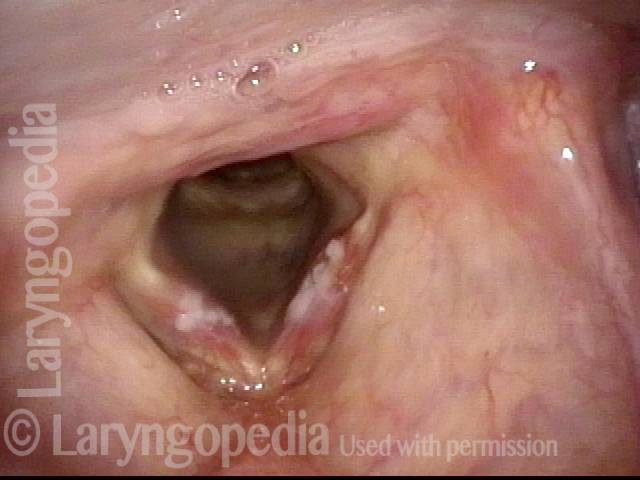
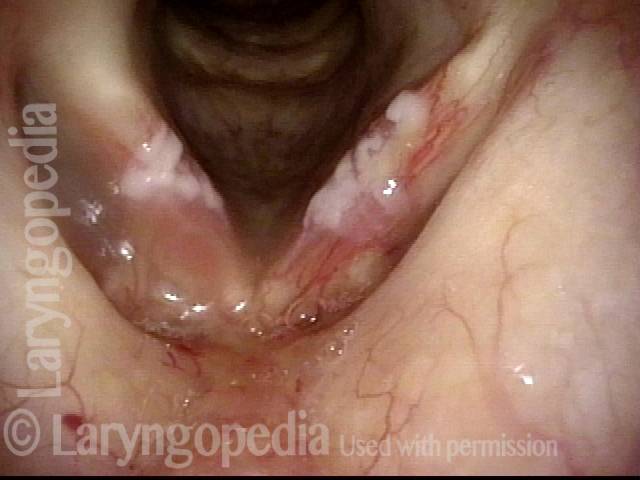
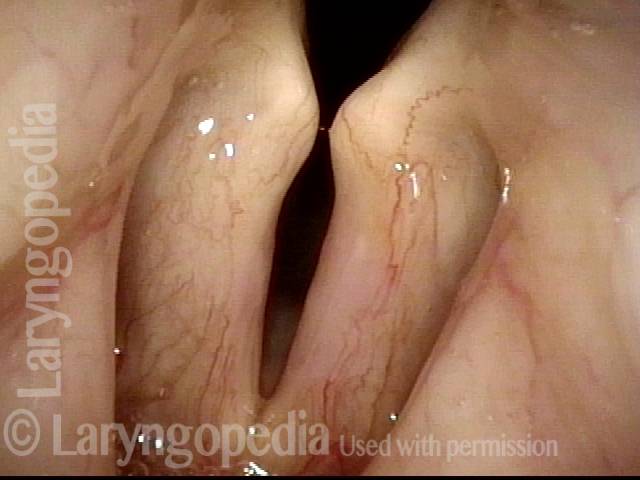
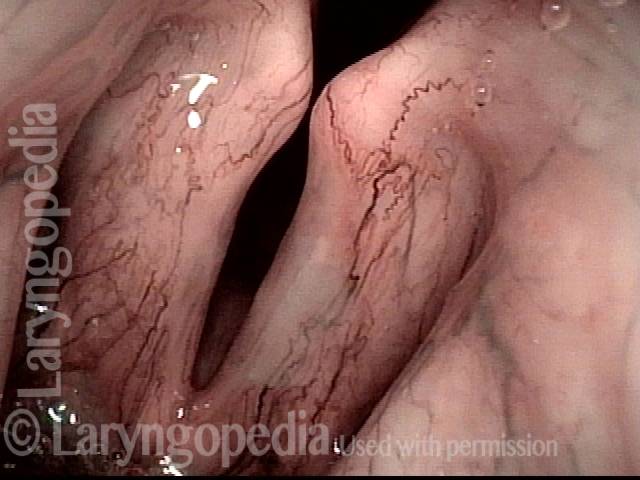
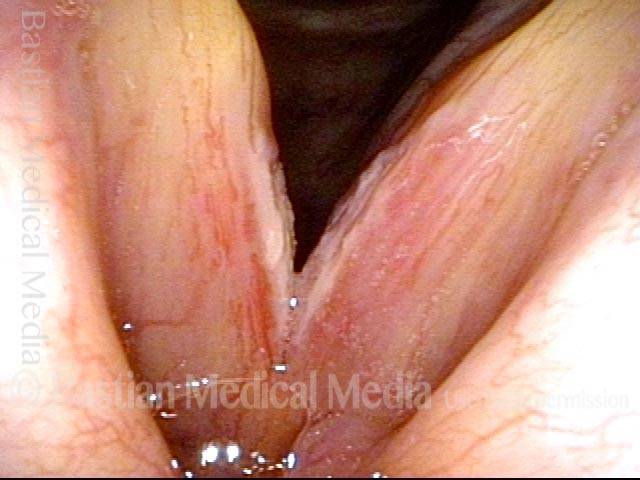
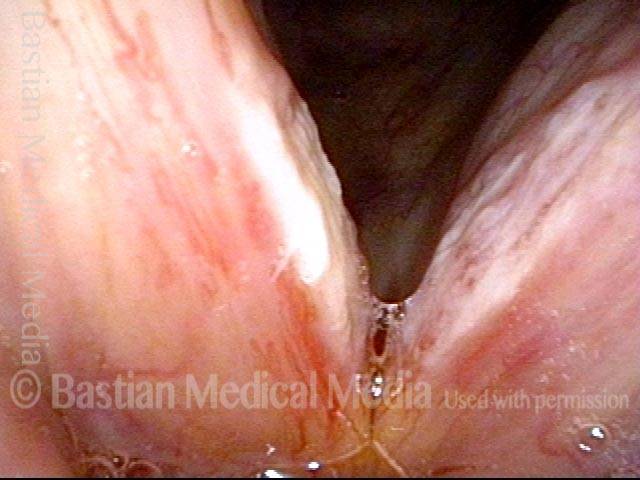
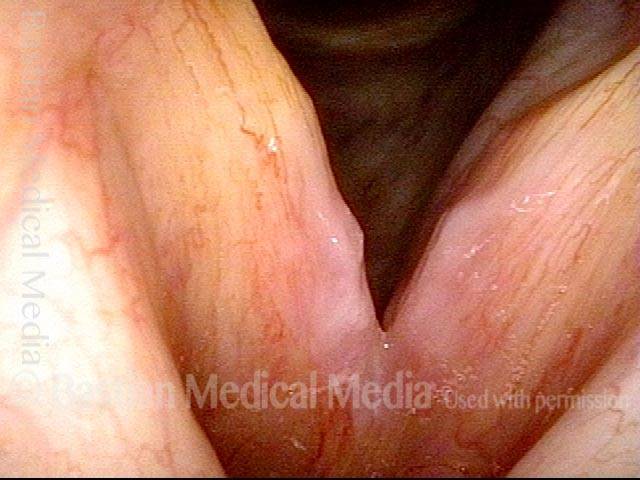
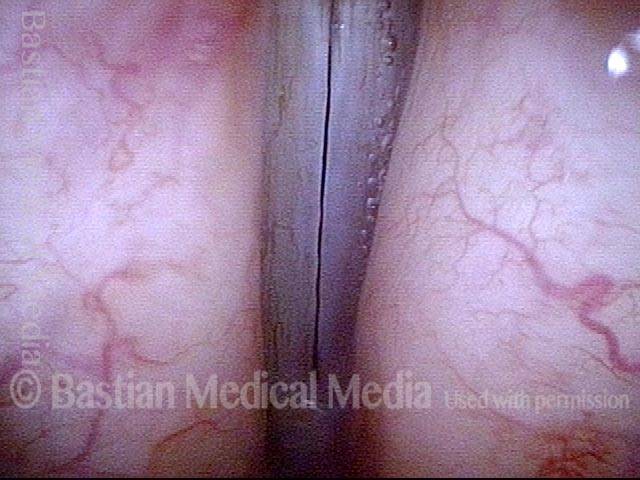
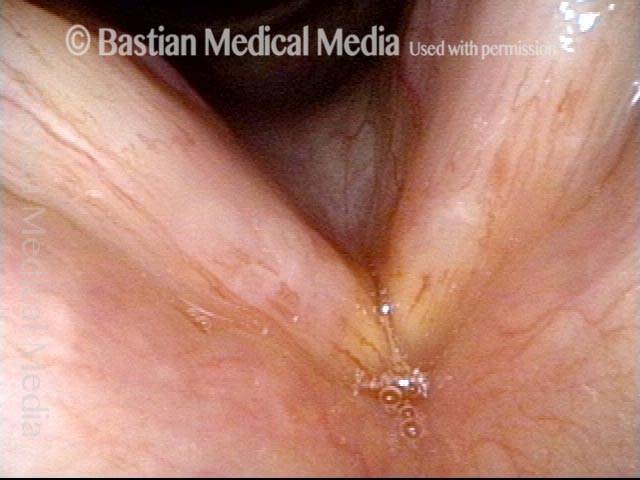
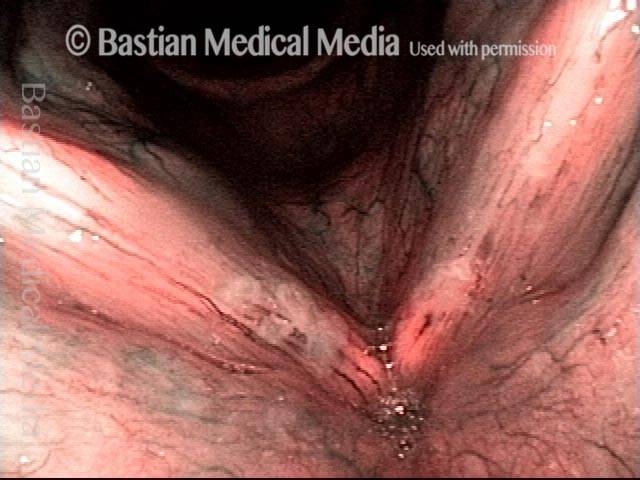
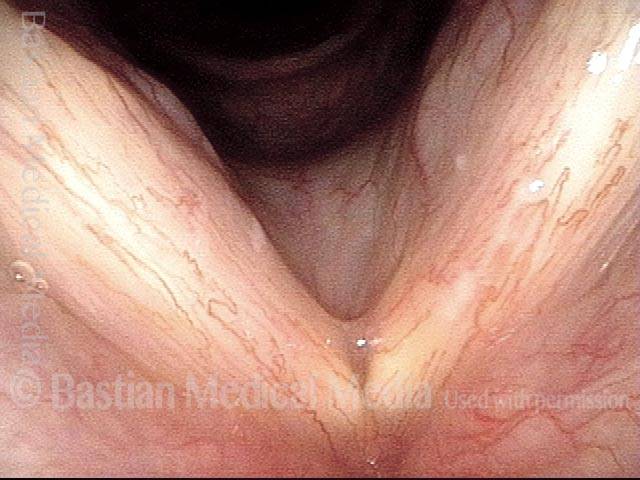
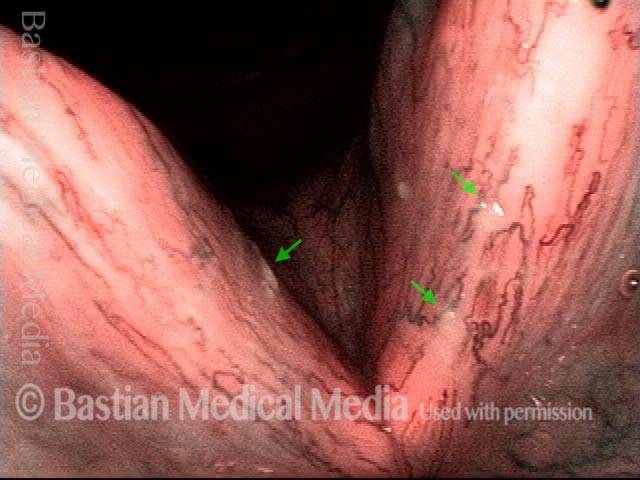
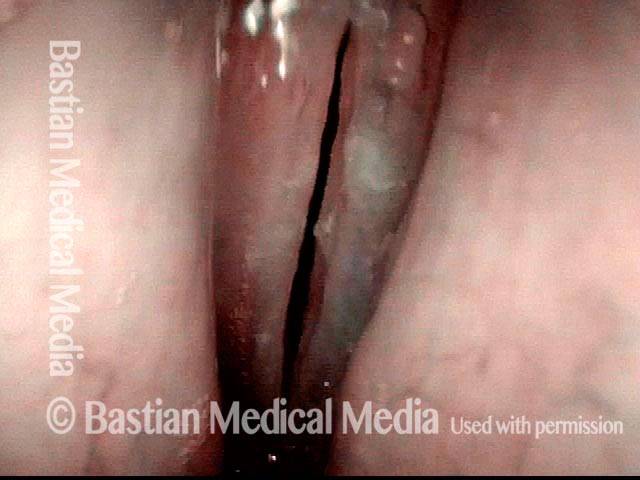
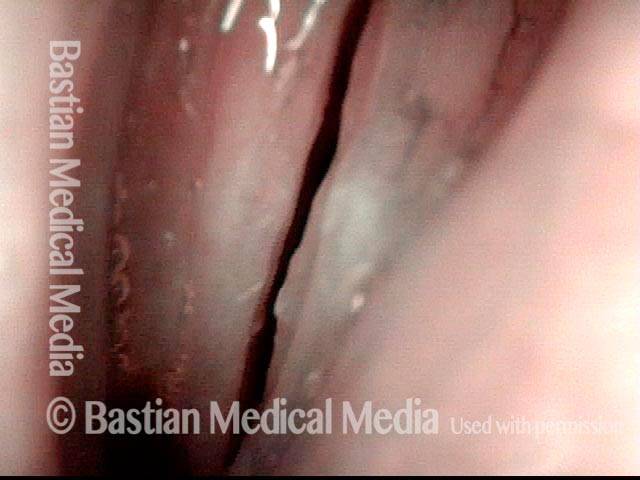
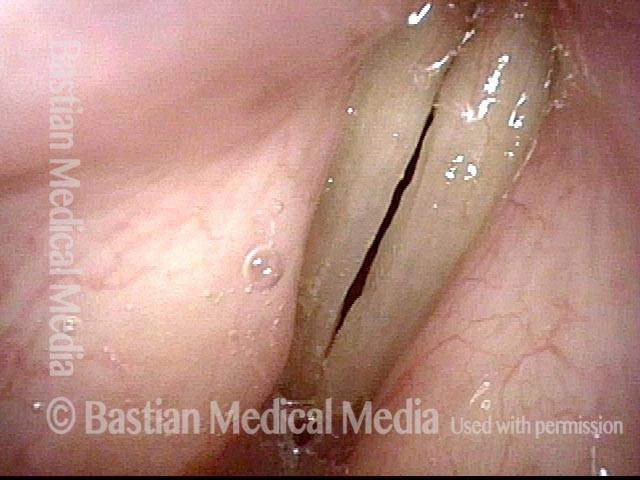
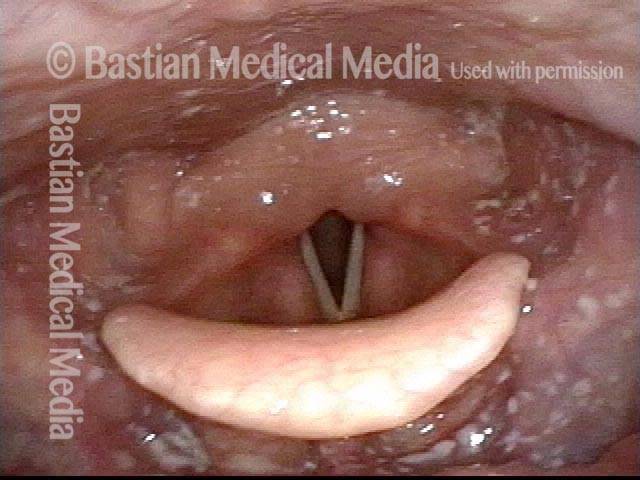
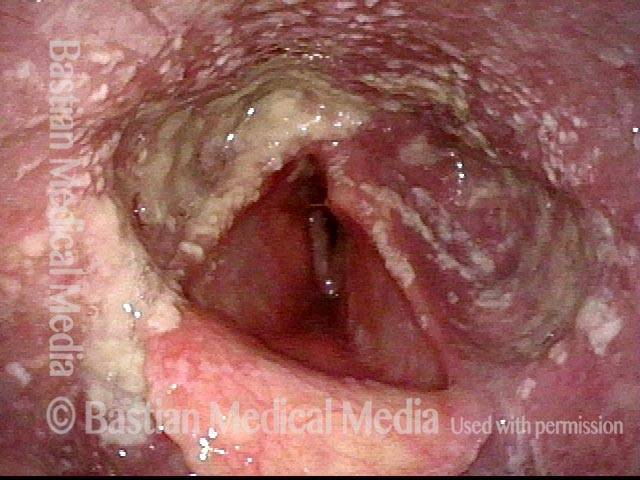
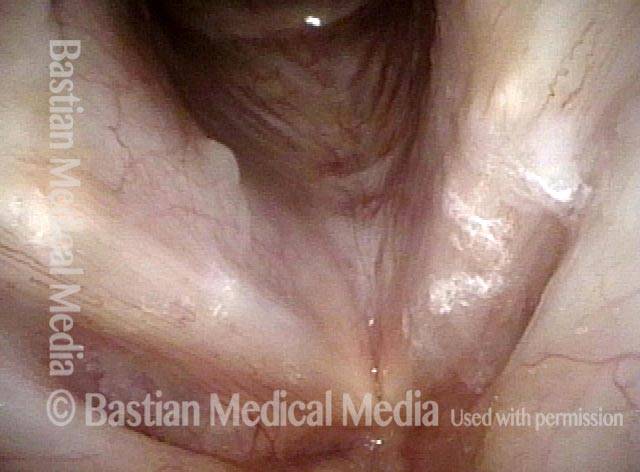
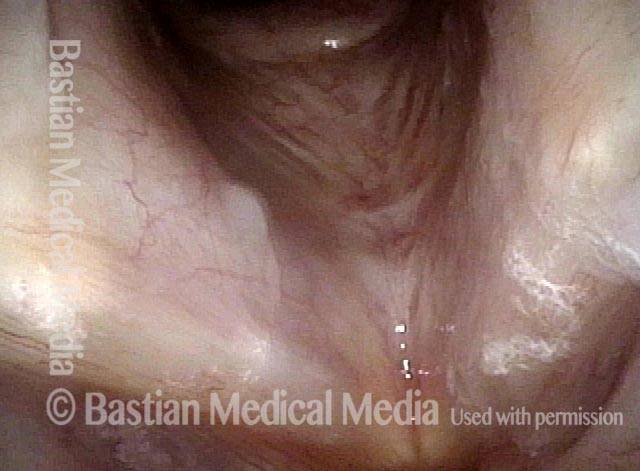
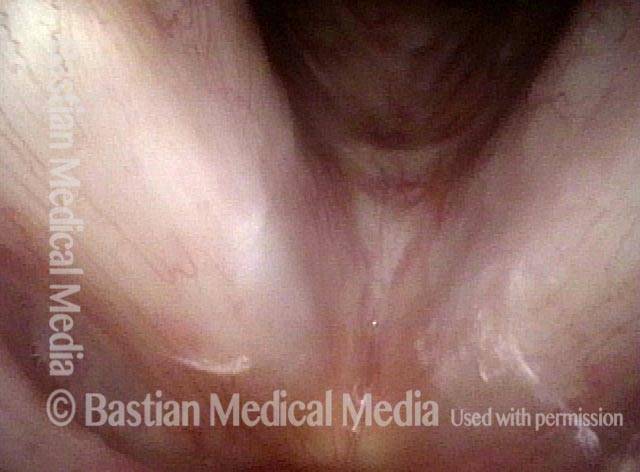
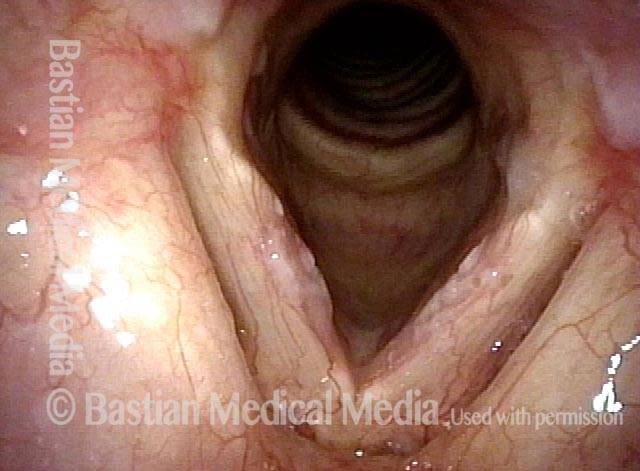
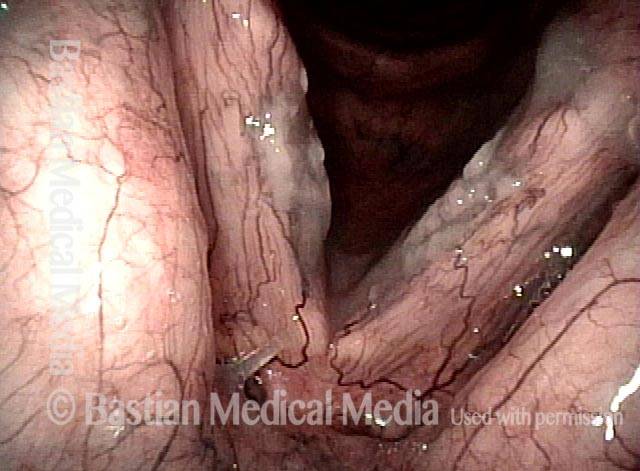
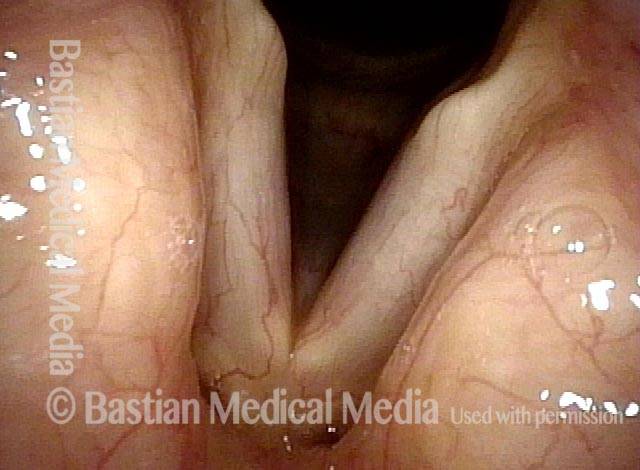
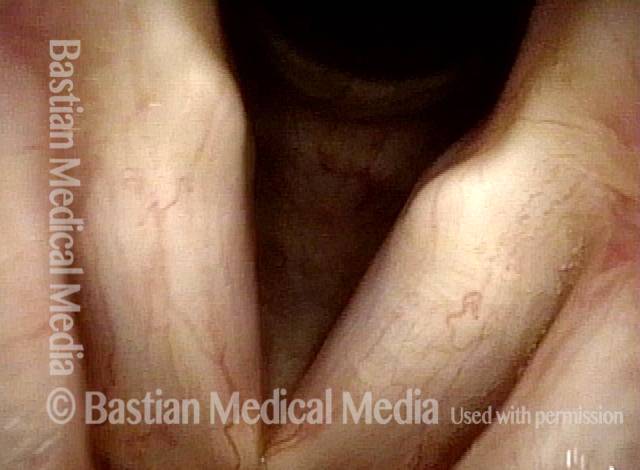
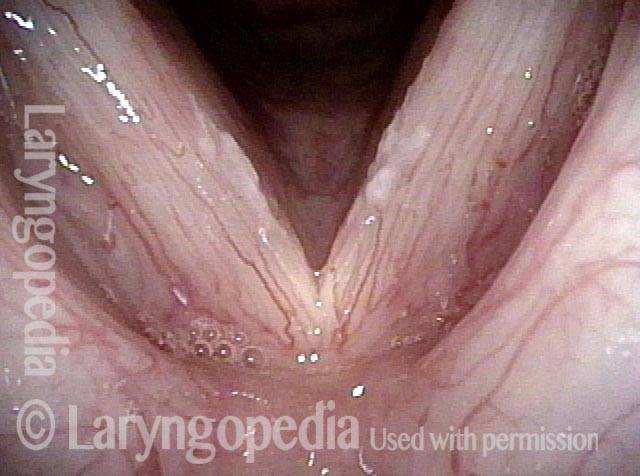
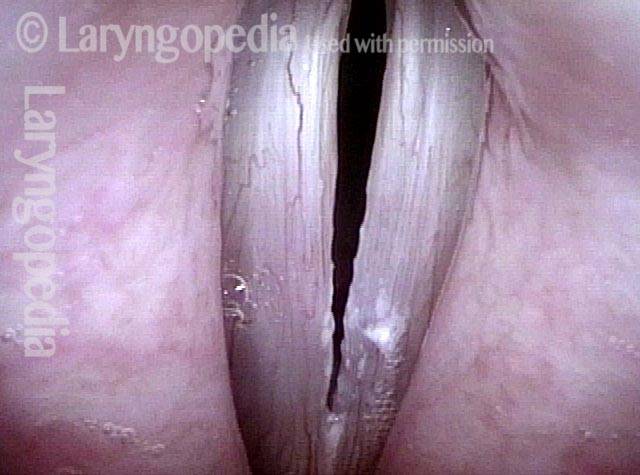
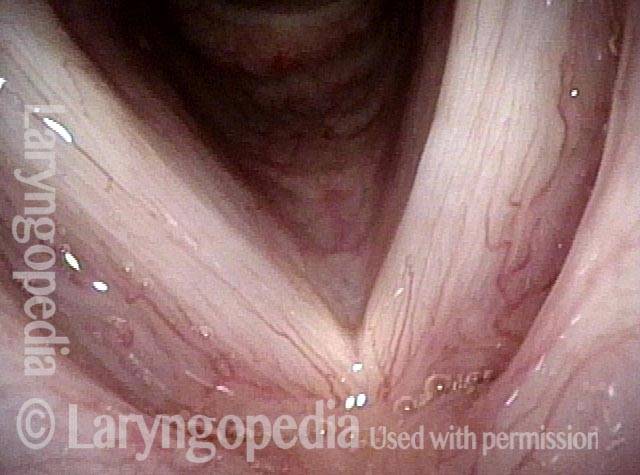
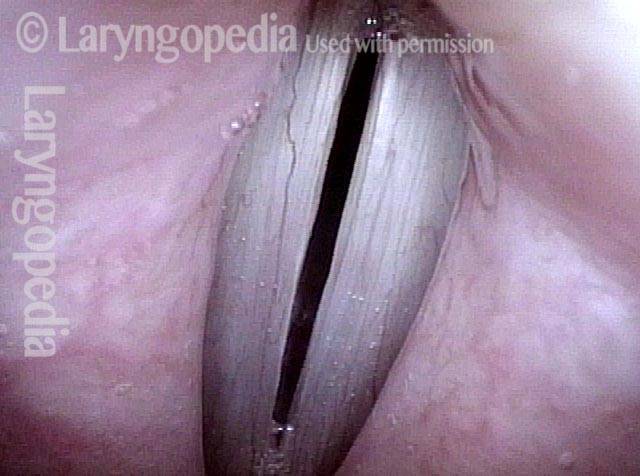
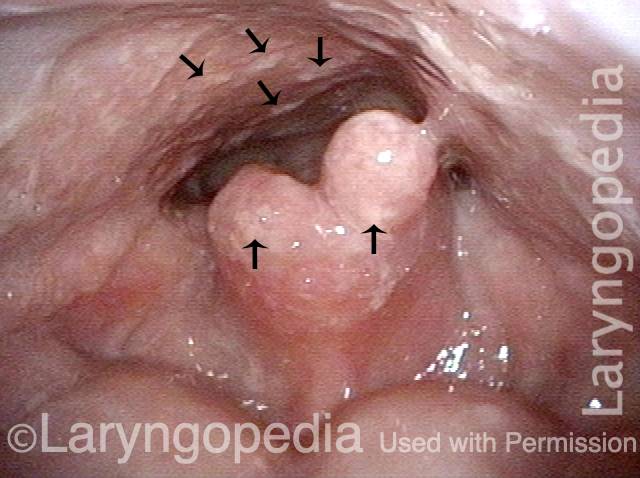
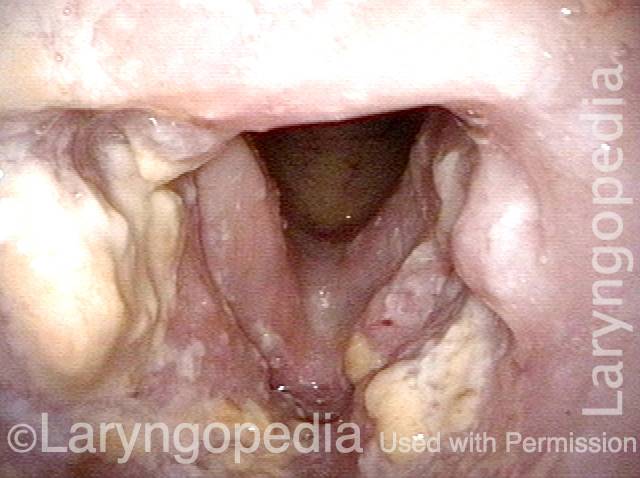
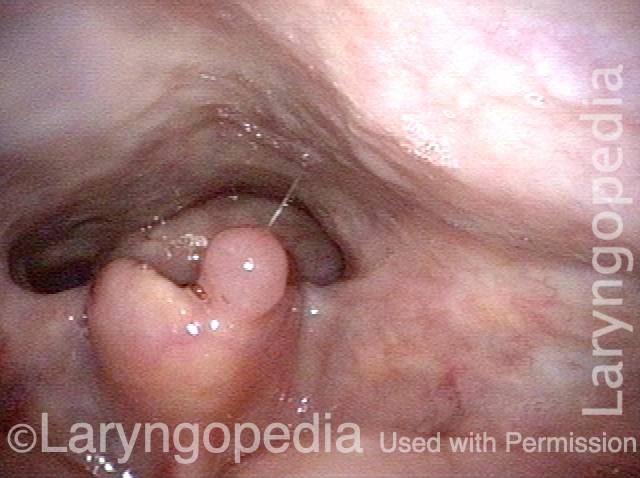
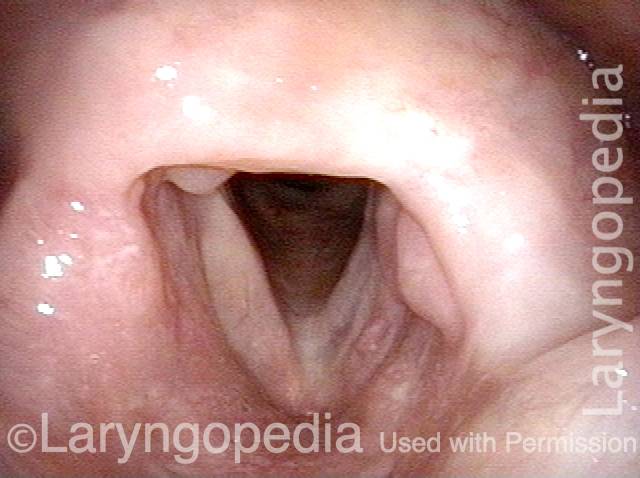
Infection with candida albicans, an ubiquitous commensal organism in the upper aerodigestive tract, usually on the vocal cord mucosa. While this organism normally causes no problem, under certain circumstances it can overgrow. These circumstances include:
(1) When other (competing) normal flora are killed through administration of antibiotics.
(2) When surface immunity of the mucosa is decreased via inhalation of steroid medication (e.g. asthma).
(3) When the individual is immunosuppressed by disease (e.g. diabetes) or other drugs.
Typical symptoms of candida laryngitis and pharyngitis include slight sore throat and hoarseness. Treatment may consist of reducing or withdrawing listed potentiators, or using an antifungal agent such as fluconazole.