
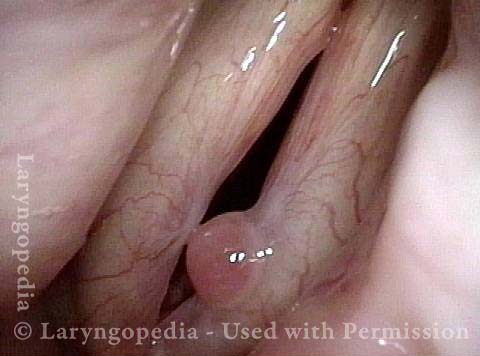
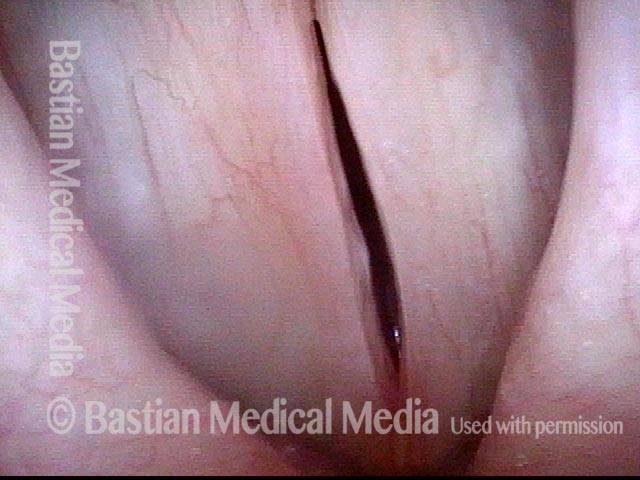
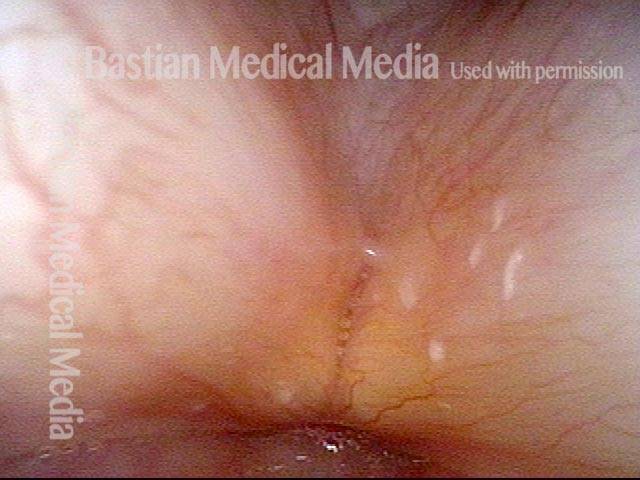
Closer view of granuloma (4 of 6)
Closer view of granuloma (4 of 6)
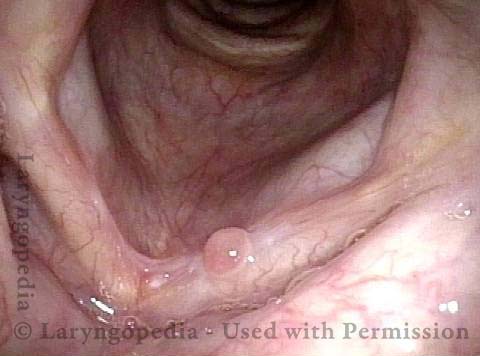
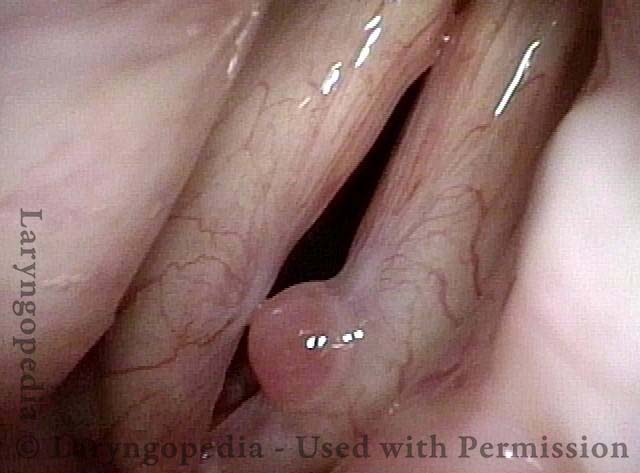
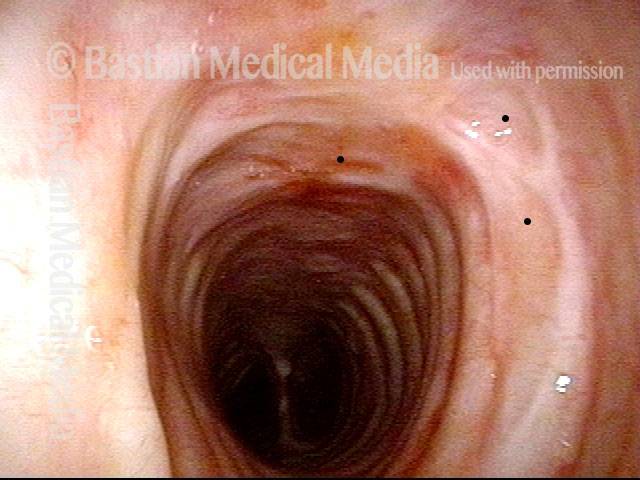
Granuloma is smaller (5 of 6)
Granuloma is smaller (5 of 6)
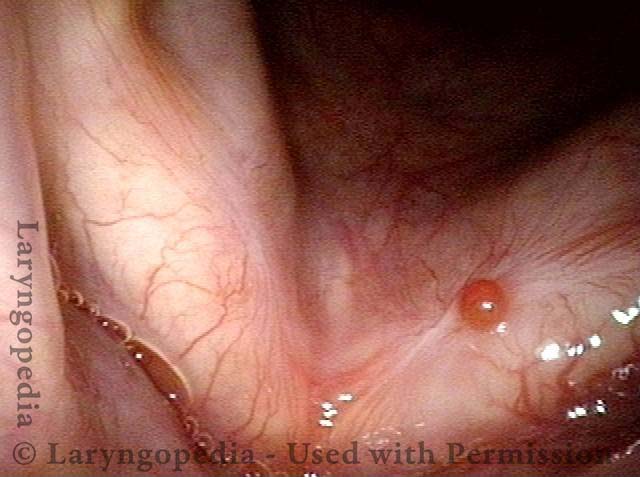
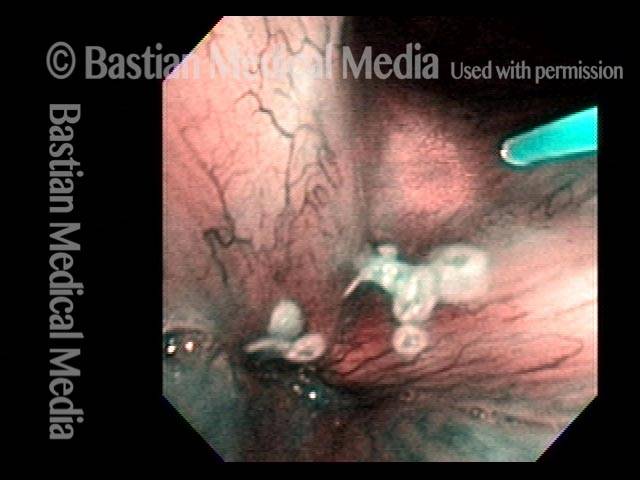
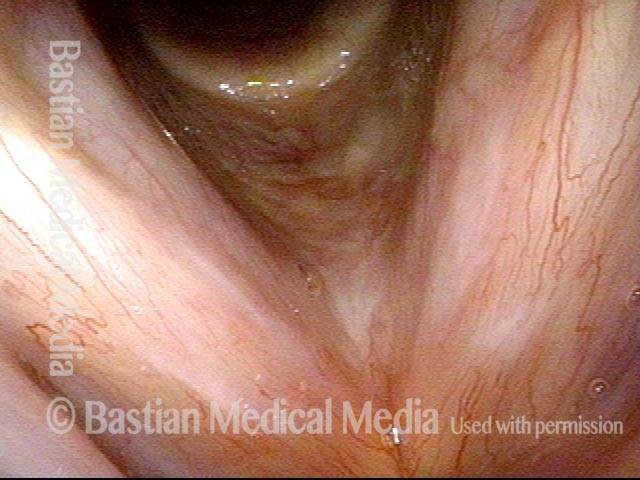
Granuloma doesn’t impede voice (6 of 6)
Granuloma doesn’t impede voice (6 of 6)
Laser Removal of Vocal Cord Cancer with Bilateral Disease
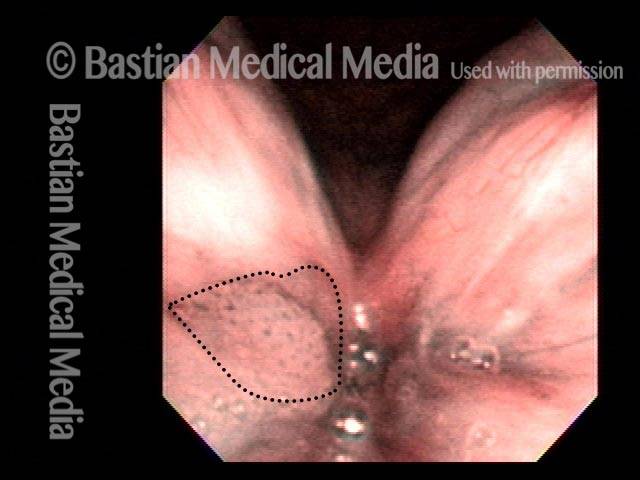
For treatment of early vocal cord cancer, both laser excision and radiotherapy are in competition as good treatment modalities. See also Early Vocal Cord Cancer: Remove with a Laser, or Radiate? Often, radiation is used when disease is bilateral, in the interest of preserving voice. This is an example of the ability to do fairly extensive laser surgery bilaterally, yet preserving good voice. This man had a friend who had severe difficulty with radiation, and he was therefore opposed to that option.
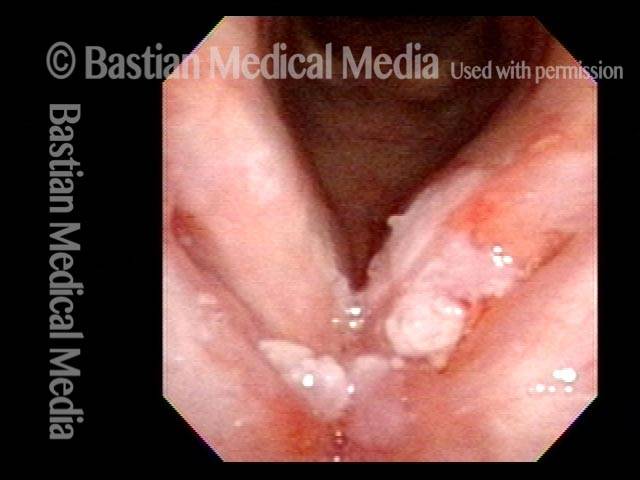
Vocal cord cancer (1 of 10)
Vocal cord cancer (1 of 10)
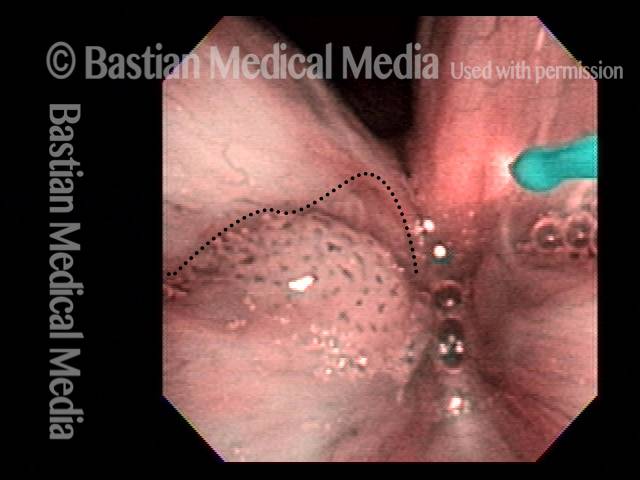
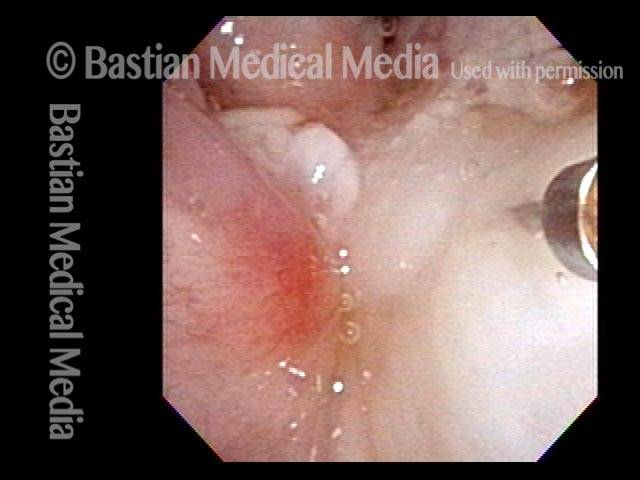
Stippling (2 of 10)
Stippling (2 of 10)
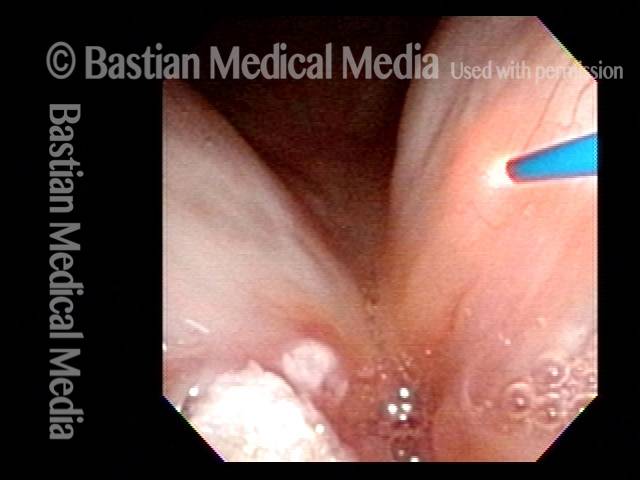
1 week after excision (3 of 10)
1 week after excision (3 of 10)
Reparative Granuloma emerges (4 of 10)
Reparative Granuloma emerges (4 of 10)
Granuloma interferes with voicing (5 of 10)
Granuloma interferes with voicing (5 of 10)
Granuloma fades away (6 of 10)
Granuloma fades away (6 of 10)
Closer view (7 of 10)
Closer view (7 of 10)
Granuloma cleft (8 of 10)
Granuloma cleft (8 of 10)
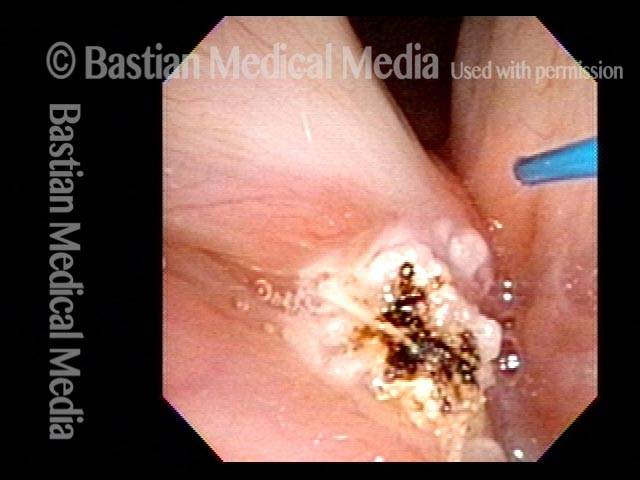
Blood tattoo (9 of 10)
Blood tattoo (9 of 10)
Voice is improved (10 of 10)
Voice is improved (10 of 10)
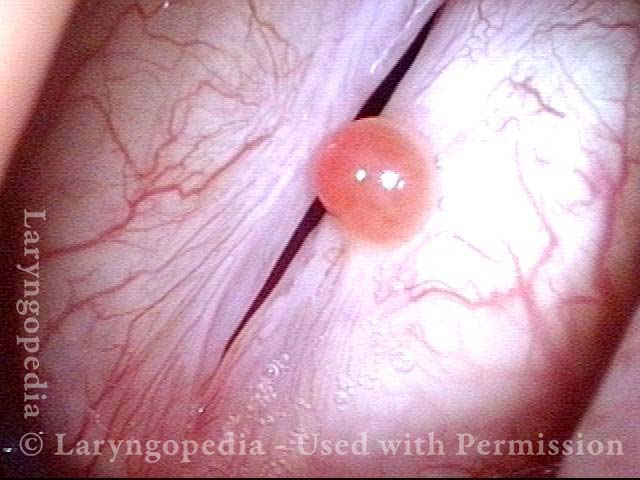
Hemorrhagic Polyp, Treated By Thulium Laser
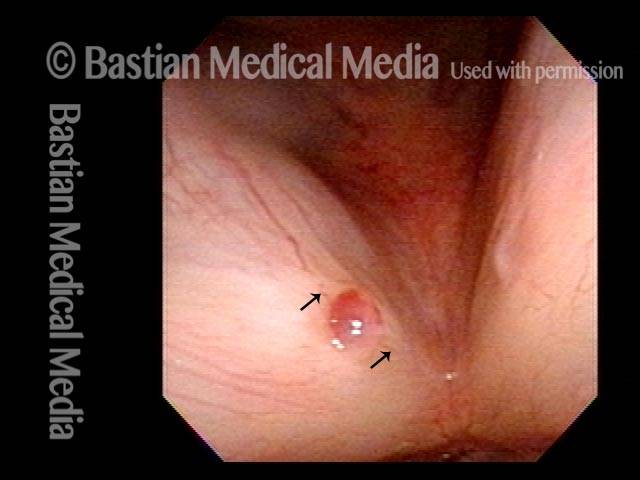
Hemorrhagic polyp, treated by thulium laser (1 of 8)
Hemorrhagic polyp, treated by thulium laser (1 of 8)
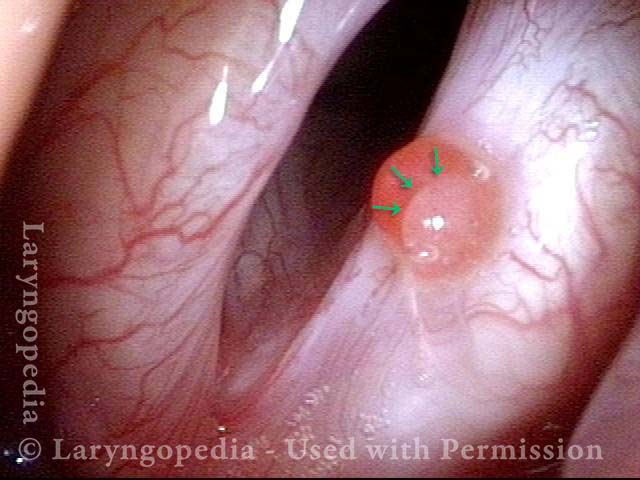
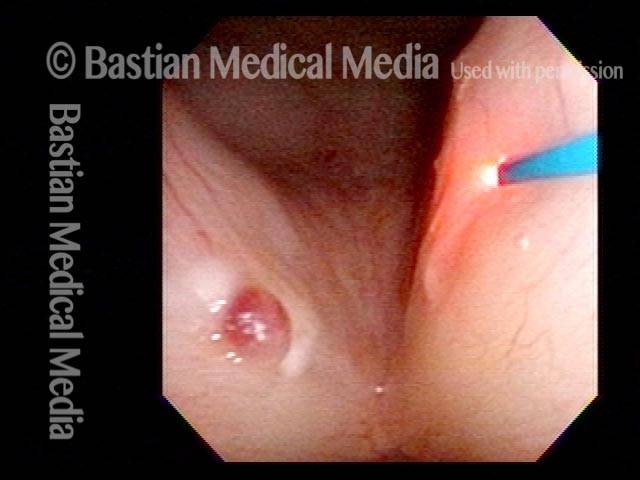
Hemorrhagic polyp, treated by thulium laser (2 of 8)
Hemorrhagic polyp, treated by thulium laser (2 of 8)
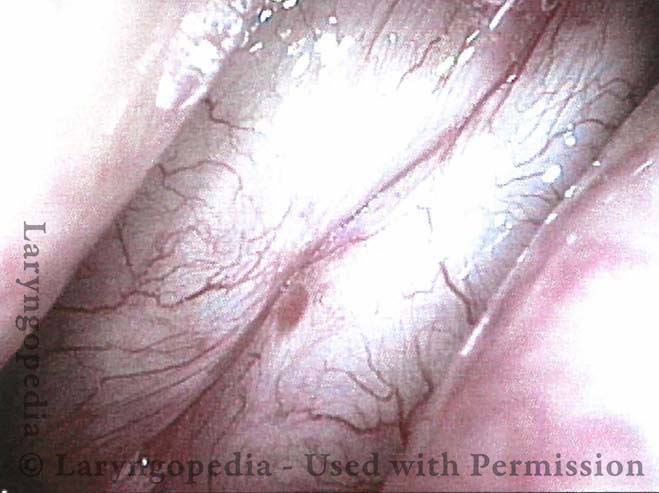
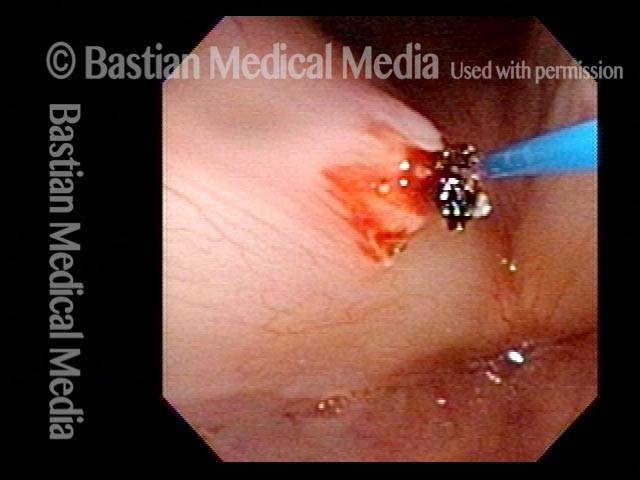
Hemorrhagic polyp, treated by thulium laser (3 of 8)
Hemorrhagic polyp, treated by thulium laser (3 of 8)
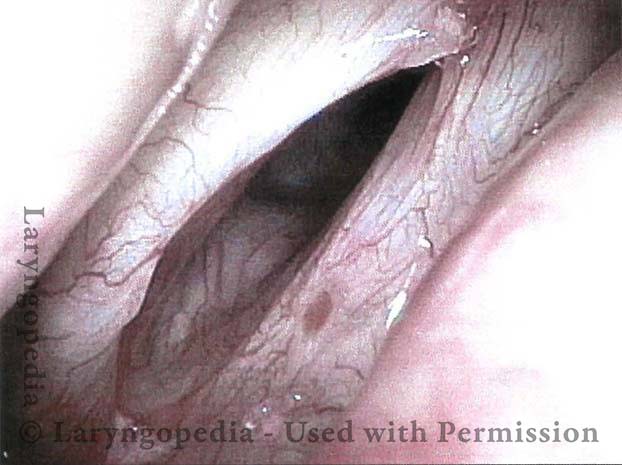
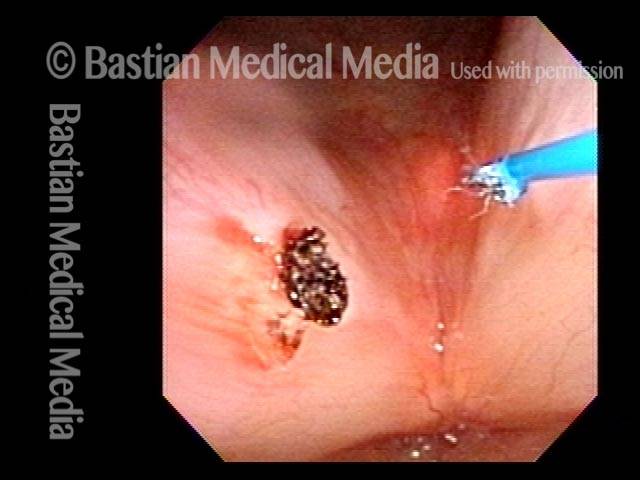
Hemorrhagic polyp, treated by thulium laser (4 of 8)
Hemorrhagic polyp, treated by thulium laser (4 of 8)
12 weeks after thulium laser treatment (5 of 8)
12 weeks after thulium laser treatment (5 of 8)
12 weeks after thulium laser treatment (6 of 8)
12 weeks after thulium laser treatment (6 of 8)
12 weeks after thulium laser treatment (7 of 8)
12 weeks after thulium laser treatment (7 of 8)
12 weeks after thulium laser treatment (8 of 8)
12 weeks after thulium laser treatment (8 of 8)
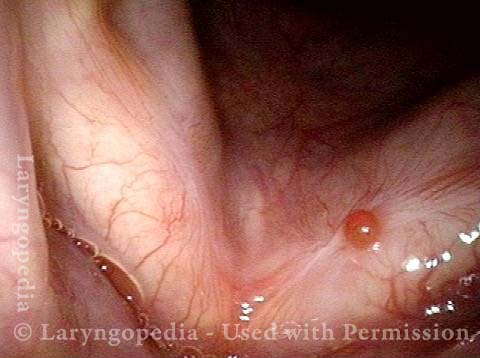
Capillary Ectasia, Before and After Laser Coagulation
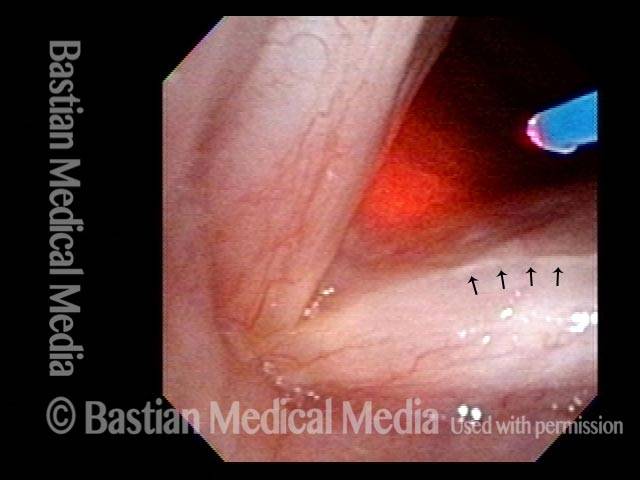
Capillary ectasia (1 of 3)
Capillary ectasia (1 of 3)
Capillary ectasia, right after laser coagulation (2 of 3)
Capillary ectasia, right after laser coagulation (2 of 3)
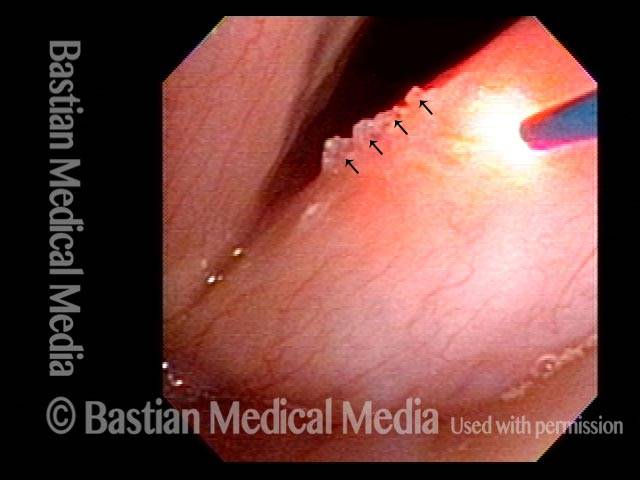
Capillary ectasia, 6 weeks after laser coagulation (3 of 3)
Capillary ectasia, 6 weeks after laser coagulation (3 of 3)
Lidocaine Injection for Aggressive “Office” Laser Treatments
Laser ablations performed in office (1 of 6)
Laser ablations performed in office (1 of 6)
Infiltrating anesthetic (2 of 6)
Infiltrating anesthetic (2 of 6)
Thulium laser procedure (3 of 6)
Thulium laser procedure (3 of 6)
Post-surgery (4 of 6)
Post-surgery (4 of 6)
Six weeks post-surgery (5 of 6)
Six weeks post-surgery (5 of 6)
Second laser sugery (6 of 6)
Second laser sugery (6 of 6)
Perfect Candidate for Thulium Laser
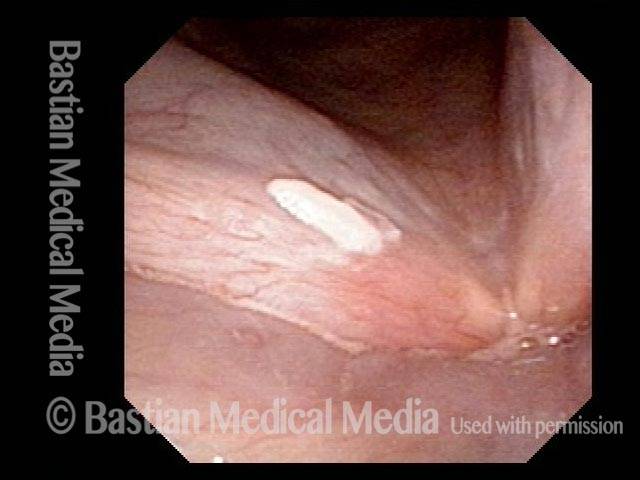
Lesion (1 of 4)
Lesion (1 of 4)
Lesion under narrow-band light (2 of 4)
Lesion under narrow-band light (2 of 4)
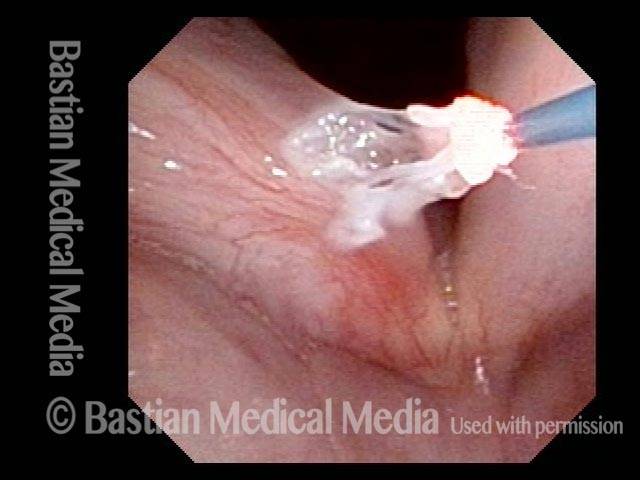
Coagulated with thulium laser (3 of 4)
Coagulated with thulium laser (3 of 4)
Finishing up (4 of 4)
Finishing up (4 of 4)
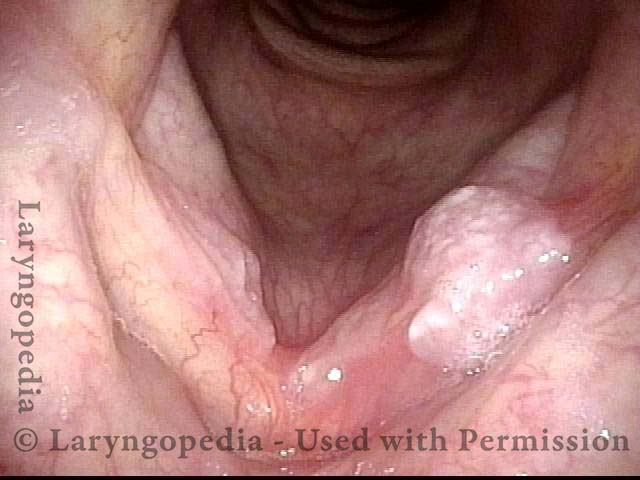
Leukoplakia Battled Over Time
Leukoplakia (1 of 8)
Leukoplakia (1 of 8)
Spilled Milk (2 of 8)
Spilled Milk (2 of 8)
Thulium laser (3 of 8)
Thulium laser (3 of 8)
Coagulated tissue (4 of 8)
Coagulated tissue (4 of 8)
Leukoplakia (5 of 8)
Leukoplakia (5 of 8)
Detachment (6 of 8)
Detachment (6 of 8)
Superficial vascular pattern (7 of 8)
Superficial vascular pattern (7 of 8)
Coagulated tissue (8 of 8)
Coagulated tissue (8 of 8)
Leukoplakia, Before, During, and After Laser Coagulation
Leukoplakia, not yet seen (1 of 6)
Leukoplakia, not yet seen (1 of 6)
Leukoplakia (2 of 6)
Leukoplakia (2 of 6)
Leukoplakia (3 of 6)
Leukoplakia (3 of 6)
Leukoplakia, coagulated by laser (4 of 6)
Leukoplakia, coagulated by laser (4 of 6)
Leukoplakia, 3 months after laser treatment (5 of 6)
Leukoplakia, 3 months after laser treatment (5 of 6)
Leukoplakia, 3 months after laser treatment (6 of 6)
Leukoplakia, 3 months after laser treatment (6 of 6)
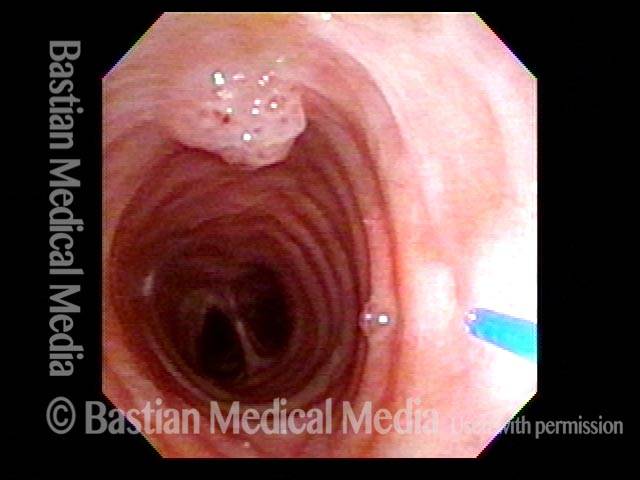
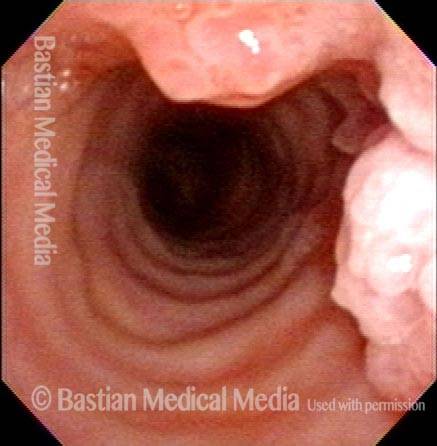
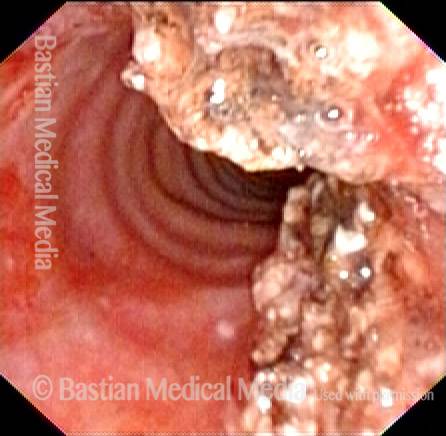
Mid-Tracheal Papilloma, Treated By Thulium Laser
Mid-tracheal papilloma, being treated by thulium laser (1 of 5)
Mid-tracheal papilloma, being treated by thulium laser (1 of 5)
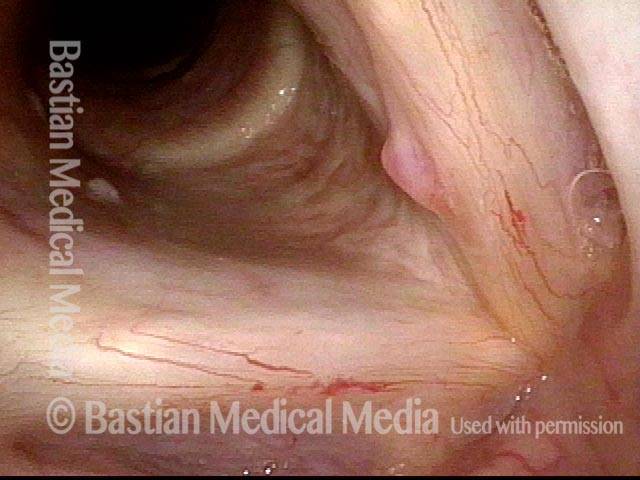
Months after treatment: no papilloma (5 of 5)
Months after treatment: no papilloma (5 of 5)
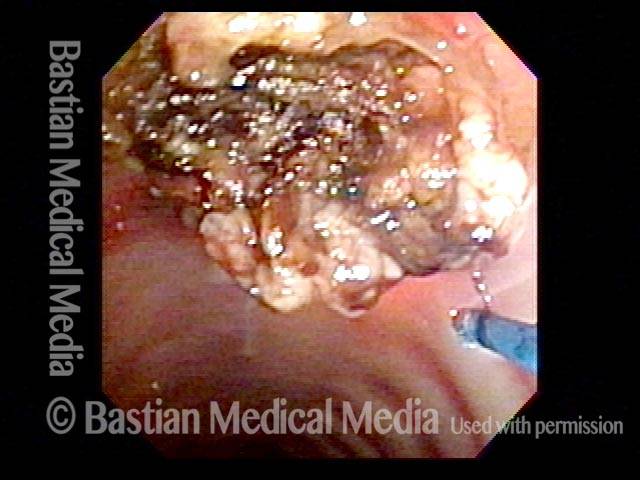
Mid-tracheal papilloma, being treated by thulium laser (2 of 5)
Mid-tracheal papilloma, being treated by thulium laser (2 of 5)
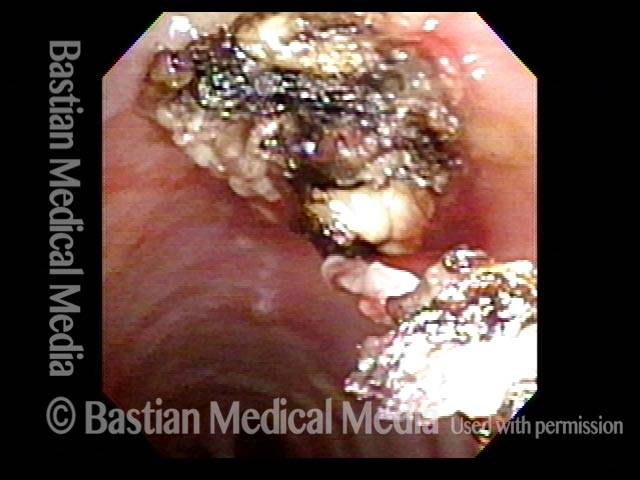
Mid-tracheal papilloma, being treated by thulium laser (3 of 5)
Mid-tracheal papilloma, being treated by thulium laser (3 of 5)
Mid-tracheal papilloma, being treated by thulium laser (4 of 5)
Mid-tracheal papilloma, being treated by thulium laser (4 of 5)
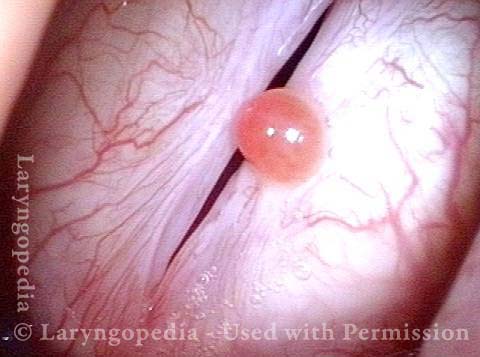
Capillary Ectasia and Hemorrhagic Polyp, Treated by Thulium Laser
Capillary ectasia and hemorrhagic polyp (1 of 7)
Capillary ectasia and hemorrhagic polyp (1 of 7)
Capillary ectasia and hemorrhagic polyp (2 of 7)
Capillary ectasia and hemorrhagic polyp (2 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (3 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (3 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (4 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (4 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (5 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (5 of 7)
Vocal cord margin (6 of 7)
Vocal cord margin (6 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (7 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (7 of 7)
Thulium Laser Surgery, With Local Anesthetic Injection, to Treat Leukoplakia
Leukoplakia, about to be treated with laser (1 of 4)
Leukoplakia, about to be treated with laser (1 of 4)
Injection of local anesthetic (2 of 4)
Injection of local anesthetic (2 of 4)
Injection of local anesthetic (3 of 4)
Injection of local anesthetic (3 of 4)
Right after thulium laser treatment (4 of 4)
Right after thulium laser treatment (4 of 4)
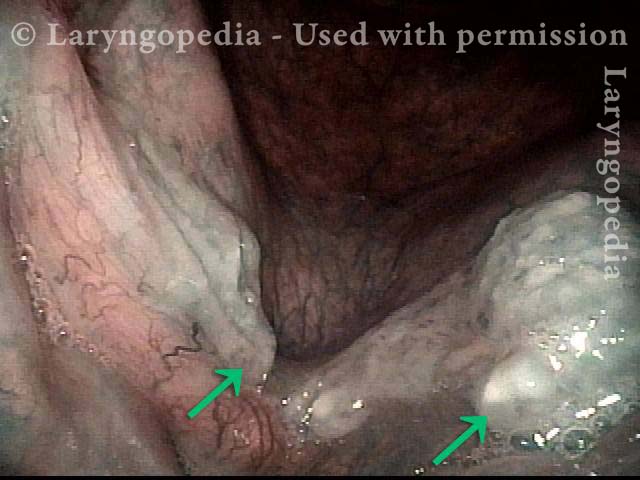
Tracheal Papillomas and the Thulium Laser
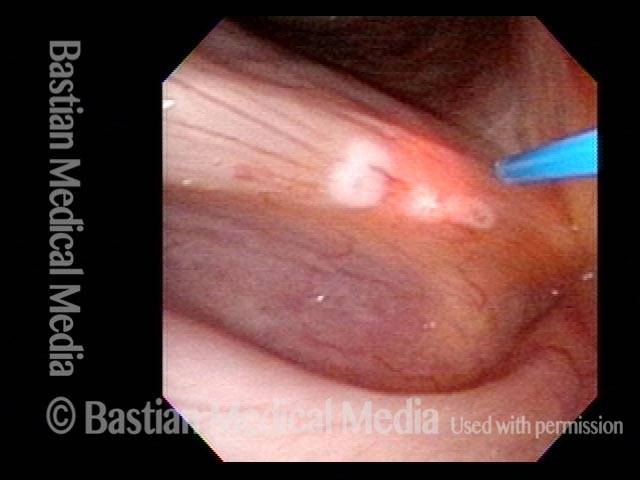
HPV 11 (1 of 2)
HPV 11 (1 of 2)
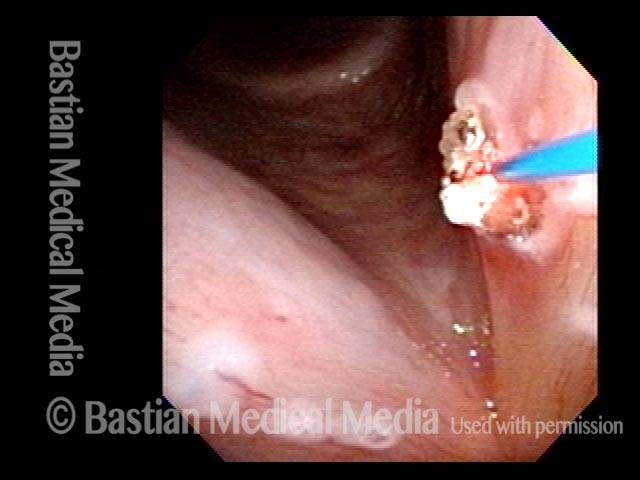
Post laser coagulation (2 of 2)
Post laser coagulation (2 of 2)
Office-Based Surgery When General Anesthesia Is too Risky
Involuntary inspiratory voice (1 of 6)
Involuntary inspiratory voice (1 of 6)
Laser posterior commissuroplasty (2 of 6)
Laser posterior commissuroplasty (2 of 6)
During the commissuroplasty (3 of 6)
During the commissuroplasty (3 of 6)
Deepening divot (4 of 6)
Deepening divot (4 of 6)
Inspiratory indrawing decreased (5 of 6)
Inspiratory indrawing decreased (5 of 6)
Phonation (6 of 6)
Phonation (6 of 6)
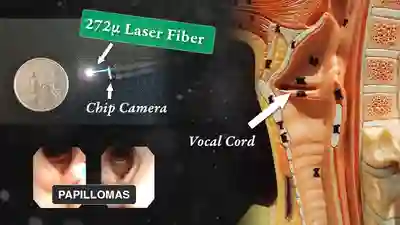
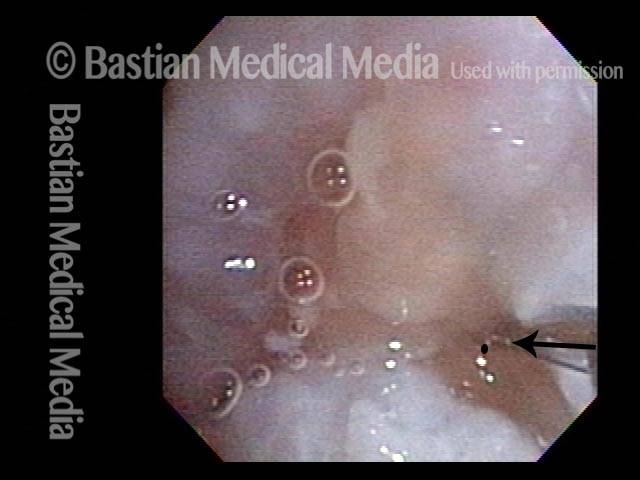
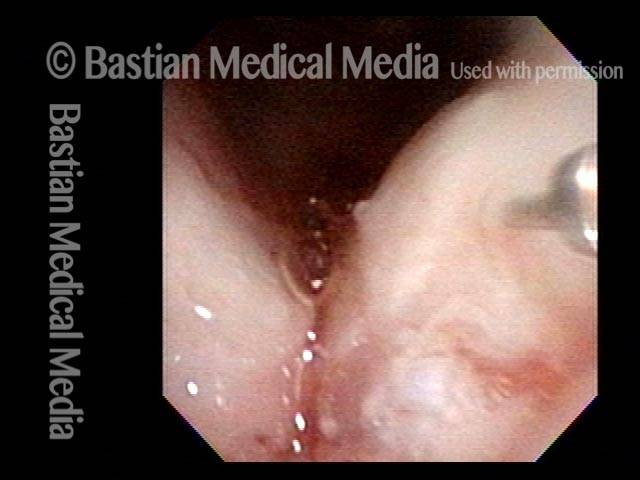
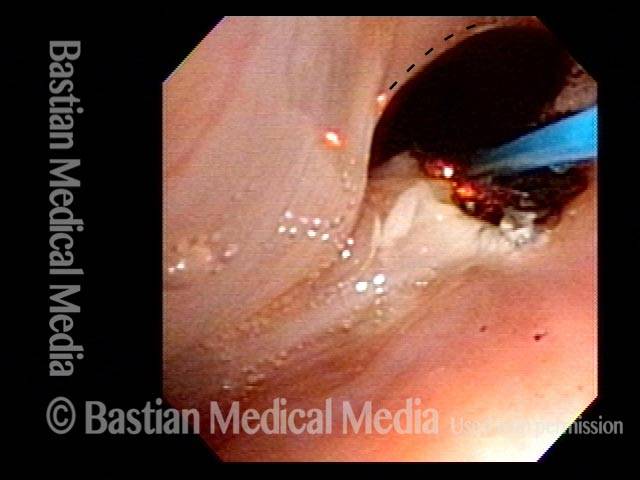
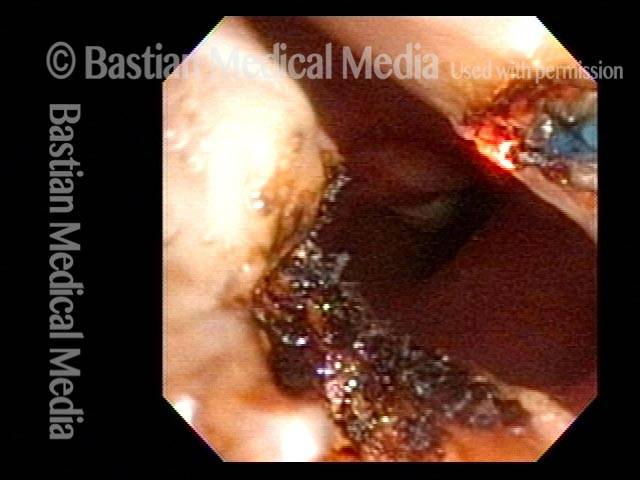
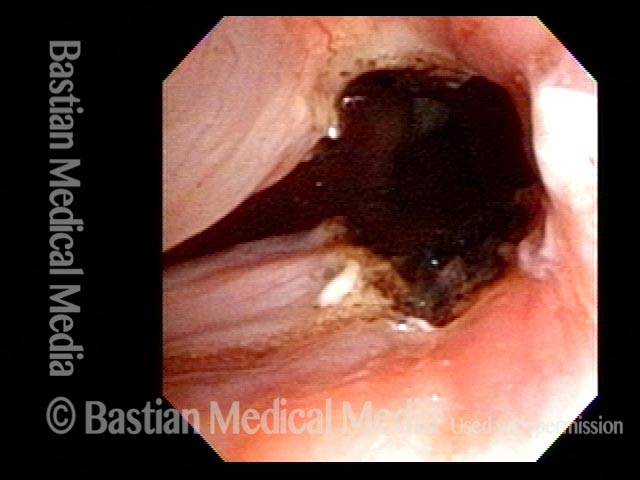
Office Coagulation of Laryngeal Papillomas
This man has had RRP (laryngeal papillomas) for many years. He has had laser ablations both in the O.R. under general anesthesia, and in an “office” laser room.
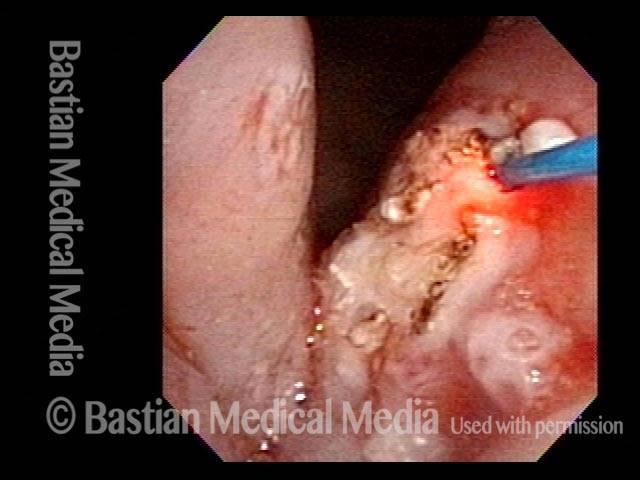
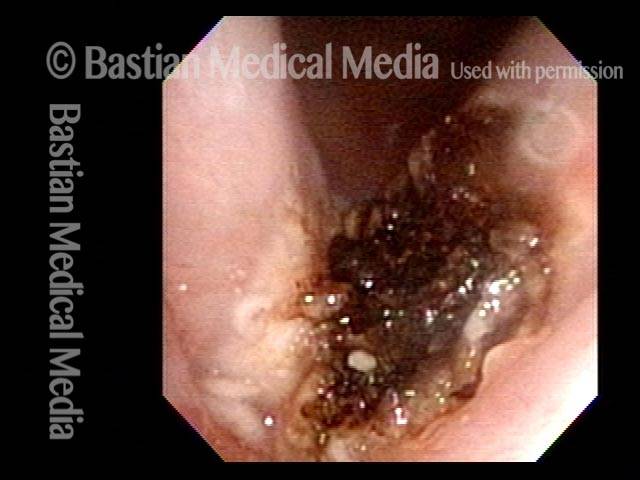
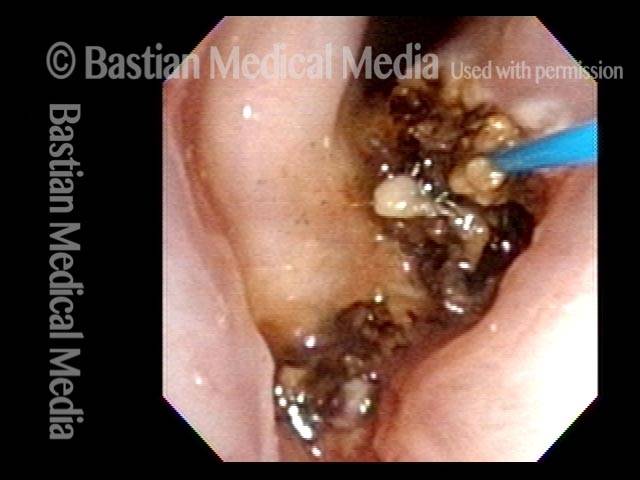
This video is an operative sequence in the latter setting. He is sitting in a chair and tolerating this procedure with the assistance of topical anesthesia and bilateral superior laryngeal nerve blocks, after which he can even drive himself home. In addition to thulium laser coagulation of the papillomas, this video also illustrates how patient movement and obscuring secretions must be managed.

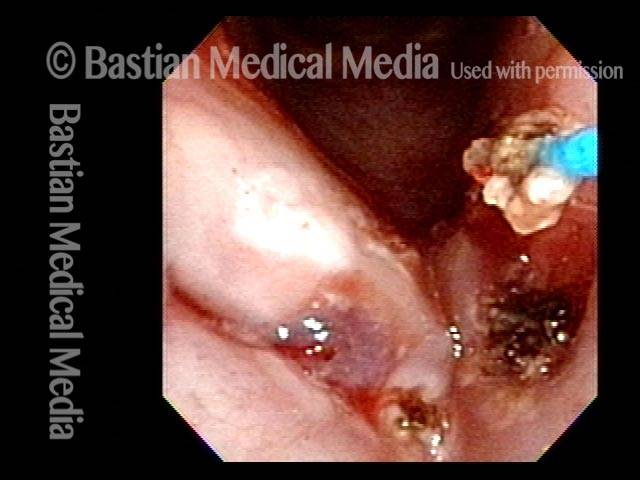
Thulium laser
This patient is sitting in a chair under topical anesthesia. He is able to minimize movement of his vocal cords, and is therefore a “perfect” candidate for office-based thulium laser ablation of residual laryngeal papilloma