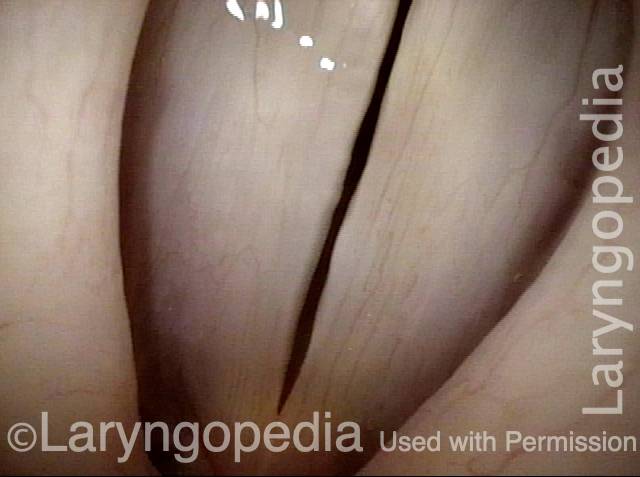
Capillary Ectasia
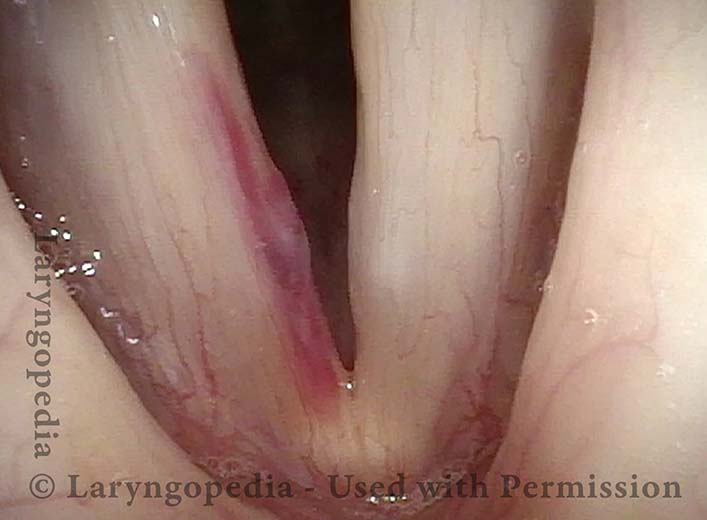
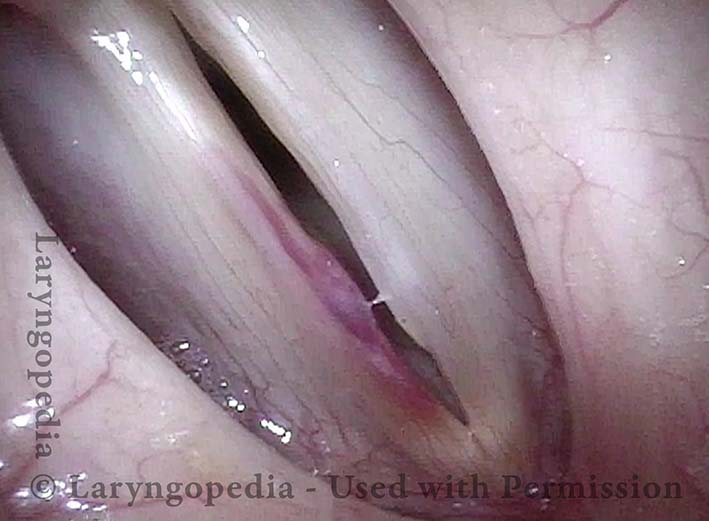
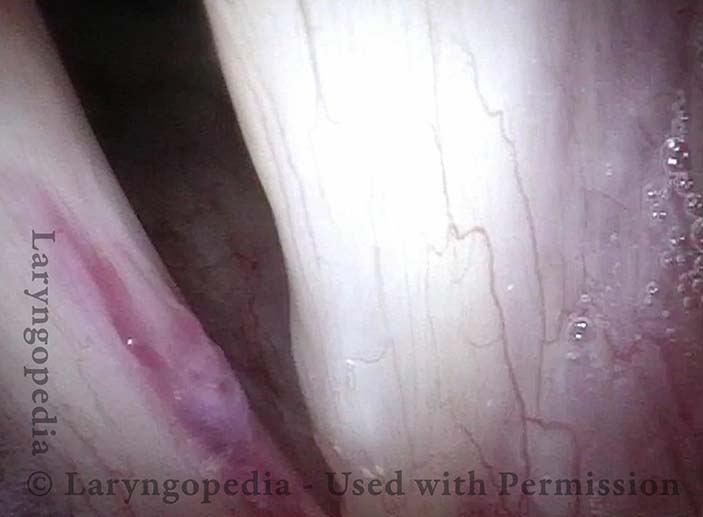
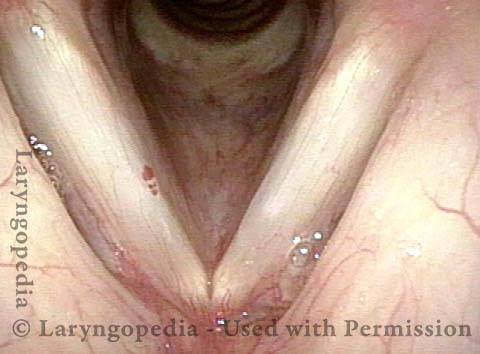
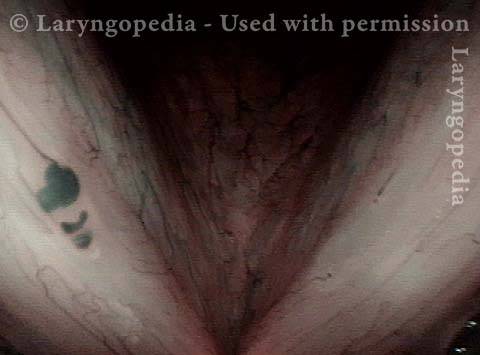
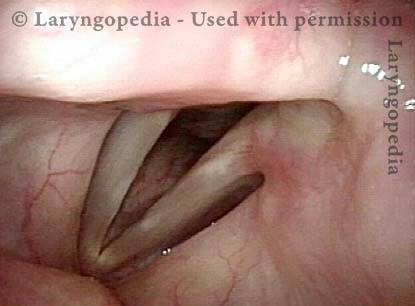
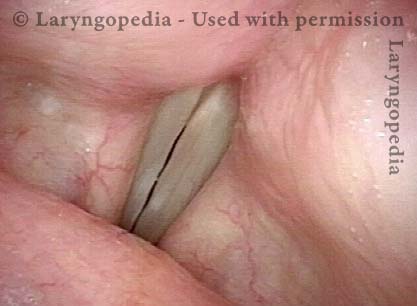
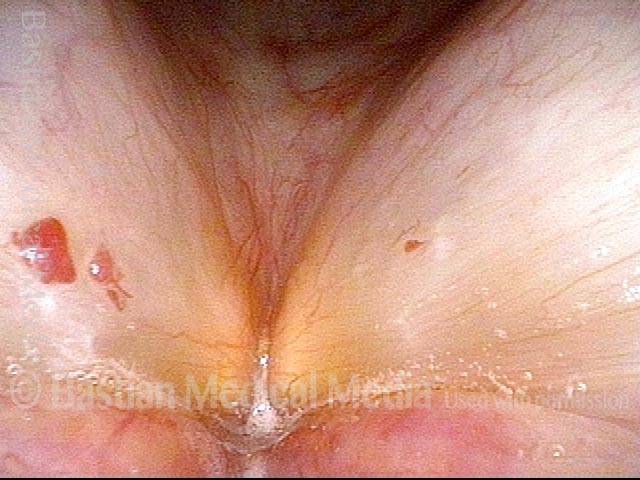
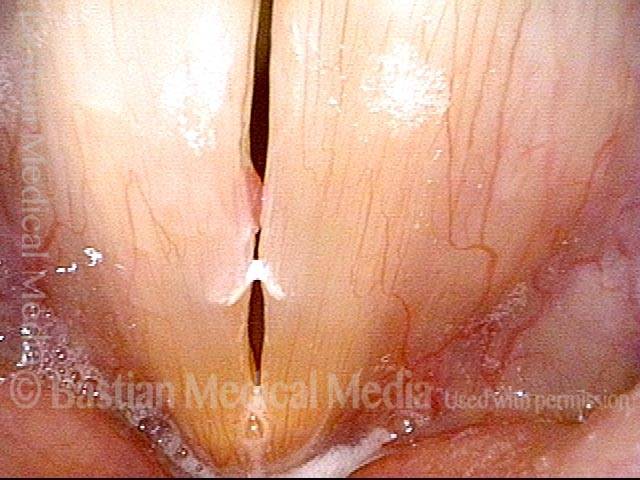
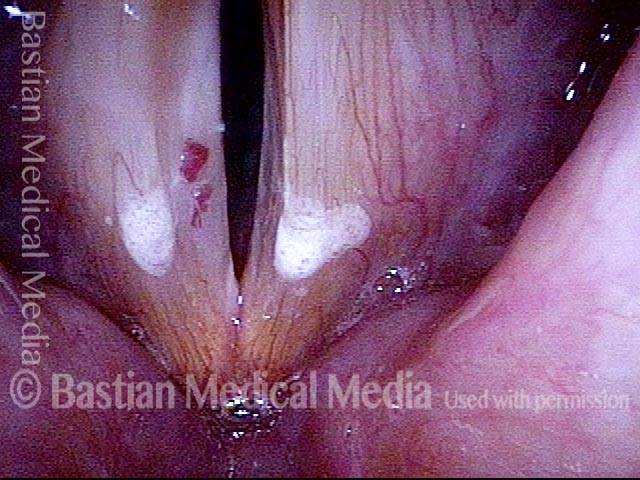
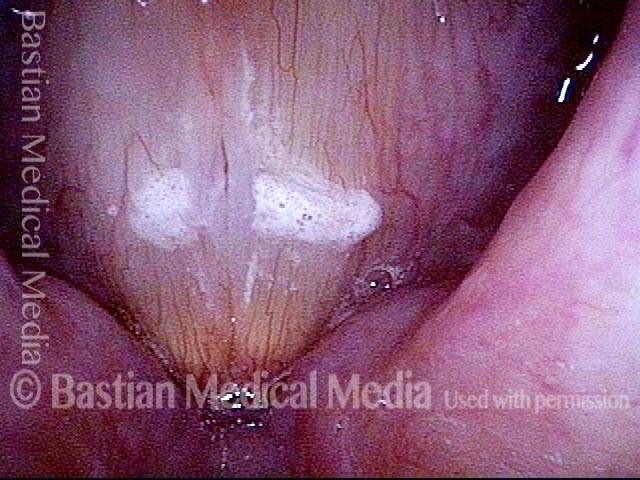
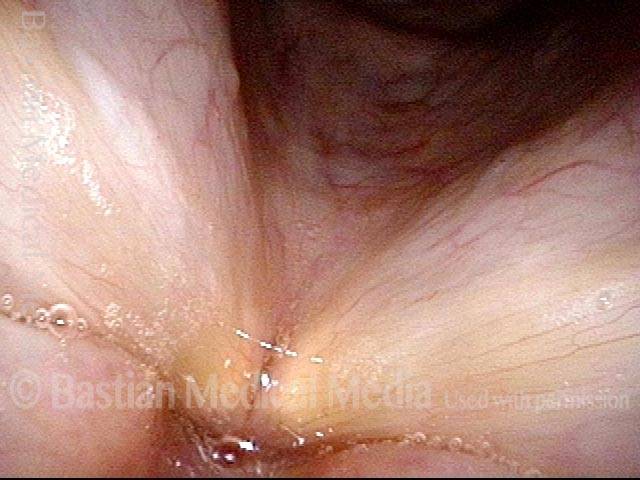
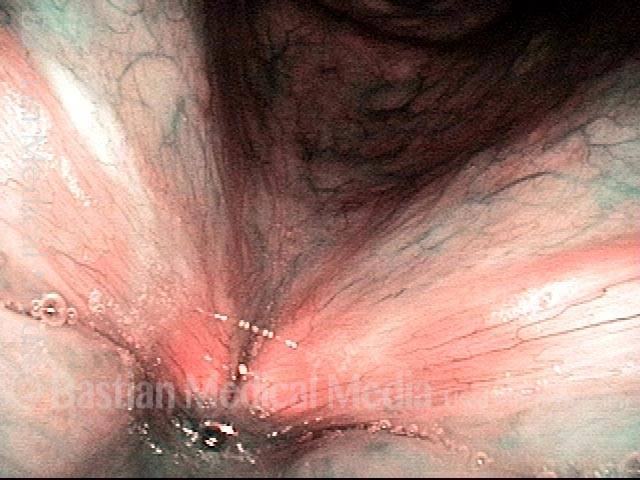
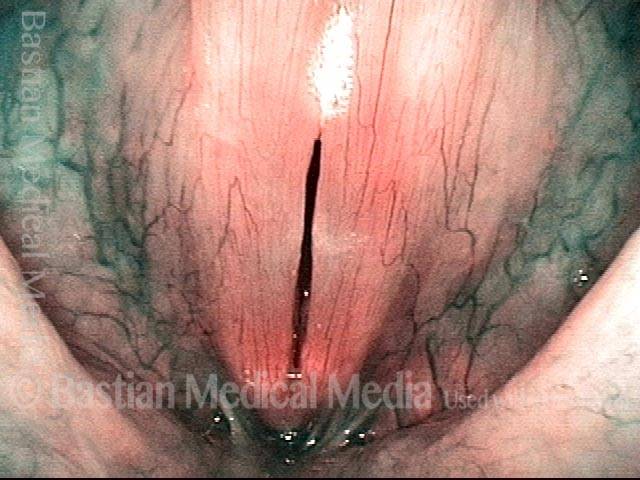
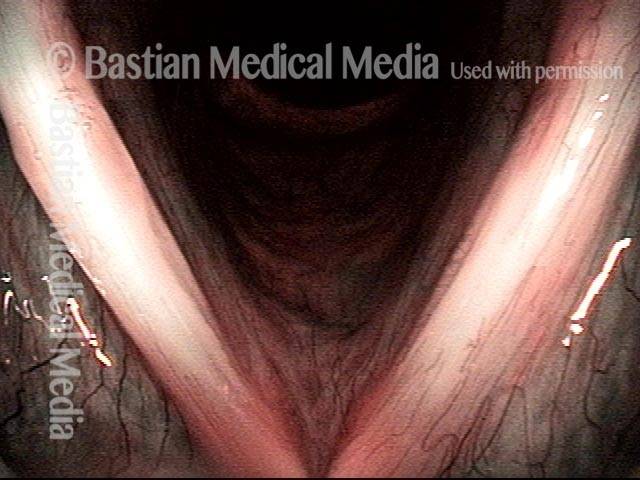
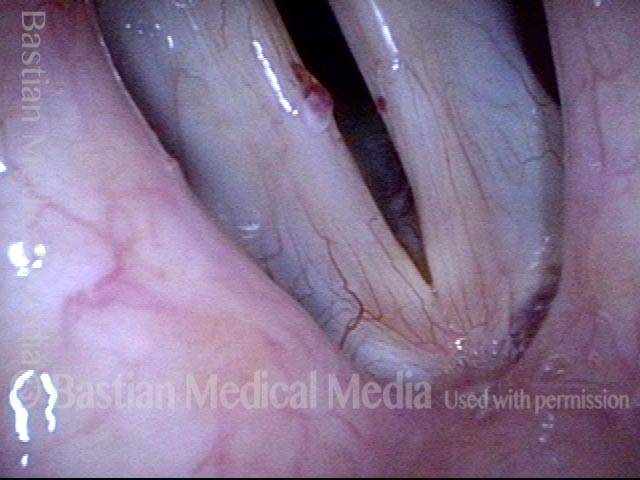
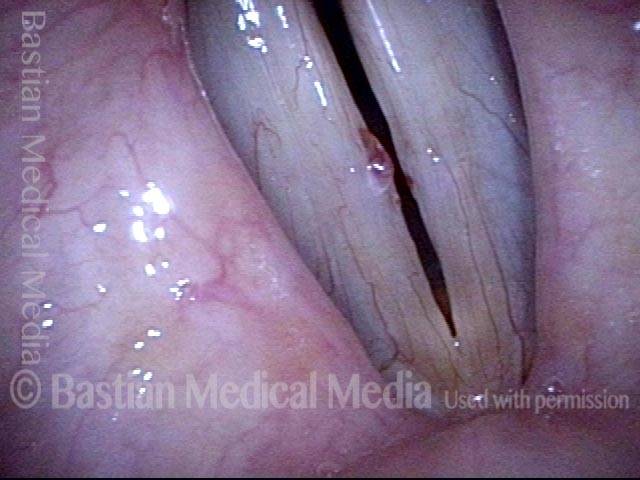
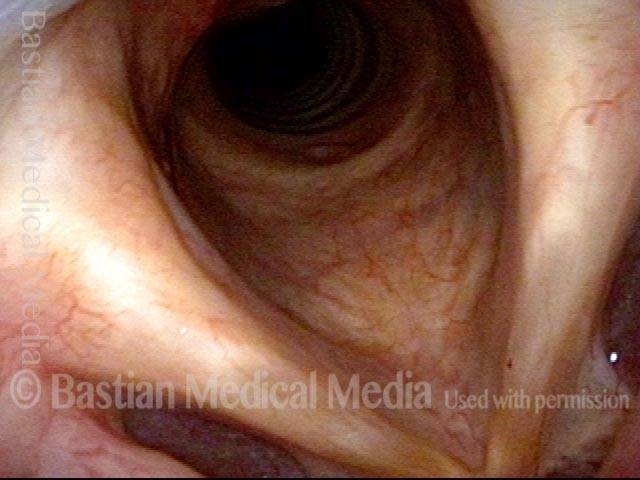
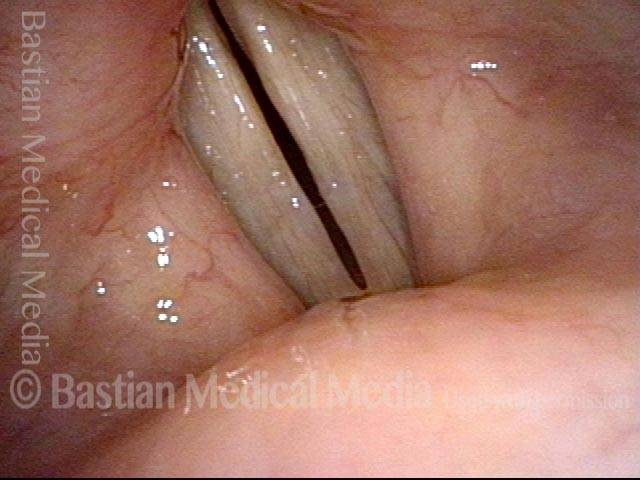
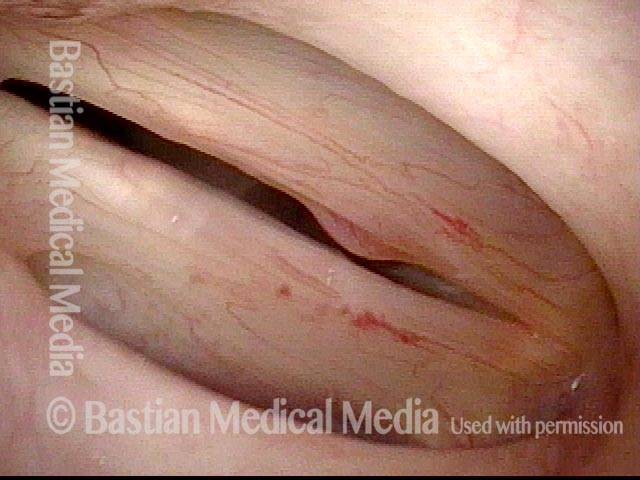
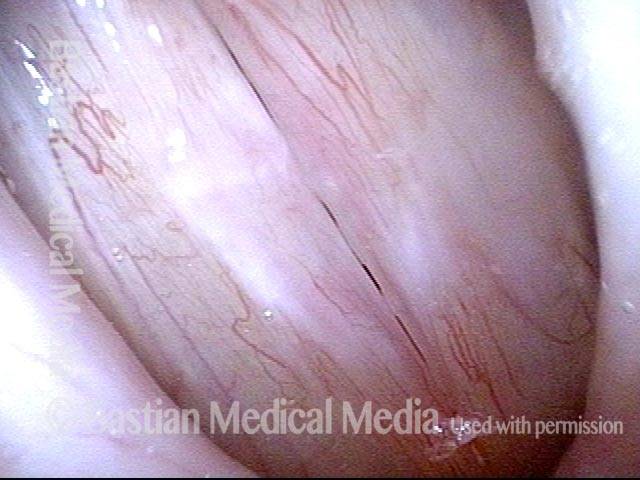
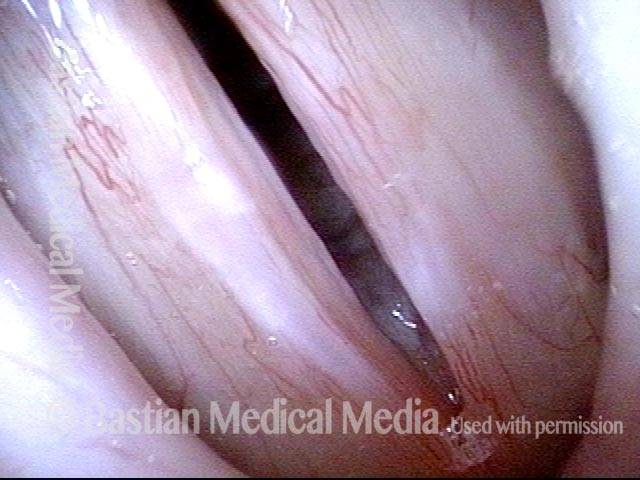
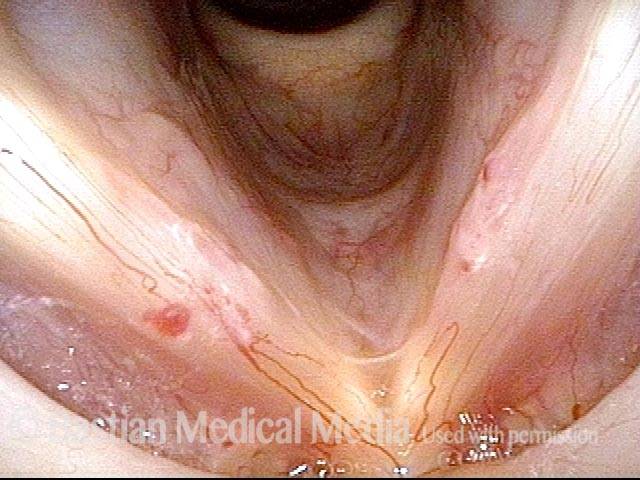
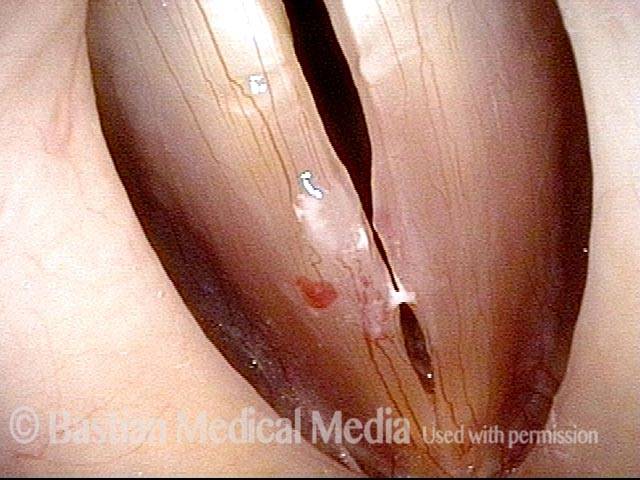
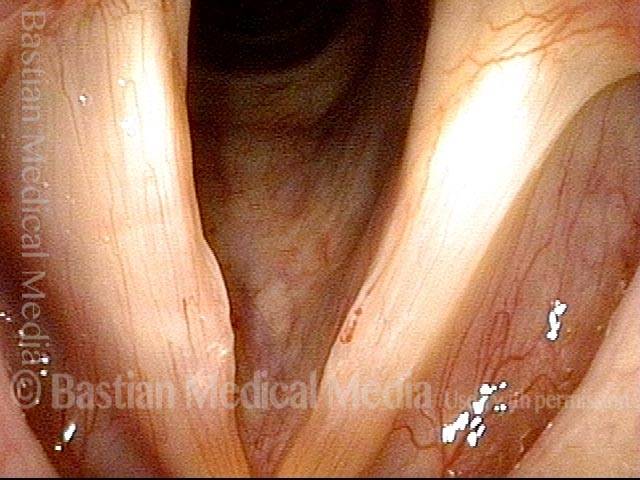
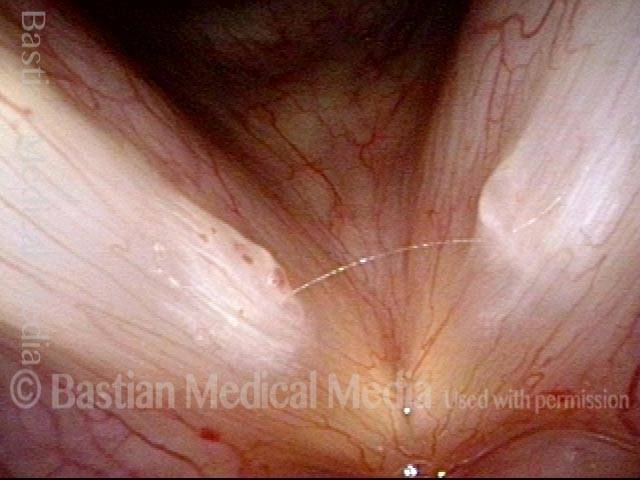
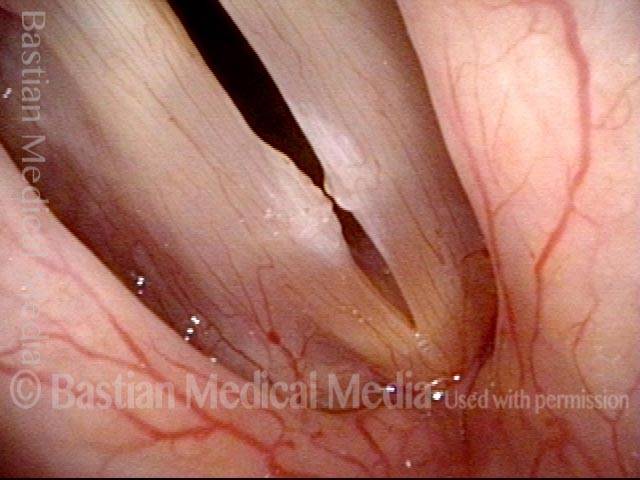
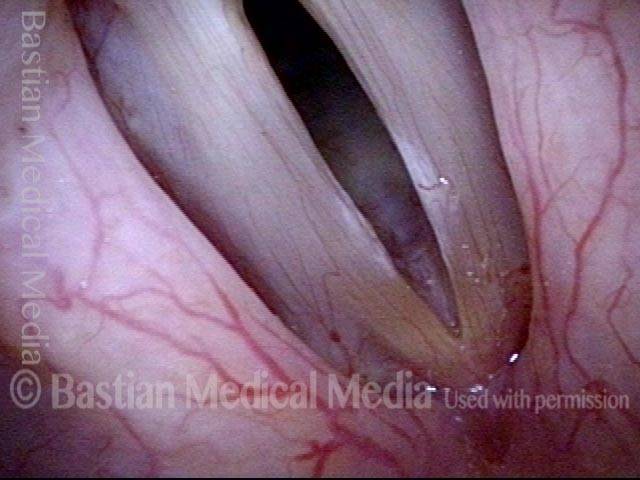
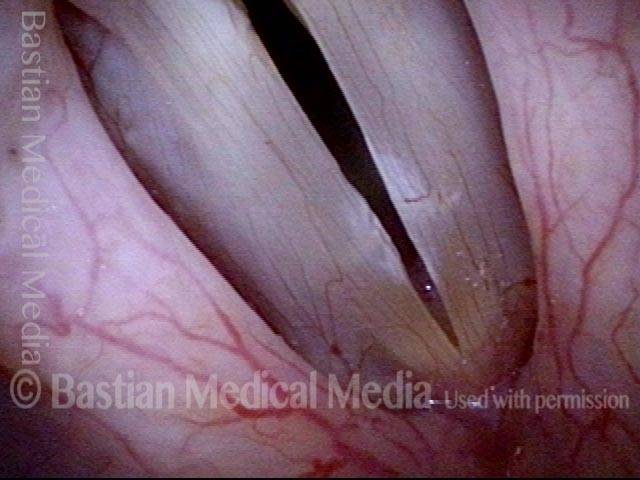
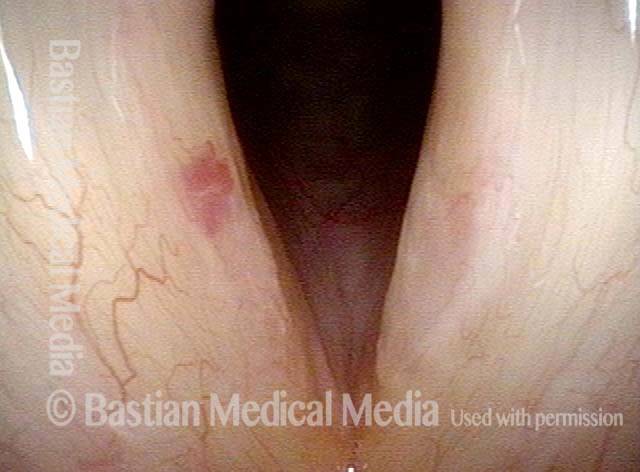
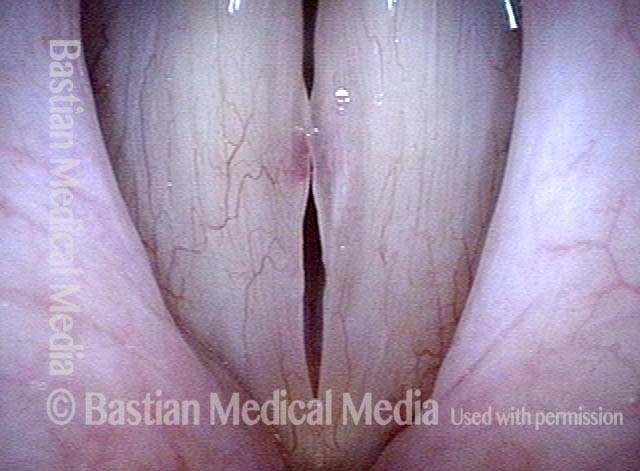
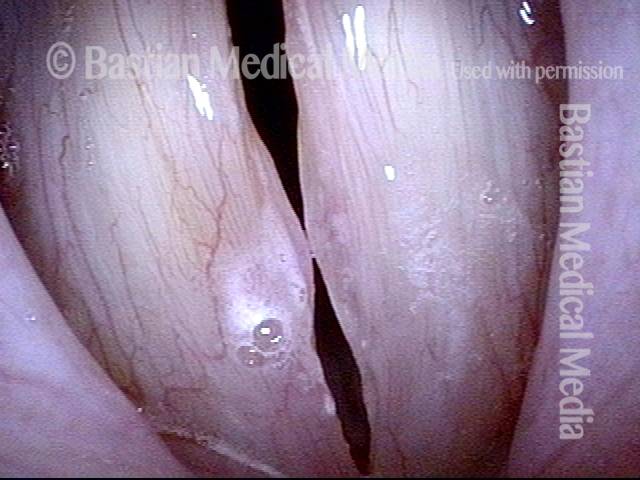
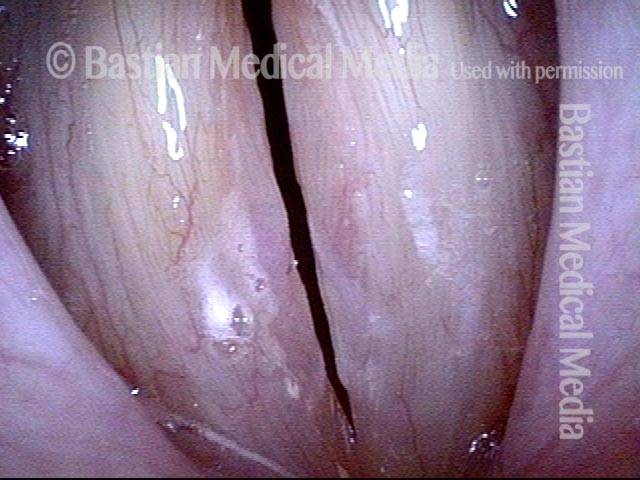
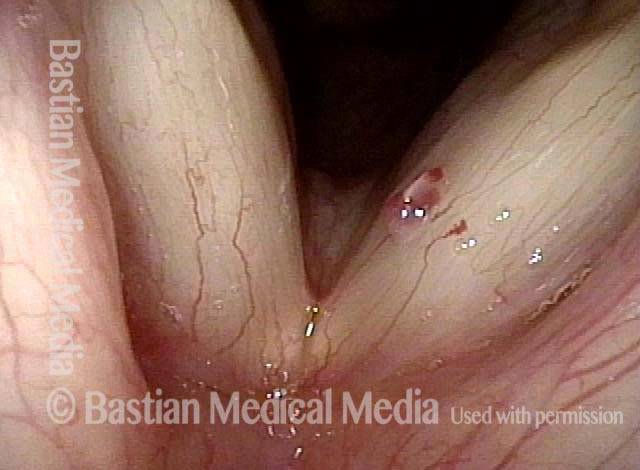
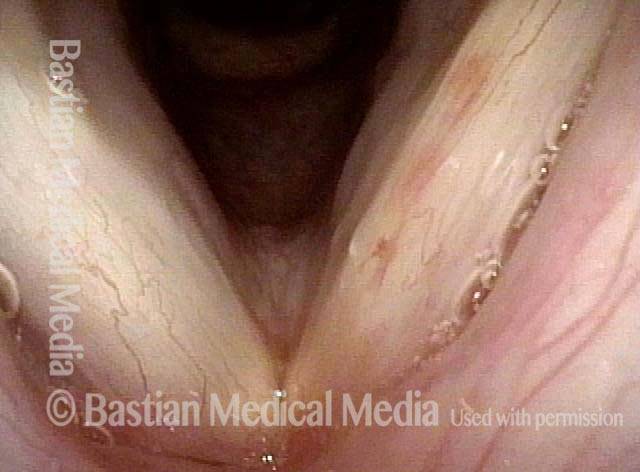
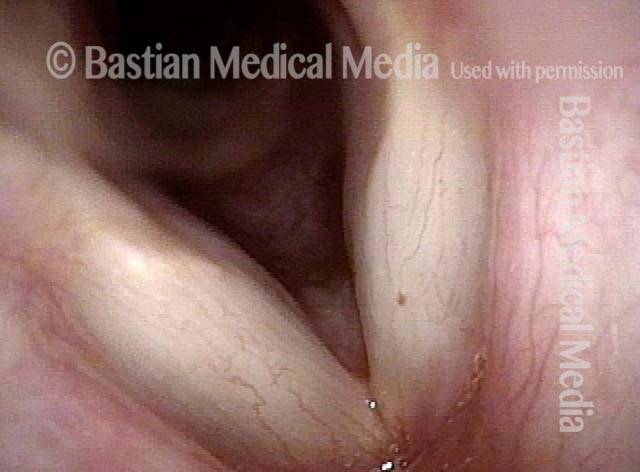
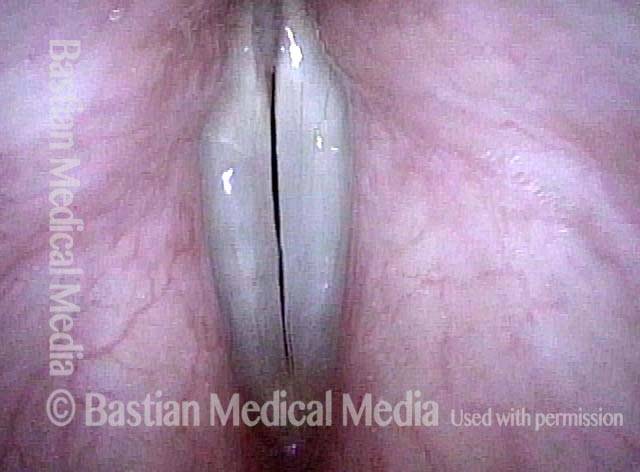
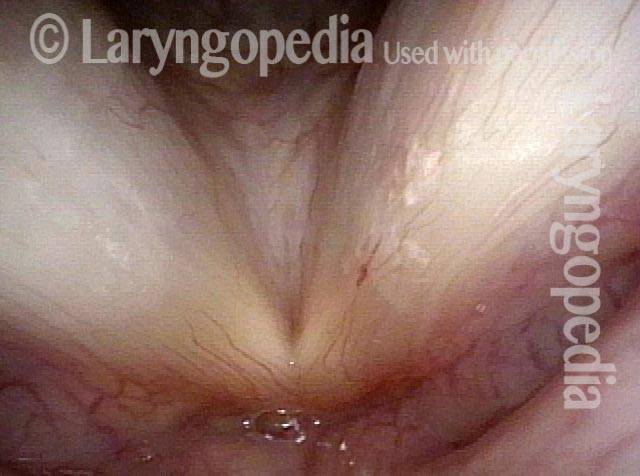
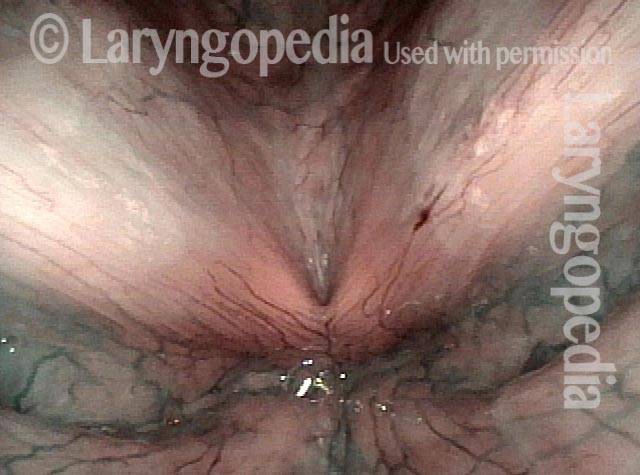
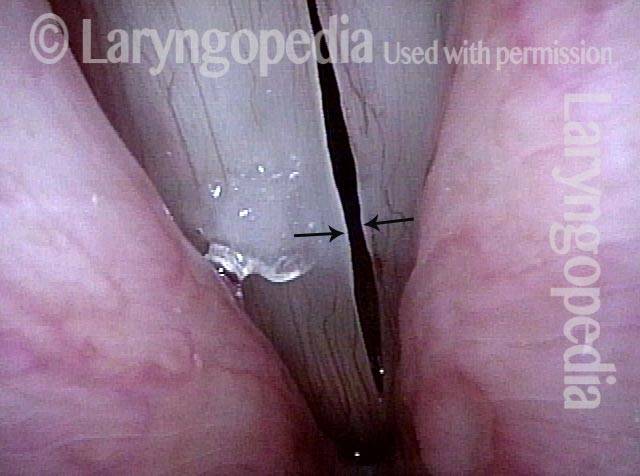
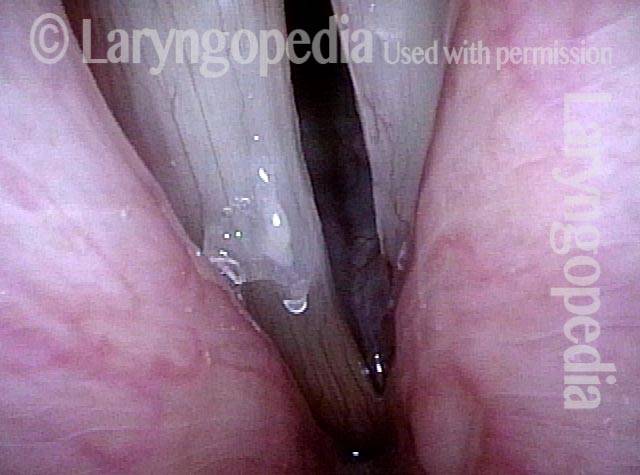
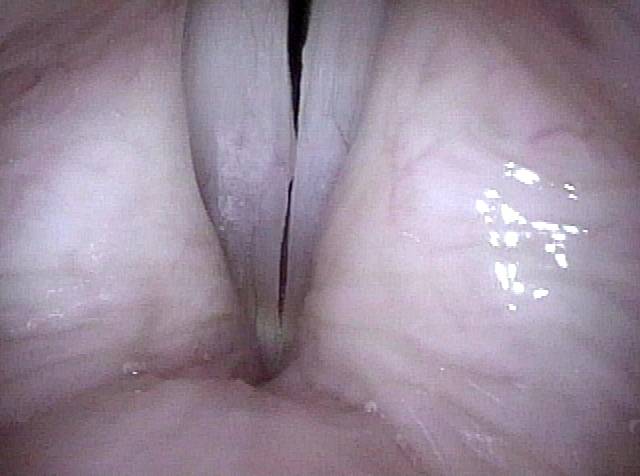
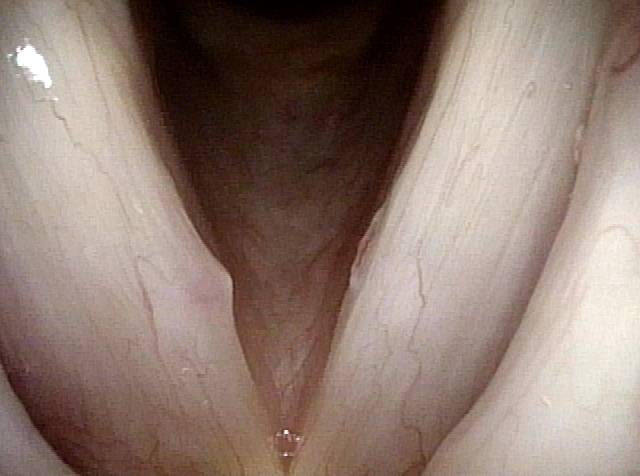
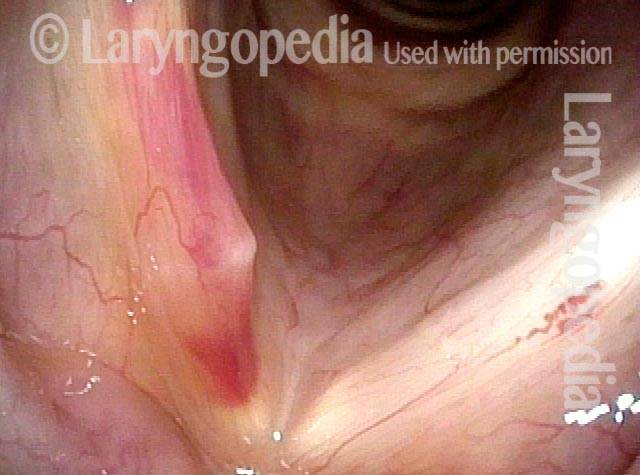
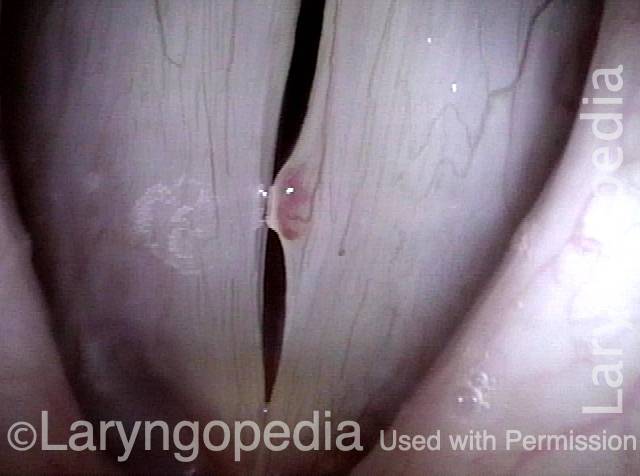
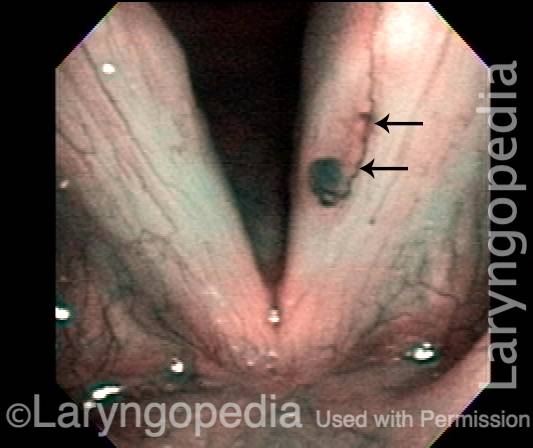
Capillary ectasia is the enlargement or dilation of capillaries on the surface of the vocal cords. Some believe it to be an estrogen effect similar to “spider veins” that one might see on the legs, for example. At our practice we think of these as mainly being another manifestation of overuse of the voice, and a response to ongoing injury of the vocal cords.
Symptoms
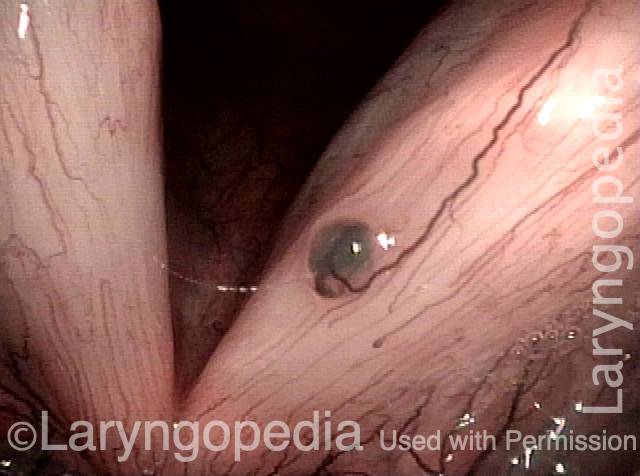
Once established, it may cause symptoms of reduced vocal endurance and exaggerated premenstrual huskiness. Capillary ectasia may also increase the risk of vocal cord bruising (hemorrhage) and hemorrhagic polyp formation.
Treatment
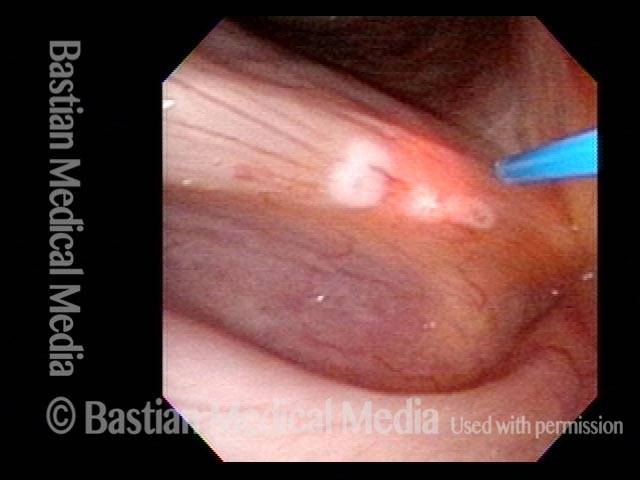
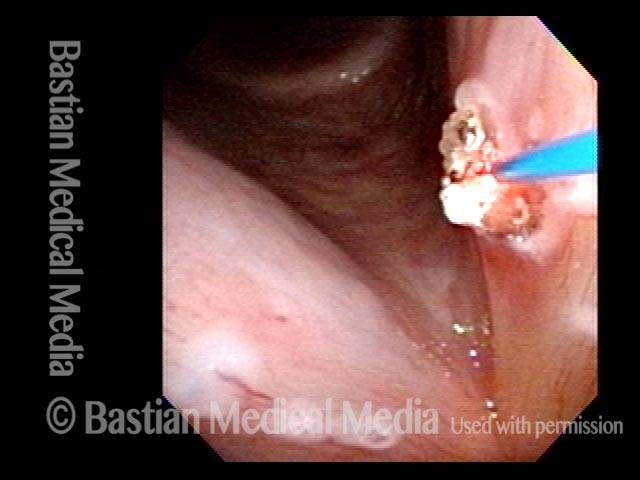
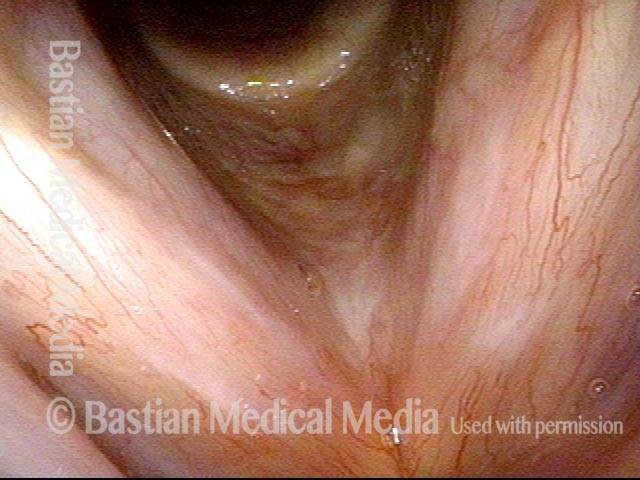
Many affected individuals, however, may “coexist” with this when armed with appropriate information about this disorder and through carefully managing amount and manner of voice use. When indicated, it is easily corrected via vocal cord microsurgery.
Vocal Cord Bruises (Hemorrhage) often Initially Obscure the Ectatic Capillary “Culprit”
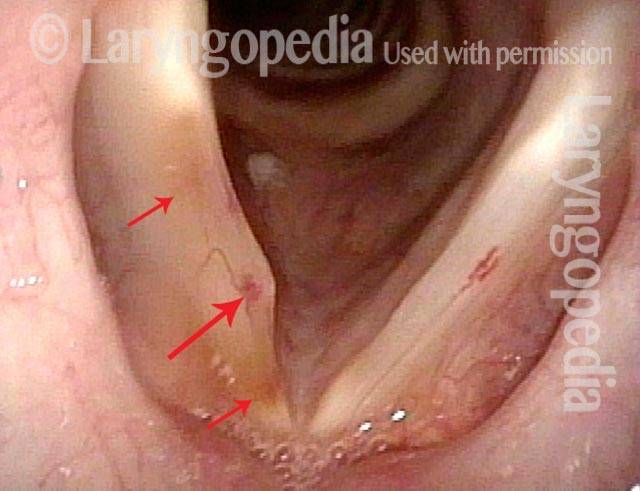
A person can experience sudden hoarseness at a time of sustained heavy voice use, or even immediately following a “scream,” or even a loud sneeze. The explanation might be a bruise of a vocal cord. This can happen to anyone but is far more likely if the person has underlying capillary ectasia.
When a bruised vocal cord is seen, therefore, the question is: “Is this a fluke bruise that can happen to anyone, or is it one explained by capillary ectasia?” In this instance, the answer is “yes.”
Singer’s Bruised Vocal Cord (1 of 8)
Singer’s Bruised Vocal Cord (1 of 8)
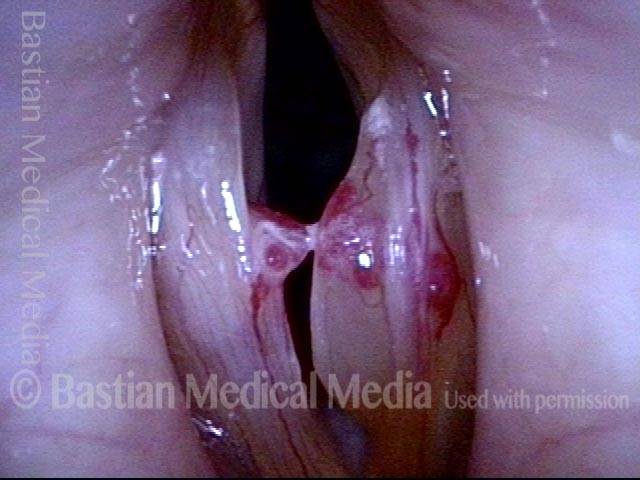
Bruise under Strobe Light (2 of 8)
Bruise under Strobe Light (2 of 8)
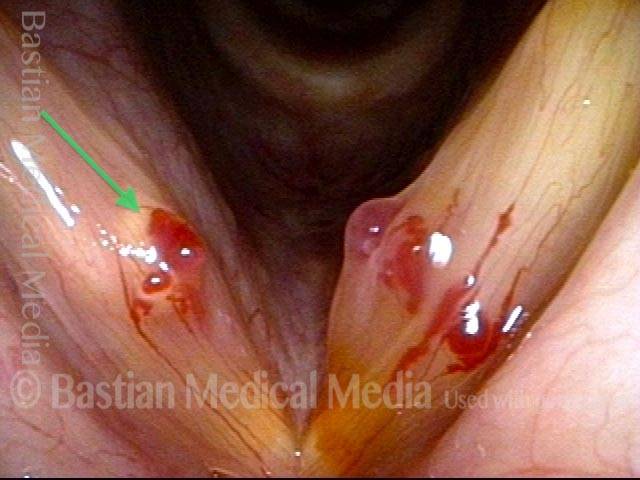
Abnormal capillary (3 of 8)
Abnormal capillary (3 of 8)
Bruise is gone (4 of 8)
Bruise is gone (4 of 8)
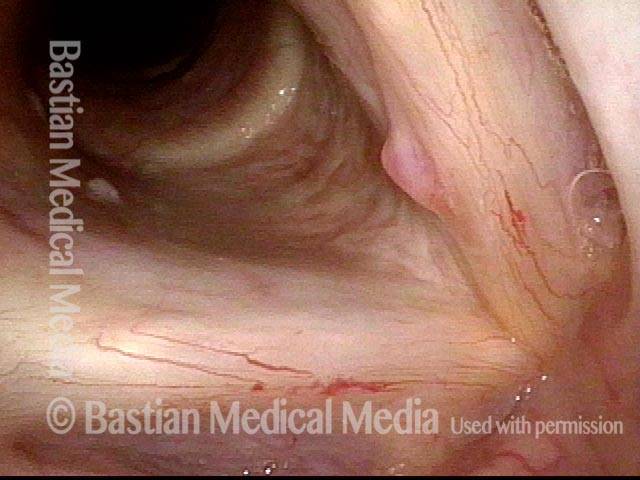
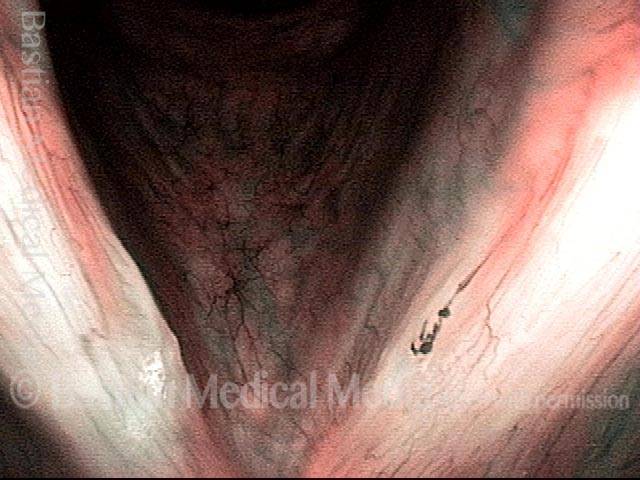
Capillaries under narrow band light (5 of 8)
Capillaries under narrow band light (5 of 8)
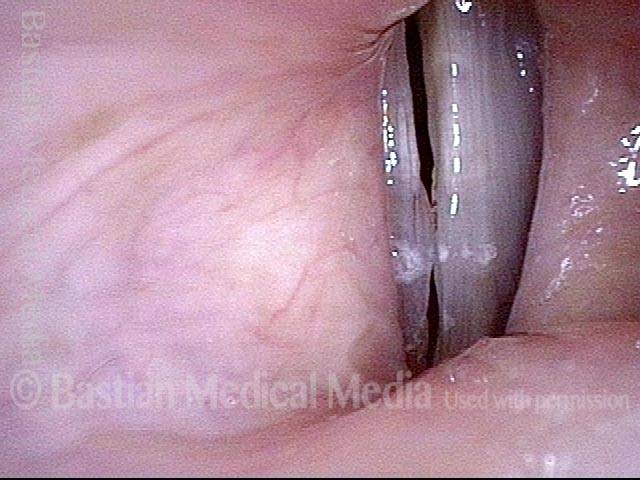
Capillaries touch during phonation (6 of 8)
Capillaries touch during phonation (6 of 8)
Post-surgical repair (7 of 8)
Post-surgical repair (7 of 8)
Margins match (8 of 8)
Margins match (8 of 8)
Capillary Ectasia, Before and After Laser Coagulation
Capillary ectasia (1 of 7)
Capillary ectasia (1 of 7)
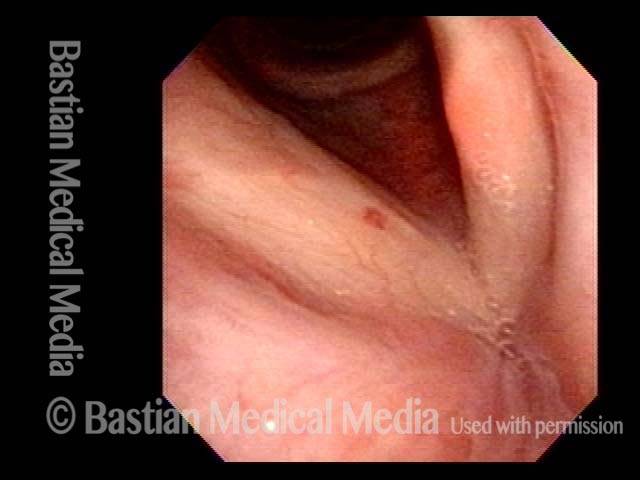
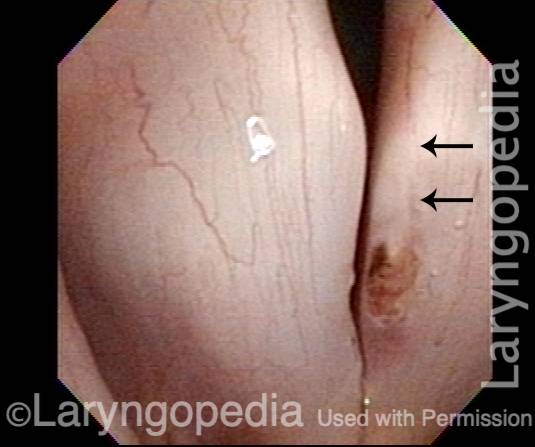
Capillary ectasia (2 of 7)
Capillary ectasia (2 of 7)
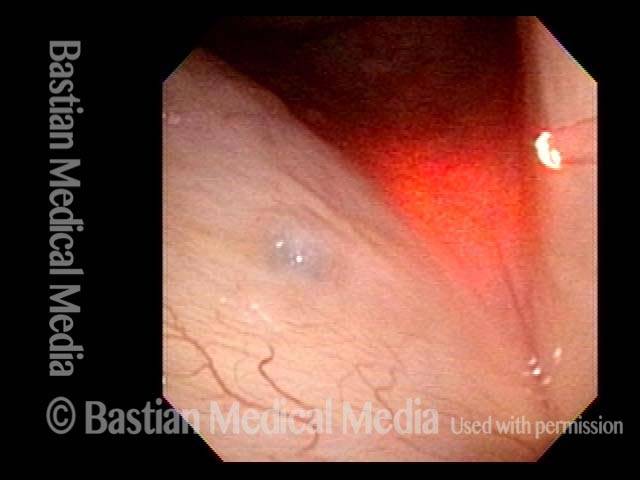
Capillary ectasia (3 of 7)
Capillary ectasia (3 of 7)
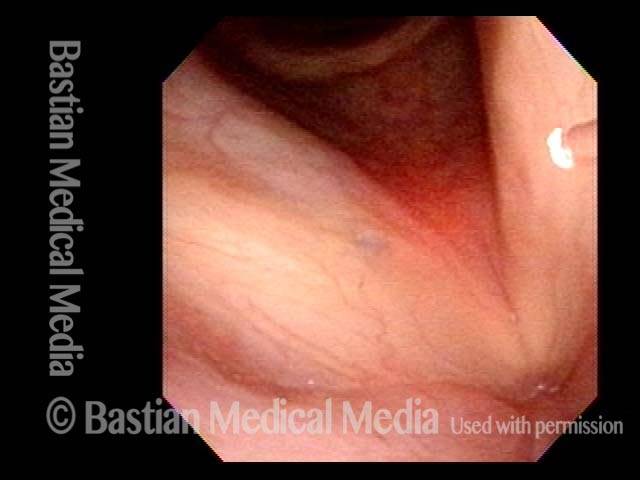
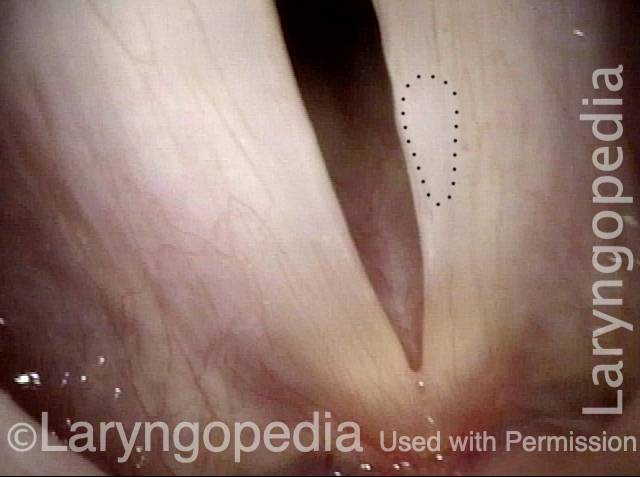
Closed phase (4 of 7)
Closed phase (4 of 7)
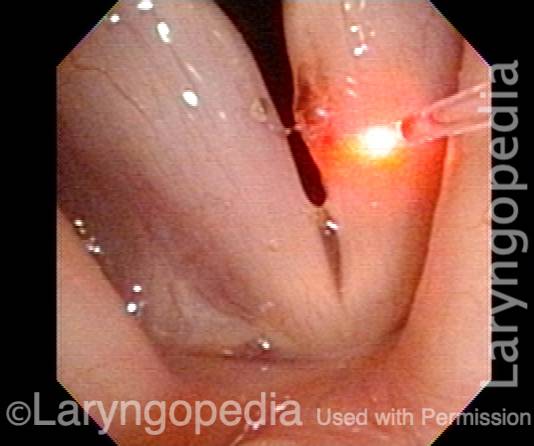
Capillary ectasia, after laser coagulation (5 of 7)
Capillary ectasia, after laser coagulation (5 of 7)
Capillary ectasia, after laser coagulation (6 of 7)
Capillary ectasia, after laser coagulation (6 of 7)
After laser coagulation (7 of 7)
After laser coagulation (7 of 7)
Example 2
Capillary ectasia (1 of 3)
Capillary ectasia (1 of 3)
Capillary ectasia, right after laser coagulation (2 of 3)
Capillary ectasia, right after laser coagulation (2 of 3)
Capillary ectasia, 6 weeks after laser coagulation (3 of 3)
Capillary ectasia, 6 weeks after laser coagulation (3 of 3)
A Vocal Cord Bruise That Could Happen To Anyone
While capillary ectasia (as seen in other photo series here) markedly increases vulnerability to vocal cord bruising, every human vocal cord has capillaries on its service, and even normal capillaries can leak and cause a bruise with sufficient vocal trauma. In this person, with an aggressive cough, her normal capillaries are the source of the bruise.
Bruised Vocal Cord (1 of 2)
Bruised Vocal Cord (1 of 2)
Bruised Vocal Cord (2 of 2)
Bruised Vocal Cord (2 of 2)
Capillary Ectasia and Hemorrhagic Polyp, Before and After Treatment
Capillary ectasia and hemorrhagic polyp (1 of 4)
Capillary ectasia and hemorrhagic polyp (1 of 4)
Capillary ectasia and hemorrhagic polyp (2 of 4)
Capillary ectasia and hemorrhagic polyp (2 of 4)
Capillary ectasia and hemorrhagic polyp, after treatment (3 of 4)
Capillary ectasia and hemorrhagic polyp, after treatment (3 of 4)
Capillary ectasia and hemorrhagic polyp, after treatment (4 of 4)
Capillary ectasia and hemorrhagic polyp, after treatment (4 of 4)
Capillary Ectasia and Hemorrhagic Polyp
Capillary ectasia and hemorrhagic polyp (1 of 2)
Capillary ectasia and hemorrhagic polyp (1 of 2)
Capillary ectasia and hemorrhagic polyp (2 of 2)
Capillary ectasia and hemorrhagic polyp (2 of 2)
Capillary Ectasia and Hemorrhagic Polyp, Treated by Thulium Laser
Capillary ectasia and hemorrhagic polyp (1 of 7)
Capillary ectasia and hemorrhagic polyp (1 of 7)
Capillary ectasia and hemorrhagic polyp (2 of 7)
Capillary ectasia and hemorrhagic polyp (2 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (3 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (3 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (4 of 7)
Capillary ectasia and hemorrhagic polyp, thulium laser treatment (4 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (5 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (5 of 7)
Vocal cord margin (6 of 7)
Vocal cord margin (6 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (7 of 7)
Capillary ectasia and hemorrhagic polyp, after treatment (7 of 7)
Capillary Ectasia with Vocal Nodules
Capillary ectasia with vocal nodules (1 of 2)
Capillary ectasia with vocal nodules (1 of 2)
Capillary ectasia with vocal nodules (2 of 2)
Capillary ectasia with vocal nodules (2 of 2)
Example 2
Capillary ectasia with vocal nodules (1 of 3)
Capillary ectasia with vocal nodules (1 of 3)
Capillary ectasia with vocal nodules (2 of 3)
Capillary ectasia with vocal nodules (2 of 3)
Capillary ectasia with vocal nodules (3 of 3)
Capillary ectasia with vocal nodules (3 of 3)
Vocal Nodules, Leukoplakia, and Capillary Ectasia
Vocal nodules, leukoplakia, and capillary ectasia (1 of 4)
Vocal nodules, leukoplakia, and capillary ectasia (1 of 4)
Vocal nodules, leukoplakia, and capillary ectasia (2 of 4)
Vocal nodules, leukoplakia, and capillary ectasia (2 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (3 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (3 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (4 of 4)
Vocal nodules, leukoplakia, and capillary ectasia: 6 months later (4 of 4)
Capillary Lake and KTP
Capillary lake (1 of 8)
Capillary lake (1 of 8)
Mucosal fatigue (2 of 8)
Mucosal fatigue (2 of 8)
Prep for laser coagulation (3 of 8)
Prep for laser coagulation (3 of 8)
KTP laser coagulation (4 of 8)
KTP laser coagulation (4 of 8)
Post laser ablation (5 of 8)
Post laser ablation (5 of 8)
Post laser ablation, distant view (6 of 8)
Post laser ablation, distant view (6 of 8)
After a weekend of vocal overuse (7 of 8)
After a weekend of vocal overuse (7 of 8)
Capillary (8 of 8)
Capillary (8 of 8)
Choral Singer’s Voice Fully Restored
Hoarse choral singer (1 of 4)
Hoarse choral singer (1 of 4)
Residual bruising (2 of 4)
Residual bruising (2 of 4)
2 months post-surgery (3 of 4)
2 months post-surgery (3 of 4)
Margins match (4 of 4)
Margins match (4 of 4)
Red Herring Capillary Ectasia and Mucosal Injuries
Ectatic capillary (1 of 4)
Ectatic capillary (1 of 4)
Ectatic capillary, narrow band light (2 of 4)
Ectatic capillary, narrow band light (2 of 4)
Margin swelling (3 of 4)
Margin swelling (3 of 4)
Bowing, atrophy, and flaccidity (4 of 4)
Bowing, atrophy, and flaccidity (4 of 4)
Ask Both Voice (via vocal phenomenology) and Larynx (via a motivated examination) to Give up their Secrets
Obvious mucosal injury (1 of 3)
Obvious mucosal injury (1 of 3)
Vocal nodules (2 of 3)
Vocal nodules (2 of 3)
Capillary ectasia (3 of 3)
Capillary ectasia (3 of 3)
The Evolution of Vocal Cord Bruising and Emergence of a Vulnerable Capillary
Margin swelling and bruising (1 of 2)
Margin swelling and bruising (1 of 2)
Six weeks later (2 of 2)
Six weeks later (2 of 2)
Pulsed KTP Laser Treatment of Vascular Abnormalities in a Singer
Ectatic capillary (1 of 7)
Ectatic capillary (1 of 7)
Polyp (2 of 7)
Polyp (2 of 7)
Feeding capillary (3 of 7)
Feeding capillary (3 of 7)
Glass fiber (4 of 7)
Glass fiber (4 of 7)
At the conclusion of the laser procedure (5 of 7)
At the conclusion of the laser procedure (5 of 7)
Blanched area (6 of 7)
Blanched area (6 of 7)
Polyp is gone (7 of 7)
Polyp is gone (7 of 7)
Share this article

Capillary ectasia (including KTP laser treatment)
This video illustrates the various causes of capillary ectasia and the treatment options that are available to patients, including pulsed-KTP laser treatment.

Nodules and Other Vocal Cord Injuries: How They Occur and Can Be Treated
This video explains how nodules and other vocal cord injuries occur: by excessive vibration of the vocal cords, which happens with vocal overuse. Having laid that foundational understanding, the video goes on to explore the roles of treatment options like voice therapy and vocal cord microsurgery.